Abstract
Background
Preterm children are at higher risk of developing mental health problems than full-term children. Deterioration of children’s mental health was observed during COVID-19 pandemic restrictive measures. Our study compared emotional and attention-deficit/hyperactivity disorder (ADHD) symptoms during school closure between preterm and full-term children.
Methods
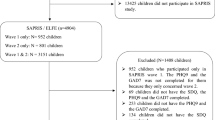
Data from two French birth cohorts—ELFE and EPIPAGE-2—were used. In 2011, infants born ≥22 weeks’ gestation were recruited. Parents completed the Strengths and Difficulties Questionnaire when the children were 9 years old and experiencing school closure. Multivariate multinomial logistic regression models were used.
Results
Subjects included 4164 full-term and 1119 preterm children. In univariate analyses, compared to full-term children: extremely and very preterm children more frequently had abnormal and borderline ADHD scores (odds ratio [OR] 1.86, 95% confidence interval [CI] 1.50–2.30, OR 1.42, 95% CI 1.08–1.85, respectively) and abnormal emotional scores (OR 1.86, 95% CI 1.43–2.40); moderate to late preterm children more often had abnormal ADHD scores (OR 1.33, 95% CI 1.01–1.78). The associations did not remain when previous symptoms at 5 years old were considered.
Conclusions
School closure during lockdown did not appear to increase the risk of mental health problems in preterm compared to full-term children.
Impact statement
-
Preterm children are at higher risk of developing mental health problems than full-term children. Deterioration in children’s mental health was observed during COVID-19 pandemic restrictions. However, whether preterm children were a particularly vulnerable subgroup during school closure is unclear.
-
In univariate analyses, extremely and very preterm children more often had abnormal and borderline ADHD symptoms and abnormal emotional symptom scores than full-term children. The associations did not remain significantly associated when previous symptoms were considered.
-
Preterm compared to full-term children more often suffer from ADHD and emotional symptoms, but school closure during lockdown did not appear to increase this risk.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
Data availability
In regards to data availability, data of the study are protected under the protection of health data regulation set by the French National Commission on Informatics and Liberty (Commission Nationale de l’Informatique et des Libertés, CNIL). The data can be available upon reasonable request after a consultation with the steering com- mittee of the Sapris study. The French law forbids us to provide free access to Sapris data; access could however be given by the steering committee after legal verification of the use of the data.
References
Hee Chung, E., Chou, J. & Brown, K. A. Neurodevelopmental outcomes of preterm infants: a recent literature review. Transl. Pediatr. 9, S3–S8 (2020).
Bogičević, L. et al. Individual attention patterns in children born very preterm and full term at 7 and 13 years of age. J. Int. Neuropsychol. Soc. 1–11 https://doi.org/10.1017/S1355617720001411 (2021).
Cronin, F. M., Segurado, R., McAuliffe, F. M., Kelleher, C. C. & Tremblay, R. E. Gestational age at birth and “body-mind” health at 5 years of age: a Population Based Cohort Study. PLoS ONE 11, e0151222 (2016).
Cooper, K. et al. Loneliness, social relationships, and mental health in adolescents during the COVID-19 pandemic. J. Affect. Disord. 289, 98–104 (2021).
Liu, J. J., Bao, Y., Huang, X., Shi, J. & Lu, L. Mental health considerations for children quarantined because of COVID-19. Lancet Child Adolesc. Health 4, 347–349 (2020).
Schmidt, S. J., Barblan, L. P., Lory, I. & Landolt, M. A. Age-related effects of the COVID-19 pandemic on mental health of children and adolescents. Eur. J. Psychotraumatol. 12, 1901407 (2021).
Ma, L. et al. Prevalence of mental health problems among children and adolescents during the COVID-19 pandemic: a systematic review and meta-analysis. J. Affect. Disord. 293, 78–89 (2021).
Moulin, F. et al. Risk and protective factors related to children’s symptoms of emotional difficulties and hyperactivity/inattention during the COVID-19-related lockdown in France: results from a community sample. Eur. Child Adolesc. Psychiatry https://doi.org/10.1007/s00787-021-01752-3 (2021).
Ehrler, M. et al. Impact of the COVID-19 pandemic on children with and without risk for neurodevelopmental impairments. Acta Paediatr. 110, 1281–1288 (2021).
Carrat, F. et al. Incidence and risk factors of COVID-19-like symptoms in the French general population during the lockdown period: a multi-cohort study. BMC Infect. Dis. 21, 169 (2021).
Charles, M. A. et al. Cohort Profile: The French national cohort of children (ELFE): birth to 5 years. Int. J. Epidemiol. 49, 368–369j (2020).
Goodman, R. Psychometric properties of the strengths and difficulties questionnaire. J. Am. Acad. Child Adolesc. Psychiatry 40, 1337–1345 (2021).
d’Acremont, M. & Linden, M. Vder Confirmatory factor analysis of the Strengths and Difficulties Questionnaire in a community sample of French-speaking adolescents. Eur. J. Psychol. Assess. 24, 1–8 (2008).
Ramirez, S. et al. Brief Research Report: the association between educational experiences and Covid-19 pandemic-related variables, and mental health among children and adolescents. Front. Psychiatry 12, 647456 (2021).
Navarro, M. C. et al. Machine learning assessment of early life factors predicting suicide attempt in adolescence or young adulthood. JAMA Netw. Open 4, e211450 (2021).
Fancourt, D., Steptoe, A. & Bu, F. Trajectories of anxiety and depressive symptoms during enforced isolation due to COVID-19 in England: a longitudinal observational study. Lancet Psychiatry 8, 141–149 (2021).
Perapoch, J. et al. Prematurity and ADHD in childhood: an observational register-based study in Catalonia. J. Atten. Disord. 25, 933–941 (2021).
Panchal, U. et al. The impact of COVID-19 lockdown on child and adolescent mental health: systematic review. Eur. Child Adolesc. Psychiatry https://doi.org/10.1007/s00787-021-01856-w (2021).
Ego, A. et al. Customized and non-customized French intrauterine growth curves. I-Methodology. J. Gynecol. Obstet. Biol. Reprod. 45, 155–164 (2016).
Burgette, L. F. & Reiter, J. P. Multiple imputation for missing data via sequential regression trees. Am. J. Epidemiol. 72, 1070–1076 (2010).
Buuren, S. V. Flexible Imputation of Missing Data 2nd edn. 444 (CRC Press, Boca Raton, FL, 2018).
Breeman, L. D., Jaekel, J., Baumann, N., Bartmann, P. & Wolke, D. Attention problems in very preterm children from childhood to adulthood: the Bavarian Longitudinal Study. J. Child Psychol. Psychiatry 57, 132–140 (2016).
Linsell, L. et al. Trajectories of behavior, attention, social and emotional problems from childhood to early adulthood following extremely preterm birth: a prospective cohort study. Eur. Child Adolesc. Psychiatry 28, 531–542 (2019).
Yates, R. et al. Rates and stability of mental health disorders in children born very preterm at 7 and 13 years. Pediatrics 145, e20192699 (2020).
Hall, J. & Wolke, D. A comparison of prematurity and small for gestational age as risk factors for age 6–13 year emotional problems. Early Hum. Dev. 88, 797–804 (2012).
Shah, R., Raju, V. V., Sharma, A. & Grover, S. Impact of COVID-19 and lockdown on children with ADHD and their families—an online survey and a continuity care model. J. Neurosci. Rural Pract. 12, 71–79 (2021).
Chronis-Tuscano, A. et al. Very early predictors of adolescent depression and suicide attempts in children with attention-deficit/hyperactivity disorder. Arch. Gen. Psychiatry 67, 1044–1051 (2010).
Geoffroy, M. C., Orri, M., Girard, A., Perret, L. C., Turecki, G. Trajectories of suicide attempts from early adolescence to emerging adulthood: prospective 11-year follow-up of a Canadian cohort. Psychol. Med. 1–11. https://doi.org/10.1017/S0033291720000732 (2020).
Hvolgaard Mikkelsen, S., Olsen, J., Bech, B. H. & Obel, C. Parental age and attention-deficit/hyperactivity disorder (ADHD). Int. J. Epidemiol. 46, 409–420 (2017).
Filatova, S., Upadhyaya, S., Luntamo, T., Sourander, A. & Chudal, R. Parental age and risk of depression: a nationwide, population-based case-control study. J. Affect. Disord. 282, 322–328 (2021).
Acknowledgements
Agence Nationale de la Recherche (ANR, 0009/SAPRIS/997/NB), Fondation pour la Recherche Médicale, Direction Générale de la Recherche et de l’Innovation, Institut Gustave Roussy, the New-Aquitaine region.
Author information
Authors and Affiliations
Consortia
Contributions
M.B. concept and design the study, interpreted the data and wrote the manuscript. M.M. did the statistical analysis, interpreted the data and revised the manuscript. F.M., X.T., S.V., S.M.C., B.F., T.S., B.G., L.M., M.N.D., M.A.C., P.Y.A., M.M., A.R., interpreted the data, critiqued the manuscript of important intellectual content and approved the final version of manuscript. C.G. concept and design the study, interpreted the data, and revised the manuscript. The SAPRIS group enrolled participants, collected the data, and revised the manuscript. Authors had access to all the data in the study and participated in the decision to submit.
Corresponding author
Ethics declarations
Competing interests
M.M. has been funded by the New-Aquitaine region (AMI Flash Recherche et Innovations COVID). The other authors have no competing interests to declare.
Consent statement
A consent form was signed by parents for inclusion.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bailhache, M., Monnier, M., Moulin, F. et al. Emotional and attention-deficit/hyperactivity disorder symptoms of preterm vs. full-term children during COVID-19 pandemic restrictions. Pediatr Res 92, 1749–1756 (2022). https://doi.org/10.1038/s41390-022-02037-4
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41390-022-02037-4
This article is cited by
-
The impact of COVID-19 lockdowns on mental health patient populations in the United States
Scientific Reports (2024)