Abstract
Background
COVID-19 pandemic introduced significant challenges that may have exacerbated healthcare worker (HCW) burnout. To date, assessments of burnout during COVID-19 pandemic have been cross-sectional, limiting our understanding of changes in burnout. This longitudinal study assessed change across time in pediatric HCW burnout during the COVID-19 pandemic and whether demographic and psychological factors were associated with changes in burnout.
Methods
This longitudinal study included 162 physicians, physician assistants, nurses, and medical technicians within the emergency department (ED), intensive care, perioperative, and inter-hospital transport services in a children’s hospital. HCW demographics, anxiety and personality traits were reported via validated measures. HCWs completed the Maslach Burnout Inventory in April 2020 and March 2021. Data were analyzed using generalized estimating equations.
Results
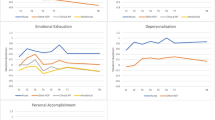
The percentage of HCWs reporting high emotional exhaustion and/or depersonalization burnout increased significantly across time (18.5% to 28.4%, P = 0.010). Factors associated with increased emotional exhaustion included working in the ED (P = 0.011) or perioperative department (P < 0.001), being a nurse or medical technician (P’s < 0.001), not having children (P < 0.001), and low conscientiousness (P < 0.001).
Conclusions
Pediatric HCW burnout significantly increased over 11-months of the COVID-19 pandemic. Results suggest that certain demographic and psychological factors may represent potential area to target for intervention for future pandemics.
Impact
-
This longitudinal study revealed that the COVID-19 pandemic has had a significant impact on pediatric healthcare worker burnout.
-
The percentage of healthcare workers reporting high levels of emotional exhaustion and depersonalization burnout increased significantly over 11-months of the COVID-19 pandemic.
-
Results suggest that certain demographic and psychological factors may represent potential targets for future interventions.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
Data availability
The de-identified datasets analyzed during the current study are available from the corresponding author upon reasonable request.
References
Bodenheimer, T. & Sinsky, C. From triple to quadruple aim: care of the patient requires care of the provider. Ann. Fam. Med. 12, 573–576 (2014).
Jun, J., Ojemeni, M. M., Kalamani, R., Tong, J. & Crecelius, M. L. Relationship between nurse burnout, patient and organizational outcomes: Systematic review. Int. J. Nurs. Stud. 119, 103933 (2021).
Kemper, K. J. et al. Burnout in pediatric residents: three years of national survey data. Pediatrics 145, e20191030 (2020).
Shanafelt, T. D. et al. Burnout and satisfaction with work-life balance among US physicians relative to the general US population. Arch. Intern. Med. 172, 1377–1385 (2012).
Buckley, L., Berta, W., Cleverley, K., Medeiros, C. & Widger, K. What is known about paediatric nurse burnout: a scoping review. Hum. Resour. Health 18, 9 (2020).
Gribben, J. L., MacLean, S. A., Pour, T., Waldman, E. D. & Weintraub, A. S. A cross-sectional analysis of compassion fatigue, burnout, and compassion satisfaction in pediatric emergency medicine physicians in the United States. Acad. Emerg. Med. 26, 732–743 (2019).
Patterson, J. & Gardner, A. Burnout rates in pediatric emergency medicine physicians. Pediatr. Emerg. Care 36, 192–195 (2020).
Starmer, A. J., Frintner, M. P. & Freed, G. L. Work-life balance, burnout, and satisfaction of early career pediatricians. Pediatrics 137, e20153183 (2016).
Maslach, C. A multidimensional theory of burnout. in Theories of organizational stress (ed. Cooper, C.) vol. 68 68–85 (Oxford University Press, 1998).
Dyrbye, L. N. et al. A cross-sectional study exploring the relationship between burnout, absenteeism, and job performance among American nurses. BMC Nurs. 18, 1–8 (2019).
Maslach, C., Jackson, S. E. & Leiter, M. P. Maslach Burnout Inventory Manual 191–205 (Consulting Psychologists Press Inc, 1996).
Montgomery, A. P., Patrician, P. A. & Azuero, A. Nurse Burnout Syndrome and Work Environment Impact Patient Safety Grade. J. Nurs. Care Qual. 37, 87–93 (2022).
Shanafelt, T. D., Dyrbye, L. N. & West, C. P. Addressing physician burnout: the way forward. JAMA 317, 901–902 (2017).
Wallace, J. E., Lemaire, J. B. & Ghali, W. A. Physician wellness: a missing quality indicator. Lancet 374, 1714–1721 (2009).
West, C. P., Dyrbye, L. N. & Shanafelt, T. D. Physician burnout: contributors, consequences and solutions. J. Intern. Med. 283, 516–529 (2018).
Schooley, B., Hikmet, N., Tarcan, M. & Yorgancioglu, G. Comparing burnout across emergency physicians, nurses, technicians, and health information technicians working for the same organization. Med. (Baltim.) 95, e2856 (2016).
Chirico, F. et al. Prevalence, risk factors and prevention of burnout syndrome among healthcare workers: an umbrella review of systematic reviews and meta-analyses. J. Health Soc. Sci. 6, 465–491 (2021).
CHIRICO, F. et al. Workplace violence against healthcare workers during the COVID-19 pandemic: A systematic review. J. Health Soc. Sci. 7, 14–35 (2022).
Fiest, K. M. et al. Experiences and management of physician psychological symptoms during infectious disease outbreaks: a rapid review. BMC Psychiatry 21, 91 (2021).
Morgantini, L. A. et al. Factors contributing to healthcare professional burnout during the COVID-19 pandemic: A rapid turnaround global survey. PloS One 15, e0238217 (2020).
Amanullah, S. & Ramesh Shankar, R. The Impact of COVID-19 on Physician Burnout Globally: A Review. in vol. 8 421 (Multidisciplinary Digital Publishing Institute, 2020).
Rodriguez, R. M. et al. Academic Emergency Medicine Physicians’ Anxiety Levels, Stressors, and Potential Stress Mitigation Measures During the Acceleration Phase of the COVID-19 Pandemic. Acad. Emerg. Med. 27, 700–707 (2020).
Kelker, H. et al. Prospective study of emergency medicine provider wellness across ten academic and community hospitals during the initial surge of the COVID-19 pandemic. BMC Emerg. Med. 21, 1–12 (2021).
Nguyen, J. et al. Impacts and challenges of the COVID-19 pandemic on emergency medicine physicians in the United States. Am. J. Emerg. Med. 48, 38–47 (2021).
Firew, T. et al. Protecting the front line: a cross-sectional survey analysis of the occupational factors contributing to healthcare workers’ infection and psychological distress during the COVID-19 pandemic in the USA. BMJ Open 10, e042752 (2020).
Maunder, R. G. et al. Psychological impact of the COVID-19 pandemic on hospital workers over time: Relationship to occupational role, living with children and elders, and modifiable factors. Gen. Hosp. Psychiatry 71, 88–94 (2021).
Brown, P. A., Slater, M. & Lofters, A. Personality and burnout among primary care physicians: an international study. Psychol. Res. Behav. Manag. 12, 169–177 (2019).
Kroencke, L., Geukes, K., Utesch, T., Kuper, N. & Back, M. Neuroticism and emotional risk during the Covid-19 Pandemic. (2020).
Heyming, T. W. et al. Predictors for COVID-19-related new-onset maladaptive behaviours in children presenting to a paediatric emergency department. J. Paediatr. Child Health https://doi.org/10.1111/jpc.15579 (2021).
Heyming, T. W. et al. Rapid antibody testing for SARS-CoV-2 vaccine response in pediatric healthcare workers. Int. J. Infect. Dis. 113, 1–6 (2021).
John, O. P., Naumann, L. P. & Soto, C. J. Paradigm shift to the integrative Big Five trait taxonomy: History, measurement, and conceptual issues. in Handbook of personality: Theory and research (eds. John, O. P., Robins, R. W. & Pervine, L. A.) 114–158 (Guilford Press, 2008).
Soto, C. J. & John, O. P. Short and extra-short forms of the Big Five Inventory–2: The BFI-2-S and BFI-2-XS. J. Res. Personal. 68, 69–81 (2017).
Schmitt, D. P., Allik, J., McCrae, R. R. & Benet-Martínez, V. The geographic distribution of Big Five personality traits: Patterns and profiles of human self-description across 56 nations. J. Cross-Cult. Psychol. 38, 173–212 (2007).
Spielberger, C. D. State-trait anxiety inventory for adults. (1983).
Kendall, P. C., Finch, A. J. Jr, Auerbach, S. M., Hooke, J. F. & Mikulka, P. J. The State-Trait Anxiety Inventory: a systematic evaluation. J. Consult. Clin. Psychol. 44, 406 (1976).
LeBlanc, V. R. & Bandiera, G. W. The effects of examination stress on the performance of emergency medicine residents. Med. Educ. 41, 556–564 (2007).
Wong, M. L., Anderson, J., Knorr, T., Joseph, J. W. & Sanchez, L. D. Grit, anxiety, and stress in emergency physicians. Am. J. Emerg. Med. 36, 1036–1039 (2018).
González-Cabrera, J., Fernández-Prada, M., Iribar-Ibabe, C. & Peinado, J. M. Acute and chronic stress increase salivary cortisol: a study in the real-life setting of a national examination undertaken by medical graduates. Stress 17, 149–156 (2014).
Spielberger, C. D., Gorsuch, P. L. & Lushene, R. E. Manual for the State-Trait Anxiety Inventory. (Consulting Psychologist Press, 1970).
Maslach, C., Jackson, S. E., Leiter, M. P., Schaufeli, W., & Schwab, R. Maslach Burnout Inventory Manual. 13–29 (Mind Garden, 2016).
Poghosyan, L., Aiken, L. H. & Sloane, D. M. Factor structure of the Maslach burnout inventory: an analysis of data from large scale cross-sectional surveys of nurses from eight countries. Int. J. Nurs. Stud. 46, 894–902 (2009).
Hwang, C.-E., Scherer, R. F. & Ainina, M. F. Utilizing the Maslach Burnout Inventory in cross-cultural research. Int. J. Manag. 20, 3 (2003).
Greenglass, E. R., Burke, R. J. & Fiksenbaum, L. Workload and burnout in nurses. J. Community Appl. Soc. Psychol. 11, 211–215 (2001).
Maslach, C., Leiter, M. P. & Schaufeli, W. Measuring Burnout. in The Oxford Handbook of Organizational Well-being (eds. Cartwright, S. & Cooper, C. L.) (Oxford University Press, 2009).
Chirico, F., Nucera, G. & Leiter, M. Measuring burnout syndrome requires reliable and standardized measures. Hong. Kong J. Emerg. Med 29, 325–326 (2022).
Pantaleoni, J. L., Augustine, E. M., Sourkes, B. M. & Bachrach, L. K. Burnout in pediatric residents over a 2-year period: a longitudinal study. Acad. Pediatr. 14, 167–172 (2014).
Campbell, J., Prochazka, A. V., Yamashita, T. & Gopal, R. Predictors of Persistent Burnout in Internal Medicine Residents: A Prospective Cohort Study. Acad. Med. 85, 1630–1634 (2010).
Geuens, N., Van Bogaert, P. & Franck, E. Vulnerability to burnout within the nursing workforce-The role of personality and interpersonal behaviour. J. Clin. Nurs. 26, 4622–4633 (2017).
Giusti, E. M. et al. The psychological impact of the COVID-19 outbreak on health professionals: a cross-sectional study. Front. Psychol. 11, 1684 (2020).
Staples, B. B. et al. Burnout and Association With Resident Performance as Assessed by Pediatric Milestones: An Exploratory Study. Acad. Pediatr. 21, 358–365 (2021).
West, C. P., Dyrbye, L. N., Erwin, P. J. & Shanafelt, T. D. Interventions to prevent and reduce physician burnout: a systematic review and meta-analysis. Lancet 388, 2272–2281 (2016).
Chirico, F. & Leiter, M. Tackling stress, burnout, suicide and preventing the “great resignation” phenomenon among healthcare workers (during and after the COVID-19 pandemic) for maintaining the sustainability of healthcare systems and reaching the 2030 sustainable development goals. J. Health Soc. Sci. 9–13 (2022).
Specht, J., Egloff, B. & Schmukle, S. C. Stability and change of personality across the life course: the impact of age and major life events on mean-level and rank-order stability of the big five. J. Pers. Soc. Psychol. 101, 862–882 (2011).
Borges, N. J. & Savickas, M. L. Personality and medical specialty choice: a literature review and integration. J of Career Assess.10, 362–380 (2002).
Spinhoven, P., Huijbers, M. J., Ormel, J. & Speckens, A. E. Improvement of mindfulness skills during mindfulness-based cognitive therapy predicts long-term reductions of neuroticism in persons with recurrent depression in remission. J. Affect. Disord. 213, 112–117 (2017).
Funding
S.R.M. is supported by the National Institutes of Health National Institute for Child Health and Human Development (K23HD105042, PI: Martin).
Author information
Authors and Affiliations
Contributions
Each author has met the Pediatric Research authorship requirements. The authors that met each criterion are listed below. - Substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data: S.R.M., Z.N.K., T.H., M.A.F., L.S., T.S., and T.M.. -Drafting the article or revising it critically for important intellectual content: S.R.M., Z.N.K., T.H., M.A.F., L.S., T.S., and T.M. -Final approval of the version to be published: S.R.M., T.H., M.A.F., L.S., T.S., Z.N.K., and T.M.
Corresponding author
Ethics declarations
Competing interests
Z.N.K. serves as a consultant for Edwards Lifesciences and Pacira and is the President of the American College of Perioperative Medicine. All other authors have no conflicts of interest to report.
Consent statement
Healthcare worker participants completed informed consent prior to completing study procedures.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Martin, S.R., Heyming, T., Morphew, T. et al. Impact of COVID-19 pandemic on pediatric healthcare burnout in acute care: a longitudinal study. Pediatr Res 94, 1771–1778 (2023). https://doi.org/10.1038/s41390-023-02674-3
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41390-023-02674-3
This article is cited by
-
A 2-year longitudinal study of anxiety caused by COVID-19 and job burnout among Iranian healthcare workers
Scientific Reports (2024)
-
“The forest and the trees”: a narrative medicine curriculum by residents for residents
Pediatric Research (2024)