Abstract
Background
Non-suicidal self-injury (NSSI) persists as a major public health challenge worldwide. Identifying and strategically targeting risk factors for NSSI constitutes a practical approach to its prevention. We aim to synthesize existing knowledge concerning the range and magnitude of risk factors for NSSI among children and adolescents, and to critically assess the robustness of the available evidence.
Methods
In this umbrella review, six bibliographic databases were systematically searched for articles published from database inception to Dec 2024. For the assessment of evidence credibility, pre-specified criteria for classifying evidence were utilized, categorized as convincing (“class I”), highly suggestive (“class II”), suggestive (“class III”), weak (“class IV”), or no evidence (“class V”). The Amstar-2 framework was employed to evaluate the quality of the evidence which graded as “high,” “moderate,” “low,” or “critically low” quality.
Results
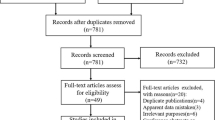
The study included meta-analyses of observational studies in the past 30 years on risk factors for NSSI in children and adolescents. We identified 16 meta-analyses comprising 410 primary studies on 43 risk factors from 38 countries, involving 2,659,156 children and adolescents. Twenty-three (e.g. LGBTIQ) risk factors were categorized as individual, followed by family level (n = 8, e.g. childhood maltreatment), school/peer level (n = 8, e.g. bully victims) and multifactorial level (n = 4, e.g. no religion). Eighteen (41.86%) risk factors provided highly suggestive (Class II) evidence of association with NSSI. Suggestive evidence (class III) indicated that NSSI was associated with adverse childhood experiences (2.31, 1.77–3.01) and being left-behind children (1.37, 1.11–1.69).
Conclusion
A multitude of risk factors spanning diverse domains were identified, highlighting the multifactorial nature of NSSI in adolescents and children. Comprehensive prevention strategies and measures should be conducted for children and adolescents to decrease the risk of NSSI and associated harms in multilevel approaches.

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Moran P, Chandler A, Dudgeon P, Kirtley OJ, Knipe D, Pirkis J, et al. The lancet commission on self-harm. Lancet. 2024;404:1445–92.
GBD 2019 Mental Disorders Collaborators. Global, regional, and national burden of 12 mental disorders in 204 countries and territories, 1990-2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet Psychiatry. 2022;9:137–50.
GBD 2019 Diseases and Injuries Collaborators. Global burden of 369 diseases and injuries in 204 countries and territories, 1990-2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet. 2020;396:1204–22.
Castelpietra G, Knudsen AKS, Agardh EE, Armocida B, Beghi M, Iburg KM, et al. The burden of mental disorders, substance use disorders and self-harm among young people in Europe, 1990–2019: findings from the Global Burden of Disease Study 2019. Lancet Reg Health Eur. 2022;16:100341.
GBD 2017 Child and Adolescent Health Collaborators, Reiner RC, Olsen HE, Ikeda CT, Echko MM, Ballestreros KE, et al. Diseases, injuries, and risk factors in child and adolescent health, 1990–2017: findings from the global burden of diseases, injuries, and risk factors 2017 study. JAMA Pediatr. 2019;173:e190337.
Hawton K, Saunders KE, O’Connor RC. Self-harm and suicide in adolescents. Lancet. 2012;379:2373–82.
Skegg K. Self-harm. Lancet. 2005;366:1471–83.
Brunner R, Kaess M, Parzer P, Fischer G, Carli V, Hoven CW, et al. Life-time prevalence and psychosocial correlates of adolescent direct self-injurious behavior: a comparative study of findings in 11 European countries. J Child Psychol Psychiatry. 2014;55:337–48.
Hawton K, James A. Suicide and deliberate self harm in young people. BMJ. 2005;330:891–4.
Muehlenkamp JJ, Claes L, Havertape L, Plener PL. International prevalence of adolescent non-suicidal self-injury and deliberate self-harm. Child Adolesc Psychiatry Ment Health. 2012;6:10.
Xiao Q, Song X, Huang L, Hou D, Huang X. Global prevalence and characteristics of non-suicidal self-injury between 2010 and 2021 among a non-clinical sample of adolescents: a meta-analysis. Front Psychiatry. 2022;13:912441.
Griffin E, McMahon E, McNicholas F, Corcoran P, Perry IJ, Arensman E. Increasing rates of self-harm among children, adolescents and young adults: a 10-year national registry study 2007-2016. Soc Psychiatry Psychiatr Epidemiol. 2018;53:663–71.
Hawton K, Witt KG, Salisbury TLT, Arensman E, Gunnell D, Hazell P, et al. Psychosocial interventions following self-harm in adults: a systematic review and meta-analysis. Lancet Psychiatry. 2016;3:740–50.
Kiekens G, Claes L, Demyttenaere K, Auerbach RP, Green JG, Kessler RC, et al. Lifetime and 12-Month nonsuicidal self-injury and academic performance in college freshmen. Suicide Life Threat Behav. 2016;46:563–76.
Gulbas LE, Hausmann-Stabile C, De Luca SM, Tyler TR, Zayas LH. An exploratory study of nonsuicidal self-injury and suicidal behaviors in adolescent Latinas. Am J Orthopsychiatry. 2015;85:302–14.
Hamza CA, Willoughby T. Nonsuicidal self-injury and suicidal risk among emerging adults. J Adolesc Health. 2016;59:411–5.
Robinson K, Garisch JA, Kingi T, Brocklesby M, O’Connell A, Langlands RL, et al. Reciprocal risk: the longitudinal relationship between emotion regulation and non-suicidal self-injury in adolescents. J Abnorm Child Psychol. 2019;47:325–32.
Knipe D, Padmanathan P, Newton-Howes G, Chan LF, Kapur N. Suicide and self-harm. Lancet. 2022;399:1903–16.
Bronfenbrenner U Ecological systems theory. Greenwich, CT: JAI. 1989.
Kiekens G, Claes L, Hasking P, Mortier P, Bootsma E, Boyes M, et al. A longitudinal investigation of non-suicidal self-injury persistence patterns, risk factors, and clinical outcomes during the college period. Psychol Med. 2023;53:6011–26.
Wu B, Zhang H, Chen J, Chen J, Liu Z, Cheng Y, et al. Potential mechanisms of non-suicidal self-injury (NSSI) in major depressive disorder: a systematic review. Gen Psychiatr. 2023;36:e100946.
Hu C, Jiang W, Wu Y, Wang M, Lin J, Chen S, et al. Microstructural abnormalities of white matter in the cingulum bundle of adolescents with major depression and non-suicidal self-injury. Psychol Med. 2024;54:1113–21.
Chen X, Xu J, Wang X, Qiu Y, Yang R, Wang Z, et al. Mediating role of anxiety and impulsivity in the association between child maltreatment and lifetime non-suicidal self-injury with and without suicidal self-injury. J Affect Disord. 2024;347:57–65.
Lee PH, Tervoclemmens B, Liu RT, Gersten MB, Jung J, Janes AC, et al. Use of tobacco products and suicide attempts among elementary school-aged children. JAMA Netw Open. 2024;7:e240376.
Xie X, Li Y, Liu J, Zhang L, Sun T, Zhang C, et al. The relationship between childhood maltreatment and non-suicidal self-injury in adolescents with depressive disorders. Psychiatry Res. 2024;331:115638.
Cwik MF, Barlow A, Tingey L, Larzelere-Hinton F, Goklish N, Walkup JT. Nonsuicidal self-injury in an American Indian reservation community: results from the White Mountain Apache surveillance system, 2007-2008. J Am Acad Child Adolesc Psychiatry. 2011;50:860–9.
Qu D, Wen X, Liu B, Zhang X, He Y, Chen D, et al. Non-suicidal self-injury in Chinese population: a scoping review of prevalence, method, risk factors and preventive interventions. Lancet Reg Health West Pac. 2023;37:100794.
Fusar-Poli P, Radua J. Ten simple rules for conducting umbrella reviews. Evid Based Ment Health. 2018;21:95–100.
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71.
Hailes HP, Yu R, Danese A, Fazel S. Long-term outcomes of childhood sexual abuse: an umbrella review. Lancet Psychiatry. 2019;6:830–9.
American Psychiatric Association(APA). Diagnostic and statistical manual of mental disorders Fifth Edition(DSM-5) Arlington American Psychiatric Association; 2013.
Radua J, Ramella-Cravaro V, Ioannidis JPA, Reichenberg A, Phiphopthatsanee N, Amir T, et al. What causes psychosis? an umbrella review of risk and protective factors. World Psychiatry. 2018;17:49–66.
Lane MM, Gamage E, Du S, Ashtree DN, McGuinness AJ, Gauci S, et al. Ultra-processed food exposure and adverse health outcomes: umbrella review of epidemiological meta-analyses. BMJ. 2024;384:e077310.
Veronese N, Demurtas J, Thompson T, Solmi M, Pesolillo G, Celotto S, et al. Effect of low-dose aspirin on health outcomes: an umbrella review of systematic reviews and meta-analyses. Br J Clin Pharmacol. 2020;86:1465–75.
Favril L, Yu R, Geddes JR, Fazel S. Individual-level risk factors for suicide mortality in the general population: an umbrella review. Lancet Public Health. 2023;8:e868–e877.
Radua J, De Prisco M, Oliva V, Fico G, Vieta E, Fusar‐Poli P. Impact of air pollution and climate change on mental health outcomes: an umbrella review of global evidence. World Psychiatry. 2024;23:244–56.
Cochrane Handbook for Systematic Reviews of Interventions. https://training.cochrane.org/handbook/current. Accessed 24 May 2024.
IntHout J, Ioannidis JPA, Rovers MM, Goeman JJ. Plea for routinely presenting prediction intervals in meta-analysis. BMJ Open. 2016;6:e010247.
Higgins JPT, Thompson SG, Spiegelhalter DJ. A re-evaluation of random-effects meta-analysis. J R Stat Soc Ser A Stat Soc. 2009;172:137–59.
Egger M, Davey Smith G, Schneider M, Minder C. Bias in meta-analysis detected by a simple, graphical test. BMJ. 1997;315:629–34.
Sterne JA, Egger M. Funnel plots for detecting bias in meta-analysis: guidelines on choice of axis. J Clin Epidemiol. 2001;54:1046–55.
Shea BJ, Reeves BC, Wells G, Thuku M, Hamel C, Moran J, et al. AMSTAR 2: a critical appraisal tool for systematic reviews that include randomised or non-randomised studies of healthcare interventions, or both. BMJ. 2017;358:j4008.
Xu T, Zhang T, Zhang F, Zhou X. Influencing factors of self-injury behaviors among Chinese adolescents: a meta-analysis. Mod Preventive Med. 2021;48:706–709713.
Tao M, Feng L, Guo F, Hai F, Yang S. Meta-analysis on the detection rate and influencing factors of non-suicide self-injury among adolescents in China. J Guangxi Med Univ. 2023;40:1627–34.
Xu D, Feng Q, Xu H. Meta-analysis of risk factors for non-suicidal self-injury among Chinese adolescents. Psychol Monthly. 2023;18:21–25.
Wen S, Guo Z, Wang T, Ou X, Xie Z, Yang Q, et al. Screen time and health risks among children and adolescents in China: a meta-analysis. China Preventive Med. 2023;24:662–7.
Witt K, Milner A, Spittal MJ, Hetrick S, Robinson J, Pirkis J, et al. Population attributable risk of factors associated with the repetition of self-harm behaviour in young people presenting to clinical services: a systematic review and meta-analysis. Eur Child Adoles Psy. 2019;28:5–18.
Wang Y, Li X, Ng CH, Xu D-W, Hu S, Yuan T. Risk factors for non-suicidal self-injury (NSSI) in adolescents: a meta-analysis. EClinicalMedicine. 2022;46:101350.
Nesi J, Burke TA, Bettis AH, Kudinova AY, Thompson EC, MacPherson HA, et al. Social media use and self-injurious thoughts and behaviors: a systematic review and meta-analysis. Clin Psychol Rev. 2021;87:102038.
Marchi M, Arcolin E, Fiore G, Travascio A, Uberti D, Amaddeo F, et al. Self-harm and suicidality among LGBTIQ people: a systematic review and meta-analysis. Int Rev Psychiatry. 2022;34:240–56.
Lin K, Ramos S, Sun J. Urbanization, self-harm, and suicidal ideation in left-behind children and adolescents in China: a systematic review and meta-analysis. Curr Opin Psychiatry. 2024;37:225–36.
Huang H, Ding Y, Wan X, Liang Y, Zhang Y, Lu G, et al. A meta-analysis of the relationship between bullying and non-suicidal self-injury among children and adolescents. Sci Rep. 2022;12:17285.
Heerde JA, Hemphill SA. Are bullying perpetration and victimization associated with adolescent deliberate self-harm? a meta-analysis. Arch Suicide Res. 2019;23:353–81.
Fox KR, Franklin JC, Ribeiro JD, Kleiman EM, Bentley KH, Nock MK. Meta-analysis of risk factors for nonsuicidal self-injury. Clin Psychol Rev. 2015;42:156–67.
Epstein S, Roberts E, Sedgwick R, Polling C, Finning K, Ford T, et al. School absenteeism as a risk factor for self-harm and suicidal ideation in children and adolescents: a systematic review and meta-analysis. Eur Child Adoles Psy. 2020;29:1175–94.
Calvo N, Lugomarín J, Oriol M, Pérezgalbarro C, Restoy D, Ramosquiroga J, et al. Childhood maltreatment and non-suicidal self-injury in adolescent population: a systematic review and meta-analysis. Child Abuse Negl. 2024;157:107048.
Haney AM. Nonsuicidal self-injury and religiosity: a meta-analytic investigation. Am J Orthopsychiatry. 2020;90:78–89.
Thornicroft G, Sunkel C, Milenova M. Commission implementation partnership. how to stop stigma: implementing the lancet commission on ending stigma and discrimination in mental health. Lancet Psychiatry. 2024;11:88–89.
Freeman M, Mulutsi NE. Law and policy are essential but insufficient to end stigma and discrimination in mental health. Lancet. 2022;400:1387–9.
Thornicroft G, Sunkel C, Alikhon Aliev A, Baker S, Brohan E, El Chammay R, et al. The Lancet Commission on ending stigma and discrimination in mental health. Lancet. 2022;400:1438–80.
Dvir M, Sarah A, Orna B. Ethnic identity and barriers for using mental health services among Arab-Bedouin women coping with emotional distresses. Arch Womens Ment Health. 2023;26:609–24.
UIS Statistics. https://data.uis.unesco.org/. Accessed 11 July 2024.
The price of inaction: the global private, fiscal and social costs of children and youth not learning | UNESCO. https://www.unesco.org/en/articles/price-inaction-global-private-fiscal-and-social-costs-children-and-youth-not-learning. Accessed 11 July 2024.
Geulayov G, Casey D, McDonald KC, Foster P, Pritchard K, Wells C, et al. Incidence of suicide, hospital-presenting non-fatal self-harm, and community-occurring non-fatal self-harm in adolescents in England (the iceberg model of self-harm): a retrospective study. Lancet Psychiatry. 2018;5:167–74.
McManus S, Gunnell D, Cooper C, Bebbington PE, Howard LM, Brugha T, et al. Prevalence of non-suicidal self-harm and service contact in England, 2000-14: repeated cross-sectional surveys of the general population. Lancet Psychiatry. 2019;6:573–81.
John A, Friedmann Y, DelPozo-Banos M, Frizzati A, Ford T, Thapar A. Association of school absence and exclusion with recorded neurodevelopmental disorders, mental disorders, or self-harm: a nationwide, retrospective, electronic cohort study of children and young people in Wales, UK. Lancet Psychiatry. 2022;9:23–34.
Bonell C, Blakemore S-J, Fletcher A, Patton G. Role theory of schools and adolescent health. Lancet Child Adolesc Health. 2019;3:742–8.
Shinde S, Weiss HA, Varghese B, Khandeparkar P, Pereira B, Sharma A, et al. Promoting school climate and health outcomes with the SEHER multi-component secondary school intervention in Bihar, India: a cluster-randomised controlled trial. Lancet. 2018;392:2465–77.
Ougrin D, Asarnow JR. The end of family therapy for self-harm, or a new beginning? Lancet Psychiatry. 2018;5:188–9.
Compulsory Education Law of the People’s Republic of China. http://www.moe.gov.cn/jyb_sjzl/sjzl_zcfg/zcfg_jyfl/202110/t20211029_575949.html. Accessed 11 June 2024.
Ministry of Education of the People’s Republic of China. MOE discusses key tasks for education supervision in 2024. 2024. http://en.moe.gov.cn/news/press_releases/202405/t20240508_1129403.html. Accessed 11 June 2024.
Kearney CA, Graczyk P. A response to intervention model to promote school attendance and decrease school absenteeism. Child Youth Care For. 2014;43:1–25.
Van Ginneken N, Chin WY, Lim YC, Ussif A, Singh R, Shahmalak U, et al. Primary-level worker interventions for the care of people living with mental disorders and distress in low- and middle-income countries. Cochrane Db Syst Rev. 2021;8:CD009149.
MacDonald S, Sampson C, Turley R, Biddle L, Ring N, Begley R, et al. Patients’ experiences of emergency hospital care following self-harm: systematic review and thematic synthesis of qualitative research. Qual Health Res. 2020;30:471–85.
Why Does Bullying Happen? Better Help. 2024. https://www.betterhelp.com. Accessed 18 July 2024.
Shinde S, Weiss HA, Khandeparkar P, Pereira B, Sharma A, Gupta R, et al. A multicomponent secondary school health promotion intervention and adolescent health: an extension of the SEHER cluster randomised controlled trial in Bihar, India. PLoS Med. 2020;17:e1003021.
Mok PLH, Antonsen S, Pedersen CB, Carr MJ, Kapur N, Nazroo J, et al. Family income inequalities and trajectories through childhood and self-harm and violence in young adults: a population-based, nested case-control study. Lancet Public Health. 2018;3:e498–e507.
Chen M, Zhou Y, Luo D, Yan S, Liu M, Wang M, et al. Association of family function and suicide risk in teenagers with a history of self-harm behaviors: mediating role of subjective wellbeing and depression. Front Public Health. 2023;11:1164999.
McConkey R, O’Hagan P, Corcoran J. The impact of a family-centred intervention for parents of children with developmental disabilities: a model project in rural Ireland. Children. 2023;10:175.
Cottrell DJ, Wright-Hughes A, Collinson M, Boston P, Eisler I, Fortune S, et al. Effectiveness of systemic family therapy versus treatment as usual for young people after self-harm: a pragmatic, phase 3, multicentre, randomised controlled trial. Lancet Psychiatry. 2018;5:203–16.
Florindo Salvador V, Gouveia-Pereira M, Simões B, Duarte E. Young adults who self-harm: Barriers to and facilitators of seeking help. Psychiatry Res. 2023;327:115390.
Strobel NA, Chamberlain C, Campbell SK, Shields L, Bainbridge RG, Adams C, et al. Family-centred interventions for Indigenous early childhood well-being by primary healthcare services. Cochrane Database Syst Rev. 2022;12:CD012463.
Lonergan A, Moriarty A, McNicholas F, Byrne T. Cyberbullying and internet safety: a survey of child and adolescent mental health practitioners. Ir J Psychol Med. 2023;40:43–50.
Gini G, Espelage DL. Peer victimization, cyberbullying, and suicide risk in children and adolescents. JAMA. 2014;312:545–6.
Kruzan KP, Whitlock J, Chapman J, Bhandari A, Bazarova N. Young adults’ perceptions of 2 publicly available digital resources for self-injury: qualitative study of a peer support app and web-based factsheets. JMIR Form Res. 2023;7:e41546.
Mann JJ, Michel CA, Auerbach RP. Improving suicide prevention through evidence-based strategies: a systematic review. Am J Psychiatry. 2021;178:611–24.
Meng S, Dong P, Sun Y, Li Y, Chang X, Sun G, et al. Guidelines for prevention and treatment of internet addiction in adolescents during home quarantine for the COVID-19 pandemic. Heart Mind. 2020;4:95.
Ozbay FA, Alatas B. Fake news detection within online social media using supervised artificial intelligence algorithms. Phys A: Stat Mech Its Appl. 2020;540:123174.
Dewani A, Memon MA, Bhatti S. Cyberbullying detection: advanced preprocessing techniques & deep learning architecture for Roman Urdu data. J Big Data. 2021;8:160.
Yadav J, Kumar D, Chauhan D Cyberbullying detection using pre-trained BERT model. 2020 International Conference on Electronics and Sustainable Communication Systems (ICESC), 2020. p. 1096–1100.
Perera A, Fernando P. Accurate cyberbullying detection and prevention on social Media. Procedia Comput Sci. 2021;181:605–11.
Wang D, Zhang M, Mujumdar AS, Yu D. Advanced detection techniques using artificial intelligence in processing of berries. Food Eng Rev. 2022;14:176–99.
Vos T, Lim SS, Abbafati C, Abbas KM, Abbasi M, Abbasifard M, et al. Global burden of 369 diseases and injuries in 204 countries and territories, 1990–2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet. 2020;396:1204–22.
Self-harm and Suicide Prevention Competence Framework. https://www.ucl.ac.uk/pals/research/clinical-educational-and-health-psychology/research-groups/core/competence-frameworks/self. Accessed 5 June 2024.
Sun Y, Bao Y, Ravindran A, Sun Y, Shi J, Lu L. Mental health challenges raised by rapid socioeconomic transformations in China: lessons learned and prevention strategies. Heart Mind. 2020;4:59.
Richardson R, Connell T, Foster M, Blamires J, Keshoor S, Moir C, et al. Risk and protective factors of self-harm and suicidality in adolescents: an umbrella review with meta-analysis. J Youth Adolescence. 2024;53:1301–22.
Acknowledgements
We wish to thank Prof. Paul Moran, Prof. Ian B Hickie and Prof. Arun Ravindran, who generously shared their experience and perspectives with us.
Funding
This work was supported in part by the Brain Science and Brain-like Intelligence Technology-National Science and Technology Major Project (2021ZD0200800, 2021ZD0200700), National Key Research and Development Project of China (2024YFC2707804), and National Natural Science Foundation of China (no. 82288101, 82301681, 82171514).
Author information
Authors and Affiliations
Contributions
L Lu, YP Bao, XX Liu, and Y Zhong proposed the topic of the meta-analysis. Y Zhong, ZW Zhang, JH Ding, YB Zheng, YF Yu and ZC Guan performed the literature search, data curation, and data visualization. Y Zhong, ZW Zhang, and JH Ding wrote the original manuscript, and XX Liu, YP Bao, D Wasserman and L Lu checked the data and critically revised the manuscript. YB Zheng, SZ Su, W Yan, J Sun, YF Yu, ZC Guan, YM Gong, Z Wang, WF Mi, YM Wang, L Shi, YK Sun, A Javed, and D Wasserman commented on and revised the manuscript. All authors were involved in reviewing and editing the manuscript.
Corresponding authors
Ethics declarations
Competing interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhong, Y., Zhang, ZW., Ding, JH. et al. What are the correlates of non-suicidal self-injury in children and adolescents? An umbrella systematic review of global evidence. Mol Psychiatry (2026). https://doi.org/10.1038/s41380-026-03605-4
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41380-026-03605-4