Abstract
Background
Packed red blood cell (pRBC) transfusions are often required in extremely premature infants but are associated with increased pro-inflammatory cytokines and adverse neurodevelopment, which may differ by sex.
Methods
In this post-hoc analysis of the Preterm Erythropoietin Neuroprotection (PENUT) Trial, associations between pRBC transfusion volume and cytokines at 0–7 and 7–14 days, MRI injury, and Bayley Scales of Infant Development (BSID-III) scores at 24 months corrected age were evaluated. Graphical network and generalized estimating equation models were used to examine interactions by sex as well as the influence of hematocrit level.
Results
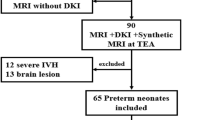
182 and 164 infants were assessed with biomarkers at 0–7 and 7–14 days, 220 infants had MRIs, and 692 infants had at least one BSID-III assessment. Infant sex modified the association between pRBC transfusion volume and IL-6 at 7–14 days but did not impact the association between transfusion volume or hematocrit and BSID-III scores. Total pRBC transfusion volume was significantly negatively associated with all BSID-III subscales after accounting for anemia and severity of illness.
Conclusion
Infant sex may impact short-term cytokine responses to transfusions but not the association between transfusion volume and long-term outcomes.
Impact
-
In a post hoc analysis of extremely preterm infants from the PENUT Trial, the relationship between transfusion exposure and pro-inflammatory cytokines, MRI scores and neurodevelopment were evaluated by sex.
-
The impact of transfusions on inflammatory cytokines may vary by sex. However, this does not appear to lead to differences in neurodevelopmental outcomes.
-
Based on current evidence, providers should not alter their transfusion practices based on sex of the infant.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 14 print issues and online access
$259.00 per year
only $18.50 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Strauss, R. G. Anaemia of prematurity: pathophysiology and treatment. Blood Rev. 24, 221–225 (2010).
Widness, J. A. et al. Changing patterns of red blood cell transfusion in very low birth weight infants. J. Pediatr. 129, 680–687 (1996).
Keir, A. K., Yang, J., Harrison, A., Pelausa, E. & Shah, P. S. Temporal changes in blood product usage in preterm neonates born at less than 30 weeks’ gestation in Canada. Transfusion 55, 1340–1346 (2015).
Maier, R. F. et al. Changing practices of red blood cell transfusions in infants with birth weights less than 1000 g. J. Pediatr. 136, 220–224 (2000).
Bell, E. F. Red cell transfusion thresholds for preterm infants: finally some answers. Arch. Dis. Child Fetal Neonatal Ed. 107, 126–130 (2022).
Cooke, R. W., Drury, J. A., Yoxall, C. W. & James, C. Blood transfusion and chronic lung disease in preterm infants. Eur. J. Pediatr. 156, 47–50 (1997).
Valieva, O. A., Strandjord, T. P., Mayock, D. E. & Juul, S. E. Effects of transfusions in extremely low birth weight infants: a retrospective study. J. Pediatr. 155, 331–37.e1 (2009).
Zhang, Z., Huang, X. & Lu, H. Association between red blood cell transfusion and bronchopulmonary dysplasia in preterm infants. Sci. Rep. 4, 4340 (2014).
Blau, J. et al. Transfusion-related acute gut injury: necrotizing enterocolitis in very low birth weight neonates after packed red blood cell transfusion. J. Pediatr. 158, 403–409 (2011).
Christensen, R. D. Associations between “early” red blood cell transfusion and severe intraventricular hemorrhage, and between “late” red blood cell transfusion and necrotizing enterocolitis. Semin Perinatol. 36, 283–289 (2012).
Christensen, R. D., Baer, V. L., Del Vecchio, A. & Henry, E. Unique risks of red blood cell transfusions in very-low-birth-weight neonates: associations between early transfusion and intraventricular hemorrhage and between late transfusion and necrotizing enterocolitis. J. Matern Fetal Neonatal Med 26, 60–63 (2013).
Singh, R., Shah, B. L. & Frantz, I. D. 3rd. Necrotizing enterocolitis and the role of anemia of prematurity. Semin Perinatol. 36, 277–282 (2012).
Stokes V., Rajai A., Mukherjee D.& Mukherjee A. Transfusion-associated necrotizing enterocolitis (NEC) in extremely preterm infants: experience of a tertiary neonatal center in UK. J. Matern. Fetal. Neonatal. Med. 1–6 (2021). https://doi.org/10.1080/14767058.2021.1874910.
Paul, D. A. et al. Increased odds of necrotizing enterocolitis after transfusion of red blood cells in premature infants. Pediatrics 127, 635–641 (2011).
Patel, R. M. et al. Association of Red Blood Cell Transfusion, Anemia, and Necrotizing Enterocolitis in Very Low-Birth-Weight Infants. JAMA 315, 889–897 (2016).
Dani, C. et al. The role of blood transfusions and iron intake on retinopathy of prematurity. Early Hum. Dev. 62, 57–63 (2001).
Inder, T. E., Clemett, R. S., Austin, N. C., Graham, P. & Darlow, B. A. High iron status in very low birth weight infants is associated with an increased risk of retinopathy of prematurity. J. Pediatr. 131, 541–544 (1997).
Zhu, Z. et al. Effect of red blood cell transfusion on the development of retinopathy of prematurity: A systematic review and meta-analysis. PLoS One 15, e0234266 (2020).
Baer, V. L. et al. Among very-low-birth-weight neonates is red blood cell transfusion an independent risk factor for subsequently developing a severe intraventricular hemorrhage?. Transfusion 51, 1170–1178 (2011).
Christensen, R. D. et al. Association, among very-low-birthweight neonates, between red blood cell transfusions in the week after birth and severe intraventricular hemorrhage. Transfusion 54, 104–108 (2014).
Basu, S., Agarwal, P., Anupurba, S., Shukla, R. & Kumar, A. Elevated plasma and cerebrospinal fluid interleukin-1 beta and tumor necrosis factor-alpha concentration and combined outcome of death or abnormal neuroimaging in preterm neonates with early-onset clinical sepsis. J. Perinatol. 35, 855–861 (2015).
Hagberg, H. et al. The role of inflammation in perinatal brain injury. Nat. Rev. Neurol. 11, 192–208 (2015).
Keir, A. K., McPhee, A. J., Andersen, C. C. & Stark, M. J. Plasma cytokines and markers of endothelial activation increase after packed red blood cell transfusion in the preterm infant. Pediatr. Res 73, 75–79 (2013).
Leviton, A. et al. The relationship between early concentrations of 25 blood proteins and cerebral white matter injury in preterm newborns: the ELGAN study. J. Pediatr. 158, 897–903 (2011).
Procianoy, R. S. & Silveira, R. C. Association between high cytokine levels with white matter injury in preterm infants with sepsis. Pediatr. Crit. Care Med. 13, 183–187 (2012).
Stark, M. J., Keir, A. K. & Andersen, C. C. Does non-transferrin bound iron contribute to transfusion related immune-modulation in preterms?. Arch. Dis. Child Fetal Neonatal Ed. 98, F424–F429 (2013).
Crawford, T. M., Andersen, C. C. & Stark, M. J. Effect of repeat transfusion exposure on plasma cytokine and markers of endothelial activation in the extremely preterm neonate. Transfusion 60, 2217–2224 (2020).
Franz, A. R. et al. Effects of Liberal vs Restrictive Transfusion Thresholds on Survival and Neurocognitive Outcomes in Extremely Low-Birth-Weight Infants: The ETTNO Randomized Clinical Trial. JAMA 324, 560–570 (2020).
Juul S. E. et al. Effect of High-Dose Erythropoietin on Blood Transfusions in Extremely Low Gestational Age Neonates: Post Hoc Analysis of a Randomized Clinical Trial. JAMA Pediatr. (2020). https://doi.org/10.1001/jamapediatrics.2020.2271.
Kirpalani, H. et al. Higher or Lower Hemoglobin Transfusion Thresholds for Preterm Infants. N. Engl. J. Med. 383, 2639–2651 (2020).
Phuong, T. V. et al. Transfusions and neurodevelopmental outcomes in extremely low gestation neonates enrolled in the PENUT Trial: a randomized clinical trial. Pediatr. Res. 90, 109–116 (2021).
Vu, P. T. et al. Transfusions and neurodevelopmental outcomes in extremely low gestation neonates enrolled in the PENUT Trial: a randomized clinical trial. Pediatr. Res 90, 109–116 (2021).
Benavides, A. et al. Sex-specific cytokine responses and neurocognitive outcome after blood transfusions in preterm infants. Pediatr. Res. (2021). https://doi.org/10.1038/s41390-021-01536-0.
Vandenbroucke, J. P. et al. Strengthening the Reporting of Observational Studies in Epidemiology (STROBE): explanation and elaboration. PLoS Med. 4, e297 (2007).
Juul S. E., Mayock D. E., Comstock B. A. & Heagerty P. J. Neuroprotective Potential of Erythropoietin in Neonates; design of a randomized trial. Maternal Health, Neonatol. Perinatol.1, (2015). https://doi.org/10.1186/s40748-015-0028-z.
Juul, S. E. et al. A Randomized Trial of Erythropoietin for Neuroprotection in Preterm Infants. N. Engl. J. Med. 382, 233–243 (2020).
Wood, T. R. et al. Early Biomarkers of Hypoxia and Inflammation and Two-Year Neurodevelopmental Outcomes in the Preterm Erythropoietin Neuroprotection (PENUT) Trial. EBioMed. 72, 103605 (2021).
Mayock, D. E. et al. Association between Term Equivalent Brain Magnetic Resonance Imaging and 2-Year Outcomes in Extremely Preterm Infants: A Report from the Preterm Erythropoietin Neuroprotection Trial Cohort. J. Pediatrics 239, 117–125 (2021). E6.
Law, J. B. et al. Diffusion Tensor Imaging Changes Do Not Affect Long-Term Neurodevelopment following Early Erythropoietin among Extremely Preterm Infants in the Preterm Erythropoietin Neuroprotection Trial. Brain Sci. 11, 1360 (2021).
Kidokoro, H., Neil, J. J. & Inder, T. E. New MR Imaging Assessment Tool to Define Brain Abnormalities in Very Preterm Infants at Term. Am. J. Neuroradiol. 34, 2208–2214 (2013).
Papile, L. A., Burnstein, J., Burnstein, R. & Koffler, H. Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weight less than. 1500 gm. J. Pediatrics 92, 529–534 (1978).
Williams, D. R. & Rast, P. Back to the basics: Rethinking partial correlation network methodology. Br. J. Math. Stat. Psychol. 73, 187–212 (2020).
Dani, C. et al. Red blood cell transfusions can induce proinflammatory cytokines in preterm infants. Transfusion 57, 1304–1310 (2017).
Hod, E. A. et al. Transfusion of red blood cells after prolonged storage produces harmful effects that are mediated by iron and inflammation. Blood 115, 4284–4292 (2010).
Patel, R. M. et al. Association of Blood Donor Sex and Age With Outcomes in Very Low-Birth-WeightInfants Receiving Blood Transfusion. JAMA Netw. Open 4, e2123942 (2021).
Vu, P. T. et al. Transfusions and neurodevelopmental outcomes in extremely low gestation neonates enrolled in the PENUT Trial: a randomized clinical trial. Pediatr. Res. 90, 109–116 (2021).
Shah P. et al. Effect of blood transfusions on cognitive development in very low birth weight infants. J. Perinatol 41, 1412–1418 (2021).
German, K. et al. Zinc Protoporphyrin-to-heme Ratio and Ferritin as Measures of Iron Sufficiency in the Neonatal Intensive Care Unit. J. Pediatrics 194, 47–53 (2018).
Benavides, A. et al. Sex Differences in the Association of Pretransfusion Hemoglobin Levels with Brain Structure and Function in the Preterm Infant. J. Pediatrics S0022-3476, 01258–0 (2021).
Lung, F. W., Shu, B. C., Chiang, T. L., Chen, P. F. & Lin, L. L. Predictive validity of Bayley scale in language development of children at 6-36 months. Pediatrics Int. 51, 666–669 (2009).
Durrant, C. et al. Developmental trajectories of infants born at less than 30 weeks’ gestation on the Bayley-III Scales. Arch. Dis. Child.-Fetal Neonatal Ed. 105, 623–627 (2020).
Song, J. et al. The association of severe anemia, red blood cell transfusion and necrotizing enterocolitis in neonates. PLOS One 16, e0254810 (2021).
Mohamed, A. & Shah, P. S. Transfusion associated necrotizing enterocolitis: a meta-analysis of observational data. Pediatrics 129, 529–540 (2012).
Wan-Huen, P., Bateman, D., Shapiro, D. M. & Parravicini, E. Packed red blood cell transfusion is an independent risk factor for necrotizing enterocolitis in premature infants. J. Perinatol. 33, 786–790 (2013).
O’Shea, T. M. et al. Elevated concentrations of inflammation-related proteins in postnatal blood predict severe developmental delay at 2 years of age in extremely preterm infants. J. Pediatrics 160, 395–401 (2021).
Leviton, A. et al. The relationship between early concentrations of 25 blood proteins and cerebral white matter injury in preterm newborns: the ELGAN study. J. Pediatrics 158, 897–903 (2011).
Acknowledgements
We would like to recognize Roberta Ballard, MD, University of California, San Francisco School of Medicine, who provided unflagging support and advice throughout the PENUT Trial, for which she was compensated. We thank the research coordinators from all 19 sites and 30 hospitals who made the PENUT study possible. Mark A. Konodi, MS, and Christopher Nefcy, BS, University of Washington, Seattle, at the data coordinating center, kept the PENUT Portal running. John A. Widness, MD, University of Iowa, Iowa City, served as PENUT Medical Monitor during the years of PENUT enrollment, for which he was compensated. The genetics core of the UW Intellectual and Developmental Disability Research Center processed the inflammatory biomarkers.
Funding
The PENUT Trial was funded by the NINDS, U01NS077955 and U01NS077953. Work for the biomarker analysis was supported in part by the NICHD, 5P50HD103524.
Author information
Authors and Affiliations
Consortia
Contributions
KRG, TRW, SG, PJH, DEM, BAC, MPD, SK, UM, JL, KP, GV and SEJ conceived the manuscript. TKB oversaw sample processing and generation of the biomarker immunoassay data. BAC, PJH and SEJ verified the data and TRW performed the statistical analyses. TRW made the tables and figures. KRG, TRW, SG drafted the manuscript. All authors contributed to editing the manuscript and approved the final draft. DEM, PJH and SEJ oversaw the methodology and administration of the PENUT Trial and resulting investigations. SEJ was the PI of the PENUT Trial and oversaw the Trial.
Corresponding author
Ethics declarations
Competing interests
Dr Juul reported receiving grants from the National Institutes of Health (NIH), CP Alliance, and Gates Foundation Grant during the conduct of the study. Mr. Comstock reported receiving grants from the NIH during the conduct of the study. Dr Heagerty reported receiving grants from the NIH to the University of Washington during the conduct of the study. No other disclosures were reported.
Ethical approval and consent for approval
The families of all participants in the primary PENUT Trial provided informed, written consent for their participation in the randomized trial. This consent included the use of data in secondary analyses, such as this one.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
German, K., Wood, T.R., Gogcu, S. et al. Neurodevelopmental outcomes after red cell transfusion exposure in male versus female extremely preterm infants. Pediatr Res 98, 2186–2194 (2025). https://doi.org/10.1038/s41390-025-04149-z
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41390-025-04149-z
This article is cited by
-
Biological sex and transfusion practices in the NICU
Pediatric Research (2025)