Abstract
Background
Neonatal sepsis is a leading cause of neonatal morbidity and mortality, associated with immunosuppression. Myeloid-derived suppressor cells (MDSCs) are cells with immunosuppressive activity, present in high amounts in cord blood. Mechanisms regulating MDSC expansion are incompletely understood. Adenosine is a metabolite with immunoregulatory effects that are elevated in cord blood.
Methods
Impact of adenosine on peripheral and cord blood mononuclear cells (PBMCs and CBMCs) was analysed by quantification of ectonucleotidases and adenosine receptor expression, MDSC induction from PBMCs and CBMCs, their suppressive capacity on T cell proliferation and effector enzyme expression by flow cytometry.
Results
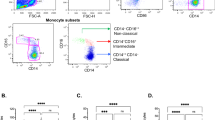
Cord blood monocytes mainly expressed CD39, while cord blood T cells expressed CD73. Adenosine-induced MDSCs from PBMCs induced indoleamine-2,3-dioxygenase (IDO) expression and enhanced arginase I expression in monocytes. Concerted action of IDO and ArgI led to effective inhibition of T cell proliferation. In addition, adenosine upregulated inhibitory A3 receptors on monocytes.
Conclusion
Adenosine acts by inducing MDSCs and upregulating inhibitory A3 receptors, probably as a mode of autoregulation. Thus, adenosine contributes to immunosuppressive status and may be a target for immunomodulation during pre- and postnatal development.
Impact
-
Immune effector cells, that is, monocytes, T cells and MDSCs from cord blood express ectonucleotidases CD39 and CD73 and may thus serve as a source for adenosine as an immunomodulatory metabolite.
-
Adenosine mediates its immunomodulatory properties in cord blood by inducing MDSCs, and by modulating the inhibitory adenosine A3 receptor on monocytes.
-
Adenosine upregulates expression of IDO in MDSCs and monocytes potentially contributing to their suppressive activity.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Elahi, S. et al. Immunosuppressive CD71+ erythroid cells compromise neonatal host defence against infection. Nature 504, 158–162 (2013).
Levy, O. et al. The adenosine system selectively inhibits TLR-mediated TNF-α production in the human newborn. J. Immunol. 177, 1956–1966 (2006).
Bono, M. R. et al. CD73 and CD39 ectonucleotidases in T cell differentiation: beyond immunosuppression. FEBS Lett. 589, 3454–3460 (2015).
Martin, C. et al. High adenosine plasma concentration as a prognostic index for outcome in patients with septic shock. Crit. Care Med. 28, 3198–3202 (2000).
Sottofattori, E., Anzaldi, M. & Ottonello, L. HPLC determination of adenosine in human synovial fluid. J. Pharm. Biomed. Anal. 24, 1143–1146 (2001).
Chen, Y. et al. ATP release guides neutrophil chemotaxis via P2Y2 and A3 receptors. Science 314, 1792–1795 (2006).
Schenk, U. et al. Purinergic control of T cell activation by ATP released through pannexin-1 hemichannels. Sci. Signal. 1, ra6–ra6 (2008).
Eltzschig, H. K., Weissmüller, T., Mager, A. & Eckle, T. Nucleotide metabolism and cell-cell interactions. Methods Mol Biol. 341, 73–87. https://doi.org/10.1385/1-59745-113-4:73 (2006).
Eltzschig, H. K. et al. Endogenous adenosine produced during hypoxia attenuates neutrophil accumulation: coordination by extracellular nucleotide metabolism. Blood 104, 3986–3992 (2004).
Colgan, S. P. et al. Coordinated adenine nucleotide phosphohydrolysis and nucleoside signaling in posthypoxic endothelium. J. Exp. Med. 198, 783–796 (2003).
Synnestvedt, K. et al. Ecto-5’-nucleotidase (CD73) regulation by hypoxia-inducible factor-1 mediates permeability changes in intestinal epithelia. J. Clin. Investig. 110, 993–1002 (2002).
Thompson, L. F. et al. Crucial role for ecto-5’-nucleotidase (CD73) in vascular leakage during hypoxia. J. Exp. Med. 200, 1395–1405 (2004).
Ehrentraut, H. et al. CD73+ regulatory T cells contribute to adenosine-mediated resolution of acute lung injury. FASEB J. 27, 2207–2219 (2013).
Grenz, A., Homann, D. & Eltzschig, H. K. Extracellular adenosine: a safety signal that dampens hypoxia-induced inflammation during ischemia. Antioxid. Redox Signal. 15, 2221–2234 (2011).
Koeppen, M., Eckle, T. & Eltzschig, H. K. Selective deletion of the A1 adenosine receptor abolishes heart-rate slowing effects of intravascular adenosine in vivo. PLoS ONE 4, e6784 (2009).
Rieber, N. et al. Neutrophilic myeloid-derived suppressor cells in cord blood modulate innate and adaptive immune responses. Clin. Exp. Immunol. 174, 45–52 (2013).
Köstlin, N. et al. Granulocytic myeloid derived suppressor cells expand in human pregnancy and modulate T-cell responses. Eur. J. Immunol. 44, 2582–2591 (2014).
Köstlin, N. et al. Granulocytic myeloid-derived suppressor cells accumulate in human placenta and polarize toward a Th2 phenotype. J. Immunol. 196, 1132–1145 (2016).
Dowling, D. J. & Levy, O. Ontogeny of early life immunity. Trends Immunol. 35, 299–310 (2014).
Pagel, J. et al. Regulatory T cell frequencies are increased in preterm infants with clinical early-onset sepsis. Clin. Exp. Immunol. 185, 219–227 (2016).
Boyum, A. Separation of leukocytes from blood and bone marrow. Introduction. Scand. J. Clin. Lab. Invest. Suppl. 97, 7 (1968).
Boyum, A. Separation of lymphocytes, lymphocyte subgroups and monocytes: a review. Lymphology 10, 71–76 (1977).
Lechner, M. G., Liebertz, D. J. & Epstein, A. L. Characterization of cytokine-induced myeloid-derived suppressor cells from normal human peripheral blood mononuclear cells. J. Immunol. 185, 2273–2284 (2010).
Köstlin, N. et al. HLA-G promotes myeloid-derived suppressor cell accumulation and suppressive activity during human pregnancy through engagement of the receptor ILT4. Eur. J. Immunol. 47, 374–384 (2017).
Degheidy, H. A. et al. Methodological comparison of two anti-ZAP-70 antibodies. Cytom. Part B 80B, 300–308 (2011).
Allard, B. et al. The ectonucleotidases CD39 and CD73: Novel checkpoint inhibitor targets. Immunol. Rev. 276, 121–144 (2017).
Reutershan, J. et al. Adenosine and inflammation: CD39 and CD73 are critical mediators in LPS‐induced PMN trafficking into the lungs. FASEB J. 23, 473–482 (2008).
Laver, J. et al. High levels of granulocyte and granulocyte-macrophage colony-stimulating factors in cord blood of normal full-term neonates. J. Pediatr. 116, 627–632 (1990).
Fiehn, C. et al. Plasma GM-CSF concentrations in rheumatoid arthritis, systemic lupus erythematosus and spondyloarthropathy. Z. Rheumatol. 51, 121–126 (1992).
Omori, F. et al. Levels of human serum granulocyte colony-stimulating factor and granulocyte-macrophage colony-stimulating factor under pathological conditions. Biotherapy 4, 147–153 (1992).
Ryzhov, S. et al. Adenosinergic regulation of the expansion and immunosuppressive activity of CD11b+Gr1+cells. J. Immunol. 187, 6120–6129 (2011).
Nowak, M. et al. The A2aR adenosine receptor controls cytokine production in iNKT cells. Eur. J. Immunol. 40, 682–687 (2010).
Regateiro, F. S. et al. Generation of anti-inflammatory adenosine by leukocytes is regulated by TGF-beta. Eur. J. Immunol. 41, 2955–2965 (2011).
Kropf, P. et al. Arginase activity mediates reversible T cell hyporesponsiveness in human pregnancy. Eur. J. Immunol. 37, 935–945 (2007).
Rivkees, S. A. et al. Influences of adenosine on the fetus and newborn. Mol. Genet. Metab. 74, 160–171 (2001).
Ehrentraut, H. et al. Adora2b adenosine receptor engagement enhances regulatory T cell abundance during endotoxin-induced pulmonary inflammation. PLoS ONE 7, e32416 (2012).
Eltzschig, H. K., Bonney, S. K. & Eckle, T. Attenuating myocardial ischemia by targeting A2B adenosine receptors. Trends Mol. Med. 19, 345–354 (2013).
Leone, R. D. & Emens, L. A. Targeting adenosine for cancer immunotherapy. J. Immunother. Cancer 6, 57 (2018).
Iris, M., Tsou, P.-S. & Sawalha, A. H. Caffeine inhibits STAT1 signaling and downregulates inflammatory pathways involved in autoimmunity. Clin. Immunol. 192, 68–77 (2018).
Speer, E. M. et al. Pentoxifylline, dexamethasone and azithromycin demonstrate distinct age-dependent and synergistic inhibition of TLR- and inflammasome-mediated cytokine production in human newborn and adult blood in vitro. PLoS ONE 13, e0196352 (2018).
Acknowledgements
This project was funded by The Federal Ministry of Education and Research (BMBF) grant no GFGL1165817-01 GL1746F to C.G. and The Ministry of Science, Research and Art Baden-Württemberg and The European Social Fund to N.K.-G.
Author information
Authors and Affiliations
Contributions
F.Ď., N.K.-G. and C.G.: substantial contributions to conception and design; F.Ď.: acquisition of data, or analysis and interpretation of data; F.Ď., C.G.: drafting the article or revising it critically for important intellectual content; C.G., C.F.P.: revising the manuscript and final approval of the version to be published.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Statement of consent
All parents gave written informed consent. The study protocol was approved by ethics committee of the Medical Faculty of Tuebingen University, application number 248/2005A.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ďurčo, F., Köstlin-Gille, N., Poets, C.F. et al. Modulatory activity of adenosine on the immune response in cord and adult blood. Pediatr Res 90, 989–997 (2021). https://doi.org/10.1038/s41390-020-01275-8
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41390-020-01275-8