Abstract
Objective
This study examines annual trends and regional disparities in interventions and in-hospital outcomes for trisomies 18 and 13.
Study design
We conducted a retrospective cohort study using nationwide data from 2011 to 2022. Patients with trisomies 18 and 13 admitted on the day of birth were identified. Nonsurgical and surgical intervention rates, survival to discharge, length of stay, and costs were analyzed by year and region.
Result
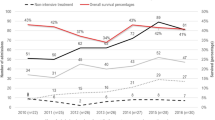
This study identified 2 245 neonates with trisomy 18 (n = 1 808) and trisomy 13 (n = 437). Nonsurgical and surgical intervention rates increased annually. Between 2011 and 2022, survival to discharge rates improved from 44.5 to 57.9%, and both hospital length of stay and costs nearly doubled. Regional disparities in survival to discharge rates were significant, with differences of up to 21.5%.
Conclusion
We observed an increase in interventions and a corresponding improvement in survival to discharge, with significant regional variations.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are not publicly available due to contractual agreements with the hospitals that provided the data for the database, which restrict public access to these datasets.
References
Stallings EB, Isenburg JL, Rutkowski RE, Kirby RS, Nembhard WN, Sandidge T, et al. National population-based estimates for major birth defects, 2016–2020. Birth Defects Res. 2024;116:e2301.
Rasmussen SA, Wong LY, Yang Q, May KM, Friedman JM. Population-based analyses of mortality in trisomy 13 and trisomy 18. Pediatrics. 2003;111:777–784.
Meyer RE, Liu G, Gilboa SM, Ethen MK, Aylsworth AS, Powell CM, et al. Survival of children with trisomy 13 and trisomy 18: a multi-state population-based study. Am J Med Genet A. 2016;170a:825–837.
Kato N, Morisaki N, Moriichi A. Trends in the survival of patients with trisomy 13 from 1995 to 2021: a population study in Japan. Am J Med Genet A. 2024;194:e63710.
Suto M, Isayama T, Morisaki N. Population-based analysis of secular trends in age at death in trisomy 18 syndrome in Japan from 1975 to 2016. Neonatology. 2021;118:47–53.
Nelson KE, Rosella LC, Mahant S, Guttmann A. Survival and surgical interventions for children with trisomy 13 and 18. JAMA. 2016;316:420–428.
Kosiv KA, Gossett JM, Bai S, Collins RT. Congenital heart surgery on in-hospital mortality in trisomy 13 and 18. Pediatrics. 2017;140:e20170772.
Haghnazarian E, Hu J, Song AY, Friedlich PS, Lakshmanan A. The association of Trisomy 13 and 18 and hospital discharge outcomes among neonates in California: A retrospective cohort study. Pediatr Neonatol. 2019;60:617–622.
Yasunaga H. Real world data in Japan: chapter II the diagnosis procedure combination database. Ann Clin Epidemiol. 2019;1:76–79.
Yamakawa K, Ohbe H, Hisamune R, Ushio N, Matsui H, Fushimi K, et al. Current clinical practice of laboratory testing of the hemostasis and coagulation system in patients with sepsis: a nationwide observational study in Japan. Jma j. 2024;7:224–231.
Yamana H, Moriwaki M, Horiguchi H, Kodan M, Fushimi K, Yasunaga H. Validity of diagnoses, procedures, and laboratory data in Japanese administrative data. J Epidemiol. 2017;27:476–482.
Acharya K, Leuthner SR, Zaniletti I, Niehaus JZ, Bishop CE, Coghill CH, et al. Medical and surgical interventions and outcomes for infants with trisomy 18 (T18) or trisomy 13 (T13) at children’s hospitals neonatal intensive care units (NICUs). J Perinatol. 2021;41:1745–1754.
St Louis JD, Bhat A, Carey JC, Lin AE, Mann PC, Smith LM, et al. The American Association for Thoracic Surgery (AATS) 2023 Expert Consensus Document: Recommendation for the care of children with trisomy 13 or trisomy 18 and a congenital heart defect. J Thorac Cardiovasc Surg. 2024;167:1519–1532.
Hafezi N, Jensen AR, Saenz ZM, Collings AT, Colgate CL, Inanc Salih ZN, et al. Surgical history and outcomes in trisomy 13 and 18: a thirty-year review. J Pediatr Surg. 2023;58:1512–1519.
Glinianaia SV, Rankin J, Tan J, Loane M, Garne E, Cavero-Carbonell C, et al. Ten-year survival of children with trisomy 13 or trisomy 18: a multi-registry European cohort study. Arch Dis Child. 2023;108:461–467.
Nishiyama M, Sekizawa A, Ogawa K, Sawai H, Nakamura H, Samura O, et al. Factors affecting parental decisions to terminate pregnancy in the presence of chromosome abnormalities: a Japanese multicenter study. Prenat Diagn. 2016;36:1121–1126.
Tamaki S, Iwatani S, Hagimoto S, Izumi A, Ikuta T, Takeoka E, et al. Impact of tracheostomies on the long-term survival of patients with trisomy 13 syndrome. Am J Med Genet A. 2023;191:2736–2742.
Ignatz-Hoover AO, Farghaly MAA, Crist A, Abdalla A, Aly H, Mohamed MA. Changes in hospital care of newborn infants with trisomy 13. Matern Child Health J. 2025;29:622–7.
Acknowledgements
We thank Ellen Daldoss from Edanz (https://jp.edanz.com/ac) for editing a draft of this manuscript.
Funding
This work was supported by the Ministry of Health, Labor and Welfare, Japan (grant numbers 23AA2003 and 22AA2003).
Author information
Authors and Affiliations
Contributions
SS, MI, AK, and KY conceived and designed the study. YS contributed to the study design and statistical methodology. HY, YK, and KF contributed to data acquisition and data curation. SS and YS performed the data analysis. SS wrote the first draft of the manuscript. MI, AK, YK, HY, HM, KF, KN, and KY critically revised the manuscript. KY supervised the study. All authors approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval and consent to participate
The study was approved by the Institutional Review Board of The University of Tokyo (approval number: 3501-(5) on 19 May 2021), and all methods were performed in accordance with the relevant guidelines and regulations. The requirement for informed consent was waived by the Institutional Review Board because all data were de-identified.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sugai, S., Sasabuchi, Y., Itsukaichi, M. et al. Annual trends and regional variations in medical interventions and survival to discharge for trisomies 18 and 13, 2011–2022: a nationwide inpatient database study. J Perinatol (2026). https://doi.org/10.1038/s41372-026-02610-3
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41372-026-02610-3