Abstract
Objective
To evaluate the utility of a point of care lung ultrasound (POC-LUS) on patient management in the Neonatal Intensive Care Unit (NICU).
Study design
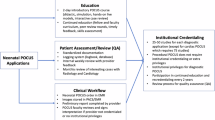
A retrospective cohort study of neonates who had POC-LUS from 2016 to 2020 in two-level III NICUs in Winnipeg, Manitoba, Canada. The primary outcome was the change in clinical management. The analysis aims mainly to describe the implementation process of the POC-LUS program.
Results
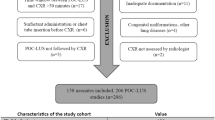
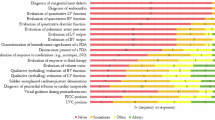
A total of 956 neonates underwent 4076 POC-LUS studies during the study period. The number of POC-LUS studies increased significantly every year, from 316 (in 2016) to 1257 (in 2020) (p < 0.001). POC-LUS resulted in a change in clinical management following 2528 POC-LUS studies (62%), while it supported continuing the same management in 1548 studies (38%).
Conclusion
POC-LUS in Manitoba increased since its inception and led to an alteration in the clinical management in a significant proportion of patients who received the service.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
All data and original material are available for transparency.
References
Lichtenstein DA, Mauriat P. Lung Ultrasound in the Critically Ill Neonate. Curr Pediatr Rev. 2012;8:217–23.
Elsayed Y, Abdelmawla M, Narvey M, Wrogemann J. A model of integrated lung and focused heart ultrasound as a new screening examination in infants at risk of respiratory or hemodynamic compromise. J Pediatr Neonatal Individ Med. 2017;6.
Liu J, Wang Y, Fu W, Yang C-S, Huang J-J. Diagnosis of neonatal transient tachypnea and its differentiation from respiratory distress syndrome using lung ultrasound. Med (Baltim). 2014;93:e197 http://content.wkhealth.com/linkback/openurl?sid=WKPTLP:landingpage&an=00005792-201412020-00025.
Yousef N, Singh Y, De Luca D. “Playing it SAFE in the NICU” SAFE-R: A targeted diagnostic ultrasound protocol for the suddenly decompensating infant in the NICU. Eur J Pediatr. 2021;181:393–8.
Louis D, Belen K, Farooqui M, Idiong N, Amer R, Hussain A, et al. Prone versus Supine Position for Lung Ultrasound in Neonates with Respiratory Distress. Am J Perinatol. 2019;38:4–9.
Abdelmawla M, Louis D, Narvey M, Elsayed Y. A lung ultrasound severity score predicts chronic lung disease in preterm infants. Am J Perinatol. 2019;36:1357–61. https://doi.org/10.1055/s-0038-1676975
Mohamed A, Mohsen N, Diambomba Y, Lashin A, Louis D, Elsayed Y, et al. Lung ultrasound for prediction of bronchopulmonary dysplasia in extreme preterm neonates: A prospective diagnostic cohort study. J Pediatr. 2021. https://doi.org/10.1016/j.jpeds.2021.06.079.
Elsayed YN, Hinton M, Graham R, Dakshinamurti S. Lung ultrasound predicts histological lung injury in a neonatal model of acute respiratory distress syndrome. Pediatr Pulmonol. 2020;July:1–11.
Soliman RM, Elsayed Y, Said RN, Abdulbaqi AM, Hashem RH, Aly H. Prediction of extubation readiness using lung ultrasound in preterm infants. Pediatr Pulmonol. 2021;56:2073–80.
Santos TM, Franci D, Coutinho CMG, Ribeiro DL, Schweller M, Matos-Souza JR, et al. A simplified ultrasound-based edema score to assess lung injury and clinical severity in septic patients. Am J Emerg Med. 2013;31:1656–60. https://doi.org/10.1016/j.ajem.2013.08.053.
Bouhemad B, Brisson H, Le-Guen M, Arbelot C, Lu Q, Rouby JJ. Bedside ultrasound assessment of positive end-expiratory pressure-induced lung recruitment. Am J Respir Crit Care Med. 2011;183:341–7.
Brat R, Yousef N, Klifa R, Reynaud S, Shankar Aguilera S, De Luca D. Lung Ultrasonography Score to Evaluate Oxygenation and Surfactant Need in Neonates Treated With Continuous Positive Airway Pressure. JAMA Pediatr. 2015;169:e151797 http://archpedi.jamanetwork.com/article.aspx?doi=10.1001/jamapediatrics.2015.1797.
Raimondi F, Migliaro F, Sodano A, Umbaldo A, Romano A, Vallone G, et al. Can neonatal lung ultrasound monitor fluid clearance and predict the need of respiratory support? Crit Care. 2012;16:R220 http://ccforum.com/content/16/6/R220.
Tusman G, Acosta CM, Costantini M. Ultrasonography for the assessment of lung recruitment maneuvers. Crit Ultrasound J. 2016;8:8 http://www.ncbi.nlm.nih.gov/pubmed/27496127.
Raimondi F, Rodriguez Fanjul J, Aversa S, Chirico G, Yousef N, De Luca D, et al. Lung Ultrasound for Diagnosing Pneumothorax in the Critically Ill Neonate. J Pediatr. 2015;175:74–8.e1.
Galbois A, Ait-Oufella H, Baudel JL, Kofman T, Bottero J, Viennot S, et al. Pleural ultrasound compared with chest radiographic detection of pneumothorax resolution after drainage. Chest. 2010;35:143–50.
Lichtenstein D, Hulot JS, Rabiller A, Tostivint I, Mezière G. Feasibility and safety of ultrasound-aided thoracentesis in mechanically ventilated patients. Intensive Care Med. 1999;25:955–8.
Pereda MA, Chavez MA, Hooper-miele CC, Gilman RH. Lung ultrasound for the diagnosis of pneumonia in children: A Meta-analysis. 2021;135:714–22.
Elsayed YN, Fraser D. Integrated evaluation of neonatal hemodynamics program optimizing organ perfusion and performance in critically ill neonates, part 1: Understanding physiology of neonatal hemodynamics. Neonatal Netw. 2016;35:143–50.
Liu J, Chi J, Ren X, Li J, Chen Y. American Journal of Emergency Medicine Lung ultrasonography to diagnose pneumothorax of the newborn ☆. Am J Emerg Med. 2017;35:1298–302. https://doi.org/10.1016/j.ajem.2017.04.001.
Chen S, Fu W, Liu J, Wang Y. Routine application of lung ultrasonography in the neonatal intensive care unit. 2017;96:e5826.
Conlon TW, Nishisaki A, Singh Y, Bhombal S, De Luca D, Kessler DO, et al. Moving beyond the stethoscope: Diagnostic point-of-care ultrasound in pediatric practice. Pediatrics. 2019;144:e20191402.
Escourrou G, De Luca D. Lung ultrasound decreased radiation exposure in preterm infants in a neonatal intensive care unit. Acta Paediatr [Internet]. 2016;n/a-n/a. Available from: http://doi.wiley.com/10.1111/apa.13369.
Corsini I, Dani C. Lung ultrasound in the neonatal intensive care unit: Review of the literature and future perspectives. 2020;(April):1550–62.
De Martino L, Yousef N, Ben-Ammar R, Raimondi F, Shankar-Aguilera S, De Luca D. Lung ultrasound score predicts surfactant need in extremely preterm neonates. Pediatrics 2018;142:e20180463.
Pezza L, Alonso-Ojembarrena A, Elsayed Y, Yousef N, Vedovelli L, Raimondi F, et al. Meta-analysis of lung ultrasound scores for early prediction of bronchopulmonary dysplasia. Ann American Thor Soc. 2021;2016:1–39.
Alonso‐Ojembarrena A, Lubián‐López SP. Lung ultrasound score as early predictor of bronchopulmonary dysplasia in very low birth weight infants. Pediatr Pulmonol. 2019;54:1404–9. https://doi.org/10.1002/ppul.24410.
Liu J, Chen XX, Li XW, Chen SW, Yan W, Fu W. Lung ultrasonography to diagnose transient tachypnea of the newborn. Chest. 2016;149:1269–75. https://doi.org/10.1016/j.chest.2015.12.024.
Cattarossi L, Copetti R, Brusa G, Pintaldi S. Lung Ultrasound Diagnostic Accuracy in Neonatal Pneumothorax. 2016;2016:6515069.
Author information
Authors and Affiliations
Contributions
All authors made a substantial contribution to the manuscript and the design of the work: Elsayed collected and analyzed data, wrote the first draft, all authors are POC-LUS instructors and participated in the practice guidelines, all authors edited and wrote part of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
This study was approved by the Ethical committee at the University of Manitoba for data collection and publication (#HS21962).
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Elsayed, Y., Narvey, M., Lashin, A. et al. Point of care lung ultrasound service in neonatal intensive care: Five years of experience in Manitoba, Canada. J Perinatol 42, 1228–1232 (2022). https://doi.org/10.1038/s41372-022-01455-w
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41372-022-01455-w
This article is cited by
-
Utilization of integrated lung ultrasound and targeted neonatal echocardiography in preterm infant follow-up: is it feasible? Assessing value and practical challenges
European Journal of Pediatrics (2026)
-
Implementation of a standardized lung ultrasound protocol for respiratory distress in a neonatal intensive care unit: an observational study
Journal of Perinatology (2024)
-
Current perception and barriers to implementing lung ultrasound in Canadian neonatal intensive care units: a national survey
European Journal of Pediatrics (2024)