Abstract
Background
Inflammatory bowel diseases are associated with various immune- and non-immune-mediated conditions. We aimed to assess the association of inflammatory bowel diseases with comorbidities at late adolescence.
Methods
Jewish Israeli adolescents who underwent a general health evaluation prior to enlistment to the Israeli Defense Forces from 2002 to 2016 were included.
Results
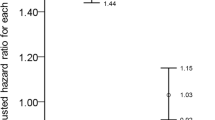
Overall, 891 subjects (595 Crohn’s disease, 296 ulcerative colitis, median age 17.1 years) and 1,141,841 controls were analyzed. Crohn’s disease was associated with arthritis (odds ratio (OR) 4.7, 95% confidence interval (CI) 2.4–9.1), thyroid disease (OR 2.6, 95% CI 1.2–5.5), atopic dermatitis (OR 2, 95% CI 1.1–3.6), autoimmune hepatitis (OR 4.4, 95% CI 2.3–8.6), nephrolithiasis (OR 3.6, 95% CI 1.2–11.4), and pancreatitis (OR 41.8, 95% CI 17.2–101.9). Ulcerative colitis was associated with arthritis (OR 3.6, 95% CI 1.0–9.8), thyroid disease (OR 4.8, 95% CI 1.2–19.4), autoimmune hepatitis (OR 8, 95% CI 4–16.2), and pancreatitis (OR 51, 95% CI 16.1–158.9). Primary sclerosing cholangitis was associated with both diseases. Asthma, celiac, type 1 diabetes, psoriasis, and bone fractures were not more common in both diseases. Male predominance was noted for most associations.
Conclusions
At adolescence, both Crohn’s disease and ulcerative colitis are associated with multiple comorbidities, not limited to autoimmune disorders.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Davidson, A. & Diamond, B. Autoimmune diseases. N. Engl. J. Med. 345, 340–350 (2001).
Kappelman, M. D. et al. Association of paediatric inflammatory bowel disease with other immune-mediated diseases. Arch. Dis. Child. 96, 1042–1046 (2011).
Bernstein, C. N., Wajda, A. & Blanchard, J. F. The clustering of other chronic inflammatory diseases in inflammatory bowel disease: a population-based study. Gastroenterology 129, 827–836 (2005).
Peng, Y. H. et al. Association of inflammatory bowel disease with asthma risk: a nationwide cohort study. Allergy Asthma Proc. 36, e92–e98 (2015).
Haapamäki, J. et al. Increased risk for coronary heart disease, asthma, and connective tissue diseases in inflammatory bowel disease. J. Crohns Colitis 5, 41–47 (2011).
Assa, A. et al. Large population study shows that adolescents with celiac disease have an increased risk of multiple autoimmune and nonautoimmune comorbidities. Acta Paediatr. 106, 967–972 (2017).
Hwang, C., Ross, V. & Mahadevan, U. Micronutrient deficiencies in inflammatory bowel disease: from A to zinc. Inflamm. Bowel Dis. 18, 1961–1981 (2012).
Caudarella, R. et al. Renal stone formation in patients with inflammatory bowel disease. Scanning Microsc. 7, 371–379 (1993).
Scoville, E. A. et al. Venous thromboembolism in patients with inflammatory bowel diseases: a case-control study of risk factors. Inflamm. Bowel Dis. 20, 631–636 (2014).
Fumery, M. et al. Thromboembolic events and cardiovascular mortality in inflammatory bowel diseases: a meta-analysis of observational studies. J. Crohns Colitis 8, 469–479 (2014).
Bessissow, T. et al. Incidence and predictors of nonalcoholic fatty liver disease by serum biomarkers in patients with inflammatory bowel disease. Inflamm. Bowel Dis. 22, 1937–1944 (2016).
Bähler, C. et al. Chronic comorbidities associated with inflammatory bowel disease: prevalence and impact on healthcare costs in Switzerland. Eur. J. Gastroenterol. Hepatol. 29, 916–925 (2017).
Lin, J. C. et al. Association between Parkinson’s disease and inflammatory bowel disease: a nationwide Taiwanese retrospective cohort study. Inflamm. Bowel Dis. 22, 1049–1055 (2016).
Bar Yehuda, S. et al. The association of Inflammatory Bowel diseases with autoimmune disorders: a population-based report from the epi-IIRN. J. Crohns Colitis 13, 324–329 (2019).
Halling, M. L. et al. Patients with inflammatory bowel disease have increased risk of autoimmune and inflammatory diseases. World J. Gastroenterol. 23, 6137–6146 (2017).
Wilson, J. C. et al. Inflammatory bowel disease and the risk of autoimmune diseases. J. Crohns Colitis 10, 186–193 (2016).
Shizuma, T. Concomitant thyroid disorders and inflammatory bowel disease: a literature review. Biomed. Res. Int. 2016, 5187061 (2016).
Vavricka, S. R. et al. Extraintestinal manifestations of inflammatory bowel disease. Inflamm. Bowel Dis. 21, 1982–1992 (2015).
Burisch, J., Jess, T., Martinato, M., Lakatos, P. L. & ECCO-EpiCom. The burden of inflammatory bowel disease in Europe. J. Crohns Colitis 7, 322–337 (2013).
Cohen, R. et al. Autoimmune disease concomitance among inflammatory bowel disease patients in the United States, 2001-2002. Inflamm. Bowel Dis. 14, 738–743 (2008).
Shah, A. et al. Link between celiac disease and inflammatory bowel disease. J. Clin. Gastroenterol. 53, 514–522 (2019)
Alper, A., Rojas-Velasquez, D. & Pashankar, D. S. Prevalence of anti-tissue transglutaminase antibodies and celiac disease in children with inflammatory bowel disease. J. Pediatr. Gastroenterol. Nutr. 66, 934–936 (2018).
Kuenzig, M. E. et al. Co-occurrence of asthma and the inflammatory bowel diseases: a systematic review and meta-analysis. Clin. Transl. Gastroenterol. 9, 188 (2018).
El-Serag, H. B. et al. The renal and urologic complications of inflammatory bowel disease. Inflamm. Bowel Dis. 3, 217–224 (1997).
Stark, C. M., Gorman, G. H. & Nylund, C. M. Association of inflammatory bowel disease and urolithiasis in hospitalized pediatric patients. Inflamm. Bowel Dis. 23, 1777–1782 (2017).
Gaspar, S. R. et al. Urolithiasis and crohn’s disease. Urol. Ann. 8, 297–304 (2016).
Srinath, A. I., Gupta, N. & Husain, S. Z. Probing the association of pancreatitis in inflammatory bowel disease. Inflamm. Bowel Dis. 22, 465–475 (2016).
Ramos, L. R. et al. Inflammatory bowel disease and pancreatitis: a review. J. Crohns Colitis 10, 95–104 (2016).
Guz-Mark, A. et al. Pediatric-onset inflammatory bowel disease poses risk for low bone mineral density at early adulthood. Dig. Liver Dis. 49, 639–642 (2017).
Walldorf, J. et al. Health care for osteoporosis in inflammatory bowel disease: unmet needs in care of male patients? J. Crohns Colitis 7, 901–907 (2013).
Bernstein, C. N. & Leslie, W. D. Review article: Osteoporosis and inflammatory bowel disease. Aliment. Pharm. Ther. 19, 941–952 (2004).
Targownik, L. E., Bernstein, C. N. & Leslie, W. D. Inflammatory bowel disease and the risk of osteoporosis and fracture. Maturitas 76, 315–319 (2013).
Terzoudis, S. et al. Increased fracture risk assessed by fracture risk assessment tool in Greek patients with Crohn’s disease. Dig. Dis. Sci. 58, 216–221 (2013).
Greenley, R. N. et al. Sports participation in youth with inflammatory bowel diseases: the role of disease activity and subjective physical health symptoms. Inflamm. Bowel Dis. 24, 247–253 (2018).
Dimitrova, A. K. et al. Prevalence of migraine in patients with celiac disease and inflammatory bowel disease. Headache 53, 344–355 (2013).
Moisset, X. et al. Migraine prevalence in inflammatory bowel disease patients: a tertiary-care centre cross-sectional study. Eur. J. Pain 21, 1550–1560 (2017).
Fraga, M. et al. Primary sclerosing cholangitis in the Swiss Inflammatory Bowel Disease Cohort Study: prevalence, risk factors, and long-term follow-up. Eur. J. Gastroenterol. Hepatol. 29, 91–97 (2017).
Kaplan, G. G. et al. Risk of comorbidities on postoperative outcomes in patients with inflammatory bowel disease. Arch. Surg. 146, 959–964 (2011).
Acknowledgements
Statistical analysis was performed by Dr. Ron Kedem (PhD), Statistician, Medical Corps, Israel Defense Force, Israel.
Author information
Authors and Affiliations
Contributions
I.G. acquired and analyzed the data and drafted the manuscript. L.H.K., S.D., and R.S. have participated in study design and critically reviewed the manuscript. A.A. was responsible for study conceptualization and design, participated in data analysis, and critically reviewed the manuscript. All authors approve the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ghersin, I., Khateeb, N., Katz, L.H. et al. Comorbidities in adolescents with inflammatory bowel disease: findings from a population-based cohort study. Pediatr Res 87, 1256–1262 (2020). https://doi.org/10.1038/s41390-019-0702-3
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41390-019-0702-3