Abstract
Objective
To identify challenges vs. supports in the NICU and after NICU discharge for parents of an infant with a major congenital anomaly.
Study design
Qualitative study.
Results
We interviewed 18 parents (13 mothers, 5 fathers) whose children were admitted to our our NICU with a major congenital anomaly. In the NICU, challenges were navigating parenthood with significant impact on parent mental health, adjusting to changing healthcare providers, and need for better interdisciplinary communication. After discharge home, challenges were an initial adjustment to life without NICU monitoring, loss of NICU medical resources, burden of caregiving, continued healthcare utilization, and financial impact.
Conclusion
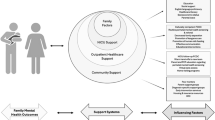
Key supports that were helpful to families were empathetic and consistent healthcare teams throughout their care journey, especially nurses; healthcare team members who went beyond medical care, consistent communication, parent engagement in NICU care, ongoing parent mental health support, and peer resources after discharge home.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Data availability
The dataset generated and analyzed during the current study are not publicly available due to privacy reasons as they include patient or parent identifiers but written transcripts with identifiers removed may be available from the corresponding author on reasonable request.
References
How Infants Die in the Neonatal Intensive Care Unit: Trends From 1999 Through 2008, Critical Care Medicine, JAMA Pediatrics, JAMA Network. 2021. https://jamanetwork.com/journals/jamapediatrics/article-abstract/1107554.
Cohen E, Berry JG, Camacho X, Anderson G, Wodchis W, Guttmann A. Patterns and Costs of Health Care Use of Children With Medical Complexity. Pediatrics. 2012;130:e1463–70.
Acharya K, Rholl E, Malin K, Malnory M, Leuthner J, Leuthner SR, et al. Parent Health-Related Quality of Life for Infants with Congenital Anomalies Receiving Neonatal Intensive Care. J Pediatrics. 2022;245:39–46.e2.
Welke N, Lagatta J, Leuthner S, Acharya K. Three-Year Post-Neonatal Intensive Care Unit Health Care Utilization Among Infants with Congenital Anomalies. J Pediatrics. 2024;265:113779.
Oftedal A, Bekkhus M, Haugen G, Hjemdal O, Czajkowski NO, Kaasen A. Long-Term Impact of Diagnosed Fetal Anomaly on Parental Traumatic Stress, Resilience, and Relationship Satisfaction. J Pediatr Psychol. 2023;48:181–92.
Miquel-Verges F, Woods SL, Aucott SW, Boss RD, Sulpar LJ, Donohue PK. Prenatal Consultation With a Neonatologist for Congenital Anomalies: Parental Perceptions. Pediatrics. 2009;124:e573–9.
Janvier A. Breathe, Baby, Breathe!: Neonatal Intensive Care, Prematurity, and Complicated Pregnancies. University of Toronto Press; 2019. 375 p.
Janvier A, Bourque CJ, Pearce R, Thivierge E, Duquette LA, Jaworski M, et al. Fragility and resilience: parental and family perspectives on the impacts of extreme prematurity. Arch Dis Child Fetal Neonatal Ed. 2023;108:575–80.
Whittingham K, Boyd RN, Sanders MR, Colditz P. Parenting and Prematurity: Understanding Parent Experience and Preferences for Support. J Child Fam Stud. 2014;23:1050–61.
Pepper D, Rempel G, Austin W, Ceci C, Hendson L. More Than Information: A Qualitative Study of Parents’ Perspectives on Neonatal Intensive Care at the Extremes of Prematurity. Adv Neonatal Care. 2012;12:303.
Leuthner SR, Bolger M, Frommelt M, Nelson R. The impact of abnormal fetal echocardiography on expectant parents’ experience of pregnancy: a pilot study. J Psychosom Obstet Gynecol. 2003;24:121–9.
Carlsson T, Starke V, Mattsson E. The emotional process from diagnosis to birth following a prenatal diagnosis of fetal anomaly: A qualitative study of messages in online discussion boards. Midwifery. 2017;48:53–9.
Gaspar CR. Parents’ Psychological Adaptation after Receiving a Fetal Diagnosis: A Systematic Review. Graduate Student J Psychol. 2022;19. Available from: https://journals.library.columbia.edu/index.php/gsjp/article/view/10106.
Hodgson J, McClaren BJ. Parental experiences after prenatal diagnosis of fetal abnormality. Semin Fetal Neonatal Med. 2018;23:150–4.
Horsch A, Brooks C, Fletcher H. Maternal coping, appraisals and adjustment following diagnosis of fetal anomaly. Prenat Diagnosis. 2013;33:1137–45.
McKechnie AC, Erickson K, Ambrose MB, Chen S, Miller SJ, Mathiason MA, et al. Development and testing of a self-report measure of preparing to parent in the context of a fetal anomaly diagnosis. Patient Educ Couns. 2021;104:666–70.
Hedrick J. The Lived Experience of Pregnancy While Carrying a Child With a Known, Nonlethal Congenital Abnormality. J Obstet Gynecologic Neonatal Nurs. 2005;34:732–40.
Lotto R, Armstrong N, Smith LK. Care provision during termination of pregnancy following diagnosis of a severe congenital anomaly – A qualitative study of what is important to parents. Midwifery. 2016;43:14–20.
Mazer P, Gischler SJ, Koot HM, Tibboel D, van Dijk M, Duivenvoorden HJ. Impact of a child with congenital anomalies on parents (ICCAP) questionnaire; a psychometric analysis. Health Qual Life Outcomes. 2008;6:102.
Holm KG, Neville AJ, Pierini A, Latos Bielenska A, Jamry-Dziurla A, Cavero-Carbonell C, et al. The Voice of Parents of Children With a Congenital Anomaly – A EUROlinkCAT Study. Front Pediatr. 2021;9. https://www.frontiersin.org/journals/pediatrics/articles/10.3389/fped.2021.654883/full.
Infant Deaths After Texas’ 2021 Ban on Abortion in Early Pregnancy, Women’s Health, JAMA Pediatrics, JAMA Network. 2024. Available from: https://jamanetwork.com/journals/jamapediatrics/article-abstract/2819785.
CDC. Centers for Disease Control and Prevention. What are Birth Defects? 2020. CDC. Available from: https://www.cdc.gov/ncbddd/birthdefects/facts.html.
Hsieh HF, Shannon SE. Three Approaches to Qualitative Content Analysis. Qual Health Res. 2005. Available from: https://journals.sagepub.com/doi/abs/10.1177/1049732305276687.
Satu E, Kyngäs S. The qualitative content analysis process. J Adv Nurs. 2008. Available from: https://onlinelibrary.wiley.com/doi/full/10.1111/j.1365-2648.2007.04569.x.
Wilpers A, Bahtiyar MO, Stitelman D, Batten J, Calix RX, Chase V, et al. The parental journey of fetal care: a systematic review and metasynthesis. Am J Obstet Gynecol MFM. 2021;3:100320.
Spence CM, Stuyvenberg CL, Kane AE, Burnsed J, Dusing SC. Parent Experiences in the NICU and Transition to Home. Int J Environ Res Public Health. 2023;20:6050.
Leuthner S, Jones EL. Fetal Concerns Program: A Model for Perinatal Palliative Care. MCN: Am J Matern/Child Nurs. 2007;32:272.
Haward MF, Lantos J, Janvier A. for the POST Group. Helping Parents Cope in the NICU. Pediatrics. 2020;145:e20193567.
Catlin A, Áskelsdóttir B, Conroy S, Rempel G. From Diagnosis to Birth: Parents’ Experience When Expecting a Child With Congenital Anomaly. Adv Neonatal Care. 2008;8:348–54.
Govindaswamy P, Laing S, Waters D, Walker K, Spence K, Badawi N. Stressors of parents of infants undergoing neonatal surgery for major non-cardiac congenital anomalies in a surgical neonatal intensive care unit. J Paediatrics Child Health. 2020;56:512–20.
Govindaswamy P, Laing S, Waters D, Walker K, Spence K, Badawi N. Needs of parents in a surgical neonatal intensive care unit. J Paediatrics Child Health. 2019;55:567–73.
Catapano F, Steinwurtzel R, Parravicini E, Wool C. A qualitative analysis of parents’ experiences while their neonates with congenital heart disease require intensive care. Front Pediatr. 2024;12. https://www.frontiersin.org/journals/pediatrics/articles/10.3389/fped.2024.1425320/full.
Uveges MK, Hamilton JB, Pados BF, Thayer WM, Hinds PS, Nolan MT. Being a “Good Parent” to a NICU Infant With a Major Congenital Anomaly. Adv Neonatal Care. 2024;24:14.
Wigert H, Dellenmark Blom M, Bry K. Parents’ experiences of communication with neonatal intensive-care unit staff: an interview study. BMC Pediatr. 2014;14:304.
Feehan K, Kehinde F, Sachs K, Mossabeb R, Berhane Z, Pachter LM, et al. Development of a Multidisciplinary Medical Home Program for NICU Graduates. Matern Child Health J. 2020;24:11–21.
DiBari JN, Rouse L. Parent Perspectives: Part 2—Considerations for the Transition Home Post-NICU Discharge. Children. 2023;10:1835.
Lakshmanan A, Kubicek K, Williams R, Robles M, Vanderbilt DL, Mirzaian CB, et al. Viewpoints from families for improving transition from NICU-to-home for infants with medical complexity at a safety net hospital: a qualitative study. BMC Pediatr. 2019;19:223.
Garfield CF, Lee YS, Kim HN, Rutsohn J, Kahn JY, Mustanski B, et al. Supporting parents of premature infants transitioning from the NICU to home: A pilot randomized control trial of a smartphone application. Internet Interventions. 2016;4:131–7.
Witt RE, Malcolm M, Colvin BN, Gill MR, Ofori J, Roy S, et al. Racism and Quality of Neonatal Intensive Care: Voices of Black Mothers. Pediatrics. 2022;150:e2022056971.
Sigurdson K, Mitchell B, Liu J, Morton C, Gould JB, Lee HC, et al. Racial/Ethnic Disparities in Neonatal Intensive Care: A Systematic Review. Pediatrics. 2019;144:e20183114.
Sigurdson K, Profit J, Dhurjati R, Morton C, Scala M, Vernon L, et al. Former NICU Families Describe Gaps in Family-Centered Care. Qual Health Res. 2020;30:1861–75.
Sigurdson K, Morton C, Mitchell B, Profit J. Disparities in NICU quality of care: a qualitative study of family and clinician accounts. J Perinatol. 2018;38:600–7.
Profit J, Gould JB, Bennett M, Goldstein BA, Draper D, Phibbs CS, et al. Racial/Ethnic Disparity in NICU Quality of Care Delivery. Pediatrics. 2017;140:e20170918.
Acknowledgements
The research team is grateful to Monica McLeod, former NICU parent, who reviewed the study design and interview guide and provided critical feedback. We are grateful to all the parents who participated in the research study and thank them for their contributions.
Funding
This study was internally supported by funds from the Department of Pediatrics, Children’s Wisconsin.
Author information
Authors and Affiliations
Contributions
JS screened and interviewed parents, conducted data analysis and wrote the first draft of the manuscript; NM contributed to study design, interview guide preparation, data analysis, and revision of manuscript; AG screened and interviewed parents and assisted in manuscript writing; TAZ screened and interviewed parents and assisted in manuscript writing; SL contributed to study design, interview guide preparation, data analysis and preparation of manuscript; JL contributed to study design and preparation of manuscript, KA designed the study, oversaw study implementation, conducted data analysis, and prepared final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
41372_2025_2255_MOESM1_ESM.docx (download DOCX )
Supplemental Table: Parents’ Experiences of their Child’s Anomaly during the Prenatal Period: Themes, Subthemes and Exemplar Quotes
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lyon, J., McAndrew, N., Geich, A. et al. Voices of parents of children with major congenital anomalies admitted to the NICU: initial diagnosis, hospitalization, and discharge home. J Perinatol 45, 755–766 (2025). https://doi.org/10.1038/s41372-025-02255-8
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41372-025-02255-8