Abstract
Background
The COVID-19 pandemic intensified psychosocial stressors, potentially contributing to increased rates of child abuse. This study aimed to compare trends in child abuse/traumatic brain injury (TBI) admissions and socioeconomic status before and after the pandemic.
Methods
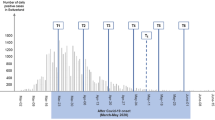
A 7-year retrospective study was conducted at a Level-1 Pediatric Trauma Center. TBI cases were identified using ICD-10 codes based on the modified CDC framework. Neighborhood disadvantage and injury severity were measured using the Social Deprivation Index (SDI) and Injury Severity Score (ISS), respectively, with higher scores indicating greater disadvantage and severity. A Bayesian structural time series (BSTS) model was employed to assess the causal impact of COVID-19 on monthly child abuse/TBI admissions, SDI, and ISS.
Results
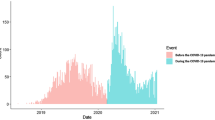
The study included 560 child abuse cases, with 62.3% involving TBI. Before COVID-19, monthly admissions averaged 5.89 for child abuse and 3.70 for child abuse with TBI, with corresponding SDI scores of 60.07 and 57.60. During the COVID era, monthly averages rose to 8.77 and 5.58 (p = 0.001, p < 0.001), and SDI scores increased to 66.32 and 61.60 (p = 0.053, p = 0.370). BSTS analysis inferred a causal impact of COVID-19 on monthly child abuse admissions (p = 0.001), monthly child abuse admissions sustaining TBI (p = 0.001), an upward trend in average monthly SDI scores (p = 0.033), and a decrease in average monthly ISS (p = 0.001).
Conclusions
The study indicates a significant increase in child abuse/TBI admissions and heightened neighborhood disadvantage during the COVID-19 pandemic.
Impact
-
This study uses Bayesian structural time series analysis to assess the COVID-19 pandemic’s causal impact on child abuse and traumatic brain injury (TBI) admissions.
-
The pandemic is linked to increased child abuse admissions and TBI cases, correlating with worsening socioeconomic conditions indicated by higher Social Deprivation Index scores.
-
Admissions did not rise significantly during the early pandemic (first 3 months, p = 0.160), but mid-to-late phases showed a significant increase (p = 0.001).
-
Injury severity, as measured by Injury Severity Score, declined, suggesting less severe injuries during the pandemic.
-
These findings emphasize the need for proactive interventions and continuous surveillance to protect vulnerable populations.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 14 print issues and online access
$259.00 per year
only $18.50 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
The datasets and R codes generated during and/or analyzed during the current study are available from the corresponding author upon reasonable request.
References
Hairston, T. K. S. et al. A traumatic pandemic: high acuity pediatric trauma in the COVID-19 era. Injury 53, 3289–3292 (2022).
Huang, N. et al. The prevalences, changes, and related factors of child maltreatment during the COVID-19 pandemic: a systematic review. Child. Abus. Negl. 135, 105992 (2023).
Zeanah, C. H. & Humphreys, K. L. Child abuse and neglect. J. Am. Acad. Child. Adolesc. Psychiatry 57, 637–644 (2018).
Loiseau, M. et al. Physical abuse of young children during the COVID-19 pandemic: Alarming increase in the relative frequency of hospitalizations during the lockdown period. Child. Abus. Negl. 122, 105299 (2021).
Stewart, S. L., Toohey, A., Celebre, A. & Poss, J. W. Abuse, mental state, and health factors pre and during the COVID-19 pandemic: a comparison among clinically referred adolescents in Ontario, Canada. Int. J. Environ. Res. Public. Health 18, 10184 (2021).
Tso, W. W. Y. et al. Mental health & maltreatment risk of children with special educational needs during COVID-19. Child. Abus. Negl. 130, 105457 (2022).
De Boer, C. et al. Effect of the COVID-19 pandemic on presentation and severity of traumatic injury due to physical child abuse across US children’s hospitals. J. Pediatr. Surg. 57, 726–731 (2022).
Katz, I. et al. One year into COVID-19: what have we learned about child maltreatment reports and child protective service responses? Child. Abus. Negl. 130, 105473 (2022).
Chaiyachati, B. H. et al. Emergency department child abuse evaluations during COVID-19: A multicenter study. Pediatrics 150, e2022056284 (2022).
Theodorou, C. M., Brown, E. G., Jackson, J. E. & Beres, A. L. Child abuse and the COVID-19 pandemic. J. Surg. Res. 276, 18–23 (2022).
Swedo, E. et al. Trends in U.S. emergency department visits related to suspected or confirmed child abuse and neglect among children and adolescents aged <18 years before and during the COVID-19 pandemic—United States, January 2019–September 2020. MMWR Morb. Mortal. Wkly. Rep. 69, 1841–1847 (2020).
The White House. Proclamation on declaring a national emergency concerning the novel coronavirus disease (COVID-19) outbreak. https://trumpwhitehouse.archives.gov/presidential-actions/proclamation-declaring-national-emergency-concerning-novel-coronavirus-disease-covid-19-outbreak/ (2020).
von Elm, E. et al. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet 370, 1453–1457 (2007).
Kovler, M. L. et al. Increased proportion of physical child abuse injuries at a level I pediatric trauma center during the COVID-19 pandemic. Child. Abus. Negl. 116, 104756 (2021).
NPR. Biden ends COVID national emergency after Congress acts. https://www.npr.org/2023/04/11/1169191865/biden-ends-covid-national-emergency.
Mummaneni, P. V. et al. Predictors of nonroutine discharge among patients undergoing surgery for grade I spondylolisthesis: insights from the Quality Outcomes Database. J. Neurosurg. Spine 32, 523–532 (2019).
Kazemi, F. et al. Evaluating the atherosclerosis cardiovascular disease risk score in patients with brain metastases: associations with overall survival and high-value care outcomes. Clin. Neurol. Neurosurg. 246, 108549 (2024).
Kazemi, F., Liu, J., Nasr, I. W., Robinson, S. & Cohen, A. R. A comparative analysis of the Trauma and Injury Severity Score and the Injury Severity Score in predicting high-value care outcomes in children with traumatic brain injury. J. Neurosurg. Pediatr. https://doi.org/10.3171/2024.8.PEDS24309 (2024).
Hedegaard, H. B., Johnson, R. L. & Ballesteros, M. F. Proposed ICD-10-CM surveillance case definitions for injury hospitalizations and emergency department visits. Natl. Health Stat. Rep. Number 100, 1–8 (2017).
De Crescenzo, L. A., Gabella, B. A. & Johnson, J. Interrupted time series design to evaluate ICD-9-CM to ICD-10-CM coding changes on trends in Colorado emergency department visits related to traumatic brain injury. Inj. Epidemiol. 8, 1–6 (2021).
Butler, D. C., Petterson, S., Phillips, R. L. & Bazemore, A. W. Measures of social deprivation that predict health care access and need within a rational area of primary care service delivery. Health Serv. Res. 48, 539–559 (2013).
Skiba, M. B., Lind, K. E., Felion, C. M., Krupnik, C. & Segrin, C. Connected Community Classification (C3): development, validation, and geospatial application for population health promotion and equity. J. Public Health Manag. Pract. 30, E74–E83 (2024).
Reshetnyak, E. et al. Impact of multiple social determinants of health on incident stroke. Stroke 51, 2445–2453 (2020).
White-Williams, C. et al. Addressing social determinants of health in the care of patients with heart failure: a scientific statement from the American Heart Association. Circulation 141, e841–e863 (2020).
Alcaraz, K. I. et al. Understanding and addressing social determinants to advance cancer health equity in the United States: a blueprint for practice, research, and policy. CA Cancer J. Clin. 70, 31–46 (2020).
Stekhoven, D. J. & Bühlmann, P. MissForest—non-parametric missing value imputation for mixed-type data. Bioinformatics 28, 112–118 (2012).
Breiman, L. Random forests. Mach. Learn. 45, 5–32 (2001).
Waljee, A. K. et al. Comparison of imputation methods for missing laboratory data in medicine. BMJ Open 3, e002847 (2013).
R: Ljung-Box Test Plot. https://search.r-project.org/CRAN/refmans/LSTS/html/Box.Ljung.Test.html.
Ljung, G. M. & Box, G. E. P. On a measure of lack of fit in time series models. Biometrika 65, 297–303 (1978).
Chan, K. C. G., Han, J., Kennedy, A. P. & Yam, S. C. P. Testing network autocorrelation without replicates. PLoS ONE 17, e0275532 (2022).
Brodersen, K. H., Gallusser, F., Koehler, J., Remy, N. & Scott, S. L. Inferring causal impact using Bayesian structural time-series models. Ann. Appl. Stat. 9, 247–274 (2015).
Feder, K. A., Mojtabai, R., Stuart, E. A., Musci, R. & Letourneau, E. J. Florida’s opioid crackdown and mortality from drug overdose, motor vehicle crashes, and suicide: a Bayesian interrupted time-series analysis. Am. J. Epidemiol. 189, 885–893 (2020).
Martin, J., Cunliffe, J., Décary-Hétu, D. & Aldridge, J. Effect of restricting the legal supply of prescription opioids on buying through online illicit marketplaces: interrupted time series analysis. BMJ 361, k2270 (2018).
Walley, A. Y. et al. Opioid overdose rates and implementation of overdose education and nasal naloxone distribution in Massachusetts: interrupted time series analysis. BMJ 346, f174–f174 (2013).
Ghose, R., Forati, A. M. & Mantsch, J. R. Impact of the COVID-19 pandemic on opioid overdose deaths: a spatiotemporal analysis. J. Urban Health 99, 316–327 (2022).
CausalImpact. https://cran.r-project.org/web/packages/CausalImpact/vignettes/CausalImpact.html.
Lawson, M., Piel, M. H. & Simon, M. Child maltreatment during the COVID-19 pandemic: consequences of parental job loss on psychological and physical abuse towards children. Child. Abus. Negl. 110, 104709 (2020).
Rodriguez, C. M. & Lee, S. J. Role of maternal emotion in child maltreatment risk during the COVID-19 pandemic. J. Fam. Violence 38, 977–987 (2023).
Karbasi, Z., Safdari, R. & Eslami, P. The silent crisis of child abuse in the COVID-19 pandemic: a scoping review. Health Sci. Rep. 5, 790 (2022).
Sidpra, J., Abomeli, D., Hameed, B., Baker, J. & Mankad, K. Rise in the incidence of abusive head trauma during the COVID-19 pandemic. Arch. Dis. Child. 106, e14 (2021).
Rapoport, E., Reisert, H., Schoeman, E. & Adesman, A. Reporting of child maltreatment during the SARS-CoV-2 pandemic in New York City from March to May 2020. Child. Abus. Negl. 116, 104719 (2021).
Sharma, S. et al. COVID-19: differences in sentinel injury and child abuse reporting during a pandemic. Child. Abus. Negl. 116, 104990 (2021).
Fornacon-Wood, I. et al. Understanding the differences between Bayesian and frequentist statistics. Int. J. Radiat. Oncol. Biol. Phys. 112, 1076–1082 (2022).
van IJzendoorn, M. H., Bakermans-Kranenburg, M. J., Coughlan, B. & Reijman, S. Annual Research Review: Umbrella synthesis of meta-analyses on child maltreatment antecedents and interventions: differential susceptibility perspective on risk and resilience. J. Child. Psychol. Psychiatry 61, 272–290 (2020).
Rafaiee, R., Mohseni, F. & Akbarian, N. Prevalence of child abuse and correlations with family factors among elementary school-aged children. Int. J. High Risk Behav. Addict. 10, 1–8 (2021).
Doidge, J. C. et al. Economic predictors of child maltreatment in an Australian population-based birth cohort. Child. Youth Serv. Rev. 72, 14–25 (2017).
Huang, M. I. et al. Increased incidence of nonaccidental head trauma in infants associated with the economic recession. J. Neurosurg. Pediatr. 8, 171–176 (2011).
Molnar, B. E. et al. Neighborhood-level social processes and substantiated cases of child maltreatment. Child. Abus. Negl. 51, 41–53 (2016).
Maguire-Jack, K. & Font, S. A. Community and individual risk factors for physical child abuse and child neglect: variations by poverty status. Child. Maltreat. 22, 215–226 (2017).
Ruffolo, L. I. et al. Outcomes after child physical abuse and association with community-level social determinants of health. J. Am. Coll. Surg. 235, 810–818 (2022).
Bezzo, F. B., Silva, L. & van Ham, M. The combined effect of Covid-19 and neighbourhood deprivation on two dimensions of subjective well-being: empirical evidence from England. PLoS ONE 16, e0255156 (2021).
Geranios, K., Kagabo, R. & Kim, J. Impact of COVID-19 and socioeconomic status on delayed care and unemployment. Health Equity 6, 91–97 (2022).
Wolf, E. R. et al. School closure and child maltreatment during the COVID-19 pandemic. Child. Maltreat. 29, 500–507 (2024).
Palusci, V. J. & Botash, A. S. Race and bias in child maltreatment diagnosis and reporting. Pediatrics 148, e2020049625 (2021).
Villaveces, A. & Viswanathan, S. Violence against children: multifaceted approaches to a complex problem. Int. J. Inj. Contr. Saf. Promot. 29, 1–2 (2022).
Branco, M. S. S., Altafim, E. R. P. & Linhares, M. B. M. Universal intervention to strengthen parenting and prevent child maltreatment: updated systematic review. Trauma Violence Abuse 23, 1658–1676 (2022).
Casillas, K. L., Fauchier, A., Derkash, B. T. & Garrido, E. F. Implementation of evidence-based home visiting programs aimed at reducing child maltreatment: a meta-analytic review. Child. Abus. Negl. 53, 64–80 (2016).
Walsh, K. et al. Child protection training for professionals to improve reporting of child abuse and neglect. Cochrane Database Syst. Rev. 7, 011775 (2022).
Bernal, J. L., Cummins, S. & Gasparrini, A. Interrupted time series regression for the evaluation of public health interventions: a tutorial. Int. J. Epidemiol. 46, 348–355 (2017).
Bernal, J. L., Cummins, S. & Gasparrini, A. The use of controls in interrupted time series studies of public health interventions. Int. J. Epidemiol. 47, 2082–2093 (2018).
Ewusie, J. E. et al. Methods, applications and challenges in the analysis of interrupted time series data: a scoping review. J. Multidiscip. Health 13, 411–423 (2020).
Moynihan, R. et al. Impact of COVID-19 pandemic on utilisation of healthcare services: a systematic review. BMJ Open 11, e045343 (2021).
Zhou, X., Andes, L. J., Rolka, D. B. & Imperatore, G. Changes in health care utilization among Medicare beneficiaries with diabetes two years into the COVID-19 pandemic. AJPM Focus 2, 100117 (2023).
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
Substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data: F.K. and A.C. Drafting the article: F.K. and J.L. Revising the article critically for important intellectual content: all authors. Final approval of the version to be published: all authors.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Consent statement
This study was approved by the IRB at our institution with the waiver of consent.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kazemi, F., Liu, J., Nasr, I.W. et al. COVID-19’s causal impact on child abuse and socioeconomic status: a Bayesian time series study. Pediatr Res 98, 599–610 (2025). https://doi.org/10.1038/s41390-025-03996-0
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41390-025-03996-0