Abstract
Objective
To evaluate the effectiveness of implementing American Academy of Pediatrics (AAP) discharge guidelines in reducing unplanned hospital readmissions within 30 days post-discharge among term ansd late preterm newborns.
Study design
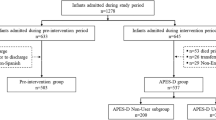
Retrospective observational study analyzing unplanned readmissions at a single-center neonatal unit from January 1, 2021, to December 31, 2024. Data were compared before (January 1, 2021–June 30, 2022) and after (July 1, 2022–December 31, 2024) guideline implementation, with subgroup analysis for the period after addition of structured support (July 1, 2023–December 31, 2024).
Result
AAP guideline implementation was associated with a statistically significant reduction in unplanned readmission rates among term infants (0.66% vs. 0.33%; P = 0.008). No reduction was evident among late preterm infants. Subgroup analysis showed further reductions post-structured support addition, though confounding by provider changes limits attribution.
Conclusion
The adoption of the AAP discharge guidelines, along with a structured process of mother and infant readiness, significantly decreassed unplanned readmission rates among term newborns.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
American Academy of Pediatrics Committee on Fetus and Newborn. Guidelines for Perinatal Care. 8th ed. Elk Grove Village, IL: American Academy of Pediatrics; 2017:392-402. Care of the Newborn: Hospital Discharge and Parent Education—Discharge of Healthy Newborn Infants.
American Academy of Pediatrics Committee on Fetus and Newborn. Hospital discharge of the high-risk neonate. Pediatrics. 2008;122:1119–26.
Smith VC, Hwang SS, Dukhovny D, Young S, Pursley DM. Neonatal intensive care unit discharge preparation, family readiness, and infant outcomes: connecting the dots. J Perinatol. 2013;33:415–21.
Jones E, Taylor B, MacArthur C, Bradshaw S, Hope L, Cummins C. Early postnatal discharge for infants: a meta-analysis. Pediatrics. 2020;146:e20193365. https://doi.org/10.1542/peds2019-3365.
Danielsen B, Castles AG, Damberg CL, Gould JB. Newborn discharge timing and readmissions: California,1992-1995. Pediatrics. 2000;106:31–9. https://doi.org/10.1542/peds.106.1.31.
Della P, Kern J, Kortsmit K, Barfield WD. Risk factors associated with 31-day unplanned hospital re-admission in newborns: a systematic review. Eur J Pediatr. 2023;182:1469–82.
Carter A, Gardner SL, Merenstein GB, Lubchenco LO Discharge planning and follow-up of the neonatal intensive care infant. In: Gardner SL, Carter BS, Enzman-Hines M, Hernandez JA, eds. Handbook of Neonatal Intensive Care. 9th ed. St. Louis, MO: Mosby/Elsevier; 2020:TBD.
Bourque SL, Machut KZ, Chuo J, Cohen S, Johnson YR, Nanda SH, et al. Children’s Hospitals Neonatal Consortium Transitions of Care and Follow-up Focus Group. Discharge Best Practices of High-Risk Infants from Regional Children’s Hospital NICUs. Hosp Pediatr. 2023;13:716–24. https://doi.org/10.1542/hpeds.2022-007063.
Kemper AR, Newman TB, Slaughter JL, Maisels MJ, Watchko JF, Downs SM, et al. Clinical practice guideline revision: management of hyperbilirubinemia in the newborn infant 35 or more weeks of gestation. Pediatrics. 2022;150:e2022058859. https://doi.org/10.1542/peds.2022-058859.
Benitz WE. Committee on Fetus and Newborn, American Academy of Pediatrics. Hospital stay for healthy term newborn infants. Pediatrics. 2015;135:948–53. https://doi.org/10.1542/peds.2015-0699.
Young PC, Korgenski K, Buchi KF. Early readmission of newborns in a large health care system. Pediatrics. 2013;131:e1538–44. https://doi.org/10.1542/peds.2012-2634.
Joyner JA, Papermaster AE, Champion JD. Characteristics of late preterm infant readmissions: A systematic review. J Am Assoc Nurse Pr. 2024;36:329–33. https://doi.org/10.1097/JXX.0000000000000986.
Amsalu R, Oltman SP, Baer RJ, Medvedev MM, Rogers EE, Jelliffe-Pawlowski L. Incidence, risk factors, and reasons for 30-day hospital readmission among healthy late preterm infants. Hosp Pediatr. 2022;12:639–49. https://doi.org/10.1542/hpeds.2021-006215.
Tomasini DK, Guindon MG, Vereen RJ, Drumm CM, Ponnapakkam AP. Readmission Reduction for Hyperbilirubinemia in Infants ≥ 35 Weeks Estimated Gestational Age Using a Standardized Protocol. Jt Comm J Qual Patient Saf. 2023;49:613–9. https://doi.org/10.1016/j.jcjq.2023.07.002.
Xu C, Bao Y, He Y, Wu M, Zhu J. Risk factors for readmission for hyperbilirubinemia in neonates with ABO hemolytic disease: a single-center retrospective cohort study. J Matern Fetal Neonatal Med. 2023;36:2238106. https://doi.org/10.1080/14767058.2023.2238106.
Burgos AE, Schmitt SK, Stevenson DK, Phibbs CS. Readmission for neonatal jaundice in California, 1991-2000: trends and implications. Pediatrics. 2008;121:e864–9. https://doi.org/10.1542/peds.2007-1214. Erratum in: Pediatrics. 2008 Sep;122(3):690.
American Academy of Pediatrics. Safe & Healthy Beginnings: Assessment of Hyperbilirubinemia, Breastfeeding Support, Coordination of Care. Publisher: American Academy of Pediatrics, 2009. ISBN 10: 1581103298. ISBN 13: 9781581103298.
Grupp-Phelan J, Taylor JA, Liu LL, Davis RL. Early newborn hospital discharge and readmission for mild and severe jaundice. Arch Pediatr Adolesc Med. 1999;153:1283–8. https://doi.org/10.1001/archpedi153.12.1283.
Elsevier Patient Education. How to Keep Your Newborn Safe and Healthy (Easy to Read). Elsevier Inc.; June, 2025.
Moon RY, Carlin RF, Hand I. TASK FORCE ON SUDDEN INFANT DEATH SYNDROME AND THE COMMITTEE ON FETUS AND NEWBORN. Sleep-Related Infant Deaths: Updated 2022 Recommendations for Reducing Infant Deaths in the Sleep Environment. Pediatrics. 2022;150:e2022057990. https://doi.org/10.1542/peds.2022-057990.
Roisné J, Delattre M, Rousseau S, Bourlet A, Charkaluk ML. Newborn follow-up after discharge from the maternity unit: Compliance with national guidelines. Arch Pediatr. 2018;25:95–99. https://doi.org/10.1016/j.arcped.2017.12.011.
Milambo JPM, Cho K, Okwundu C, Olowoyeye A, Ndayisaba L, Chand S, et al. Newborn follow-up after discharge from a tertiary care hospital in the Western Cape region of South Africa: a prospective observational cohort study. Glob Health Res Policy. 2018;3:2. https://doi.org/10.1186/s41256-017-0057-4.
Pepper M, Campbell OMR, Woodd SL. Current approaches to following up women and newborns after discharge from childbirth facilities: a scoping review. Glob Health Sci Pr. 2024;12:e2300377 https://doi.org/10.9745/GHSP-D-23-00377.
Tomashek KM, Shapiro-Mendoza CK, Weiss J, Kotelchuck M, Barfield W, Evans S, et al. Early discharge among late preterm and term newborns and risk of neonatal morbidity. Semin Perinatol. 2006;30:61–8. https://doi.org/10.1053/j.semperi.2006.02.003.
Paul IM, Lehman EB, Hollenbeak CS, Maisels MJ. Preventable newborn readmissions since passage of the Newborns’ and Mothers’ Health Protection Act. Pediatrics. 2006;118:2349–58. https://doi.org/10.1542/peds.2006-2043.
Escobar GJ, Greene JD, Hulac P, Kincannon E, Bischoff K, Gardner MN, et al. Rehospitalisation after birth hospitalisation: patterns among infants of all gestations. Arch Dis Child. 2005;90:125–31. https://doi.org/10.1136/adc.2003.039974.
Watt S, Sword W, Krueger P. Longer postpartum hospitalization options-who stays, who leaves, what changes?. BMC Pregnancy Childbirth. 2005;5:13. https://doi.org/10.1186/1471-2393-5-13.
Meara E, Kotagal UR, Atherton HD, Lieu TA. Impact of early newborn discharge legislation and early follow-up visits on infant outcomes in a state Medicaid population. Pediatrics. 2004;113:1619–27. https://doi.org/10.1542/peds.113.6.1619.
Kotagal UR, Atherton HD, Eshett R, Schoettker PJ, Perlstein PH. Safety of early discharge for Medicaid newborns. JAMA. 1999;282:1150–6. https://doi.org/10.1001/jama.282.12.1150.
Shakib J, Buchi K, Smith E, Korgenski K, Young PC. Timing of initial well-child visit and readmissions of newborns. Pediatrics. 2015;135:469–74. https://doi.org/10.1542/peds.2014-2329.
Nelson VR. The effect of newborn early discharge follow-up program on pediatric urgent care utilization. J Pediatr Health Care. 1999;13:58–61. https://doi.org/10.1016/S0891-5245(99)90054-8.
Kuzniewicz MW, Parker SJ, Schnake-Mahl A, Escobar GJ. Hospital readmissions and emergency department visits in moderate preterm, late preterm, and early term infants. Clin Perinatol. 2013;40:753–75. https://doi.org/10.1016/j.clp.2013.07.008.
Karnati S, Kollikonda S, Abu-Shaweesh J. Late preterm infants - Changing trends and continuing challenges. Int J Pediatr Adolesc Med. 2020;7:36–44. https://doi.org/10.1016/j.ijpam.2020.02.006.
Hamilton E, Dyachenko A, Ciampi A, et al. Estimating risk of severe neonatal morbidity in preterm births under 32 weeks of gestation. J Matern Fetal Neonatal Med. 2020;33:73–80. https://doi.org/10.1080/14767058.2018.1487395.
Underwood MA, Danielsen B, Gilbert WM. Costs, Causes, and Rates of Rehospitalization in Preterm Infants. J Perinatol. 2007;27:614–9. https://doi.org/10.1038/sj.jp.7211801.
Anderson JG, Rogers EE, Baer RJ, et al. Racial and ethnic disparities in preterm infant mortality and severe morbidity: a population-based study. Neonatology. 2018;113:44–54. https://doi.org/10.1159/000480536.
Bentz MG, Carmona N, Bhagwat MM, et al. Beyond “Asian”: specific East and Southeast Asian races or ethnicities associated with jaundice readmission. Hosp Pediatr. 2018;8:269–73. https://doi.org/10.1542/hpeds.2017-0234.
Jarrett O, Gim D, Puusepp-Benazzouz H, Liu A, Bhurawala H. Factors contributing to neonatal readmissions to a level 4 hospital within 28 days after birth. J Paediatr Child Health. 2022;58:1251–5. https://doi.org/10.1111/jpc.15970.
Karnati Harron K, Gilbert R, Cromwell D, Oddie S, van der Meulen J. Newborn Length of Stay and Risk of Readmission. Paediatr Perinat Epidemiol. 2017;31:221–32. https://doi.org/10.1111/ppe.12359.
Ekéus C, Högberg U, Norman M, et al. Vacuum-assisted birth and risk for cerebral complications in term newborn infants: a population-based cohort study. BMC Pregnancy Childbirth. 2014;14:36. https://doi.org/10.1186/1471-2393-14-36.
Sarik DA, Matsuda Y, Terrell EA, Sotolongo E, Hernandez M, Tena F, et al. A telehealth nursing intervention to improve the transition from the neonatal intensive care unit to home for infants & caregivers: Preliminary evaluation. J Pediatr Nurs. 2022;67:139–47. https://doi.org/10.1016/j.pedn.2022.09.003.
Acknowledgements
We thank the neonatologists, neonatal nurse practitioners, care managers, and healthcare outpatient schedulers at AdventHealth Celebration for their contributions to the implementation of the discharge guidelines.
Funding
No funding was secured for this study.
Author information
Authors and Affiliations
Contributions
JMLDR conceptualized the study, collected data, and drafted the initial manuscript; JP performed statistical analyses and revised the manuscript; WO supervised the study, interpreted data, and critically revised the manuscript. All authors approved the final manuscript as submitted.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
The AdventHealth Institutional Review Board approved this study. A waiver of parental consent was granted due to the retrospective nature of the research and the absence of direct interventions. The study was performed in accordance with the Declaration of Helsinki.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lopez Da Re, J.M., Pepe, J. & Oh, W. Implementation of the AAP discharge guidelines reduces unplanned readmissions of newborn infants: a single-center study. J Perinatol 46, 454–459 (2026). https://doi.org/10.1038/s41372-025-02485-w
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41372-025-02485-w