Abstract
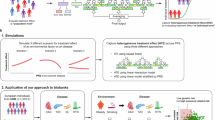
Patients with depression are at increased risk for a range of comorbid diseases, with, however, unclear explanations. In this large community-based cohort study of the UK Biobank, 24,130 patients diagnosed with depression were compared to 120,366 matched individuals without such a diagnosis. Follow-up was conducted from 6 months after the index date until death or the end of 2019, for the occurrence of 470 medical conditions and 16 specific causes of death. The median age at the time of the depression diagnosis was 62.0 years, and most of the patients were female (63.63%). During a median follow-up of 4.94 years, 129 medical conditions were found to be significantly associated with a prior diagnosis of depression, based on adjusted Cox regression models. Using disease trajectory network analysis to visualize the magnitude of disease–disease associations and the temporal order of the associated medical conditions, we identified three main affected disease clusters after depression (i.e., cardiometabolic diseases, chronic inflammatory diseases, and diseases related to tobacco abuse), which were further linked to a wider range of other conditions. In addition, we also identified three depression-mortality trajectories leading to death due to cardiovascular disease, respiratory system disease and malignant neoplasm. In conclusion, an inpatient diagnosis of depression in later life is associated with three distinct network-based clusters of medical conditions, indicating alterations in the cardiometabolic system, chronic status of inflammation, and tobacco abuse as key pathways to a wide range of other conditions downstream. If replicated, these pathways may constitute promising targets for the health promotion among depression patients.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
Data from the UK Biobank (http://www.ukbiobank.ac.uk/) are available to all researchers upon making an application. Part of this research was conducted using the UK Biobank Resource under Application 54803.
Code availability
All statistical analyses were conducted by the following software tools: Python v. 3.8, and Cytoscape Desktop v. 3.8.0. All codes associated with the current submission is available, and can be requested by contacting the corresponding authors.
References
Kessler RC, Bromet EJ. The epidemiology of depression across cultures. Annu Rev Public Health. 2013;34:119–38.
Bromet E, Andrade LH, Hwang I, Sampson NA, Alonso J, de Girolamo G, et al. Cross-national epidemiology of DSM-IV major depressive episode. BMC Med. 2011;9:90.
The global burden of disease: 2004 update. https://www.who.int/healthinfo/global_burden_disease/2004_report_update/en/, 2004, Accessed Date Accessed 2004.
WHO. Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet. 2018;392:1789–858.
Akula M, Kulikova A, Khan DA, Brown ES. The relationship between asthma and depression in a community-based sample. J Asthma. 2018;55:1271–7.
Alonso J, de Jonge P, Lim CC, Aguilar-Gaxiola S, Bruffaerts R, Caldas-de-Almeida JM, et al. Association between mental disorders and subsequent adult onset asthma. J Psychiatr Res. 2014;59:179–88.
de Jonge P, Alonso J, Stein DJ, Kiejna A, Aguilar-Gaxiola S, Viana MC, et al. Associations between DSM-IV mental disorders and diabetes mellitus: a role for impulse control disorders and depression. Diabetologia. 2014;57:699–709.
Wium-Andersen MK, Wium-Andersen IK, Jorgensen MB, McGue M, Jorgensen TSH, Christensen K, et al. The association between depressive mood and ischemic heart disease: a twin study. Acta Psychiatr Scand. 2019;140:265–74.
Wang S, Mao S, Xiang D, Fang C. Association between depression and the subsequent risk of Parkinson’s disease: a meta-analysis. Prog Neuropsychopharmacol Biol Psychiatry. 2018;86:186–92.
Kessing LV. Depression and the risk for dementia. Curr Opin Psychiatry. 2012;25:457–61.
Gao YH, Zhao HS, Zhang FR, Gao Y, Shen P, Chen RC, et al. The relationship between depression and asthma: a meta-analysis of prospective studies. PLoS One. 2015;10:e0132424.
Seligman F, Nemeroff CB. The interface of depression and cardiovascular disease: therapeutic implications. Ann N. Y Acad Sci. 2015;1345:25–35.
Mezuk B, Eaton WW, Albrecht S, Golden SH. Depression and type 2 diabetes over the lifespan: a meta-analysis. Diabetes Care. 2008;31:2383–90.
Momen NC, Plana-Ripoll O, Agerbo E, Benros ME, Borglum AD, Christensen MK, et al. Association between mental disorders and subsequent medical conditions. N. Engl J Med. 2020;382:1721–31.
Plana-Ripoll O, Pedersen CB, Agerbo E, Holtz Y, Erlangsen A, Canudas-Romo V, et al. A comprehensive analysis of mortality-related health metrics associated with mental disorders: a nationwide, register-based cohort study. Lancet. 2019;394:1827–35.
Plana-Ripoll O, Pedersen CB, Holtz Y, Benros ME, Dalsgaard S, de Jonge P, et al. Exploring comorbidity within mental disorders among a danish national population. JAMA Psychiatry. 2019;76:259–70.
Mulugeta A, Zhou A, King C, Hypponen E. Association between major depressive disorder and multiple disease outcomes: a phenome-wide Mendelian randomisation study in the UK Biobank. Mol Psychiatry. 2020;25:1469–76.
Tang B, Yuan S, Xiong Y, He Q, Larsson SC. Major depressive disorder and cardiometabolic diseases: a bidirectional Mendelian randomisation study. Diabetologia. 2020;63:1305–11.
Li GH, Cheung CL, Chung AK, Cheung BM, Wong IC, Fok MLY, et al. Evaluation of bi-directional causal association between depression and cardiovascular diseases: a Mendelian randomization study. Psychol Med. 2020: 1–12. [Epub ahead of print].
Jensen AB, Moseley PL, Oprea TI, Ellesoe SG, Eriksson R, Schmock H, et al. Temporal disease trajectories condensed from population-wide registry data covering 6.2 million patients. Nat Commun. 2014;5:4022.
Yang H, Pawitan Y, He W, Eriksson L, Holowko N, Hall P, et al. Disease trajectories and mortality among women diagnosed with breast cancer. Breast Cancer Res. 2019;21:95.
Siggaard T, Reguant R, Jorgensen IF, Haue AD, Lademann M, Aguayo-Orozco A, et al. Disease trajectory browser for exploring temporal, population-wide disease progression patterns in 7.2 million Danish patients. Nat Commun. 2020;11:4952.
Fry A, Littlejohns TJ, Sudlow C, Doherty N, Adamska L, Sprosen T, et al. Comparison of sociodemographic and health-related characteristics of UK Biobank participants with those of the general population. Am J Epidemiol. 2017;186:1026–34.
Sudlow C, Gallacher J, Allen N, Beral V, Burton P, Danesh J, et al. UK biobank: an open access resource for identifying the causes of a wide range of complex diseases of middle and old age. PLoS Med. 2015;12:e1001779.
Townsend P, Phillimore P, Beattie A. Health and deprivation: inequality and the North. London: Routledge; 1988.
Quan H, Sundararajan V, Halfon P, Fong A, Burnand B, Luthi JC, et al. Coding algorithms for defining comorbidities in ICD-9-CM and ICD-10 administrative data. Med Care. 2005;43:1130–9.
Chiolero A, Santschi V, Paccaud F. Public health surveillance with electronic medical records: at risk of surveillance bias and overdiagnosis. Eur J Public Health. 2013;23:350–1.
Salari N, Hosseinian-Far A, Jalali R, Vaisi-Raygani A, Rasoulpoor S, Mohammadi M, et al. Prevalence of stress, anxiety, depression among the general population during the COVID-19 pandemic: a systematic review and meta-analysis. Globalization health. 2020;16:1–11.
Davis KA, Sudlow CL, Hotopf M. Can mental health diagnoses in administrative data be used for research? A systematic review of the accuracy of routinely collected diagnoses. BMC Psychiatry. 2016;16:263.
Davis KAS, Bashford O, Jewell A, Shetty H, Stewart RJ, Sudlow CLM, et al. Using data linkage to electronic patient records to assess the validity of selected mental health diagnoses in English Hospital Episode Statistics (HES). PLoS ONE. 2018;13:e0195002.
Burns EM, Rigby E, Mamidanna R, Bottle A, Aylin P, Ziprin P, et al. Systematic review of discharge coding accuracy. J Public Health (Oxf). 2012;34:138–48.
International classification of diseases for mortality and morbidity statistics (10th Revision). https://www.who.int/classifications/icd/icdonlineversions/en/, 2019, Accessed Date Accessed 2019.
Smaardijk VR, Lodder P, Kop WJ, van Gennep B, Maas A, Mommersteeg PMC. Sex- and gender-stratified risks of psychological factors for incident ischemic heart disease: systematic review and meta-analysis. J Am Heart Assoc. 2019;8:e010859.
Swain NR, Lim CC, Levinson D, Fiestas F, de Girolamo G, Moskalewicz J, et al. Associations between DSM-IV mental disorders and subsequent non-fatal, self-reported stroke. J Psychosom Res. 2015;79:130–6.
Pan A, Keum N, Okereke OI, Sun Q, Kivimaki M, Rubin RR, et al. Bidirectional association between depression and metabolic syndrome: a systematic review and meta-analysis of epidemiological studies. Diabetes Care. 2012;35:1171–80.
Scott KM, de Jonge P, Alonso J, Viana MC, Liu Z, O’Neill S, et al. Associations between DSM-IV mental disorders and subsequent heart disease onset: beyond depression. Int J Cardiol. 2013;168:5293–9.
Martin DJ, Ul-Haq Z, Nicholl BI, Cullen B, Evans J, Gill JM, et al. Cardiometabolic disease and features of depression and bipolar disorder: population-based, cross-sectional study. Br J Psychiatry. 2016;208:343–51.
Miller AH, Maletic V, Raison CL. Inflammation and its discontents: the role of cytokines in the pathophysiology of major depression. Biol Psychiatry. 2009;65:732–41.
Heidt T, Sager HB, Courties G, Dutta P, Iwamoto Y, Zaltsman A, et al. Chronic variable stress activates hematopoietic stem cells. Nat Med. 2014;20:754–8.
Lanquillon S, Krieg JC, Bening-Abu-Shach U, Vedder H. Cytokine production and treatment response in major depressive disorder. Neuropsychopharmacology. 2000;22:370–9.
Kenis G, Maes M. Effects of antidepressants on the production of cytokines. Int J Neuropsychopharmacol. 2002;5:401–12.
Pollock BG, Laghrissi-Thode F, Wagner WR. Evaluation of platelet activation in depressed patients with ischemic heart disease after paroxetine or nortriptyline treatment. J Clin Psychopharmacol. 2000;20:137–40.
Musselman DL, Tomer A, Manatunga AK, Knight BT, Porter MR, Kasey S, et al. Exaggerated platelet reactivity in major depression. Am J Psychiatry. 1996;153:1313–7.
Kuijpers PMJC, Hamulyak K, Strik JJMH, Wellens HJJ, Honig A. Beta-thromboglobulin and platelet factor 4 levels in post-myocardial infarction patients with major depression. Psychiatry Res. 2002;109:207–10.
Kiecolt-Glaser JK, Derry HM, Fagundes CP. Inflammation: depression fans the flames and feasts on the heat. Am J Psychiatry. 2015;172:1075–91.
Boden JM, Fergusson DM. Alcohol and depression. Addiction. 2011;106:906–14.
Whooley MA, de Jonge P, Vittinghoff E, Otte C, Moos R, Carney RM, et al. Depressive symptoms, health behaviors, and risk of cardiovascular events in patients with coronary heart disease. JAMA. 2008;300:2379–88.
Weinberger AH, Kashan RS, Shpigel DM, Esan H, Taha F, Lee CJ, et al. Depression and cigarette smoking behavior: a critical review of population-based studies. Am J Drug Alcohol Abus. 2017;43:416–31.
Chaiton MO, Cohen JE, O’Loughlin J, Rehm J. A systematic review of longitudinal studies on the association between depression and smoking in adolescents. BMC Public Health. 2009;9:356.
Acknowledgements
We thank the team members and colleagues involved in West China Biomedical Big Data Center—UK Biobank project for their support.
Funding
This work is supported by the National Natural Science Foundation of China (No. 81971262 to HS), West China Hospital COVID-19 Epidemic Science and Technology Project (No. HX-2019-nCoV-014 to HS), Sichuan University Emergency Grant (No. 2020scunCoVyingji10002 to HS), EU Horizon2020 Research and Innovation Action Grant (847776 to UV and FF), Startup Fund for high-level talents of Fujian Medical University (XRCZX2020007 to HY), and Key Research and Development Program of Science and Technology Department of Sichuan Province (NO. 2019YFS0536 to LY).
Author information
Authors and Affiliations
Contributions
HS, HY, and FF were responsible for the study concept and design. ZY, HY, YS, LY, and YQ did the data and project management. XH, CH, HY, and WC did the data cleaning and analysis. XH, CH, HS, HY, and FF interpreted the data. XH, CH, FF, HY, and HS drafted the paper. All authors approved the final paper as submitted and agree to be accountable for all aspects of the work. The corresponding author attests that all listed authors meet authorship criteria and that no others meeting the criteria have been omitted.
Corresponding authors
Ethics declarations
Ethics approval
The UK Biobank has full ethical approval from the NHS National Research Ethics Service (reference number: 16/NW/0274), and this study was also approved by the biomedical research ethics committee of West China Hospital (reference number: 2019–1171).
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Han, X., Hou, C., Yang, H. et al. Disease trajectories and mortality among individuals diagnosed with depression: a community-based cohort study in UK Biobank. Mol Psychiatry 26, 6736–6746 (2021). https://doi.org/10.1038/s41380-021-01170-6
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41380-021-01170-6
This article is cited by
-
Depressive symptom trajectories and the association with diabetes and cardiovascular diseases in middle-aged and older Chinese adults: a cohort study
BMC Public Health (2026)
-
Associations of six dietary patterns with all-cause and cause-specific mortality among individuals with depression in the UK biobank: a prospective cohort study
European Journal of Nutrition (2026)
-
Disease trajectories and medical expenditures of older adults with disabilities: insights from China’s long-term care insurance program
BMC Geriatrics (2025)
-
Disease trajectory and mortality among sepsis patients: a prospective cohort study
BMC Infectious Diseases (2025)
-
Disease and mortality trajectories of cognitively able autistic individuals in mid- and later adulthood
BMC Medicine (2025)