Abstract
Background
A body shape index (ABSI) is an emerging anthropometric indicator, challenging two traditional parameters: body mass index (BMI) and waist circumference (WC). We aimed to systematically compare and validate the capability of anthropometric indicators for determining pediatric high blood pressure (HBP).
Methods
A total of 3150 participants aged 7–17 years were enrolled from Suzhou, China. Areas under the receiver operating characteristic curve (AUC) were obtained to evaluate the performance of anthropometric indicators in detecting HBP. DeLong’s test was used to examine whether the AUCs of anthropometric indicators in contrast to BMI or original ABSI were statistically different. Furthermore, a meta-analysis was performed to combine results from this study and five similar articles from databases.
Results
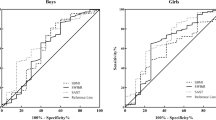
In Suzhou population, BMI exhibited the largest AUC (AUC = 0.705), followed by WC (AUC = 0.669) and original ABSI (AUC = 0.514). Modified ABSI (AUC: 0.537–0.681), although had slightly better performance than original ABSI, was still less valuable than BMI (P < 0.05), either in the total sample or in boys. The meta-analysis with 21108 children and adolescents subsequently confirms the results derived from Suzhou population.
Conclusions
In predicting pediatric HBP, original ABSI and modified ABSI underperform BMI and WC.
Impact
-
The current study is the first to evaluate whether original ABSI or modified ABSI is comparable to BMI and WC for screening HBP in children and adolescents.
-
In predicting pediatric HBP, original ABSI and modified ABSI do not perform as well as traditional anthropometric indicators, such as BMI and WC.
-
BMI remains the optimal indicator in pediatric HBP screening.
-
This study provides a theoretical basis for the early identification of HBP in children and adolescents by adopting effective predictors.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Joseph, P. et al. Reducing the global burden of cardiovascular disease, Part 1: The epidemiology and risk factors. Circ. Res. 121, 677–694 (2017).
Flynn, J. T. et al. Clinical practice guideline for screening and management of high blood pressure in children and adolescents. Pediatrics 140, e20171904 (2017).
Ma, S. J., Yang, L., Zhao, M. & Xi, B. Changing trends in the level of blood pressure and prevalence of hypertension among children and adolescents from 1991 to 2015. Chin. J. Epidemiol. 41, 178–183 (2020) (in Chinese).
Kollias, A., Dafni, M., Poulidakis, E., Ntineri, A. & Stergiou, G. S. Out-of-office blood pressure and target organ damage in children and adolescents: a systematic review and meta-analysis. J. Hypertens. 32, 2315–2331 (2014). Discussion 2331.
Kollias, A. et al. Adiposity, blood pressure, and carotid intima-media thickness in greek adolescents. Obesity (Silver Spring) 21, 1013–1017 (2013).
Brady, T. M., Solomon, B. S., Neu, A. M., Siberry, G. K. & Parekh, R. S. Patient-, provider-, and clinic-level predictors of unrecognized elevated blood pressure in children. Pediatrics 125, e1286–e1293 (2010).
Hansen, M. L., Gunn, P. W. & Kaelber, D. C. Underdiagnosis of hypertension in children and adolescents. JAMA 298, 874–879 (2007).
Okafor, C., Anyaehie, U. & Ofoegbu, E. The magnitude of obesity and its relationship to blood pressure among the residents of enugu metropolis in South East Nigeria. Ann. Med. Health Sci. Res. 4, 624–629 (2014).
Chandra, A. et al. The relationship of body mass and fat distribution with incident hypertension: observations from the Dallas Heart Study. J. Am. Coll. Cardiol. 64, 997–1002 (2014).
Koebnick, C. et al. High blood pressure in overweight and obese youth: implications for screening. J. Clin. Hypertens. (Greenwich) 15, 793–805 (2013).
Xu, Y., Yan, W. & Cheung, Y. B. Body shape indices and cardiometabolic risk in adolescents. Ann. Hum. Biol. 42, 70–75 (2015).
Wang, M. et al. Body mass index percentiles and elevated blood pressure among children and adolescents. J. Hum. Hypertens. 34, 319–325 (2020).
Ononamadu, C. J. et al. Comparative analysis of anthropometric indices of obesity as correlates and potential predictors of risk for hypertension and prehypertension in a population in Nigeria. Cardiovasc. J. Afr. 28, 92–99 (2017).
Wang, S. et al. A novel quantitative body shape score for detecting association between obesity and hypertension in China. BMC Public Health 15, 7 (2015).
Jung, C., Fischer, N., Fritzenwanger, M. & Figulla, H. R. Anthropometric indices as predictors of the metabolic syndrome and its components in adolescents. Pediatr. Int. 52, 402–409 (2010).
Song, L. et al. Height and prevalence of hypertension in a middle-aged and older Chinese population. Sci. Rep. 6, 39480 (2016).
Krakauer, N. Y. & Krakauer, J. C. A new body shape index predicts mortality hazard independently of body mass index. PLoS ONE 7, e39504 (2012).
Chung, W., Park, C. G. & Ryu, O. H. Association of a new measure of obesity with hypertension and health-related quality of life. PLoS ONE 11, e0155399 (2016).
Cheung, Y. B. “A body shape index” in middle-age and older Indonesian population: scaling exponents and association with incident hypertension. PLoS ONE 9, e85421 (2014).
He, S. & Chen, X. Could the new body shape index predict the new onset of diabetes mellitus in the Chinese population? PLoS ONE 8, e50573 (2013).
Mameli, C. et al. The association between a body shape index and cardiovascular risk in overweight and obese children and adolescents. PLoS ONE 13, e0190426 (2018).
Ji, M., Zhang, S. & An, R. Effectiveness of a body shape index (ABSI) in predicting chronic diseases and mortality: a systematic review and meta-analysis. Obes. Rev. 19, 737–759 (2018).
Tong, Y. & Han, E. Associations between body shape, body adiposity and other indices: a case study of hypertension in Chinese children and adolescents. Ann. Hum. Biol. 46, 460–466 (2019).
Perona, J. S. et al. Waist circumference and abdominal volume index are the strongest anthropometric discriminators of metabolic syndrome in spanish adolescents. Eur. J. Clin. Invest. 49, e13060 (2019).
Tee, J. Y. H., Gan, W. Y. & Lim, P. Y. Comparisons of body mass index, waist circumference, waist-to-height ratio and a body shape index (ABSI) in predicting high blood pressure among Malaysian adolescents: a cross-sectional study. BMJ Open 10, e032874 (2020).
Yazdi, M. et al. Validity of anthropometric indices in predicting high blood pressure risk factors in Iranian children and adolescents: Caspian-V Study. J. Clin. Hypertens. (Greenwich) 22, 1009–1017 (2020).
Cristine Silva, K., Santana Paiva, N., Rocha de Faria, F., Franceschini, S. & Eloiza Piore, S. Predictive ability of seven anthropometric indices for cardiovascular risk markers and metabolic syndrome in adolescents. J. Adolesc. Health 66, 491–498 (2020).
Duncan, M. J., Mota, J., Vale, S., Santos, M. P. & Ribeiro, J. C. Associations between body mass index, waist circumference and body shape index with resting blood pressure in Portuguese adolescents. Ann. Hum. Biol. 40, 163–167 (2013).
National Health Commission of the People’s Republic of China. WS/T 610-2018 Reference of Screening for Elevated Blood Pressure among children and adolescents aged 7~18 years (Standards Press of China, 2018).
Metz, C. E. Some practical issues of experimental design and data analysis in radiological ROC studies. Invest. Radiol. 24, 234–245 (1989).
DeLong E. R., D D., Clarke-Pearson D. L. Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics 44, 837–845 (1988).
Whiting, P. F., R, A., Westwood, M. E. & Mallett, S. Quadas-2: a revised tool for the quality assessment of diagnostic accuracy studies. Ann. Intern. Med. 155, 529–536 (2011).
Baker, W. L. et al. Understanding heterogeneity in meta-analysis: the role of meta-regression. Int J. Clin. Pract. 63, 1426–1434 (2009).
Ashwell, M., Gunn, P. & Gibson, S. Waist-to-height ratio is a better screening tool than waist circumference and BMI for adult cardiometabolic risk factors: systematic review and meta-analysis. Obes. Rev. 13, 275–286 (2012).
Lek, N., Yan, W., Zhang, Y., Wang, Q. & Cheung, Y. B. Indices of central and general obesity and cardiometabolic risk among adolescents in three ethnic groups in North-West China. Ann. Hum. Biol. 43, 18–24 (2016).
Lo, K., Wong, M., Khalechelvam, P. & Tam, W. Waist-to-height ratio, body mass index and waist circumference for screening paediatric cardio-metabolic risk factors: a meta-analysis. Obes. Rev. 17, 1258–1275 (2016).
Koren, D. et al. Anthropometric predictors of visceral adiposity in normal-weight and obese adolescents. Pediatr. Diabetes 14, 575–584 (2013).
Brambilla, P. et al. Crossvalidation of anthropometry against magnetic resonance imaging for the assessment of visceral and subcutaneous adipose tissue in children. Int J. Obes. (Lond.) 30, 23–30 (2006).
Benfield, L. L. et al. Magnetic resonance imaging of abdominal adiposity in a large cohort of british children. Int. J. Obes. (Lond.) 32, 91–99 (2008).
Acknowledgements
This study was supported by the National Natural Science Foundation of China (grant: 81602911), Natural Science Foundation of Jiangsu Province-Youth Project (BK20160337), Priority Academic Program Development of Jiangsu Higher Education Institutions (PAPD), Gusu Health Talents Program Training Project in Suzhou, China (GSWS2020100).
Author information
Authors and Affiliations
Contributions
J.Y.Y. and J.H. contributed to the design and concept of the manuscript. W.X.G., C.Q.X., and L.P.Y. were responsible for the analysis, interpretation of data, and manuscript drafting. Y.X., J.Y.L., and F.L. were responsible for the critical revision of the manuscript for intellectual content. All authors were involved in writing the paper and had final approval of the submitted and published versions.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Consent statement
For the recruited participants, informed consent forms in writing duly signed by their guardians were collected before their examination. The project was reviewed by the ethics committees of the Suzhou Center for Disease Prevention and Control.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Ge, W., Yi, L., Xiao, C. et al. Effectiveness of a body shape index in predicting pediatric high blood pressure. Pediatr Res 92, 871–879 (2022). https://doi.org/10.1038/s41390-021-01844-5
Received:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41390-021-01844-5
This article is cited by
-
Comparative analysis of adiposity indices for predicting 2-year hypertension incidence in children and adolescents: a retrospective study
Pediatric Research (2025)
-
Tri-ponderal mass index and left ventricular hypertrophy in a cohort of caucasian children and adolescents with obesity
Italian Journal of Pediatrics (2024)