Abstract
Background
We aimed to evaluate the trajectory of skin barrier properties in full-term newborns during the first four days after birth.
Methods
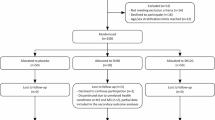
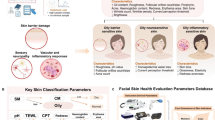
Based on the MKNFOAD cohort (NCT02889081), transepidermal water loss (TEWL), stratum corneum hydration (SCH), skin pH, and sebum content at five anatomical sites (cheek, forehead, volar forearm, abdomen, and dorsal lower leg) were examined once within 96 h after birth in 384 full-term infants. Multivariable linear regression analysis was performed to assess variations in these skin barrier parameters with age adjusted for gestational age, neonate’s sex, parents’ allergy history, delivery mode, amniotic fluid characteristics, and birth weight. The regression coefficient (ß) and 95% confidence interval were reported.
Results
We analyzed a total of 384 neonates including 198 (51.6%) boys. TEWL values remained stable and showed no significant association with age (days). pH values exhibited a declining trend with age (p for trend <0.001). Both SCH values and sebum content grew with age (p for trend <0.001).
Conclusion
During the first four days after birth, the skin TEWL remained stable, pH decreased, and the SCH and sebum content increased over time. These findings provide insights into the neonatal skin physiological development at the beginning of life.
Impact
-
From birth to 96 h, TEWL was stable, pH showed a steep decline, SCH and sebum content increased.
-
This study provides the first evidence of skin adaptation in the newborn due to changes in utero to after birth in the first 4 days of life in an Asian population.
-
These findings will provide a new theoretical basis for neonatal skin physiology and clinical strategies for guiding newborn skin care.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
Data availability
The data that support the findings of this study are available from the corresponding author on reasonable request.
References
Madison, K. C. Barrier function of the skin: “la raison d'être” of the epidermis. J. Invest. Dermatol. 121, 231–241 (2003).
Proksch, E., Brandner, J. M. & Jensen, J. M. The skin: an indispensable barrier. Exp. Dermatol 17, 1063–1072 (2008).
Stamatas, G. N., Nikolovski, J., Mack, M. C. & Kollias, N. Infant skin physiology and development during the first years of life: a review of recent findings based on in vivo studies. Int J. Cosmet. Sci. 33, 17–24 (2011).
Giusti, F., Martella, A., Bertoni, L. & Seidenari, S. Skin barrier, hydration, and pH of the skin of infants under 2 years of age. Pediatr. Dermatol. 18, 93–96 (2001).
Williams, M. L., Hanley, K., Elias, P. M. & Feingold, K. R. Ontogeny of the epidermal permeability barrier. J. Investig. Dermatol. Symp. Proc. 3, 75–79 (1998).
McAleer, M. A. et al. Early-life regional and temporal variation in filaggrin-derived natural moisturizing factor, filaggrin-processing enzyme activity, corneocyte phenotypes and plasmin activity: implications for atopic dermatitis. Br. J. Dermatol. 179, 431–441 (2018).
Darmstadt, G. L. et al. Effect of topical treatment with skin barrier-enhancing emollients on nosocomial infections in preterm infants in Bangladesh: a randomised controlled trial. Lancet 365, 1039–1045 (2005).
Nako, Y. et al. Effects of bathing immediately after birth on early neonatal adaptation and morbidity: a prospective randomized comparative study. Pediatr. Int. 42, 517–522 (2000).
Ye, Y. et al. Dynamic trends in skin barrier function from birth to age 6 months and infantile atopic dermatitis: A Chinese prospective cohort study. Clin. Transl. Allergy 11, e12043 (2021).
Ye, Y. et al. Maternal periconceptional folate status and infant atopic dermatitis: A prospective cohort study. Pediatr. Allergy Immunol. 32, 137–145 (2021).
Walters, R. M., Khanna, P., Chu, M. & Mack, M. C. Developmental Changes in Skin Barrier and Structure during the First 5 Years of Life. Ski. Pharm. Physiol. 29, 111–118 (2016).
Rutter, N. & Hull, D. Water loss from the skin of term and preterm babies. Arch. Dis. Child 54, 858–868 (1979).
Kikuchi, K., Kobayashi, H., O’goshi, K. I. & Tagami, H. Impairment of skin barrier function is not inherent in atopic dermatitis patients: a prospective study conducted in newborns. Pediatr. Dermatol. 23, 109–113 (2006).
Fluhr, J. W. et al. Infant epidermal skin physiology: adaptation after birth. Br. J. Dermatol. 166, 483–490 (2012).
Ludriksone, L., Bartels, N. G., Kanti, V., Blume-Peytavi, U. & Kottner, J. Skin barrier function in infancy: a systematic review. Arch. Dermatol. Res. 306, 591–599 (2014).
Nishijima, K., Yoneda, M., Hirai, T., Takakuwa, K. & Enomoto, T. Biology of the vernix caseosa: A review. J. Obstet. Gynaecol. Res. 45, 2145–2149 (2019).
Visscher, M. O. et al. Neonatal skin maturation-vernix caseosa and free amino acids. Pediatr. Dermatol. 28, 122–132 (2011).
King, A., Balaji, S. & Keswani, S. G. Biology and function of fetal and pediatric skin. Facial Plast. Surg. Clin. North Am. 21, 1–6 (2013).
Visscher, M. O. et al. Vernix caseosa in neonatal adaptation. J. Perinatol. 25, 440–446 (2005).
Mauro, T. et al. Barrier recovery is impeded at neutral pH, independent of ionic effects: implications for extracellular lipid processing. Arch. Dermatol. Res. 290, 215–222 (1998).
Rippke, F., Schreiner, V. & Schwanitz, H. J. The acidic milieu of the horny layer: new findings on the physiology and pathophysiology of skin pH. Am. J. Clin. Dermatol. 3, 261–272 (2002).
Fluhr, J. W. et al. Stratum corneum acidification in neonatal skin: secretory phospholipase A2 and the sodium/hydrogen antiporter-1 acidify neonatal rat stratum corneum. J. Invest Dermatol. 122, 320–329 (2004).
Hoeger, P. H. & Enzmann, C. C. Skin physiology of the neonate and young infant: a prospective study of functional skin parameters during early infancy. Pediatr. Dermatol. 19, 256–262 (2002).
Fox, C., Nelson, D. & Wareham, J. The timing of skin acidification in very low birth weight infants. J. Perinatol. 18, 272–275 (1998).
Green, M., Carol, B. & Behrendt, H. Physiologic skin pH patterns in infants of low birth weight. The onset of surface acidification. Am. J. Dis. Child 115, 9–16 (1968).
Chiou, Y. B. & Blume-Peytavi, U. Stratum corneum maturation. A review of neonatal skin function. Ski. Pharm. Physiol. 17, 57–66 (2004).
Bartels, N. G. et al. Influence of bathing or washing on skin barrier function in newborns during the first four weeks of life. Ski. Pharm. Physiol. 22, 248–257 (2009).
Thiboutot, D. Regulation of human sebaceous glands. J. Invest. Dermatol. 123, 1–12 (2004).
Zouboulis, C. C. et al. Frontiers in sebaceous gland biology and pathology. Exp. Dermatol. 17, 542–551 (2008).
Zouboulis, C. C. [The sebaceous gland]. Hautarzt 61, 467–468 (2010).
Bautista, M. I., Wickett, R. R., Visscher, M. O., Pickens, W. L. & Hoath, S. B. Characterization of vernix caseosa as a natural biofilm: comparison to standard oil-based ointments. Pediatr. Dermatol. 17, 253–260 (2000).
Hoath, S. B., Pickens, W. L. & Visscher, M. O. The biology of vernix caseosa. Int J. Cosmet. Sci. 28, 319–333 (2006).
Fluhr, J. W. et al. Functional skin adaptation in infancy ‐ almost complete but not fully competent. Exp. Dermatol. 19, 483–492 (2010).
Agache, P., Blanc, D., Barrand, C. & Laurent, R. Sebum levels during the first year of life. Br. J. Dermatol. 103, 643–649 (1980).
Henderson, C. A., Taylor, J. & Cunliffe, W. J. Sebum excretion rates in mothers and neonates. Br. J. Dermatol. 142, 110–111 (2000).
Man, M. Q. et al. Variation of Skin Surface pH, Sebum Content and Stratum Corneum Hydration with Age and Gender in a Large Chinese Population. Ski. Pharm. Physiol. 22, 190–199 (2009).
Giltay, E. J. & Gooren, L. J. Effects of sex steroid deprivation/administration on hair growth and skin sebum production in transsexual males and females. J. Clin. Endocrinol. Metab. 85, 2913–2921 (2000).
Acknowledgements
We thank all mothers and their infants for participation in the MKNFOAD study, and all of the staff involved in the study at the recruiting hospital for their cooperation.
Funding
National Natural Science Foundation of China (82304017); Children’s Atopic Dermatitis Research Program of Beijing Health Alliance Charitable Foundation (KH000678-04) and Canada‐China Clinical Research Program (201607).
Author information
Authors and Affiliations
Contributions
Project management and study design: Weitao Tang, Liuhui Wang and Ying Ye (principal investigator). Data collection: Weitao Tang. Skin barrier examination: Yalan Dou. Data input and statistical analysis: Weitao Tang, Yuanzhou Peng and Yi Zhan. Manuscript drafting: Weitao Tang and YingYe. Ming Li, Liuhui Wang and Xiaohua Zhang conceived the study. Weili Yan supervised the statistical analyses. Ying Ye made the final approval of the manuscript. All authors contributed to data interpretation and reviewing the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
The study population was from the MKNFOAD birth cohort in Shanghai. The MKNFOAD protocol was approved by the institutional ethics review board (approval number: 2016-34) and was registered at www.cliinicaltrials.org (NCT 02889081). Signed informed consent was obtained from the legal guardians of participants before data collection began.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tang, W., Peng, Y., Dou, Y. et al. Changes in skin barrier over the first four days of life: a cross-sectional study. Pediatr Res 97, 1072–1078 (2025). https://doi.org/10.1038/s41390-024-03530-8
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41390-024-03530-8