Abstract
Background
Infants with severe bronchopulmonary dysplasia (sBPD) progress through phases of illness. We created a longitudinal interdisciplinary assessment tool to track infant progress, then utilized it to evaluate the impact of tracheostomy.
Methods
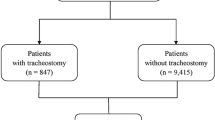
An iterative interview process with interprofessional experts was used to develop the tool for infants with grade 2/3 BPD. Qualitative coding determined common themes, which interviewees ranked by importance to develop the tool. We then retrospectively compared pairwise scores before and after tracheostomy placement.
Results
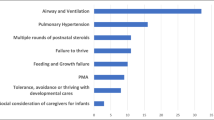
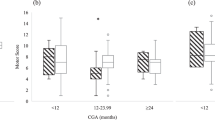
The assessment tool has twelve categories with items corresponding to four phases of illness. Total scores improved post tracheostomy, driven by significant improvements in systemic steroid, sedation, FiO2, weight, tolerance of cares, and developmental participation.
Conclusions
We present a user-friendly interdisciplinary scoring tool for sBPD to help providers and families align care goals and track longitudinal progress. Tracheostomy placement was associated with a change to less acute phases of sBPD.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
Clinical data used for this study is limited for availability due to protected health information, but de-identified summary data may be made available upon request.
References
Abman SH, Collaco JM, Shepherd EG, Keszler M, Cuevas-Guaman M, Welty SE, et al. Interdisciplinary care of children with severe bronchopulmonary dysplasia. J Pediatr. 2017;181:12–28.e1. https://doi.org/10.1016/j.jpeds.2016.10.082.
Stoll BJ, Hansen NI, Bell EF, Walsh MC, Carlo WA, Shankaran S, et al. Trends in care practices, morbidity, and mortality of extremely preterm neonates, 1993-2012. JAMA. 2015;314:1039 https://doi.org/10.1001/jama.2015.10244.
Jensen EA, Dysart K, Gantz MG, McDonald S, Bamat NA, Keszler M, et al. The diagnosis of bronchopulmonary dysplasia in very preterm infants. an evidence-based approach. Am J Respir Crit Care Med. 2019;200:751–9. https://doi.org/10.1164/rccm.201812-2348OC.
Jensen EA, Edwards EM, Greenberg LT, Soll RF, Ehret DEY, Horbar JD. Severity of bronchopulmonary dysplasia among very preterm infants in the United States. Pediatrics. 2021;148:e2020030007. https://doi.org/10.1542/peds.2020-030007.
Grover TR, Brozanski BS, Barry J, Zaniletti I, Asselin JM, Durand DJ, et al. High surgical burden for infants with severe chronic lung disease (sCLD). J Pediatr Surg. 2014;49:1202–5. https://doi.org/10.1016/j.jpedsurg.2014.02.087.
Vyas-Read S, Logan JW, Cuna AC, Machry J, Leeman KT, Rose RS, et al. A comparison of newer classifications of bronchopulmonary dysplasia: findings from the Children’s Hospitals Neonatal Consortium Severe BPD Group. J Perinatol. 2022;42:58–64. https://doi.org/10.1038/s41372-021-01178-4.
Murthy K, Porta NFM, Lagatta JM, Zaniletti I, Truog WE, Grover TR, et al. Inter-center variation in death or tracheostomy placement in infants with severe bronchopulmonary dysplasia. J Perinatol. 2017;37:723–7. https://doi.org/10.1038/jp.2016.277.
Shepherd EG, Knupp AM, Welty SE, Susey KM, Gardner WP, Gest AL. An interdisciplinary bronchopulmonary dysplasia program is associated with improved neurodevelopmental outcomes and fewer rehospitalizations. J Perinatol. 2012;32:33–8. https://doi.org/10.1038/jp.2011.45.
Logan JW, Lynch SK, Curtiss J, Shepherd EG. Clinical phenotypes and management concepts for severe, established bronchopulmonary dysplasia. Paediatr Respir Rev. 2019;31:58–63. https://doi.org/10.1016/j.prrv.2018.10.004.
Kielt MJ, Logan JW, Backes CH, Conroy S, Reber KM, Shepherd EG, et al. Noninvasive respiratory severity indices predict adverse outcomes in bronchopulmonary dysplasia. J Pediatr. 2022;242:129–36.e2. https://doi.org/10.1016/j.jpeds.2021.11.015.
Jung YH, Jang J, Kim H-S, Shin SH, Choi CW, Kim E-K, et al. Respiratory severity score as a predictive factor for severe bronchopulmonary dysplasia or death in extremely preterm infants. BMC Pediatr. 2019;19:121 https://doi.org/10.1186/s12887-019-1492-9.
Miller AN, Curtiss J, Taylor SN, Backes CH, Kielt MJ. A review and guide to nutritional care of the infant with established bronchopulmonary dysplasia. J Perinatol. 2023;43:402–10. https://doi.org/10.1038/s41372-022-01578-0.
Hanin M, Susey K, Beck C, Gest A, Shepherd E. Behavioral signs of respiratory instability: the development and administration of a scale to monitor signs of respiratory distress during developmental interventions in infants with bronchopulmonary dysplasia. Newborn Infant Nurs Rev. 2009;9:175–81. https://doi.org/10.1053/j.nainr.2009.06.004.
Susey K, Hanin M, Wortner A, Mandich M, Scott K, Stephenson K, et al. Validity and reliability of the behavioral signs of respiratory instability (BSRI) © scale during activity for infants with bronchopulmonary dysplasia. J Perinatol. 2023;43:1015–9. https://doi.org/10.1038/s41372-023-01682-9.
Gursoy T, Hayran M, Derin H, Ovali F. A clinical scoring system to predict the development of bronchopulmonary dysplasia. Amer J Perinatol. 2014;32:659–66. https://doi.org/10.1055/s-0034-1393935.
Yu Z, Wang L, Wang Y, Zhang M, Xu Y, Liu A. Development and validation of a risk scoring tool for bronchopulmonary dysplasia in preterm infants based on a systematic review and meta-analysis. Healthcare. 2023;11:778 https://doi.org/10.3390/healthcare11050778.
Donda K, Agyemang CO, Adjetey NA, Agyekum A, Princewill N, Ayensu M, et al. Tracheostomy trends in preterm infants with bronchopulmonary dysplasia in the United States: 2008-2017. Pediatr Pulmonol. 2021;56:1008–17. https://doi.org/10.1002/ppul.25273.
Yallapragada S, Savani RC, Mūnoz-Blanco S, Lagatta JM, Truog WE, Porta NFM, et al. Qualitative indications for tracheostomy and chronic mechanical ventilation in patients with severe bronchopulmonary dysplasia. J Perinatol. 2021;41:2651–7. https://doi.org/10.1038/s41372-021-01165-9.
Singer LT, Kercsmar C, Legris G, Orlowski JP, Hill BP, Doershuk C. Developmental sequelae of long-term infant tracheostomy. Dev Med Child Neurol. 1989;31:224–30. https://doi.org/10.1111/j.1469-8749.1989.tb03982.x.
Annesi CA, Levin JC, Litt JS, Sheils CA, Hayden LP. Long-term respiratory and developmental outcomes in children with bronchopulmonary dysplasia and history of tracheostomy. J Perinatol. 2021;41:2645–50. https://doi.org/10.1038/s41372-021-01144-0.
Luo J, Shepard S, Nilan K, Wood A, Monk HM, Jensen EA, et al. Improved growth and developmental activity post tracheostomy in preterm infants with severe BPD. Pediatr Pulmonol. 2018;53:1237–44. https://doi.org/10.1002/ppul.24087.
Mandy G, Malkar M, Welty SE, Brown R, Shepherd E, Gardner W, et al. Tracheostomy placement in infants with bronchopulmonary dysplasia: safety and outcomes. Pediatr Pulmonol. 2013;48:245–9. https://doi.org/10.1002/ppul.22572.
DeMauro SB, D’Agostino JA, Bann C, Bernbaum J, Gerdes M, Bell EF, et al. Developmental outcomes of very preterm infants with tracheostomies. J Pediatr. 2014;164:1303–10.e2. https://doi.org/10.1016/j.jpeds.2013.12.014.
Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006;3:77–101. https://doi.org/10.1191/1478088706qp063oa.
Author information
Authors and Affiliations
Contributions
Kara Mickas conceptualized and designed the study, collected data, carried out initial analysis, drafted the initial manuscript, and critically reviewed and revised the manuscript. Manisha Khakoo conceptualized and designed the study, collected data, carried out analysis, and critically reviewed and revised the manuscript. Drs Kristen Leeman and Jonathan Levin conceptualized and designed the study, coordinated and supervised data collection and data analysis, critically reviewed and revised the manuscript. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mickas, K.H., Khakoo, M.A., Leeman, K.T. et al. Development of an interdisciplinary tool to assess severe BPD phase of illness and application evaluating impact of tracheostomy. J Perinatol (2026). https://doi.org/10.1038/s41372-026-02620-1
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41372-026-02620-1