Abstract
Background
Follow-up of very preterm infants is essential for reducing risks of health and developmental problems and relies on parental engagement. We investigated parents’ perceptions of post-discharge healthcare for their children born very preterm in a European multi-country cohort study.
Methods
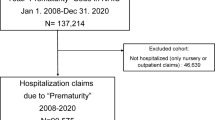
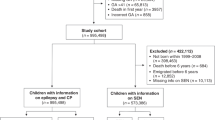
Data come from a 5-year follow-up of an area-based cohort of births <32 weeks’ gestation in 19 regions from 11 European countries. Perinatal data were collected from medical records and 5-year data from parent-report questionnaires. Parents rated post-discharge care related to their children’s preterm birth (poor/fair/good/excellent) and provided free-text suggestions for improvements. We analyzed sociodemographic and medical factors associated with poor/fair ratings, using inverse probability weights to adjust for attrition bias, and assessed free-text responses using thematic analysis.
Results
Questionnaires were returned for 3635 children (53.8% response rate). Care was rated as poor/fair for 14.2% [from 6.1% (France) to 31.6% (Denmark)]; rates were higher when children had health or developmental problems (e.g. cerebral palsy (34.4%) or epilepsy (36.9%)). From 971 responses, 4 themes and 25 subthemes concerning care improvement were identified.
Conclusions
Parents’ experiences provide guidance for improving very preterm children’s post-discharge care; this is a priority for children with health and developmental problems as parental dissatisfaction was high.
Impact
-
In a European population-based very preterm birth cohort, parents rated post-discharge healthcare as poor or fair for 14.2% of children, with a wide variation (6.1–31.6%) between countries.
-
Dissatisfaction was reported in over one-third of cases when children had health or developmental difficulties, such as epilepsy or cerebral palsy.
-
Parents’ free-text suggestions for improving preterm-related post-discharge healthcare were similar across countries; these focused primarily on better communication with parents and better coordination of care.
-
Parents’ lived experiences are a valuable resource for understanding where care improvements are needed and should be included in future research.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Delnord, M. et al. Variations in very preterm birth rates in 30 high-income countries: are valid international comparisons possible using routine data? BJOG 124, 785–794 (2017).
Blencowe, H. et al. National, regional, and worldwide estimates of preterm birth rates in the year 2010 with time trends since 1990 for selected countries: a systematic analysis and implications. Lancet 379, 2162–2172 (2012).
Saigal, S. & Doyle, L. W. An overview of mortality and sequelae of preterm birth from infancy to adulthood. Lancet 371, 261–269 (2008).
Synnes, A. et al. Determinants of developmental outcomes in a very preterm Canadian cohort. Arch. Dis. Child. Fetal Neonatal Ed. 102, F235–F234 (2017).
McManus, B. M., Richardson, Z., Schenkman, M., Murphy, N. & Morrato, E. H. Timing and intensity of early intervention service use and outcomes among a safety-net population of children. JAMA Netw. Open 2, e187529 (2019).
Little, A. A., Kamholz, K., Corwin, B. K., Barrero-Castillero, A. & Wang, C. J. Understanding barriers to early intervention services for preterm infants: lessons from two states. Acad. Pediatr. 15, 430–438 (2015).
Gustavsson, S., Gremyr, I. & Kenne Sarenmalm, E. Designing quality of care-contributions from parents: parents’ experiences of care processes in paediatric care and their contribution to improvements of the care process in collaboration with healthcare professionals. J. Clin. Nurs. 25, 742–751 (2016).
Junewicz, A. & Youngner, S. J. Patient-satisfaction surveys on a scale of 0 to 10: improving health care, or leading it astray? Hastings Cent. Rep. 45, 43–51 (2015).
Rucci, P. et al. Measuring parents’ perspective on continuity of care in children with special health care needs. Int. J. Integr. Care 15, e046 (2015).
Pritchard, M. A., Colditz, P. B., Beller, E. M. & Queensland Optimising Preterm Infant Outcomes Group. Parental experiences and preferences which influence subsequent use of post-discharge health services for children born very preterm. J. Paediatr. Child Health 44, 281–284 (2008).
Spittle, A., Orton, J., Anderson, P., Boyd, R. & Doyle, L. W. Early developmental intervention programmes post-hospital discharge to prevent motor and cognitive impairments in preterm infants. Cochrane Database Syst. Rev. 12, CD005495 (2012).
Benzies, K. M., Magill-Evans, J. E., Hayden, K. A. & Ballantyne, M. Key components of early intervention programs for preterm infants and their parents: a systematic review and meta-analysis. BMC Pregnancy Childbirth 13, S10 (2013).
Spittle, A. J., Treyvaud, K., Lee, K. J., Anderson, P. J. & Doyle, L. W. The role of social risk in an early preventative care programme for infants born very preterm: a randomized controlled trial. Dev. Med. Child Neurol. 60, 54–62 (2018).
Ballantyne, M., Benzies, K. M., Rosenbaum, P. & Lodha, A. Mothers’ and health care providers’ perspectives of the barriers and facilitators to attendance at Canadian neonatal follow-up programs. Child Care Health Dev. 41, 722–733 (2015).
Callanan, C. et al. Children followed with difficulty: how do they differ? J. Paediatr. Child Health 37, 152–156 (2001).
Butt, M. L., Pinelli, J. & Hunsberger, M. Parents’ perceptions of ambulatory neonatal follow-up programs. J. Neonatal Nurs. 16, 126–137 (2010).
Hagen, I. H., Iversen, V. C., Nesset, E., Orner, R. & Svindseth, M. F. Parental satisfaction with neonatal intensive care units: a quantitative cross-sectional study. BMC Health Serv. Res. 19, 37 (2019).
McIntyre, L. L. & Zemantic, P. K. Examining services for young children with autism spectrum disorder: parent satisfaction and predictors of service utilization. Early Child. Educ. J. 45, 727–734 (2017).
Zeitlin, J. et al. Cohort profile: Effective Perinatal Intensive Care in Europe (EPICE) very preterm birth cohort. Int. J. Epidemiol. 49, 372–386 (2020).
Zeitlin, J. et al. Use of evidence based practices to improve survival without severe morbidity for very preterm infants: results from the EPICE population based cohort. BMJ 354, i2976 (2016).
Sentenac, M. et al. Maternal education and language development at 2 years corrected age in children born very preterm: results from a European population-based cohort study. J. Epidemiol. Community Health 74, 346–353 (2020).
Monier, I. et al. Fetal and neonatal outcomes of preterm infants born before 32 weeks of gestation according to antenatal vs postnatal assessments of restricted growth. Am. J. Obstet. Gynecol. 216, 516 e511–516 e510 (2017).
Seppanen, A. V. et al. Specialist health care services use in a European cohort of infants born very preterm. Dev. Med. Child Neurol. 61, 832–839 (2019).
Cummings, P. Methods for estimating adjusted risk ratios. Stata J. 9, 175–196 (2009).
Seaman, S. R., White, I. R., Copas, A. J. & Li, L. Combining multiple imputation and inverse-probability weighting. Biometrics 68, 129–137 (2012).
Bonnet, C. et al. Low breastfeeding continuation to 6 months for very preterm infants: a European multiregional cohort study. Matern. Child Nutr. 15, e12657 (2018).
Johnson, S. et al. Neurodevelopmental outcomes following late and moderate prematurity: a population-based cohort study. Arch. Dis. Child. Fetal Neonatal Ed. 100, F301–F308 (2015).
Larkin, P. J., Dierckx de Casterle, B. & Schotsmans, P. Multilingual translation issues in qualitative research: reflections on a metaphorical process. Qual. Health Res. 17, 468–476 (2007).
Esposito, N. From meaning to meaning: the influence of translation techniques on non-English focus group research. Qual. Health Res. 11, 568–579 (2001).
MacBean, V., Drysdale, S. B., Zivanovic, S., Peacock, J. L. & Greenough, A. Participant retention in follow-up studies of prematurely born children. BMC Public Health 19, 1233 (2019).
European Commission. State of health in the EU: Companion report 2017. https://ec.europa.eu/health/sites/health/files/state/docs/2017_companion_en.pdf (2017). Accessed 2 Aug 2020.
Stepurko, T., Pavlova, M. & Groot, W. Overall satisfaction of health care users with the quality of and access to health care services: a cross-sectional study in six Central and Eastern European countries. BMC Health Serv. Res. 16, 342 (2016).
Wendt, C., Kohl, J., Mischke, M. & Pfeifer, M. How do Europeans perceive their healthcare system? patterns of satisfaction and preference for state involvement in the field of healthcare. Eur. Sociol. Rev. 26, 177–192 (2009).
Bleich, S. N., Ozaltin, E. & Murray, C. K. How does satisfaction with the health-care system relate to patient experience? Bull. World Health Organ. 87, 271–278 (2009).
Galle, A., Van Parys, A. S., Roelens, K. & Keygnaert, I. Expectations and satisfaction with antenatal care among pregnant women with a focus on vulnerable groups: a descriptive study in Ghent. BMC Womens Health 15, 112 (2015).
de Silva, A. A framework for measuring responsiveness. GPE Discussion Paper Series: No. 32. https://www.who.int/responsiveness/papers/paper32.pdf?ua=1 (2000). Accessed 2 Aug 2020.
Kowalewski, M. Dissatisfied and critical citizens: the political effect of complaining. Society 56, 453–460 (2019).
Papanicolas, I., Cylus, J. & Smith, P. C. An analysis of survey data from eleven countries finds that ‘satisfaction’ with health system performance means many things. Health Aff. 32, 734–742 (2013).
Butt, M. L. et al. Development and evaluation of an instrument to measure parental satisfaction with quality of care in neonatal follow-up. J. Dev. Behav. Pediatr. 30, 57–65 (2009).
Tran, V.-T., Riveros, C., Péan, C., Czarnobroda, A. & Ravaud, P. Patients’ perspective on how to improve the care of people with chronic conditions in France: a citizen science study within the ComPaRe e-cohort. BMJ Qual. Saf. 28, 875–886 (2019).
Chang, J. T. et al. Patients’ global ratings of their health care are not associated with the technical quality of their care. Ann. Intern. Med. 144, 665–672 (2006).
Brenner, M. et al. Management and integration of care for children living with complex care needs at the acute-community interface in Europe. Lancet Child Adolesc. Health 2, 822–831 (2018).
Brenner, M. et al. Children’s complex care needs: a systematic concept analysis of multidisciplinary language. Eur. J. Pediatr. 177, 1641–1652 (2018).
EFCNI, van Kempen, A., van Steenbrugge, G., van Wassenaer-Leemhuis, A. & Wolke, D. European Standards of Care for Newborn Health: coordination and integration of care after discharge home. https://newborn-health-standards.org/wp-content/uploads/2019/04/TEG_Follow_up_complete.pdf (2018). Accessed 6 Apr 2020.
EFCNI, Jaekel, J., Johnson, S., Wolke, D. & van Wassenaer-Leemhuis, A. European Standards of Care for Newborn Health: meeting special needs at school. https://newborn-health-standards.org/wp-content/uploads/2019/04/TEG_Follow_up_complete.pdf (2018). Accessed 6 Apr 2020.
EFCNI, Houtzager, B. A., van Wassenaer-Leemhuis, A., Wolke, D. & Virchez, M. European Standards of Care for Newborn Health: parental mental health. https://newborn-health-standards.org/wp-content/uploads/2019/04/TEG_Follow_up_complete.pdf (2018). Accessed 6 Apr 2020.
Acknowledgements
The research received funding from the European Union’s Horizon 2020 Research and Innovation Programme under grant agreement No. 633724. A.-V.S. has a doctoral contract funded by Sorbonne Université Collège Doctoral, Paris, France.
Author information
Authors and Affiliations
Consortia
Contributions
A.-V.S., E.S.D., L.T., R.E.R., S.P., H.P., M.C., J.Z., and the SHIPS Research Group made substantial contributions to conception and design and acquisition of data. A.-V.S., P.S., and J.Z. analyzed the data. A.-V.S., P.S., E.S.D., L.T., R.E.R., S.P., H.P., L.J.I.Z., M.C., and J.Z. contributed to interpretation of data, drafting the article, revising it critically for important intellectual content, and approved the final version to be published. Members of the SHIPS research group approved the final version to be published.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Patient consent
Ethics approvals and parental consent were obtained according to national legislation in each country before data collection.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Seppänen, AV., Sauvegrain, P., Draper, E.S. et al. Parents’ ratings of post-discharge healthcare for their children born very preterm and their suggestions for improvement: a European cohort study. Pediatr Res 89, 1004–1012 (2021). https://doi.org/10.1038/s41390-020-01120-y
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41390-020-01120-y
This article is cited by
-
Neonatal neurodevelopmental follow-up in the UK: a survey of current practice and future recommendations
BMC Pediatrics (2025)
-
Hospital-to-home transitions for children with medical complexity: part 1, a systematic review of reported outcomes
European Journal of Pediatrics (2023)
-
Hospital-to-home transitions for children with medical complexity: part 2—a core outcome set
European Journal of Pediatrics (2023)
-
Risk factors for cerebral palsy and movement difficulties in 5-year-old children born extremely preterm
Pediatric Research (2023)
-
Families’ perspectives on monitoring infants’ health and development after discharge from NICUs
Pediatric Research (2021)