Abstract
Objective
To perform three studies needed to design the “U-BET” trial (Umbilical cord Blood for Extremely-low-gestational-age Transfusions).
Study design
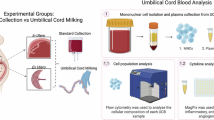
(1) Survey-based self-assessment of Intermountain Health obstetricians regarding drawing umbilical cord blood. (2) Determine the percentage of the potentially donating neonates who have type O blood (to be utilized in U-BET). (3) Quantify cord blood drawn using American Red Cross collection kits.
Results
(1) 72% of respondents declared experience drawing cord blood; 62% with the placenta in utero. (2) Of the past 100,000 women delivering, 48% were type O, and 66% of neonates born to them were type O. (3) The volume of cord blood obtained at 10 births ranged from 20 to 86 mL after the placenta was delivered vs. 14 to157 mL when in utero.
Conclusion
The U-BET trial will consent type O women and use Red Cross kits to draw term umbilical cord blood while the placenta is still in utero.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
Deidentified data will be shared on request to the corresponding author.
Code availability
Computer code used for statistical analysis will be shared on request to the corresponding author.
References
Christensen RD, Bahr TM, Christensen TR, Ohls RK, Krong J, Carlton LC, et al. Banked term umbilical cord blood to meet the packed red blood cell transfusion needs of extremely-low-gestational-age neonates: a feasibility analysis. J Perinatol. 2024;44:873–9.
Bianchi M, Papacci P, Valentini CG, Barbagallo O, Vento G, Teofili L. Umbilical cord blood as a source for red-blood-cell transfusion in neonatology: a systematic review. Vox Sang. 2018;113:713–25.
Bianchi M, Orlando N, Barbagallo O, Sparnacci S, Balentini CG, Carducci B, et al. Allogenic cord blood red blood cells: assessing cord blood unit fractionation and validation. Blood Trans. 2021;19:435–44.
Teofili L, Papacci P, Orlando N, Bianchi M, Pasciuto T, Mozzetta I, et al. BORN study: a multicenter randomized trial investigating cord blood red blood cell transfusions to reduce the severity of retinopathy of prematurity in extremely low gestational age neonates. Trials. 2022;23:1010.
Teofili L, Papacci P, Bartolo M, Molisso A, Orlando N, Pane L, et al. Transfusion-free survival predicts severe retinopathy in preterm neonates. Front Pediatr. 2022;10:814194.
Teofili L, Papacci P, Giannantonio C, Bianchi M, Valentini DG, Vento G. Allogenic cord blood transfusion in preterm infants. Clin Perinatol. 2023;50:88193.
Pellegrino C, Papacci P, Beccia F, Serrao F, Cantone GV, Cannetti G, et al. Differences in cerebral tissue oxygenation in preterm neonates receiving adult or cord blood red blood cell transfusions. JAMA Netw Open. 2023;6:e2341643.
Teofili L, Papacci P, Dani C, Cresi F, Remaschi G, Pellegrino C, et al. Cord blood transfusions in extremely low gestational age neonates to reduce severe retinopathy of prematurity: results of a prespecified interim analysis of the randomized BORN trial. Ital J Pediatr. 2024;50:142.
AABB. Standards for blood banks and transfusion services (BB/TS Standards). 33rd ed. AABB: California 2022.
Hughes CS, Schmitt S, Passarella M, Lorch SA, Phibbs CS. Who’s in the NICU? A population-level analysis. J Perinatol. 2024;44:1416–23.
Bell EF, Hintz SR, Hansen NI, Bann CM, Wyckoff MH, DeMauro SB, et al. Mortality, in-hospital morbidity, care practices, and 2-year outcomes for extremely Preterm infants in the US, 2013-2018. JAMA. 2022;327:248–63.
Clark C, Gibbs JA, Maniello R, Outerbridge EW, Aranda JV. Blood transfusion: a possible risk factor in retrolental fibroplasia. Acta Paediatr Scand. 1981;70:537–9.
Thomas K, Shah PS, Canning R, Harrison A, Lee SK, Dow KE. Retinopathy of prematurity: risk factors and variability in Canadian neonatal intensive care units. J Neonatal Perinat Med. 2015;8:207–14.
Bas AY, Demirel N, Koc E, Ulubas Isik D, Hirfanoglu İM, Tunc T, TR-ROP Study Group. Incidence, risk factors and severity of retinopathy of prematurity in Turkey (TR-ROP study): a prospective, multicentre study in 69 neonatal intensive care units. Br J Ophthalmol. 2018;102:1711–6.
Uberos J, Fernandez-Marin E, Campos-Martinez A, Ruiz-Lopez A, Garcia-Serrano JL. Blood products transfusion and retinopathy of prematurity: a cohort study. Acta Ophthalmol. 2023;101:e294–e301.
Glaser K, Härtel C, Dammann O, Herting E, Andres O, Speer CP, et al. German neonatal network. Erythrocyte transfusions are associated with retinopathy of prematurity in extremely low gestational age newborns. Acta Paediatr. 2023;112:2507–15.
Ramaswamy VV, Abiramalatha T, Bandyopadhyay T, Shaik NB, Bandiya P, Nanda D, et al. ELBW and ELGAN outcomes in developing nations-Systematic review and meta-analysis. PLoS ONE. 2021;16:e0255352.
Bahr TM, Snow GL, Christensen TR, Davenport P, Henry E, Tweddell SM, et al. Can red blood cell and platelet transfusions have a pathogenic role in bronchopulmonary dysplasia? J Pediatr. 2024;265:113836.
Patel RM, Knezevic A, Yang J, Shenvi N, Hinkes M, Roback JD, et al. Enteral iron supplementation, red blood cell transfusion, and risk of bronchopulmonary dysplasia in very-low-birth-weight infants. Transfusion. 2019;59:1675–82.
Zhang Z, Huang X, Lu H. Association between red blood cell transfusion and bronchopulmonary dysplasia in preterm infants. Sci Rep. 2014;4:4340.
Zhang H, Fang J, Su H, Chen M. Risk factors for bronchopulmonary dysplasia in neonates born at #1500 g (1999–2009). Pediatr Int. 2011;53:915–20.
Vu, Ohls PT, Mayock DE RK, German KR, Comstock BA, Heagerty PJ, et al. Transfusions and neurodevelopmental outcomes in extremely low gestation neonates enrolled in the PENUT Trial: a randomized clinical trial. Pediatr Res. 2021;90:109–16.
Shah P, Cannon DC, Lowe JR, Phillips J, Christensen RD, Kamath-Rayne B, et al. Effect of blood transfusions on cognitive development in very low birth weight infants. J Perinatol. 2021;41:1412–8.
Del Vecchio A, Henry E, D’Amato G, Cannuscio A, Corriero L, Motta M, et al. Instituting a program to reduce the erythrocyte transfusion rate was accompanied by reductions in the incidence of bronchopulmonary dysplasia, retinopathy of prematurity and necrotizing enterocolitis. J Matern Fetal Neonatal Med. 2013;26:77–9.
Bahr TM, Ohls RK, Henry E, Davenport P, Ilstrup SJ, Kelley WE, et al. The number of blood transfusions received and the incidence and severity of chronic lung disease among NICU patients born >31 weeks gestation. J Perinatol. 2025;45:218–23.
Puia-Dumitrescu M, Tanaka DT, Spears TG, Daniel CJ, Kumar KR, Athavale K, et al. Patterns of phlebotomy blood loss and transfusions in extremely low birth weight infants. J Perinatol. 2019;39:1670–5.
Bolat F, Dursun M, Sarıaydın M. Packed red blood cell transfusion as a predictor of moderate-severe bronchopulmonary dysplasia: a comparative cohort study of very preterm infants. Am J Perinatol. 2024;41:e1499–e1507.
Keir AK, McPhee AJ, Andersen CC, Stark MJ. Plasma cytokines and markers of endothelial activation increase after packed red blood cell transfusion in the preterm infant. Pediatr Res. 2013;73:75–9.
Dani C, Poggi C, Gozzini E, Leonardi V, Sereni A, Abbate R, et al. Red blood cell transfusions can induce proinflammatory cytokines in preterm infants. Transfusion. 2017;57:1304–10.
Erdöl H, Hacioglu D, Kola M, Turk A, Aslan Y. Investigation of the effect of hemoglobin F and A levels on development of retinopathy of prematurity. J AAPOS. 2017;21:136–40.
Torrejon-Rodriguez L, Pinilla-Gonzalez A, Lara Cantón I, Albiach-Delgado A, Cascant-Vilaplana MM, Cernada M, et al. Effect of autologous umbilical cord blood transfusion in the development of retinopathy of prematurity: randomized clinical trial—study protocol. Front Pediatr. 2023;11:1269797.
Christensen RD, Bahr TM, Davenport P, Sola-Visner MC, Ohls RK, Ilstrup SJ, et al. Implementing evidence-based restrictive neonatal intensive care unit platelet transfusion guidelines. J Perinatol. 2024;44:1394–401.
Bahr TM, Christensen TR, Ilstrup SJ, Ohls RK, Christensen RD. Term umbilical cord blood, fully tested and processed, as the source of red blood cell transfusions for extremely-low-gestational age neonates. Semin Fetal Neo Med. 2024;30:101545. https://doi.org/10.1016/j.siny.2024.101545.
Surbek DV, Visca E, Steinmann C, Tichelli A, Schatt S, Hahn S, et al. Umbilical cord blood collection before placental delivery during cesarean delivery increased cord blood volume and nucleated cell number available for transplantation. Am J Obstet Gynecol. 2000;183:218–21.
WHO. Guideline: delayed umbilical cord clamping for improved maternal and infant health and nutrition outcomes. Geneva: World Health Organization; 2014.
Acknowledgments
The authors thank Lindsay Carlton and Stacy Breeze of the Intermountain Health Women and Newborns Research Department for their work on the survey and for Institutional Review Board communications. We also thank Dr. Luciana Teofili, Transfusion Medicine, Fondazione Policlinico Universitario A. Gemelli–Università Cattolica del Sacro Cuore, Rome, Italy, for helpful discussions.
Author information
Authors and Affiliations
Contributions
TMB, RKO, TRC, and RDC; conception and design, assembly of data, data analysis, manuscript writing, final approval of the manuscript. JMP, MCM, HAD, JCE, and SJI; conception and design and final approval of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bahr, T.M., Ohls, R.K., Christensen, T.R. et al. Three studies needed to inform the design of the U-BET (umbilical cord blood for extremely low-gestational-age transfusions) clinical trial. J Perinatol 46, 55–60 (2026). https://doi.org/10.1038/s41372-025-02345-7
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41372-025-02345-7