Abstract
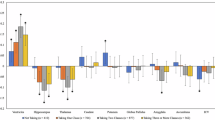
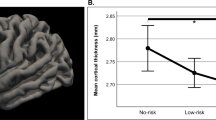
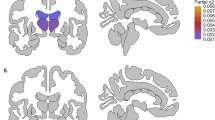
Recent research suggests that brain anatomy may help identify the most effective pharmacological treatment for each individual with bipolar disorder and reduce trial-and-error prescribing. We aimed to investigate whether brain anatomy predicts whether a medication is currently prescribed or has been discontinued, as a proxy for treatment effectiveness. The rationale is that medications that provide clinical benefit without unacceptable side effects are likely to be continued, whereas those with limited benefit or poor tolerability are typically discontinued. We used T1-weighted MRI from twelve ENIGMA-BD cohorts (n = 2462; 473 individuals with BD [61% female, age 18–73] and 1989 controls) to derive regional cortical thickness and surface area and subcortical volumes. Site differences were harmonized using ComBat models fitted on controls’ data. Within cross-validation, models were trained to first adjust for cumulative dose and other covariates and then predict medication status. On test sets, current prescription (vs. discontinuation) of lithium was predicted by greater cortical thickness and reduced surface area, whereas current prescription (vs. discontinuation) of antidepressants and atypical antipsychotics was predicted by greater cortical thickness. Predictive regions for atypical antipsychotics were generally consistent across subgroups of age, gender, illness duration, and history of psychosis, and in the largest site, and differed from those associated with cumulative effects of medication on the cortex. Predictions were poor for subcortical volumes and for antiepileptic mood stabilizers and typical antipsychotics. These findings provide preliminary support that cortical anatomy may help inform future development of biomarkers for treatment selection, pending validation in longitudinal studies.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Vieta E, Berk M, Schulze TG, Carvalho AF, Suppes T, Calabrese JR, et al. Bipolar disorders. Nat Rev Primer. 2018;4:1–16.
Samamé C, Martino DJ, Strejilevich SA. Longitudinal course of cognitive deficits in bipolar disorder: a meta-analytic study. J Affect Disord. 2014;164:130–8.
Crump C, Sundquist K, Winkleby MA, Sundquist J. Comorbidities and mortality in bipolar disorder: a Swedish national cohort study. JAMA Psychiatry. 2013;70:931–9.
Pompili M, Gonda X, Serafini G, Innamorati M, Sher L, Amore M, et al. Epidemiology of suicide in bipolar disorders: A systematic review of the literature. Bipolar Disord. 2013;15:457–90.
Singh B, Yocum AK, Strawbridge R, Young AH, Patel R. Patterns of pharmacotherapy for bipolar disorder: A GBC survey. Bipolar Disord. 2024;26:22–32.
Hidalgo-Mazzei D, Mantingh T, Pérez de Mendiola X, Samalin L, Undurraga J, Strejilevich S, et al. Clinicians’ preferences and attitudes towards the use of lithium in the maintenance treatment of bipolar disorders around the world: A survey from the ISBD Lithium task force. Int J Bipolar Disord. 2023;11:20.
National Collaborating Centre for Mental Health (UK). Bipolar Disorder: The Management of Bipolar Disorder in Adults. in Children and Adolescents, in Primary and Secondary Care (British Psychological Society, 2006).
Geddes JR, Miklowitz DJ. Treatment of bipolar disorder. Lancet. 2013;381:1672–82.
Ching CRK, Hibar DP, Gurholt TP, Nunes A, Thomopoulos SI, Abé C, et al. What we learn about bipolar disorder from large-scale neuroimaging: Findings and future directions from the ENIGMA Bipolar Disorder Working Group. Hum Brain Mapp. 2020;43:56–82.
Hibar DP, Westlye LT, Doan NT, Jahanshad N, Cheung JW, Ching CRK, et al. Cortical abnormalities in bipolar disorder: an MRI analysis of 6503 individuals from the ENIGMA Bipolar Disorder Working Group. Mol Psychiatry. 2018;23:932–42.
Hibar DP, Westlye LT, van Erp TG, Rasmussen J, Leonardo CD, Faskowitz J, et al. Subcortical volumetric abnormalities in bipolar disorder. Mol Psychiatry. 2016;21:1710–6.
Fortea, L, Ortuño, M, De Prisco, M, Oliva, V, Albajes-Eizagirre, A, Fortea, A et al. Atlas of gray matter volume differences across psychiatric conditions: A systematic review with a novel meta-analysis that considers co-occurring disorders. Biol Psychiatry (2024).
Zhang W, Xiao Y, Sun H, Patino LR, Tallman MJ, Weber WA, et al. Discrete patterns of cortical thickness in youth with bipolar disorder differentially predict treatment response to quetiapine but not lithium. Neuropsychopharmacology. 2018;43:2256–63.
Lei D, Qin K, Li W, Pinaya WHL, Tallman MJ, Patino LR, et al. Brain morphometric features predict medication response in youth with bipolar disorder: a prospective randomized clinical trial. Psychol Med. 2023;53:4083–93.
Bernardo M, Vieta E, Saiz Ruiz J, Rico-Villademoros F, Alamo C, Bobes J, et al. Recommendations for switching antipsychotics. A position statement of the spanish society of psychiatry and the spanish society of biological psychiatry. Rev Psiquiatr Salud Ment Engl Ed. 2011;4:150–68.
Chakrabarti S. Treatment-adherence in bipolar disorder: A patient-centred approach. World J Psychiatry. 2016;6:399–409.
Öhlund L, Ott M, Oja S, Bergqvist M, Lundqvist R, Sandlund M, et al. Reasons for lithium discontinuation in men and women with bipolar disorder: a retrospective cohort study. BMC Psychiatry. 2018;18:37.
Devulapalli KK, Ignacio RV, Weiden P, Cassidy KA, Williams TD, Safavi R, et al. Why do persons with bipolar disorder stop their medication? Psychopharmacol Bull. 2010;43:5–14.
Collins, GS, Moons, KGM, Dhiman, P, Riley, RD, Beam, AL, Van Calster, B et al. TRIPOD+AI statement: updated guidance for reporting clinical prediction models that use regression or machine learning methods. BMJ e078378 (2024) https://doi.org/10.1136/bmj-2023-078378.
Palau P, Solanes A, Madre M, Saez-Francas N, Sarró S, Moro N, et al. Improved estimation of the risk of manic relapse by combining clinical and brain scan data. Span J Psychiatry Ment Health. 2023;16:235–43.
Salazar de Pablo G, Radua J, Frearson G, Young AH, Arango C, Kelleher I, et al. Development and validation of a prognostic model and risk calculator for the estimation of bipolar-spectrum disorder risk in hospitalised adolescents with non-psychotic/non-bipolar mental disorders. Mol Psychiatry. 2025. https://doi.org/10.1038/s41380-025-03244-1
Drugs@FDA: FDA-Approved Drugs. https://www.accessdata.fda.gov/scripts/cder/daf/.
Nath M, Gupta V. Mood Stabilizers. StatPearls. Treasure Island (FL): StatPearls Publishing; 2025.
Depression Resource Guides | Community Care of North Carolina. https://www.communitycarenc.org/what-we-do/clinical-programs/behavioral-health-integration/clinical-resources/depression.
British National Formulary (BNF) | Pharmaceutical Press. https://www.pharmaceuticalpress.com/products/british-national-formulary/.
UpToDate: Trusted, evidence-based solutions for modern healthcare. https://www.wolterskluwer.com/en/solutions/uptodate.
Leucht S, Crippa A, Siafis S, Patel MX, Orsini N, Davis JM. Dose-response meta-analysis of antipsychotic drugs for acute schizophrenia. Am J Psychiatry. 2020;177:342–53.
Gardner DM, Murphy AL, O’Donnell H, Centorrino F, Baldessarini RJ. International consensus study of antipsychotic dosing. Am J Psychiatry. 2010;167:686–93.
Thompson PM, Jahanshad N, Ching CRK, Salminen LE, Thomopoulos SI, Bright J, et al. ENIGMA and global neuroscience: A decade of large-scale studies of the brain in health and disease across more than 40 countries. Transl Psychiatry. 2020;10:1–28.
Desikan RS, Ségonne F, Fischl B, Quinn BT, Dickerson BC, Blacker D, et al. An automated labeling system for subdividing the human cerebral cortex on MRI scans into gyral based regions of interest. NeuroImage. 2006;31:968–80.
Fischl B, Sereno MI, Dale AM. Cortical surface-based analysis: II: Inflation, flattening, and a surface-based coordinate system. NeuroImage. 1999;9:195–207.
Radua J, Vieta E, Shinohara R, Kochunov P, Quidé Y, Green MJ, et al. Increased power by harmonizing structural MRI site differences with the ComBat batch adjustment method in ENIGMA. NeuroImage. 2020;218:116956.
Solanes A, Palau P, Fortea L, Salvador R, González-Navarro L, Llach CD, et al. Biased accuracy in multisite machine-learning studies due to incomplete removal of the effects of the site. Psychiatry Res Neuroimaging. 2021;314:111313.
Sun D, Rakesh G, Haswell CC, Logue M, Baird CL, O’Leary EN, et al. A comparison of methods to harmonize cortical thickness measurements across scanners and sites. NeuroImage. 2022;261:119509.
Radua J, Koutsouleris N. Ten simple rules for using machine learning in mental health research. Biol Psychiatry. 2024;96:511–3.
Solanes A, Gosling CJ, Fortea L, Ortuño M, Lopez-Soley E, Llufriu S, et al. Removing the effects of the site in brain imaging machine-learning - Measurement and extendable benchmark. Neuroimage. 2023;265:119800.
Öhlund L, Ott M, Bergqvist M, Oja S, Lundqvist R, Sandlund M, et al. Clinical course and need for hospital admission after lithium discontinuation in patients with bipolar disorder type I or II: Mirror-image study based on the LiSIE retrospective cohort. BJPsych Open. 2019;5:e101.
Kishi T, Sakuma K, Okuya M, Matsuda Y, Esumi S, Hashimoto Y, et al. Recurrence of mania or depression among adult bipolar patients who continued using lithium: A single-group summary meta-analysis of randomized trials. J Clin Psychopharmacol. 2020;40:468–74.
Altshuler L, Suppes T, Black D, Nolen WA, Keck PE Jr, Frye MA, et al. Impact of antidepressant discontinuation after acute bipolar depression remission on rates of depressive relapse at 1-year follow-up. Am J Psychiatry. 2003;160:1252–62.
Bertolini F, Ostuzzi G, Pievani M, Aguglia A, Bartoli F, Bortolaso P, et al. Comparing long-acting antipsychotic discontinuation rates under ordinary clinical circumstances: A survival analysis from an observational, pragmatic study. CNS Drugs. 2021;35:655–65.
Ketter TA, Brooks JO, Hoblyn JC, Champion LM, Nam JY, Culver JL, et al. Effectiveness of lamotrigine in bipolar disorder in a clinical setting. Journal of Psychiatric Research. 2008;43:13–23.
Bowden CL. Anticonvulsants in bipolar disorders: current research and practice and future directions. Bipolar Disorders. 2009;11:20–33.
Taylor C, Fricker AD, Devi LA, Gomes I. Mechanisms of action of antidepressants: from neurotransmitter systems to signaling pathways. Cell Signal. 2005;17:549–57.
Phillips ML, Swartz HA. A critical appraisal of neuroimaging studies of bipolar disorder: toward a new conceptualization of underlying neural circuitry and a road map for future research. Am J Psychiatry. 2014;171:829–43.
Abé C, Ching CRK, Liberg B, Lebedev AV, Agartz I, Akudjedu TN, et al. Longitudinal structural brain changes in bipolar disorder: A multicenter neuroimaging study of 1232 individuals by the ENIGMA Bipolar Disorder Working Group. Biol Psychiatry. 2022;91:582–92.
Robinson JL, Bearden CE, Monkul ES, Tordesillas-Gutiérrez D, Velligan DI, Frangou S, et al. Fronto-temporal dysregulation in remitted bipolar patients: An fMRI delayed-non-match-to-sample (DNMS) study. Bipolar Disord. 2009;11:351–60.
Schumer MC, Chase HW, Rozovsky R, Eickhoff SB, Phillips ML. Prefrontal, parietal, and limbic condition-dependent differences in bipolar disorder: A large-scale meta-analysis of functional neuroimaging studies. Mol Psychiatry. 2023;28:2826–38.
Seeman MV. The pharmacodynamics of antipsychotic drugs in women and men. Front. Psychiatry. 2021;12:650904.
Galbally M, Wynter K, Siskind D, Correll CU, Northwood K, Every-Palmer S. Sex differences between female and male individuals in antipsychotic efficacy and adverse effects in the treatment of schizophrenia. CNS Drugs. 2024;38:559–70.
McDonald C. Brain structural effects of psychopharmacological treatment in bipolar disorder. Curr Neuropharmacol. 2015;13:445–57.
Lyoo IK, Dager SR, Kim JE, Yoon SJ, Friedman SD, Dunner DL, et al. Lithium-induced gray matter volume increase as a neural correlate of treatment response in bipolar disorder: A longitudinal brain imaging study. Neuropsychopharmacology. 2010;35:1743–50.
Ochoa ELM. Lithium as a neuroprotective agent for bipolar disorder: An overview. Cell Mol Neurobiol. 2022;42:85–97.
Hozer F, Sarrazin S, Laidi C, Favre P, Pauling M, Cannon D, et al. Lithium prevents grey matter atrophy in patients with bipolar disorder: an international multicenter study. Psychol Med. 2021;51:1201–10.
Hajek T, Bauer M, Simhandl C, Rybakowski J, O’Donovan C, Pfennig A, et al. Neuroprotective effect of lithium on hippocampal volumes in bipolar disorder independent of long-term treatment response. Psychol Med. 2014;44:507–17.
Sämann PG, Höhn D, Chechko N, Kloiber S, Lucae S, Ising M, et al. Prediction of antidepressant treatment response from gray matter volume across diagnostic categories. Eur Neuropsychopharmacol. 2013;23:1503–15.
Wu P, Zhang A, Sun N, Lei L, Liu P, Wang Y, et al. Cortical thickness predicts response following 2 weeks of SSRI regimen in first-episode, drug-naive major depressive disorder: An MRI study. Front Psychiatry. 2021;12:751756.
Sara SJ. The locus coeruleus and noradrenergic modulation of cognition. Nat Rev Neurosci. 2009;10:211–23.
Jacobs BL, Azmitia EC. Structure and function of the brain serotonin system. Physiol Rev. 1992;72:165–229.
Duman RS, Aghajanian GK. Synaptic dysfunction in depression: potential therapeutic targets. Science. 2012;338:68–72.
Castrén E, Hen R. Neuronal plasticity and antidepressant actions. Trends Neurosci. 2013;36:259–67.
Castrén E, Monteggia LM. Brain-Derived neurotrophic factor signaling in depression and antidepressant action. Biol Psychiatry. 2021;90:128–36.
Sheline YI, Price JL, Yan Z, Mintun MA. Resting-state functional MRI in depression unmasks increased connectivity between networks via the dorsal nexus. Proc Natl Acad Sci USA. 2010;107:11020–5.
Menculini G, Steardo L Jr, Sciarma T, D’Angelo M, Lanza L, Cinesi G, et al. Sex differences in bipolar disorders: impact on psychopathological features and treatment response. Front Psychiatry. 2022;13:926594.
Smilowitz S, Aftab A, Aebi M, Levin J, Tatsuoka C, Sajatovic M. Age-related differences in medication adherence, symptoms, and stigma in poorly-adherent adults with bipolar disorder. J Geriatr Psychiatry Neurol. 2020;33:250–5.
Karanti A, Bobeck C, Osterman M, Kardell M, Tidemalm D, Runeson B, et al. Gender differences in the treatment of patients with bipolar disorder: a study of 7354 patients. J Affect Disord. 2015;174:303–9.
Oliva V, Vieta E. Predicting the past: The risks and rewards of post-hoc findings. Eur Neuropsychopharmacol J Eur Coll Neuropsychopharmacol. 2025;92:21–22.
De Prisco M, Vieta E. The never-ending problem: Sample size matters. Eur Neuropsychopharmacol J Eur Coll Neuropsychopharmacol. 2024;79:17–8.
Boonstra G, van Haren NE, Schnack HG, Cahn W, Burger H, Boersma M, et al. Brain volume changes after withdrawal of atypical antipsychotics in patients with first-episode schizophrenia. J Clin Psychopharmacol. 2011;31:146–53.
Dietze LMF, McWhinney SR, Favre P, Abé C, Alexander N, Barkhau C, et al. White matter microstructure in obesity and bipolar disorders: an ENIGMA bipolar disorder working group study in 2186 individuals. Mol Psychiatry. 2025;30:1770–9.
Rivas-Fernández MÁ, Domingo-Ayllón M, De Prisco M, Fernández-Corcuera P, Canales-Rodríguez EJ, Vieta E, et al. Impact of bipolar disorder increased white matter hyperintensities on white matter connectivity. Bipolar Disord. 2025;27:289–97.
Montejo L, Sole B, Fortea L, Jimenez E, Martinez-Aran A, Martinez-Heras E, et al. Study protocol - elucidating the neural correlates of functional remediation for older adults with bipolar disorder. Front Psychiatry. 2023;14:1302255.
Radua J, Fortea L, Goikolea JM, Zorrilla I, Bernardo M, Arrojo M, et al. Meta-analysis of the effects of adjuvant drugs in co-occurring bipolar and substance use disorder. Span J Psychiatry Ment Health. 2024;17:239–50.
Acknowledgements
This work was supported by funding from the Milken Institute/Baszucki Brain Research Fund, especially for SK and AS. The ENIGMA Working Group acknowledges the NIH Big Data to Knowledge (BD2K) award for foundational support and consortium development (U54 EB020403 to Paul M. Thompson). For a complete list of ENIGMA-related grant support, please see http://enigma.ini.usc.edu/about-2/funding/. CRKC, LN, MJYK, YI, SIT and PMT were supported by R21 MH139001, R01 MH129742, R01 MH131806, R01 AG058854, R01 MH134962. Research reported in this publication was supported by the Office Of The Director, National Institutes Of Health of the National Institutes of Health under Award Number S10OD032285. The IDIBAPS (Clinic) and Barcelona (FIGMAG/Clinic) MRI acquisition studies were supported by the Spanish Ministry of Science and Innovation. Instituto de Salud Carlos III (PI15/00283, PI19/00394, and PI22/00261), integrated into the Plan Nacional de I + D + I and co-financed by ERDF Funds from the European Commission (“A Way of Making Europe”), CIBERSAM, and the CERCA Program / Generalitat de Catalunya and Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement and Departament de Salut (SLT002/16/00331, SLT006/17/00357, 2017SGR1365, 2021 SGR 01128). The CIAM group (PI: FMH) was supported by the University Research Committee, University of Cape Town, and South African funding bodies National Research Foundation (SANRF) and Medical Research Council (SAMRC); DJS from CIAM was supported by the SAMRC. The COGSBD study was supported by project grants from the Rebecca L Cooper Medical Research Foundation, the Jack Brockhoff Foundation, the Henry Freeman Trust, the Society of Mental Health Research, the Barbara Dicker Brain Sciences Foundation, and the University of Melbourne. TVR was supported by an NHMRC Early Career Fellowship (GNT1088785), a Dame Kate Campbell Fellowship from the University of Melbourne, and an Al and Val Rosenstrauss Fellowship from the Rebecca L Cooper Medical Research Fellowship. JK was supported by a Swinburne University/Australian Postgraduate Award. L Furlong was supported by an Australian Rotary Health/Ian Parker Bipolar Research Fund postgraduate scholarship. SLR was supported by an NHMRC Senior Fellowship (GNT1154651) The Imaging Genetics in Psychosis (IGP) study was supported by Project Grants from the Australian National Health and Medical Research Council (NHMRC; APP630471 and APP1081603), and the Macquarie University’s ARC Centre of Excellence in Cognition and its Disorders (CE110001021). MJG was supported by an Australian Research Council Future Fellowship (FT0991511; 2009-13) and an R.D. Wright Biomedical Career Development Award from the NHMRC (1061875; 2014-17). The FOR2107 cohorts (Marburg and Münster) and the Münster Neuroimaging Cohort (MNC) are part of the German multicenter consortium “Neurobiology of Affective Disorders. A translational perspective on brain structure and function,” funded by the German Research Foundation (Deutsche Forschungsgemeinschaft DFG; Forschungsgruppe/Research Unit FOR2107). TK (speaker FOR2107; DFG grant numbers KI588/14-1, KI588/14-2, KI588/20-1, KI588/22-1), UD (co-speaker FOR2107; DA 1151/5-1, DA 1151/5-2, DA1151/6-1, DA1151/9-1, DA1151/10-1, DA1151/11-1), BS (FOR2107 extension project STR 1146/18-1). A full list of acknowledgements can be found here: https://for2107.de/acknowledgements/?lang=en. This work was also partly funded by the DFG SFB/TRR 393 (project grant no 521379614). The University of Galway research was supported by the Health Research Board (HRA-POR-324) awarded to DMC. We thank the participants and the support of the Wellcome-Trust HRB Clinical Research Facility and the Center for Advanced Medical Imaging, St. James Hospital, Dublin, Ireland. The Groningen study was founded by EU-FP7-HEALTH-222963 ‘MOODIN- FLAME’ and EU-FP7-PEOPLE-286334 ‘PSYCHAID’. The San Raffaele site was supported by the European Union H2020 EU.3.1.1 grant 754740 MOODSTRATIFICATION. The Singapore study was supported by a research grant from the Singapore Bioimaging Consortium (RP C009/06) awarded to KS. COGSBD cohort. SK and AS were supported by funding from the Milken Institute/Baszucki Brain Research Fund. IHG was supported by the National Institutes of Health (R37MH101495). CRKC, OAA, SIT, and PMT are supported in part by the U.S. NIMH, under grants R01MH129742 and R01MH131806. The National University of Defense Technology research was supported by the National Natural Science Foundation of China (U24A20339), the STI 2030-Major Projects (2022ZD0208903), and the Science and Technology Innovation Program of Hunan Province (2023RC1004 and 2024QK2006). E.J.C.R. acknowledges financial support from the “Ramón y Cajal” Excellence Fellowship (Grant RYC2023-042763-I), funded by the Ministry of Science, Innovation and Universities (MICIU) and the Spanish State Research Agency (AEI, 10.13039/50110001103), and co-financed by the European Social Fund Plus (ESF+). Finally, we would like to acknowledge the late Professor Dan J. Stein for his longstanding leadership and collaboration within ENIGMA-Bipolar Working Group and for his invaluable contributions to psychiatry, neuroscience, and mental health research. His intellectual generosity, mentorship, and unwavering support shaped this work and the broader field in lasting ways. His scientific legacy and his kindness to colleagues continue to inspire us.
Author information
Authors and Affiliations
Consortia
Contributions
AS, LFo, OAA, CRKC, ToH, DHM, LLZ, CMcD, JR, and EdV designed the study. PMT, CRKC, LN, CMcD, and JR acquired research funding for the ENIGMA-BD Medications Initiative; for funding of site cohorts, please see the Acknowledgements. JR, AS, MARF, and LFo developed the methodology. ADG, AJ, AK, AP, AS, BB, BCMH, BS, CMcD, CRKC, DG, DHM, DJS, DMC, EJCR, EJL, EMTM, EPC, EdV, EnV, FB, FH, FSa, FSc, FSt, FTO, HJ, HT, IB, IHG, IN, JAK, JB, JR, KF, KS, LFo, LFu, LLZ, LN, LT, MA, MARF, MDS, MJG, MJYK, NA, OAA, PFC, PMT, RS, SIT, SK, SLR, SM, SMcW, SP, SS, TB, TEVR, TiH, ToH, TK, UD, YI, and YQ were involved in data collection, processing, and quality control. SK, AS, and CMcD curated the database. AS, MARF, LFo, and JR conducted the statistical analyses and drafted the manuscript. All authors critically revised the manuscript and approved its final version.
Corresponding authors
Ethics declarations
Competing interests
TK received unrestricted educational grants (unrelated to the present work) from: Servier, Janssen, Recordati, Aristo, Otsuka, and Neuraxpharm. EV has received grants and served as a consultant, advisor, or CME speaker for the following entities (unrelated to the present work): AB-Biotics, Abbott, AbbVie, Adamed, Aimentia, Angelini, Biogen, Biohaven, Boehringer Ingelheim, Casen-Recordati, Celon, Compass, Dainippon Sumitomo Pharma, Ethypharm, Ferrer, Gedeon Richter, GH Research, Glaxo Smith-Kline, Idorsia, Janssen, Lundbeck, Neuraxpharm, Newron, Novartis, Organon, Otsuka, Rovi, Sage, Sanofi-Aventis, Sunovion, Takeda, and Viatris. JR has received CME honoraria from Inspira Networks and Evidenze Health for machine learning courses promoted by Adamed and Viatris, outside the submitted work. All other authors report no biomedical financial interest or potential conflicts of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Fortea, L., Rivas-Fernández, M.Á., Solanes, A. et al. Cortical morphometry might predict currently prescribed vs. discontinued medications in bipolar disorder, even after controlling for the cumulative dose effects: An ENIGMA mega-analysis. Mol Psychiatry (2026). https://doi.org/10.1038/s41380-026-03536-0
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41380-026-03536-0