Abstract
Background
BMI as a body weight indicator, may inadequately represent the biological effect of body fat on lipid profiles. This study aims to assess whether body fat indicators were superior to BMI for recognizing children with dyslipidemia.
Methods
A nationwide cross-sectional study involving 8944 pediatric participants aged 6–18 years. Measures of fat mass index (FMI), fat mass percentage (FMP), BMI, and four lipid profiles were obtained.
Results
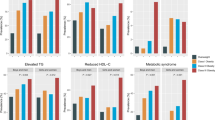
Among boys, the standard multi-linear regression coefficients of FMI for TC, LDL-C, and TG were higher than those of BMI (P < 0.01), but not for HDL-C. Also, the prevalence ratios and area under curves (AUCs) of excess fat classified by FMI for specific abnormal lipid profiles (except for HDL-C) were greater than overweight classified by BMI. The AUCs for detecting children with abnormal TC, LDL-C, and TG of FMI-based excess fat were 3.9%, 5.6%, and 2.8% higher than those of BMI-based overweight, respectively, all P < 0.01. Among girls, the associations of BMI with lipid profiles were substantially similar to FMI. All these results were almost identical when FMP was used instead of FMI.
Conclusions
DXA measured body fat performs better than BMI in identifying abnormal lipid profiles in boys but not in girls.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Joshi, S. M. et al. Tracking of cardiovascular risk factors from childhood to young adulthood - the Pune Children’s Study. Int. J. Cardiol. 175, 176–178 (2014).
Juhola, J. et al. Tracking of serum lipid levels, blood pressure, and body mass index from childhood to adulthood: the Cardiovascular Risk in Young Finns Study. J. Pediatr. 159, 584–590 (2011).
Haney, E. M. et al. Screening and treatment for lipid disorders in children and adolescents: systematic evidence review for the US Preventive Services Task Force. Pediatrics 120, e189–e214 (2007).
Gazzola, K., Reeskamp, L. & van den Born, B. J. Ethnicity, lipids and cardiovascular disease. Curr. Opin. Lipidol. 28, 225–230 (2017).
Eslami, A. et al. Sex-specific incidence rates and risk factors of premature cardiovascular disease. A long term follow up of the Tehran Lipid and Glucose Study. Int. J. Cardiol. 227, 826–832 (2017).
Centers for Disease Control and Prevention (CDC). Prevalence of abnormal lipid levels among youths --- United States, 1999-2006. MMWR Morb. Mortal Wkly Rep. 59, 29–33 (2010).
Nogueira-de-Almeida, C. A. & Mello, E. D. Correlation of body mass index Z-scores with glucose and lipid profiles among overweight and obese children and adolescents. J. Pediatr. 94, 308–312 (2017).
Boyd, G. S. et al. Effect of obesity and high blood pressure on plasma lipid levels in children and adolescents. Pediatrics 116, 442–446 (2005).
Lipsky, L. M. et al. Body mass index and adiposity indicators associated with cardiovascular biomarkers in youth with type 1 diabetes followed prospectively. Pediatr. Obes. 12, 468–476 (2017).
Daniels, S. R. & Greer, F. R. Committee on N. Lipid screening and cardiovascular health in childhood. Pediatrics 122, 198–208 (2008).
Expert Panel on Integrated Guidelines for Cardiovascular Health and Risk Reduction in Children and Adolescents, National Heart, Lung, and Blood Institute. Expert panel on integrated guidelines for cardiovascular health and risk reduction in children and adolescents: summary report. Pediatrics 128(Suppl 5), S213–S256 (2011).
Mechanick, J. I., Hurley, D. L. & Garvey, W. T. Adiposity-based chronic disease as a new diagnostic term: the American Association of Clinical Endocrinologists and American College of Endocrinology Position Statement. Endocr. Pract. 23, 372–378 (2017).
Romero-Corral, A. et al. Accuracy of body mass index in diagnosing obesity in the adult general population. Int J. Obes. 32, 959–966 (2008).
Wells, J. C. Sexual dimorphism of body composition. Best. Pract. Res. Clin. Endocrinol. Metab. 21, 415–430 (2007).
Borrud, L. G. et al. Body composition data for individuals 8 years of age and older: U.S. population, 1999-2004. Vital. Health Stat. 11, 1–87 (2010).
Lamb, M. M. et al. Association of body fat percentage with lipid concentrations in children and adolescents: United States, 1999-2004. Am. J. Clin. Nutr. 94, 877–883 (2011).
Lee, J. M. et al. Poor performance of body mass index as a marker for hypercholesterolemia in children and adolescents. Arch. Pediatr. Adolesc. Med. 163, 716–723 (2009).
Daniels, S. R. Lipid concentrations in children and adolescents: it is not all about obesity. Am. J. Clin. Nutr. 94, 699–700 (2011).
Liu, J. et al. Bone mineral density reference standards for Chinese children aged 3-18: cross-sectional results of the 2013-2015 China Child and Adolescent Cardiovascular Health (CCACH) Study. BMJ Open 7, e014542 (2017).
Dong, H., et al. Alarming trends in ideal cardiovascular health among children and adolescents in Beijing, China, 2004 to 2014. Int. J. Cardiol. 231, 264–270 (2017).
de Onis, M. et al. Development of a WHO growth reference for school-aged children and adolescents. Bull. World Health Organ. 85, 660–667 (2007).
Baim, S. et al. Official positions of the International Society for Clinical Densitometry and executive summary of the 2007 ISCD Pediatric Position Development Conference. J. Clin. Densitom. 11, 6–21 (2008).
Ma, H. M. et al. Pubertal development timing in urban Chinese boys. Int. J. Androl. 34, e435–e445 (2011).
Sun, Y. et al. National estimates of the pubertal milestones among urban and rural Chinese girls. J. Adolesc. Health 51, 279–284 (2012).
Johnson, R. W. An introduction to the bootstrap. Teach. Stat. 23, 49–54 (2001).
Deddens, J. A. & Petersen, M. R. Approaches for estimating prevalence ratios. Occup. Environ. Med. 65, 501–506 (2008).
Oliosa, P. R., et al. Body fat percentage is better than indicators of weight status to identify children and adolescents with unfavorable lipid profile. J. Pediatr. (RioJ). 95, 112–118 (2019). https://doi.org/10.1016/j.jped.2017.11.003.
Bijari, B. et al. The relationship between serum lipids and obesity among elementary school in Birjand: a case control study. J. Res Health Sci. 15, 83–87 (2015).
de Quadros, T. M. B. et al. Predictive capacity of anthropometric indicators for dyslipidemia screening in children and adolescents. J. Pediatr. 91, 455–463 (2015).
Pinhas-Hamiel, O. et al. Lipid and insulin levels in obese children: changes with age and puberty. Obesity 15, 2825–2831 (2007).
Jois, A. et al. Relationship of high leptin levels with an adverse lipid and insulin profile in 6-8 year-old children in Spain. Nutr. Metab. Cardiovasc. Dis. 25, 1111–1116 (2015).
Bohn, B. et al. BMI or BIA: is body mass index or body fat mass a better predictor of cardiovascular risk in overweight or obese children and adolescents? A German/Austrian/Swiss Multicenter APV analysis of 3,327 children and adolescents. Obes. Facts 8, 156–165 (2015).
Araujo, A. J., Santos, A. C. & Prado, W. L. Body composition of obese adolescents: association between adiposity indicators and cardiometabolic risk factors. J. Hum. Nutr. Diet. 30, 193–202 (2017).
Bauer, J. et al. Dual-energy X-ray absorptiometry prediction of adipose tissue depots in children and adolescents. Pediatr. Res. 72, 420–425 (2012).
Lemos, T. & Gallagher, D. Current body composition measurement techniques. Curr. Opin. Endocrinol. Diabetes Obes. 24, 310–314 (2017).
Min, K. B. & Min, J. Y. Android and gynoid fat percentages and serum lipid levels in United States adults. Clin. Endocrinol. 82, 377–387 (2015).
Elffers, T. W. et al. Body fat distribution, in particular visceral fat, is associated with cardiometabolic risk factors in obese women. PLoS ONE 12, e0185403 (2017).
Pellegrini, M. et al. Role of the sex hormone estrogen in the prevention of lipid disorder. Curr. Med. Chem. 21, 2734–2742 (2014).
Jolliffe, C. J. & Janssen, I. Distribution of lipoproteins by age and gender in adolescents. Circulation 114, 1056–1062 (2006).
Klop, B., Elte, J. W. & Cabezas, M. C. Dyslipidemia in obesity: mechanisms and potential targets. Nutrients 5, 1218–1240 (2013).
Acknowledgements
We thank the other investigators, the staff, and the participants of the CCACH study for their valuable contributions. The study was supported by grants from the “Twelfth Five Year Plan” of the China National Science and Technology (2012BAI03B03), the National Key Research and Development Program of China (2016YFC1300101, 2016YFC0900602), and the Beijing Training Project for the Leading Talents in Science and Technology (2011LJ07).
China Child and Adolescent Cardiovascular Health (CCACH) Collaboration Group
Hong Cheng3, Guimin Huang3, Dongqing Hou3, Fangfang Chen3, Wenpeng Wang3, Feng Xiong5, Jinghui Sun6, Wenqing Ding7, Weili Yan8, Bo Xi9
Author information
Authors and Affiliations
Consortia
Contributions
H.L., J.M., T.H., and Y.Y. conceptualized the study concept and design. J.M., J.L., Y.Y., and X.Z. conducted research; H.L., J.M., and P.X. analyzed the data; and H.L., J.M., T.H., and Y.Y. drafted the manuscript. All authors were involved in writing the paper and had final approval of the submitted and published versions.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Li, H., Huang, T., Liu, J. et al. Body fat indicators perform better than body mass index in identifying abnormal lipid profiles in boys but not in girls. Pediatr Res 85, 617–624 (2019). https://doi.org/10.1038/s41390-019-0287-x
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41390-019-0287-x