Abstract
Objective
The aim of this quality improvement project was to increase preoperative enteral feeding and breastfeeding rates in term neonates with congenital heart disease (CHD).
Methods
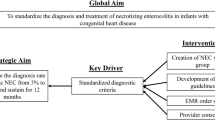
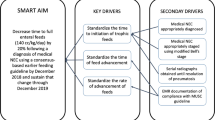
A multidisciplinary team developed and implemented a preoperative feeding protocol for neonates with congenital heart disease. The primary outcome was the presence of preoperative enteral feeding by May 2025. Secondary outcomes included breastfeeding rates and time to first feed. The process measure was the rate of reference to the feeding protocol in provider notes. Our balancing measure was a rule out or diagnosis of necrotizing enterocolitis requiring medical or surgical treatment in the preoperative period. Infants were identified using the Pediatric Cardiac Critical Care Collaborative (PC4). Data was collected from chart review and analyzed with statistical process control charts. The pre-implementation period was from June 2022 to June 2023, the implementation period was from July 2023 to June 2024, and the sustainment period was from July 2024 through May 2025.
Results
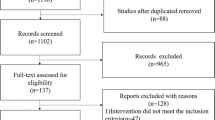
The number of neonates that met the inclusion criteria was 121. The rate of overall enteral feeding increased significantly from 72% in the pre-implementation phase (June 2022-June 2023) to 93% in the sustainment phase (July 2024–May 2025) (p = 0.026). Additionally, we found an improvement in our secondary outcomes and no change to the balancing measures.
Conclusion
This quality improvement initiative, which centered on creating and implementing a clear, standardized, evidence-based feeding protocol while utilizing interdisciplinary collaboration, led to an increase in overall rates of preoperative enteral feeding for newborns with CHD in a level IV intensive care nursery.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Marino LV, Johnson MJ, Davies NJ, Kidd CS, Fienberg J, Richens T, et al. Improving growth of infants with congenital heart disease using a consensus-based nutritional pathway. Clin Nutr. 2020;39:2455–62. https://doi.org/10.1016/j.clnu.2019.10.031.
Karpen HE. Nutrition in the cardiac newborns: evidence-based nutrition guidelines for cardiac newborns. Clin Perinatol. 2016;43:131–45. https://doi.org/10.1016/J.CLP.2015.11.009.
Ross F, Latham G, Joffe D, Richards M, Geiduschek J, Eisses M, et al. Preoperative malnutrition is associated with increased mortality and adverse outcomes after pediatric cardiac surgery. Cardiol Young-. 2017;27:1716–25.
Martini S, Beghetti I, Annunziata M, Aceti A, Galletti S, Ragni L, et al. Enteral nutrition in term infants with congenital heart disease: knowledge gaps and future directions to improve clinical practice. Nutrients. 2021;13:1–13. https://doi.org/10.3390/NU13030932.
Luca AC, Miron IC, Mîndru DE, Curpan AS, Stan RC, Tarca E, et al. Optimal nutrition parameters for neonates and infants with congenital heart disease. Nutrients. 2022;14. https://doi.org/10.3390/NU14081671.
Kelleher ST, McMahon CJ, James A. Necrotizing Enterocolitis in children with congenital heart disease: a literature review. Pediatr Cardiol. 2021;42:1688–99. https://doi.org/10.1007/S00246-021-02691-1.
O’Neal Maynord P, Johnson M, Xu M, Slaughter JC, Killen SA. A multi-interventional nutrition program for newborns with congenital heart disease. J Pediatr. 2021;228:66–73.e2. https://doi.org/10.1016/J.JPEDS.2020.08.039.
Chitale R, Ferguson K, Talej M, Yang WC, He S, Edmond KM, et al. Early enteral feeding for preterm or low birth weight infants: a systematic review and meta-analysis. Pediatrics. 2022;150:e2022057092E https://doi.org/10.1542/peds.2022-057092E.
Thoene M, Anderson-Berry A. Early enteral feeding in preterm infants: a narrative review of the nutritional, metabolic, and developmental benefits. Nutrients. 2021;13:2289 https://doi.org/10.3390/nu13072289.
Gao L, Shen W, Wu F, Liu L, Chang Y, Zhang R, et al. Effect of early initiation of enteral nutrition on short-term clinical outcomes of very premature infants: A national multicenter cohort study in China. Nutrition. 2023;107:111912. https://doi.org/10.1016/j.nut.2022.111912.
Bell D, Suna J, Marathe SP, Perumal G, Betts K, Venugopal P, et al. Feeding neonates and infants prior to surgery for congenital heart defects: systematic review and meta-analysis. Child. 2022;9. https://doi.org/10.3390/children9121856.
Penk J, Cagle W, Holloway A, Connolly J, Miles A, Bhakta R, et al. Multicenter evaluation of pre-operative feeding in infants with ductal dependent circulation. Pediatr Cardiol. 2024;45:1461–5. https://doi.org/10.1007/s00246-023-03182-1.
Cognata A, Kataria-Hale J, Griffiths P, Maskatia S, Rios D, O’Donnell A, et al. Human milk use in the preoperative period is associated with a lower risk for necrotizing Enterocolitis in neonates with complex congenital heart disease. J Pediatr. 2019;215:11–16.e2. https://doi.org/10.1016/j.jpeds.2019.08.009.
Elgersma KM, Wolfson J, Fulkerson JA, Georgieff MK, Looman WS, Spatz DL, et al. Human milk feeding and direct breastfeeding improve outcomes for infants with single ventricle congenital heart disease: propensity score-matched analysis of the NPC-QIC Registry. J Am Heart Assoc. 2023;12:e030756 https://doi.org/10.1161/JAHA.123.030756.
Jadcherla SR, Vijayapal AS, Leuthner S. Feeding abilities in neonates with congenital heart disease: a retrospective study. J Perinatol. 2009;29:112–8. https://doi.org/10.1038/jp.2008.136.
Slicker J, Sables-Baus S, Lambert LM, Peterson LE, Ocampo EC. Perioperative feeding approaches in single ventricle infants: a survey of 46 centers. Congenit Heart Dis. 2016;11:707–15. https://doi.org/10.1111/CHD.12390.
Tume LN, Balmaks R, Da Cruz E, Latten L, Verbruggen S, Valla FV. Enteral feeding practices in infants with congenital heart disease across European PICUs: A European Society of Pediatric and Neonatal Intensive Care Survey. Pediatr Crit Care Med. 2018;19:137–44. https://doi.org/10.1097/PCC.0000000000001412.
Furlong-Dillard J, Neary A, Marietta J, Jones C, Jeffers G, Gakenheimer L, et al. Evaluating the impact of a feeding protocol in neonates before and after biventricular cardiac surgery. Pediatr Qual Saf. 2018;3:e080 https://doi.org/10.1097/pq9.0000000000000080.
Lagerquist E, al-Haddad BJS, Irvine J, Muskthel L, Rios A, Upadhyay K. Feeding volume advancement in preterm neonates: A level 4 neonatal intensive care unit quality improvement initiative. Nut Clin Pr. 2023;38:1175–80. https://doi.org/10.1002/ncp.10992.
Tume LN, Valla FV, Joosten K, Jotterand Chaparro C, Latten L, Marino L, et al. Nutritional support for children during critical illness: European Society of Pediatric and Neonatal Intensive Care (ESPNIC) metabolism, endocrine and nutrition section position statement and clinical recommendations. Intensive Care Med. 2020;46:411–25. https://doi.org/10.1007/s00134-019-05922-5.
Slicker J, Hehir DA, Horsley M, Monczka J, Stern KW, Roman B, et al. Nutrition algorithms for infants with hypoplastic left heart syndrome; birth through the first interstage period. Congenit Heart Dis. 2013;8:89–102. https://doi.org/10.1111/j.1747-0803.2012.00705.x.
Neu J. Necrotizing Enterocolitis: the search for a unifying pathogenic theory leading to prevention. Pediatr Clin North Am. 1996;43:409–32.
Provost LP, Murray SK. The Health Care Data Guide: Learning from Data for Improvement, 1st ed. San Francisco, CA: Jossey-Bass; 2011.
Pappas LB, Erickson LA, Ricketts AM, Moehlmann ML, Hahn AM, Daniel JM. Pre-operative enteral feeding in single-ventricle CHD patients and necrotising enterocolitis risk. Cardiol Young-. 2024;34:364–9. https://doi.org/10.1017/S1047951123001580.
Elgersma KM, Spatz DL, Fulkerson JA, Wolfson J, Georgieff MK, Looman WS, et al. Patterns of breastfeeding and human milk feeding in infants with single-ventricle congenital heart disease: a population study of the National Pediatric Cardiology Quality Improvement Collaborative Registry. Breastfeed Med. 2023;18:315–25. https://doi.org/10.1089/bfm.2023.0036.
Baley J, Committee on Fetus and Newborn, Watterberg K, Cummings J, Eichenwald E, Poindexter B, et al. Skin-to-skin care for term and preterm infants in the neonatal ICU. Pediatrics. 2015;136:596–9. https://doi.org/10.1542/peds.2015-2335.
Acknowledgements
The authors would like to thank all clinical and administrative staff in the UCSF ICN for their dedication to give high quality care throughout the unit and for their contributions to this project.
Funding
No funding was secured for this study.
Author information
Authors and Affiliations
Contributions
PBB was responsible for study design, data collection, data analysis, figure creation, manuscript writing, and revision. KGG was involved in study design, data analysis, and manuscript revision. CM was involved in study design, intervention implementation, and manuscript revision. MH was involved in study design, intervention implementation as the primary dietitian in the unit, leading protocol teaching, and manuscript revision. KPP gave advice for study design, data collection, and analysis. She critically revised the manuscript. MAS oversaw study design, data collection, and analysis. She critically revised the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Brandfonbrener, P.B., Gorsky, K.G., Marks, C. et al. Improving preoperative enteral feeding for newborns with congenital heart disease. J Perinatol (2026). https://doi.org/10.1038/s41372-026-02606-z
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41372-026-02606-z