Abstract
Background
The protective effect of breastfeeding on celiac disease (CD) onset is controversial. We studied a wide range of milk components in milk produced by celiac mothers following long-term gluten-free diet (GFD) in comparison to milk produced by healthy mothers.
Methods
Breast-milk samples from celiac (n = 33) and healthy (n = 41) mothers were obtained during the first year of lactation. A panel of bioactive components was analyzed by enzyme-linked immunosorbent assay in the aqueous fraction. We studied molecules involved in defenses, immunoregulation, and strengthening of the gut–epithelial barrier.
Results
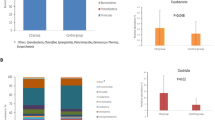
During late lactation (from 6 to 12 months after delivery), the content of total immunoglobulin A (IgA) and IgM was significantly lower in the milk produced by celiac patients. Nevertheless, gliadin (GFD)-specific IgA relative contribution was higher in this group, in contrast to tetanus toxoid-specific antibodies. The balance between pro-inflammatory and anti-inflammatory molecules was different. While interleukin-6, tumor necrosis factor-α, and monocyte chemoattractant protein-1 were most frequently found in samples from celiac mothers, soluble Toll-like receptor-2 prevalence was lower.
Conclusions
We describe differences between the innate and adaptive immune profile of milk produced by celiac and healthy mothers. These results might explain previous controversial reports about breastfeeding and CD protection.
Impact
-
In spite of a long-term adherence to GFD, the milk produced by mothers with CD exhibit a different immune profile, in relation with some immunoregulatory factors and antibody content.
-
This work shows a more comprehensive characterization of milk from celiac mothers, including macronutrients, lysozymes, growth factors, and immunoregulatory components that had not been studied before.
-
The present study widens the available data regarding the characteristics of human milk of celiac mothers following GFD.
-
Further follow-up studies of the health of children who were breastfed by celiac mothers will be necessary in order to also estimate the impact of the present results therein.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Husby, S. et al. European Society Paediatric Gastroenterology, Hepatology and Nutrition Guidelines for Diagnosing Coeliac Disease 2020. J. Pediatr. Gastroenterol. Nutr. 70, 141–156 (2020).
Popp, A. & Mäki, M. Changing pattern of childhood celiac disease epidemiology: contributing factors. Front. Pediatr. 7, 1–16 (2019).
Akobeng, A. K., Ramanan, A. V., Buchan, I. & Heller, R. F. Effect of breast feeding on risk of coeliac disease: a systematic review and meta-analysis of observational studies. Arch. Dis. Child. 91, 39–43 (2006).
Szajewska, H. et al. PREVENTCD Study Group. Systematic review with meta-analysis: early infant feeding and coeliac disease-update 2015. Aliment. Pharm. Ther. 41, 1038–1054 (2015).
Szajewska, H. et al. Systematic review: early infant feeding and the prevention of coeliac disease. Aliment. Pharm. Ther. 36, 607–618 (2012).
Lionetti, E. et al. Introduction of gluten, HLA status, and the risk of celiac disease in children. N. Engl. J. Med. 371, 1295–1303 (2014).
Vriezinga, S. L. et al. Randomized feeding intervention in infants at high risk for celiac disease. N. Engl. J. Med. 371, 1304–1315 (2014).
Aronsson, C. A. et al. Age at gluten introduction and risk of celiac disease. Pediatrics 135, 239–245 (2015).
Olivares, M. et al. Human milk composition differs in healthy mothers and mothers with celiac disease. Eur. J. Nutr. 54, 119–128 (2015).
Roca, M. et al. PREVENT CD Study Group. Anti-gliadin antibodies in breast milk from celiac mothers on a gluten-free diet. Eur. J. Nutr. [Internet] 57, 1947–1955 (2018).
Brazilian Network of Human Milk. Technical Standards and Manuals (2008). http://www.redeblh.fiocruz.br.
Rodríguez-Camejo, C. et al. Impact of Holder pasteurization on immunological properties of human breast milk over the first year of lactation. Pediatr. Res. 87, 32–41 (2020).
Rodríguez-Camejo, C. et al. Antibody profile of colostrum and the effect of processing in human milk banks: Implications in immunoregulatory properties. J. Hum. Lact. 34, 137–147 (2018).
Trend, S. et al. Levels of innate immune factors in preterm and term mothers’ breast milk during the 1st month postpartum. Br. J. Nutr. 115, 1178–1193 (2016).
Team. R. C. A Language and Environment for Statistical Computing (R Foundation for Statistical Computing, Vienna, Austria).
Nommsen, L. A., Lovelady, C. A., Heinig, M. J., Lönnerdal, B. & Dewey, K. G. Determinants of energy, protein, lipid, and lactose concentrations in human milk during the first 12 mo of lactation: the DARLING Study. Am. J. Clin. Nutr. 53, 457–465 (1991).
FieldsD, A. & Demerath, E. W. Human milk composition: nutrients and bioactive factors. Pediatr. Clin. N. Am. 60, 49–74 (2013).
Wierdsma, N. J., van Bokhorst-de van der Schueren, M. A. E., Berkenpas, M., Mulder, C. J. J. & van Bodegraven, A. A. Vitamin and mineral deficiencies are highly prevalent in newly diagnosed celiac disease patients. Nutrients 5, 3975–3992 (2013).
Mesin, L., Sollid, L. M. & Di Niro, R. The intestinal B-cell response in celiac disease. Front. Immunol. 4, 3 (2012).
Syage, J. A. et al. Determination of gluten consumption in celiac disease patients on a gluten-free diet. Am. J. Clin. Nutr. 107, 201–207 (2018).
US Food and Drug Administration. Guidance for Industry; Gluten-Free Labeling of Foods (US Food and Drug Administration, 2014).
Betts, C. B. et al. Mucosal immunity in the female murine mammary gland. J. Immunol. 201, 734–746 (2018).
Bode, L. et al. It’s alive: microbes and cells in human milk and their potential benefits to mother and infant. Adv. Nutr. 5, 571–573 (2014).
Mosconi, E. et al. Breast milk immune complexes are potent inducers of oral tolerance in neonates and prevent asthma development. Mucosal Immunol. 3, 461–474 (2010).
Yamamoto, T., Tsubota, Y., Kodama, T., Kageyama-Yahara, N. & Kadowaki, M. Oral tolerance induced by transfer of food antigens via breast milk of allergic mothers prevents offspring from developing allergic symptoms in a mouse food allergy model. Clin. Dev. Immunol. http://www.ncbi.nlm.nih.gov/pubmed/22505952 (2012).
Verhasselt, V. Neonatal tolerance under breastfeeding influence: the presence of allergen and transforming growth factor-β in breast milk protects the progeny from allergic asthma. J. Pediatr. 156 S16–S20 (2010).
Penttila, I. A. Milk-derived transforming growth factor-β and the infant immune response. J. Pediatr. 156, S21–S25 (2010).
Olivares, M. et al. Human milk composition differs in healthy mothers and mothers with celiac disease. Eur. J. Nutr. 54, 119–128 (2014).
Oddy, W. H. & Rosales, F. A systematic review of the importance of milk TGF-β on immunological outcomes in the infant and young child. Pediatr. Allergy Immunol. 21, 47–59 (2010).
Dowling, D. J. & Levy, O. Ontogeny of early life immunity. Trends Immunol. 35, 299–310 (2014).
Casavale, K. O. et al. NIH workshop on human milk composition: summary and visions. Am. J. Clin. Nutr. 110, 769–779 (2019).
Järvinen, K. M., Martin, H. & Oyoshi, M. K. Immunomodulatory effects of breast milk on food allergy. Ann. Allergy Asthma Immunol. 123, 133–143 (2019).
Acknowledgements
We are deeply grateful to the donors of milk samples and to ACELU for its contribution to the essential communication logistics. We thank L. Carroscia, M.D. and the technical staff of HMB for their invaluable collaboration. We also thank José Fuentes for his assistance with statistical analysis, and A.I. Zambrana, M.Sc. for proofreading this manuscript. This work was supported by the Consejo Sectorial de Investigación Científica – Universidad de la República (CSIC ID – 205/2015 to E.V.), a postgraduate scholarship to E.V. (Agencia Nacional de Innovación e Investigación—ANII), and the Programa de Desarrollo de las Ciencias Básicas (PECECIBA; to A.H., E.V., and C.R.-C.).
Author information
Authors and Affiliations
Contributions
The author’s responsibilities were as follows: E.V. contributed to design, experimental analysis, and revision of the manuscript. A.H. contributed to the conception, design, discussion, drafting, and revision of the manuscript. A.P. and L.F. contributed to the logistics to obtain milk samples and the analyses of macronutrients. V.C. performed logistic regression analyses of data. C.R.-C. contributed with technical assistance in experimental work and discussion.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
Written informed consent was obtained from all volunteers.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Villamil, E., Rodríguez-Camejo, C., Puyol, A. et al. Immune profiling of breast milk from mothers with treated celiac disease. Pediatr Res 89, 488–495 (2021). https://doi.org/10.1038/s41390-020-0901-y
Received:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41390-020-0901-y