Abstract
Background
Currently, studies on the lifetime prevalence of schizophrenia in the general population have not been updated or limited to a single country or region. The lifetime prevalence of schizophrenia may differ in other populations with certain relevant influencing factors or conditions. Globally, there is a lack of meta-analyses focusing on the lifetime prevalence of schizophrenia in specific populations. This study aims to determine the lifetime prevalence of schizophrenia in the general population, homeless populations, offenders, populations with comorbid mental disorders, populations with comorbid physical illnesses, populations at high genetic risk, populations exposed to stress, low-income populations, and indigenous populations, and to identify relevant factors.
Methods
Meta-analysis was used to estimate the combined lifetime prevalence of schizophrenia in the general population and eight other groups. To explore the sources of heterogeneity and identify factors associated with changes in prevalence, we conducted subgroup analyses of the general population, the homeless population, and the criminal population, examining geographic regions, sociodemographic factors, and methodological characteristics. Meta-regression in the general population examined the relationship between schizophrenia and mean age, publication year, and bias risk.
Results
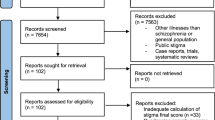
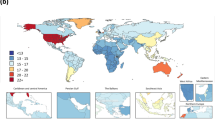
109 articles were included. Among them, 60 reported results from a sample of 20,910,871 individuals from the general population across 24 countries, 21 involved 6,605 individuals from the homeless population in 11 countries, there were 36 studies involving seven different population groups. The lifetime prevalence of schizophrenia is 0.62% (95% CI [0.51%–0.76%]) in the general population and 10.02% (95% CI [7.38%–13.47%]) in the homeless populations. Asia has the lowest lifetime prevalence of schizophrenia in both the general population and the homeless population, at 0.47% (95% CI [0.35%–0.64%]) and 4.68% (95% CI [2.11%–10.07%]).
Conclusions
Findings indicate that schizophrenia is more prevalent in special populations than in the general population. Understanding and addressing the risk factors contributing to elevated prevalence in vulnerable populations is essential for developing targeted prevention strategies and improving early intervention efforts.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author, Yuqiu Zhou, upon reasonable request.
References
Solmi M, Seitidis G, Mavridis D, Correll CU, Dragioti E, Guimond S, et al. Incidence, prevalence, and global burden of schizophrenia - data, with critical appraisal, from the Global Burden of Disease (GBD) 2019. Mol Psychiatry. 2023;28:5319–27.
Laursen TM, Nordentoft M, Mortensen PB. Excess early mortality in schizophrenia. Annu Rev Clin Psychol. 2014;10:425–48.
Cloutier M, Aigbogun MS, Guerin A, Nitulescu R, Ramanakumar AV, Kamat SA, et al. The economic burden of schizophrenia in the United States in 2013. J Clin Psychiatry. 2016;77:764–71.
Chong HY, Teoh SL, Wu DBC, Kotirum S, Chiou CF, Chaiyakunapruk N. Global economic burden of schizophrenia: A systematic review. Neuropsychiatr Dis Treat. 2016;12:357–73.
Thornicroft G Shunned: Discrimination against people with mental illness. Oxford University Press; 2006. 322 p.
Patel V, Chisholm D, Parikh R, Charlson FJ, Degenhardt L, Dua T, et al. Addressing the burden of mental, neurological, and substance use disorders: Key messages from Disease Control Priorities, 3rd edition. Lancet. 2016;387:1672–85.
Kessler RC, Angermeyer M, Anthony JC, DE Graaf R, Demyttenaere K, Gasquet I, et al. Lifetime prevalence and age-of-onset distributions of mental disorders in the World Health Organization’s World Mental Health Survey Initiative. World Psychiatry. 2007;6:168–76.
McGrath J, Saha S, Chant D, Welham J. Schizophrenia: A concise overview of incidence, prevalence, and mortality. Epidemiol Rev. 2008;30:67–76.
Saha S, Chant D, Welham J, McGrath J. A systematic review of the prevalence of schizophrenia. PLoS Med. 2005;2:e141.
Organization WH The ICD-10 Classification of Mental and Behavioural Disorders: Clinical Descriptions and Diagnostic Guidelines. World Health Organization; 1992. 377 p.
Regier DA, Narrow WE, Rae DS, Manderscheid RW, Locke BZ, Goodwin FK. The de facto US mental and addictive disorders service system. Epidemiologic catchment area prospective 1-year prevalence rates of disorders and services. Arch Gen Psychiatry. 1993;50:85–94.
Mueser KT, McGurk SR. Schizophrenia. The Lancet. 2004;363:2063–72.
Bhugra D. The global prevalence of schizophrenia. PLoS Med. 2005;2:e151. quiz e175
Pignon B, Schürhoff F, Baudin G, Tortelli A, Ferchiou A, Saba G, et al. Relationship between incidence and prevalence in psychotic disorders: An incidence–prevalence–mortality model. Int J Methods Psych Res. 2018;27:e1719.
Thara R, Kamath S. Women and schizophrenia. Indian J Psychiatry. 2015;57:S246–251.
Nowrouzi B, Kamhi R, Hu J, Kennedy JL, Matmari M, De Luca V. Age at onset mixture analysis and systematic comparison in schizophrenia spectrum disorders: Is the onset heterogeneity dependent on heterogeneous diagnosis? Schizophr Res. 2015;164:83–91.
McGrath JJ. Variations in the incidence of schizophrenia: Data versus dogma. Schizophr Bull. 2006;32:195–7.
de Salvia D, Barbato A, Salvo P, Zadro F. Prevalence and incidence of schizophrenic disorders in Portogruaro. An Italian case register study. J Nerv Ment Dis. 1993;181:275–82.
Luo Y, Pang L, Zhao Y, Guo C, Zhang L, Zheng X. Gender difference in the association between education and schizophrenia in Chinese adults. BMC Psychiatry. 2020;20:296.
Xiang YT, Ma X, Cai ZJ, Li SR, Xiang YQ, Guo HL, et al. Prevalence and socio-demographic correlates of schizophrenia in Beijing, China. Schizophr Res. 2008;102:270–7.
Hogerzeil SJ, Hoek HW, van Hemert AM. The impact of study design on schizophrenia incidence estimates: A systematic review of Northern European studies 2008-2019. Schizophr Res. 2021;231:134–41.
McGrath J, Saha S, Welham J, El Saadi O, MacCauley C, Chant D. A systematic review of the incidence of schizophrenia: The distribution of rates and the influence of sex, urbanicity, migrant status and methodology. BMC Med. 2004;2:13.
van Os J, Kenis G, Rutten BPF. The environment and schizophrenia. Nature. 2010;468:203–12.
Sullivan PF, Daly MJ, O’Donovan M. Genetic architectures of psychiatric disorders: The emerging picture and its implications. Nat Rev Genet. 2012;13:537–51.
Stilo SA, Murray RM. Non-Genetic factors in schizophrenia. Curr Psychiatry Rep. 2019;21:100.
Cho MJ, Kim JK, Jeon HJ, Suh T, Chung IW, Hong JP, et al. Lifetime and 12-Month prevalence of DSM-IV psychiatric disorders among Korean adults. J Nerv Ment Dis. 2007;195:203–10.
Cabassa LJ, Lewis-Fernández R, Wang S, Blanco C. Cardiovascular disease and psychiatric disorders among Latinos in the United States. Soc Psychiatry Psychiatr Epidemiol. 2017;52:837–46.
Krueger RF, Bezdjian S. Enhancing research and treatment of mental disorders with dimensional concepts: Toward DSM-V and ICD-11. World Psychiatry. 2009;8:3–6.
Charlson FJ, Ferrari AJ, Santomauro DF, Diminic S, Stockings E, Scott JG, et al. Global epidemiology and burden of schizophrenia: Findings from the global burden of disease study 2016. Schizophr Bull. 2018;44:1195–203.
Ayano G, Tesfaw G, Shumet S. The prevalence of schizophrenia and other psychotic disorders among homeless people: A systematic review and meta-analysis. BMC Psychiatry. 2019;19:370.
Swanson JW, Stenger M, Easter MM, Bareis N, Chwastiak L, Dixon LB, et al. Mental disorders and criminal legal involvement: Evidence from a national diagnostic epidemiological survey. PLOS Ment Health. 2025;2:e0000257.
GBD 2019 Mental Disorders Collaborators. Global, regional, and national burden of 12 mental disorders in 204 countries and territories, 1990-2019: A systematic analysis for the Global Burden of Disease Study 2019. Lancet Psychiatry. 2022;9:137–50.
Solmi M, Radua J, Olivola M, Croce E, Soardo L, Salazar de Pablo G, et al. Age at onset of mental disorders worldwide: Large-scale meta-analysis of 192 epidemiological studies. Mol Psychiatry. 2022;27:281–95.
Wainberg ML, Scorza P, Shultz JM, Helpman L, Mootz JJ, Johnson KA, et al. Challenges and opportunities in global mental health: A research-to-practice perspective. Curr Psychiatry Rep. 2017;19:28.
Gottesman II, Erlenmeyer-Kimling L. Family and twin strategies as a head start in defining prodromes and endophenotypes for hypothetical early-interventions in schizophrenia. Schizophr Res. 2001;51:93–102.
Armando M, Sandini C, Chambaz M, Schaer M, Schneider M, Eliez S. Coping strategies mediate the effect of stressful life events on schizotypal traits and psychotic symptoms in 22q11.2 deletion syndrome. Schizophr Bull. 2018;44:S525–35.
Werner S, Malaspina D, Rabinowitz J. Socioeconomic status at birth is associated with risk of schizophrenia: Population-based multilevel study. Schizophr Bull. 2007;33:1373–8.
Folsom D, Jeste DV. Schizophrenia in homeless persons: A systematic review of the literature. Acta Psychiatr Scand. 2002;105:404–13.
Khokhar JY, Dwiel LL, Henricks AM, Doucette WT, Green AI. The link between schizophrenia and substance use disorder: A unifying hypothesis. Schizophr Res. 2018;194:78–85.
Benros ME, Nielsen PR, Nordentoft M, Eaton WW, Dalton SO, Mortensen PB. Autoimmune diseases and severe infections as risk factors for schizophrenia: A 30-year population-based register study. Am J Psychiatry. 2011;168:1303–10.
Clancy MJ, Clarke MC, Connor DJ, Cannon M, Cotter DR. The prevalence of psychosis in epilepsy; a systematic review and meta-analysis. BMC Psychiatry. 2014;14:75.
Pillinger T, Beck K, Gobjila C, Donocik JG, Jauhar S, Howes OD. Impaired glucose homeostasis in first-episode schizophrenia: A systematic review and meta-analysis. JAMA Psychiatry. 2017;74:261–9.
Zabala-Baños MC, Segura A, Maestre-Miquel C, Martínez-Lorca M, Rodríguez-Martín B, Romero D, et al. Mental disorder prevalence and associated risk factors in three prisons of Spain. Rev Esp Sanid Penit. 2016;18:13–23.
Robin RW, Gottesman II, Albaugh B, Goldman D. Schizophrenia and psychotic symptoms in families of two american indian tribes. BMC Psychiatry. 2007;7:30.
McHugh ML. Interrater reliability: The kappa statistic. Biochem Med (Zagreb). 2012;22:276–82.
Lortie CJ Doing Meta-Analysis with R - A Hands-On Guide. J Stat Soft [Internet]. 2022 [cited 2024 July 12];102(Book Review 2). Available from: https://www.jstatsoft.org/v102/b02/
Higgins JPT, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327:557–60.
Rücker G, Schwarzer G. Beyond the forest plot: The drapery plot. Res Synth Methods. 2021 Jan;12:13–9.
Wells GA, Shea B, O’Connell D, Peterson J, Welch V, Losos M, et al. The newcastle-ottawa scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. 2000 [cited 2025 Nov 20]; Available from: https://scholar.archive.org/work/zuw33wskgzf4bceqgi7opslsre/access/wayback/www3.med.unipmn.it/dispense_ebm/2009-2010/Corso%20Perfezionamento%20EBM_Faggiano/NOS_oxford.pdf
Egger M, Davey Smith G, Schneider M, Minder C. Bias in meta-analysis detected by a simple, graphical test. BMJ. 1997;315:629–34.
Brown AS. The environment and susceptibility to schizophrenia. Prog Neurobiol. 2011;93:23–58.
Fazel S, Khosla V, Doll H, Geddes J. The prevalence of mental disorders among the homeless in western countries: Systematic review and meta-regression analysis. PLoS Med. 2008;5:e225.
Aldridge RW, Story A, Hwang SW, Nordentoft M, Luchenski SA, Hartwell G, et al. Morbidity and mortality in homeless individuals, prisoners, sex workers, and individuals with substance use disorders in high-income countries: A systematic review and meta-analysis. Lancet (Lond Engl). 2018;391:241–50.
Sullivan PF, Kendler KS, Neale MC. Schizophrenia as a complex trait: Evidence from a meta-analysis of twin studies. Arch Gen Psychiatry. 2003;60:1187–92.
Gottesman II, Laursen TM, Bertelsen A, Mortensen PB. Severe mental disorders in offspring with 2 psychiatrically ill parents. Arch Gen Psychiatry. 2010;67:252–7.
Davis J, Eyre H, Jacka FN, Dodd S, Dean O, McEwen S, et al. A review of vulnerability and risks for schizophrenia: Beyond the two hit hypothesis. Neurosci Biobehav Rev. 2016;65:185–94.
Kessler RC, Amminger GP, Aguilar-Gaxiola S, Alonso J, Lee S, Ustün TB. Age of onset of mental disorders: A review of recent literature. Curr Opin Psychiatry. 2007;20:359–64.
Burns JK, Tomita A, Kapadia AS. Income inequality and schizophrenia: Increased schizophrenia incidence in countries with high levels of income inequality. Int J Soc Psychiatry. 2014;60:185–96.
Woolway GE, Smart SE, Lynham AJ, Lloyd JL, Owen MJ, Jones IR, et al. Schizophrenia polygenic risk and experiences of childhood adversity: A systematic review and meta-analysis. Schizophr Bull. 2022;48:967–80.
Dawidowski B, Górniak A, Podwalski P, Lebiecka Z, Misiak B, Samochowiec J. The role of cytokines in the pathogenesis of schizophrenia. J Clin Med. 2021;10:3849.
Fiorillo A, Giordano A. The biopsychosocial model of schizophrenia and cancer: Unraveling the etiopathogenesis of complex diseases. Eur Psychiatry. 2022;65:e86.
Tsemberis S, Gulcur L, Nakae M. Housing First, consumer choice, and harm reduction for homeless individuals with a dual diagnosis. Am J Public Health. 2004;94:651–6.
Padgett DK, Stanhope V, Henwood BF, Stefancic A. Substance use outcomes among homeless clients with serious mental illness: Comparing Housing First with Treatment First programs. Community Ment Health J. 2011;47:227–32.
Drake RE, Bond GR IPS Support Employment: A 20-Year Update. American Journal of Psychiatric Rehabilitation [Internet]. 2011 July 1 [cited 2024 Sept 21]; Available from: https://www.tandfonline.com/doi/abs/10.1080/15487768.2011.598090
Seidman LJ, Nordentoft M. New targets for prevention of schizophrenia: Is it time for interventions in the premorbid phase? Schizophr Bull. 2015;41:795–800.
Simeone JC, Ward AJ, Rotella P, Collins J, Windisch R. An evaluation of variation in published estimates of schizophrenia prevalence from 1990─2013: A systematic literature review. BMC Psychiatry. 2015;15:193.
Moreno-Küstner B, Martín C, Pastor L. Prevalence of psychotic disorders and its association with methodological issues. A systematic review and meta-analyses. PLoS One. 2018;13:e0195687.
Fusar-Poli P, Borgwardt S, Bechdolf A, Addington J, Riecher-Rössler A, Schultze-Lutter F, et al. The psychosis high-risk state: A comprehensive state-of-the-art review. JAMA Psychiatry. 2013;70:107–20.
Budziszewska MD, Babiuch-Hall M, Wielebska K. Love and romantic relationships in the voices of patients who experience psychosis: An interpretive phenomenological analysis. Front Psychol. 2020;11:570928.
Tandon R, Nasrallah HA, Keshavan MS. Schizophrenia, ‘just the facts’ 4. Clinical features and conceptualization. Schizophr Res. 2009;110:1–23.
Regier DA, Narrow WE, Clarke DE, Kraemer HC, Kuramoto SJ, Kuhl EA, et al. DSM-5 field trials in the United States and Canada, Part II: Test-retest reliability of selected categorical diagnoses. Am J Psychiatry. 2013;170:59–70.
Sartorius N, Kaelber CT, Cooper JE, Roper MT, Rae DS, Gulbinat W, et al. Progress toward achieving a common language in psychiatry. Results from the field trial of the clinical guidelines accompanying the WHO classification of mental and behavioral disorders in ICD-10. Arch Gen Psychiatry. 1993;50:115–24.
Patel V, Prince M. Global mental health: A new global health field comes of age. JAMA. 2010;303:1976–7.
Kraemer HC. Validity and psychiatric diagnoses. JAMA Psychiatry. 2013;70:138–9.
Garson E, Castle DJ, George TP. Substance-Induced psychosis: A narrative review. Curr Addctn Rep. 2023;10:335–40.
Murrie B, Lappin J, Large M, Sara G. Transition of substance-induced, brief, and atypical psychoses to schizophrenia: A systematic review and meta-analysis. Schizophr Bull. 2020;46:505–16.
Martin MS, Hynes K, Hatcher S, Colman I. Diagnostic error in correctional mental health. J Correct Health Care. 2016;22:109–17.
Emilian C, Al-Juffali N, Fazel S. Prevalence of severe mental illness among people in prison across 43 countries: A systematic review and meta-analysis. Lancet, Public Health. 2025;10:e97–110.
Abdullah T, Brown TL. Mental illness stigma and ethnocultural beliefs, values, and norms: An integrative review. Clin Psychol Rev. 2011;31:934–48.
Schalbroeck R. The social defeat hypothesis of schizophrenia: A parsimonious explanation for multiple psychosis risk factors? Psychol Med. 2023;53:286–7.
Newbury JB, Arseneault L, Caspi A, Moffitt TE, Odgers CL, Belsky DW, et al. Association between genetic and socioenvironmental risk for schizophrenia during upbringing in a UK longitudinal cohort. Psychol Med. 2022;52:1527–37.
Chien WT, Thompson DR, Norman I. Evaluation of a peer-led mutual support group for Chinese families of people with schizophrenia. Am J Community Psychol. 2008;42:122–34.
Allison S, Bastiampillai T, Licinio J, Fuller DA, Bidargaddi N, Sharfstein SS. When should governments increase the supply of psychiatric beds? Mol Psychiatry. 2018;23:796–800.
GBD 2016 Alcohol and Drug Use Collaborators. The global burden of disease attributable to alcohol and drug use in 195 countries and territories, 1990–2016: A systematic analysis for the global burden of disease study 2016. Lancet, Psychiatry. 2018;5:987–1012.
Gao YN. Relationship between psychiatric inpatient beds and jail populations in the United States. J Psychiatr Pract. 2021;27:33–42.
World Health Organization. Depressive disorder (depression). 2025 [cited 2025 Sept 28]. Depressive disorder (depression). Available from: https://www.who.int/news-room/fact-sheets/detail/depression
Pignon B, Szöke A, Ku B, Melchior M, Schürhoff F. Urbanicity and psychotic disorders: Facts and hypotheses. Dialogues Clin Neurosci. 2023;25:122–38.
Funding
This study was supported by The Natural Science Foundation of China (72074063).
Author information
Authors and Affiliations
Contributions
Shuxin Zhang and Yuqiu Zhou take responsibility for the integrity of the data and the accuracy of the data analysis. Concept and design: Shuxin Zhang, Yubin Chen, Linghui Zhang, Xinyu Yang, Yang Feng, Yuqiu Zhou. Acquisition, analysis, or interpretation of data: Shuxin Zhang, Yubin Chen, Junhui Dong, Minle Lu, Na Zhou, Yang Feng, Yuqiu Zhou. Drafting of the manuscript: Shuxin Zhang, Yubin Chen, Linghui Zhang. Critical revision of the manuscript for important intellectual content: Shuxin Zhang, Yubin Chen, Linghui Zhang, Yang Feng, Yuqiu Zhou. Statistical analysis: Shuxin Zhang, Yubin Chen, Linghui Zhang, Yu Zhang, Yuqiu Zhou. Administrative, technical, or material support: Shuxin Zhang, Yubin Chen, Linghui Zhang, Xinyu Yang, Yang Feng, Yuqiu Zhou. Supervision: Yuqiu Zhou.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, S., Chen, Y., Zhang, L. et al. Global lifetime prevalence of schizophrenia: A systematic review and meta-analysis. Mol Psychiatry (2026). https://doi.org/10.1038/s41380-026-03533-3
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41380-026-03533-3