Abstract
Objective
Placement of a GT after a ventriculoperitoneal shunt (VPS) is a known risk factor for VPS infection, but the timing and sequence between procedures is poorly delineated in the neonatal population. The aims of this study were (1) determine the rate of meningitis in infants with a VPS and GT compared to VPS, (2) identify meningitis pathogens, and (3) define the optimal sequence and timing between placement of VPS and GT to minimize device-associated infections.
Study design
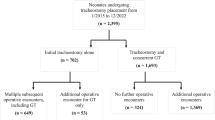
This retrospective cohort study includes infants with VPS placement from two level IV NICUs from January 1, 2010 to August 31, 2022. Infants with VPS placed for all causes of hydrocephalus were included. We compared infants with and without GTs, defined as gastrostomy or gastrojejunostomy tubes. The outcome of VPS-associated meningitis was defined by positive cerebral spinal fluid culture after VPS placement.
Result
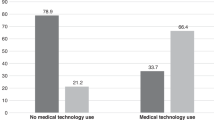
The incidence of VPS-associated meningitis in VPS and GT infants was 10.6% versus 3.4% in VPS only infants (p = 0.013, OR 0.3, 95% CI 0.12, 0.86). Pseudomonas species were the most common etiology of meningitis in VPS and GT infants while enterococcus was the most the common pathogen in VPS only cohort. In the subgroup of infants with VPS and GT, there was no statistical difference in rates of VPS-associated meningitis in those with VPS placed first and those with GT placed first.
Conclusion
In infants with hydrocephalus requiring VPS, GT placement was a risk factor for VPS-associated meningitis and may impact pathogenic cause of meningitis. Larger, multicenter cohorts may be helpful to determine optimal sequence and timing of VPS and GT placement in these high-risk infants.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
This data is not publicly available.
References
Sewell E, Roberts J, Mukhopadhyay S. Association of infection in neonates and long-term neurodevelopmental outcome. Clin Perinatol. 2021;48:251–61.
Sewell E, Cohen S, Zaniletti I, Couture D, Dereddy N, Coghill CH, et al. Surgical interventions and short-term outcomes for preterm infants with post-haemorrhagic hydrocephalus: a multicentre cohort study. Arch Dis Child Fetal Neonatal Ed. 2024;110:10–6.
Al-Holou WN, Wilson TJ, Ali ZS, Brennan RP, Bridges KJ, Guivatchian T, et al. Gastrostomy tube placement increases the risk of ventriculoperitoneal shunt infection: a multiinstitutional study. J Neurosurg. 2018;131:1062–67.
Gerges C, Wijesekera O, Herring E, Adesina A, Wright CH, Woodard J, et al. Evaluation of risk of gastrostomy and ventriculoperitoneal shunt placement in pediatric patients: a systematic review of the literature. World Neurosurg. 2021;152:180–8 e1.
Oterdoom LH, Marinus Oterdoom DL, Ket JCF, van Dijk JMC, Scholten P. Systematic review of ventricular peritoneal shunt and percutaneous endoscopic gastrostomy: a safe combination. J Neurosurg. 2017;127:899–904.
Tyler K, Leon SM, Lowe S, Kellogg R, Lena J, Privette AR, et al. Risk of ventriculoperitoneal shunt infection with coexisting percutaneous endoscopic gastrostomy tube and associated factors. Heliyon. 2020;6:e03523.
Alligood DM, Gilna GP, Huerta CT, Iglesias NJ, Parreco JP, Perez EA, et al. Assessing safety and timing of ventriculoperitoneal shunt and gastrostomy tube placement in newborns. J Pediatr Surg. 2025;60:162196.
Tunkel AR, Hasbun R, Bhimraj A, Byers K, Kaplan SL, Scheld WM, et al. 2017 Infectious Diseases Society of America’s clinical practice guidelines for healthcare-associated ventriculitis and meningitis. Clin Infect Dis. 2017;64:e34–e65.
Gassas A, Kennedy J, Green G, Connolly B, Cohen J, Dag-Ellams U, et al. Risk of ventriculoperitoneal shunt infections due to gastrostomy feeding tube insertion in pediatric patients with brain tumors. Pediatr Neurosurg. 2006;42:95–9.
Author information
Authors and Affiliations
Contributions
KL participated to the conceptualization, investigation, and writing of the original manuscript. AP contributed to the investigation and critical review of the final manuscript. ZH contributed to the formal analysis and critical review of the manuscript. BA contributed to the data curation and critical review of the manuscript. ES contributed to the conceptualization, investigation, and critical review of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval & consent to participate
The Children’s Healthcare of Atlanta IRB approved this study (STUDY00001524). A waiver of HIPAA authorization and informed consent was granted. This research involving human subjects, human material, or human data is in accordance with the Declaration of Helsinki.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Limpose, K.L., Piazza, A.J., He, Z. et al. Impact of gastrostomy tube placement on meningitis in infants with hydrocephalus requiring ventriculoperitoneal shunt. J Perinatol (2026). https://doi.org/10.1038/s41372-026-02625-w
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41372-026-02625-w