Abstract
Objective
To compare resting energy expenditure (REE) among premature infants exposed to recorded maternal heartbeat and voice (MHV) vs. ambient noise.
Study design
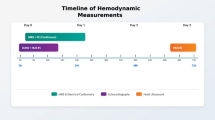
A prospective, randomized crossover pilot trial evaluating the effect of MHV on REE using indirect calorimetry in hemodynamically stable premature infants born at 26–34 weeks’ gestation. MHV recordings were digitally overlapped, and exposure sequence was randomized.
Result
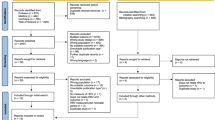
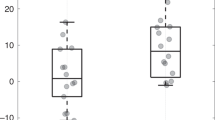
Among 34 measurements from seventeen subjects, REE was significantly lower during MHV exposure compared to ambient noise (61.4 ± 10.3 vs. 70.9 ± 10.3 kcal/kg/day, p = 0.0001). Mean heart rate was also significantly lower with MHV (144 ± 13 vs. 150 ± 11 bpm, p = 0.028), with no differences in other vital signs.
Conclusion
REE of premature infants decreased during exposure to MHV when compared with ambient noise. MHV may serve as a potential noninvasive therapeutic intervention to improve metabolic efficiency in premature infants, potentially helping with improved growth.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Hepper PG, Shahidullah BS. Development of fetal hearing. Arch Dis Child Fetal Neonatal Ed. 1994;71:F81–7.
Noise: a hazard for the fetus and newborn. American Academy of Pediatrics. Committee on Environmental Health. Pediatrics. 1997;100:724–7.
Pineda R, Guth R, Herring A, Reynolds L, Oberle S, Smith J. Enhancing sensory experiences for very preterm infants in the NICU: an integrative review. J Perinatol. 2017;37:323–32.
Brandon DH, Holditch-Davis D, Belyea M. Preterm infants born at less than 31 weeks’ gestation have improved growth in cycled light compared with continuous near darkness. J Pediatr. 2002;140:192–9.
Morag I, Xiao YT, Bruschettini M. Cycled light in the intensive care unit for preterm and low birth weight infants. Cochrane Database Syst Rev. 2024;12:CD006982.
Vasquez-Ruiz S, Maya-Barrios JA, Torres-Narvaez P, Vega-Martinez BR, Rojas-Granados A, Escobar C, et al. A light/dark cycle in the NICU accelerates body weight gain and shortens time to discharge in preterm infants. Early Hum Dev. 2014;90:535–40.
Feldman R, Rosenthal Z, Eidelman AI. Maternal-preterm skin-to-skin contact enhances child physiologic organization and cognitive control across the first 10 years of life. Biol Psychiatry. 2014;75:56–64.
Parga JJ, Bhatt RR, Kesavan K, Sim MS, Karp HN, Harper RM, et al. A prospective observational cohort study of exposure to womb-like sounds to stabilize breathing and cardiovascular patterns in preterm neonates. J Matern Fetal Neonatal Med. 2018;31:2245–51.
Webb AR, Heller HT, Benson CB, Lahav A. Mother’s voice and heartbeat sounds elicit auditory plasticity in the human brain before full gestation. Proc Natl Acad Sci USA. 2015;112:3152–7.
Loewy J, Stewart K, Dassler AM, Telsey A, Homel P. The effects of music therapy on vital signs, feeding, and sleep in premature infants. Pediatrics. 2013;131:902–18.
Rand K, Lahav A. Maternal sounds elicit lower heart rate in preterm newborns in the first month of life. Early Hum Dev. 2014;90:679–83.
Scala M, Seo S, Lee-Park J, McClure C, Scala M, Palafoutas JJ, et al. Effect of reading to preterm infants on measures of cardiorespiratory stability in the neonatal intensive care unit. J Perinatol. 2018;38:1536–41.
Provenzi L, Broso S, Montirosso R. Do mothers sound good? A systematic review of the effects of maternal voice exposure on preterm infants’ development. Neurosci Biobehav Rev. 2018;88:42–50.
Zimmerman E, Keunen K, Norton M, Lahav A. Weight gain velocity in very low-birth-weight infants: effects of exposure to biological maternal sounds. Am J Perinatol. 2013;30:863–70.
Lubetzky R, Mimouni FB, Dollberg S, Reifen R, Ashbel G, Mandel D. Effect of music by Mozart on energy expenditure in growing preterm infants. Pediatrics. 2010;125:e24–8.
Birnholz JC, Benacerraf BR. The development of human fetal hearing. Science. 1983;222:516–8.
Lim R, Brichta AM. Anatomical and physiological development of the human inner ear. Hear Res. 2016;338:9–21.
Pujol R, Hilding D. Anatomy and physiology of the onset of auditory function. Acta Otolaryngol. 1973;76:1–10.
Querleu D, Renard X, Versyp F, Paris-Delrue L, Crepin G. Fetal hearing. Eur J Obstet Gynecol Reprod Biol. 1988;28:191–212.
Sohmer H, Perez R, Sichel JY, Priner R, Freeman S. The pathway enabling external sounds to reach and excite the fetal inner ear. Audiol Neurootol. 2001;6:109–16.
Starr A, Amlie RN, Martin WH, Sanders S. Development of auditory function in newborn infants revealed by auditory brainstem potentials. Pediatrics. 1977;60:831–9.
da Rocha EE, Alves VG, da Fonseca RB. Indirect calorimetry: methodology, instruments and clinical application. Curr Opin Clin Nutr Metab Care. 2006;9:247–56.
Verma S, Bailey SM, Mally PV, Howell HB. Longitudinal measurements of resting energy expenditure by indirect calorimetry in healthy term infants during the first 2 months of life. Am J Perinatol. 2019;36:918–23.
Freymond D, Schutz Y, Decombaz J, Micheli JL, Jequier E. Energy balance, physical activity, and thermogenic effect of feeding in premature infants. Pediatr Res. 1986;20:638–45.
Hulzebos CV, Sauer PJ. Energy requirements. Semin Fetal Neonatal Med. 2007;12:2–10.
Mehta NM, Bechard LJ, Dolan M, Ariagno K, Jiang H, Duggan C. Energy imbalance and the risk of overfeeding in critically ill children. Pediatr Crit Care Med. 2011;12:398–405.
Singer P, Singer J. Clinical guide for the use of metabolic carts: indirect calorimetry-no longer the orphan of energy estimation. Nutr Clin Pract. 2016;31:30–8.
Sion-Sarid R, Cohen J, Houri Z, Singer P. Indirect calorimetry: a guide for optimizing nutritional support in the critically ill child. Nutrition. 2013;29:1094–9.
McClave SA, Taylor BE, Martindale RG, Warren MM, Johnson DR, Braunschweig C, et al. Guidelines for the provision and assessment of nutrition support therapy in the adult critically Ill patient: Society of Critical Care Medicine (SCCM) and American Society for Parenteral and Enteral Nutrition (A.S.P.E.N. JPEN J Parenter Enter Nutr. 2016;40:159–211.
Howell HB, Farkouh-Karoleski C, Weindler M, Sahni R. Resting energy expenditure in infants with congenital diaphragmatic hernia without respiratory support at time of neonatal hospital discharge. J Pediatr Surg. 2018;53:2100–4.
Moreira ME, Vieira AA, Mendes Soares FV, Bastos Lopes R, Gomes P, Abranches AD, et al. Determining the least time required for measuring energy expenditure in premature neonates. J Perinat Med. 2007;35:71–5.
Soares FV, Moreira ME, Abranches AD, Ramos JR, Gomes Junior SC. Indirect calorimetry: a tool to adjust energy expenditure in very low birth weight infants. J Pediatr. 2007;83:567–0.
Summer SS, Pratt JM, Koch EA, Anderson JB. Testing a novel method for measuring sleeping metabolic rate in neonates. Respir Care. 2014;59:1095–100.
Sohmer H, Freeman S. The pathway for the transmission of external sounds into the fetal inner ear. J Basic Clin Physiol Pharmacol. 2001;12:91–9.
Das R, Jana N, Arora N, Sengupta S. Ultrasound assessment of fetal hearing response to vibroacoustic stimulation. J Matern Fetal Neonatal Med. 2020;33:2326–32.
Lee GY, Kisilevsky BS. Fetuses respond to father’s voice but prefer mother’s voice after birth. Dev Psychobiol. 2014;56:1–11.
Ockleford EM, Vince MA, Layton C, Reader MR. Responses of neonates to parents’ and others’ voices. Early Hum Dev. 1988;18:27–36.
Kent WD, Tan AK, Clarke MC, Bardell T. Excessive noise levels in the neonatal ICU: potential effects on auditory system development. J Otolaryngol. 2002;31:355–60.
Filippa M, Devouche E, Arioni C, Imberty M, Gratier M. Live maternal speech and singing have beneficial effects on hospitalized preterm infants. Acta Paediatr. 2013;102:1017–20.
Filippa M, Monaci MG, Spagnuolo C, Serravalle P, Daniele R, Grandjean D. Maternal speech decreases pain scores and increases oxytocin levels in preterm infants during painful procedures. Sci Rep. 2021;11:17301.
Malchaire J, d, Palella AAFR BI. Evaluation of the metabolic rate based on the recording of the heart rate. Ind Health. 2017;55:219–32.
Cooper L, Morrill A, Russell RB, Gooding JS, Miller L, Berns SD. Close to me: enhancing kangaroo care practice for NICU staff and parents. Adv Neonatal Care. 2014;14:410–23.
Lemmen D, Fristedt P, Lundqvist A. Kangaroo care in a neonatal context: parents’ experiences of information and communication of nurse-parents. Open Nurs J. 2013;7:41–8.
Pathak BG, Sinha B, Sharma N, Mazumder S, Bhandari N. Effects of kangaroo mother care on maternal and paternal health: systematic review and meta-analysis. Bull World Health Organ. 2023;101:391–402G.
Cooper JA, Watras AC, O’Brien MJ, Luke A, Dobratz JR, Earthman CP, et al. Assessing validity and reliability of resting metabolic rate in six gas analysis systems. J Am Diet Assoc. 2009;109:128–32.
Crouter SE, Antczak A, Hudak JR, DellaValle DM, Haas JD. Accuracy and reliability of the ParvoMedics TrueOne 2400 and MedGraphics VO2000 metabolic systems. Eur J Appl Physiol. 2006;98:139–51.
Acknowledgements
We would like to thank all the patients and their families for participating in this study. Additionally, we would like to thank Dr. Jonathan Lebowitz for his contribution.
Funding
The Stefan Bennett Fellowship Research Fund in Neonatology and KiDS of NYU provided funding for this study.
Author information
Authors and Affiliations
Contributions
GK, SS, ES, HH, and SV conceptualized and designed the study, collected data, coordinated and supervised data collection, carried out analysis, drafted the initial manuscript, and reviewed and revised the manuscript. SB, BK, RS and PM conceptualized and designed the study, designed the data collection instruments, and critically reviewed and revised the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kaur, G., Bailey, S.M., Schneider, S. et al. A prospective randomized crossover trial studying the effects of maternal heartbeat and voice sounds on resting energy expenditure in preterm infants. J Perinatol 46, 410–415 (2026). https://doi.org/10.1038/s41372-025-02453-4
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41372-025-02453-4