Abstract
Objective
To evaluate the efficacy and safety of Tumguide®, a radiation-free, transillumination-guided system for gastric tube (GT) placement in neonates.
Study design
This single-center prospective observational study enrolled neonates requiring GT placement. Tumguide® was used to guide placement. Primary outcomes were intragastric placement success rate and accuracy, defined as radiographically confirmed positioning not requiring adjustment.
Results
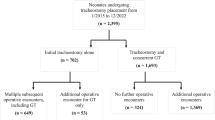
A total of 71 procedures were performed in 55 neonates. Median gestational age was 37.1 weeks, and median birth weight was 2480 g. The overall intragastric placement success rate was 99%, with 73% accuracy. No adverse events were reported. Protocol modifications significantly improved accuracy from 17% to 85% (p < 0.001). Tumguide® maintained high accuracy across varying body weights.
Conclusions
Tumguide® enables accurate and successful GT placement in neonates. Its real-time visualization and compatibility with small-caliber tubes support its utility as a practical alternative to traditional methods.
Clinical Trial Registration (if any)
This study was registered in the University Hospital Medical Information Network Clinical Trials Registry in Japan (ID: UMIN000055947, URL: https://center6.umin.ac.jp/cgi-open-bin/ctr_e/ctr_view.cgi?recptno=R000063917).
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
The datasets generated and analyzed during the current study are available from the corresponding author on reasonable request.
References
Lyman B, Kemper C, Northington L, Yaworski JA, Wilder K, Moore C, et al. Use of temporary enteral access devices in hospitalized neonatal and pediatric patients in the United States. JPEN J Parenter Enter Nutr. 2016;40:574–80.
Taylor SJ, Karpasiti T, Milne D. Safety of blind versus guided feeding tube placement: Misplacement and pneumothorax risk. Intensive Crit Care Nurs. 2023;76:103387.
NHS Improvement. Patient Safety Alert: nasogastric tube misplacement: continuing risk of death and severe harm. NHS/PSA/RE/2016/006. 2016.
Metheny NA, Meert KL, Clouse RE. Complications related to feeding tube placement. Curr Opin Gastroenterol. 2007;23:178–82.
Sinnathamby A, Low JM, Dale Lincoln Ser Keng L, Yvonne Peng Mei N. Watch your numbers! Avoiding gastric perforation from feeding tubes in neonates. Pediatr Neonatol. 2021;62:681–2.
Hanafy Eel- D, Ashebu SD, Naqeeb NA, Nanda HB. Pericardial sac perforation: a rare complication of neonatal nasogastric tube feeding. Pediatr Radio. 2006;36:1096–8.
Thames Valley & Wessex Neonatal Operational Delivery Network. Neonatal orogastric and nasogastric tube guideline (NGT feeding). Version 1. 2024.
Metheny NA, Krieger MM, Healey F, Meert KL. A review of guidelines to distinguish between gastric and pulmonary placement of nasogastric tubes. Heart Lung. 2019;48:226–35.
Cirgin Ellett ML, Cohen MD, Perkins SM, Smith CE, Lane KA, Austin JK. Predicting the insertion length for gastric tube placement in neonates. J Obstet Gynecol Neonatal Nurs. 2011;40:412–21.
Freeman D, Saxton V, Holberton J. A weight-based formula for the estimation of gastric tube insertion length in newborns. Adv Neonatal Care. 2012;12:179–82.
Irving SY, Rempel G, Lyman B, Servilla WMA, Northington L, Guenter. Pediatric nasogastric tube placement and verification: best practice recommendations from the NOVEL project. Nutr Clin Pr. 2018;33:921–7.
Gislason-Lee AJ. Patient X-ray exposure and ALARA in the neonatal intensive care unit: global patterns. Pediatr Neonatol. 2021;62:3–10.
Lin T, Gifford W, Lan Y, Qin X, Liu X, Wang J, et al. Diagnostic accuracy of ultrasonography for detecting nasogastric tube (NGT) placement in adults: a systematic review and meta analysis. Int J Nurs Stud. 2017;71:80–8.
Bear DE, Champion A, Lei K, Smith J, Beale R, Camporota L, et al. Use of an electromagnetic device compared with chest X-ray to confirm nasogastric feeding tube position in critical care. JPEN J Parenter Enter Nutr. 2016;40:581–6.
Taylor SJ, Milne D, Zeino Z, Griffiths L, Clemente R, Greer-Rogers F, et al. Validation of image interpretation for direct vision-guided feeding tube placement. Nutr Clin Pract. 2023;38:1360–7.
Shadid H, Keckeisen M, Zarrinpar A. Safety and efficacy of electromagnetic-guided bedside placement of nasoenteral feeding tubes versus standard placement. Am Surg. 2017;83:1184–7.
Taylor SJ, Milne D, Zeino Z, Griffiths L, Clemente R, Greer-Rogers F, et al. An externally validated guide to anatomical interpretation using a direct-vision (‘IRIS’) feeding tube. Clin Nutr ESPEN. 2024;60:356–61.
Hirano H, Masaki H, Kamada T, Taniguchi Y, Masaki E. Biologically transparent illumination is a safe, fast, and simple technique for detecting the correct position of the nasogastric tube in surgical patients under general anesthesia. PLoS One. 2021;16:e0250258.
Masaki H, Hirano H, Takahashi J, Kamada T, Masaki E. An improved biologically transparent illumination system that increases the accuracy of detecting the correct position of a nasogastric tube in the stomach. PLoS One. 2023;18:e0295415.
Satake R, Yamakawa H, Aoki N, Tanaka R, Yoshimoto S, Okunobo T, et al. A biologically transparent illumination device is more useful in children for detecting the position of the nasogastric tube in the stomach. Pediatr Surg Int. 2024;40:275.
Kuroda J, Okazaki K. Pilot study using an optical fiber light source to guide nasogastric/orogastric tube insertion in neonates. J Perinatol. 2023;43:1179–80.
Henderson RDE, Padash S, Adams SJ, Augusta C, Yi X, Babyn P. Neonatal catheter and tube placement and radiographic assessment statistics in relation to important anatomic landmarks. Am J Perinatol. 2024;41:e2299–e2306.
Dias FSB, Jales RM, Alvares BR, Caldas JPS, Carmona EV. Randomized clinical trial comparing two methods of measuring insertion length of nasogastric tubes in newborns. JPEN J Parenter Enter Nutr. 2020;44:912–9.
Manzo BF, Marcatto JO, Ferreria B, Galvão Diniz C, Parker LA. Comparison of 3 methods for measuring gastric tube length in newborns: a randomized clinical trial. Adv Neonatal Care. 2023;23:E79–E86.
Gulati IK, Jadcherla SR. Gastroesophageal reflux disease in the neonatal intensive care unit infant: who needs to be treated and what approach is beneficial?. Pediatr Clin North Am. 2019;66:461–73.
Nobile S, Marchionni P, Noviello C, Carnielli VP. Correlation between cardiorespiratory events and gastro-esophageal reflux in preterm and term infants: analysis of predisposing factors. Early Hum Dev. 2019;134:14–8.
Slocum C, Arko M, Di Fiore J, Martin RJ, Hibbs AM. Apnea, bradycardia and desaturation in preterm infants before and after feeding. J Perinatol. 2009;29:209–12.
Ellett ML, Cohen MD, Perkins SM, Croffie JM, Lane KA, Austin JK. Comparing methods of determining insertion length for placing gastric tubes in children 1 month to 17 years of age. J Spec Pediatr Nurs. 2012;17:19–32.
Nguyen S, Fang A, Saxton V, Holberton J. Accuracy of a weight-based formula for neonatal gastric tube insertion length. Adv Neonatal Care. 2016;16:158–61.
Ni M, Adam ME, Akbar F, Huddy JR, Borsci S, Buckle P, et al. Development and validation of ester impregnated pH strips for locating nasogastric feeding tubes in the stomach-a multicentre prospective diagnostic performance study. Diagn Progn Res. 2021;5:22.
Chen Y, Xu M, Cheng Y, Li S, Gao H, Kong S, et al. Confirming gastric tube placement in neurocritical patients using the combined effects of end-tidal CO2 and pH testing: a prospective diagnostic study. Intensive Crit Care Nurs. 2025;88:103922.
Chau JPC, Liu X, Choi KC, Lo SHS, Lam SKY, Chan KM, et al. Diagnostic accuracy of end-tidal carbon dioxide detection in determining correct placement of nasogastric tube: an updated systematic review with meta-analysis. Int J Nurs Stud. 2021;123:104071.
Torsy T, Saman R, Boeykens K, Duysburgh I, Van Damme N, Beeckman D. Comparison of two methods for estimating the tip position of a nasogastric feeding tube: a randomized controlled trial. Nutr Clin Pr. 2018;33:843–850.
McMullen CD, Anstey C, Garrett P, Moore J. Nasogastric tube placement under sonographic observation: a comparison study of ultrasound and chest radiography in mechanically ventilated patients. Aust Crit Care. 2022;35:181–5.
Dias FSB, Alvares BR, Jales RM, Franco APV, Silva JEFD, Fabene SMS, et al. The use of ultrasonography for verifying gastric tube placement in newborns. Adv Neonatal Care. 2019;19:219–25.
Hall EJ. Radiation biology for pediatric radiologists. Pediatr Radio. 2009;39:S57–S64.
Acknowledgements
The authors thank the nursing staff for their essential contributions to the successful completion of this study.
Funding
Partial funding for this study was provided by internal research grants from the International University of Health and Welfare. The funding source had no role in the design or conduct of the study.
Author information
Authors and Affiliations
Contributions
HS conceptualized and designed the study, oversaw the project, performed the procedures, analyzed the data, drafted the initial manuscript, and submitted the final manuscript. AY, MS, and KO contributed to clinical procedures and data collection. TM, DM, and YG assisted with manuscript preparation and critically reviewed and revised the text for significant intellectual content. JT served as advisor for the Tumguide® system. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
41372_2026_2643_MOESM2_ESM.pdf (download PDF )
Supplemental Figure 1. Radiographic confirmation of feeding tube tip position categories after the removal of the optical fiber
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shimozawa, H., Yamakami, A., Sagara, M. et al. Efficacy and accuracy of the transillumination-guided gastric tube placement in neonates. J Perinatol (2026). https://doi.org/10.1038/s41372-026-02643-8
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41372-026-02643-8