Abstract
Background
To present the clinical characteristics, diagnostic approach, therapeutic management, and outcomes of congenital H-type tracheoesophageal fistula (H-TEF) based on the experience of the National Center for Children’s Health in China.
Methods
A retrospective review of patients with H-TEF from 2007 to 2025 was performed. Patients were stratified by the occurrence of major complications (Clavien-Dindo grade ≥ III) for comparative analysis. Univariate analyses were performed to identify associated risk factors.
Results
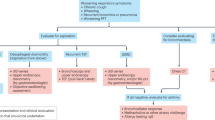
The study cohort comprised 51 patients. The median age at diagnosis was 1 month. Bronchoscopy demonstrated the highest detection rate (100%), followed by upper gastrointestinal contrast study (UGI) (96%). None of the patients who underwent precise fistula localization (with placement of a polyester traction suture) developed anastomotic leakage or recurrent fistula. The overall complication rate was 41.2%, with a major complication rate of 29.4%. No statistically significant risk factors for major complications were identified within this cohort.
Conclusions
Modifying patient positioning during UGI can enhance its diagnostic ability. Precise localization of the fistula tract and the use of nerve monitoring may help minimize postoperative complications. While no risk factors achieved statistical significance, the study was not powered to exclude potential clinically relevant effects.
Impact
-
An upper gastrointestinal contrast study can reach a diagnostic yield of 96% under proper positioning during the procedure.
-
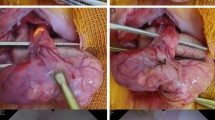
Intraoperative precision localization of the fistula demonstrated favorable outcomes and reduced surgical complexity.
-
No recurrent laryngeal nerve injury occurred in any patient who underwent intraoperative nerve monitoring (overall incidence 13.73%).
-
Complications occurred in 41.2% (29.4% major). No statistically significant risk factors were detected, although clinical effects cannot be entirely ruled out due to the limited cohort size.
-
Despite representing the largest reported cohort in China to date, future prospective, multi-center studies with extended follow-up are warranted.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 14 print issues and online access
$259.00 per year
only $18.50 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are not publicly available due to privacy restrictions, but are available from the corresponding author on reasonable request.
References
Sampat, K. & Losty, P. D. Diagnostic and management strategies for congenital H-Type Tracheoesophageal fistula: a systematic review. Pediatr. Surg. Int. 37, 539–547 (2021).
van Lennep, M. et al. Oesophageal Atresia. Nat. Rev. Dis. Prim. 5, 26 (2019).
Li, G. et al. Comprehensive insights into Tracheoesophageal Fistula pathophysiology, diagnosis, treatment, and future directions. Adv. Sci. 12, e02825 (2025).
Gross, R. E. The Surgery of Infancy and Childhood: Its Principles and Techniques WB Saunders, (1953).
Więckowski, P. R., Łysak, J. M., Maciejewski, I. Z. & Wolski, M. A cautionary tale: undetected H-Type Tracheoesophageal Fistula in an adolescent male. Cureus 16, e57647 (2024).
Anadolulu, A. I. et al. Comparison of diagnostic methods, surgical approaches and outcome for congenital H-Type Tracheoesophageal fistula: a systematic review. J. Pediatr. Surg. 60, 162343 (2025).
Koivusalo, A. I., Suominen, J. S., Nokso-Koivisto, J. & Pakarinen, M. P. Vocal cord paralysis after repair of esophageal atresia. Eur. J. Pediatr. Surg. 34, 50–55 (2023).
Ebbott, D. et al. Long-term aerodigestive morbidities after Esophageal Atresia/Tracheoesophageal fistula repair. J. Pediatr. Surg. 60, 162384 (2025).
Fallon, S. C. et al. Congenital H-Type Tracheoesophageal Fistula: a multicenter review of outcomes in a rare disease. J. Pediatr. Surg. 52, 1711–1714 (2017).
Zani, A. et al. Long-term outcomes following h-Type Tracheoesophageal Fistula repair in Infants. Pediatr. Surg. Int. 33, 187–190 (2017).
Dai, J. et al. Experience of diagnosis and treatment of 31 H-Type Tracheoesophageal fistula in a single clinical center. Pediatr. Surg. Int. 34, 715–719 (2018).
Taghavi, K. et al. H-Type Congenital Tracheoesophageal Fistula: Insights from 70 Years of the Royal Children’s Hospital Experience. J. Pediatr. Surg. 56, 686–691 (2021).
Morchio, C. et al. Diagnosis and management of congenital H-Type Tracheoesophageal Fistula: Results of a National Survey. Children 11, 423 (2024).
Solomon, B. D. Vacterl/Vater Association. Orphanet J. Rare Dis. 6, 56 (2011).
van de Putte, R. et al. Spectrum of congenital anomalies among Vacterl cases: A Eurocat population-based study. Pediatr. Res 87, 541–549 (2019).
Clavien, P. A. et al. The Clavien-Dindo classification of surgical complications: five-year experience. Ann. Surg. 250, 187–196 (2009).
Holder, T. M., Cloud, D. T., Lewis, J. E. & Pilling, G. P. Esophageal Atresia and Tracheoesophageal Fistula. A survey of its members by the surgical section of the American Academy of Pediatrics. Pediatrics 34, 542–549 (1964).
Al-Salem, A. H., Mohaidly, M. A., Al-Buainain, H. M. H., Al-Jadaan, S. & Raboei, E. Congenital H-Type Tracheoesophageal Fistula: A National Multicenter Study. Pediatr. Surg. Int. 32, 487–491 (2016).
Suen, H. C. Congenital H-type tracheoesophageal fistula in adults. J. Thorac. Dis. 10, S1905–S1910 (2018).
Yang, S. et al. Detail correction for gross classification of Esophageal Atresia based on 434 cases in China. Chin. Med. J. 135, 485–487 (2021).
Ng, J., Antao, B., Bartram, J., Raghavan, A. & Shawis, R. Diagnostic difficulties in the management of H-type Tracheoesophageal Fistula. Acta Radio. 47, 801–805 (2006).
Tiwari, C., Nagdeve, N., Saoji, R., Nama, N. & Khan, M. A. Congenital H-type Tracheo-Oesophageal fistula: an institutional review of a 10-year period. J. Mother Child 24, 2–8 (2021).
He, Q. et al. Flexible endoscopic identification and catheterization of congenital H-Type Tracheoesophageal fistula using a laryngeal mask. Dig. Endosc. 34, 228–233 (2021).
Parolini, F. et al. Cervical/Thoracotomic/Thoracoscopic approaches for H-type congenital Tracheo-Esophageal fistula: a systematic review. Int J. Pediatr. Otorhinolaryngol. 78, 985–989 (2014).
Genty, E. et al. Congenital Tracheoesophageal fistula without esophageal Atresia. Int J. Pediatr. Otorhinolaryngol. 48, 231–238 (1999).
Hua, K. et al. The intraoperative localization in recurrent Tracheoesophageal Fistula after Esophageal Atresia repair: a comparative study. BMC Pediatr. 24, 796 (2024).
Zhao, J. et al. Thoracoscopic repair for esophageal pulmonary fistula after Esophageal Atresia Repair. J. Pediatr. Surg. 57, 538–542 (2022).
Toczewski, K., Rygl, M., Dzielendziak, A., Frybova, B. & Patkowski, D. Thoracoscopic repair of congenital isolated H-Type Tracheoesophageal Fistula. J. Pediatr. Surg. 56, 1386–1388 (2021).
Audry, G. et al. Postoperative Recurrence of Esophago-Tracheal Fistula. Significance of Peroperative Catheterization of the Fistula with Tracheoscopy. Apropos of 10 Cases. Chir. Pediatr. 30, 77–81 (1989).
Beasley, S. W. & Myers, N. A. The diagnosis of congenital Tracheoesophageal Fistula. J. Pediatr. Surg. 23, 415–417 (1988).
Garcia, N. M., Thompson, J. W. & Shaul, D. B. Definitive localization of isolated Tracheoesophageal Fistula using Bronchoscopy and Esophagoscopy for Guide Wire Placement. J. Pediatr. Surg. 33, 1645–1647 (1998).
Hotta, Y. et al. Precise localization of a recurrent Tracheo-Oesophageal Fistula using retrograde guide wire placement. Paediatr. Anaesth. 12, 541–543 (2002).
Conforti, A. et al. Cervical repair of congenital tracheoesophageal fistula: complications lurking!. J. Pediatr. Surg. 51, 1623–1626 (2016).
Acknowledgements
None.
Funding
This work was supported by Beijing Municipal Science & Technology Commission (Z211100002921062) and Natural Science Foundation of Tibet Autonomous Region (XZZR20242020[W]).
Author information
Authors and Affiliations
Contributions
Yong Zhao contributed to the study’s conception and design, acquisition of data, and critical revision of the manuscript for important intellectual content. Zonghan Li and Shihui Tan contributed to the conception and design, acquisition of data, analysis and interpretation of data, and drafting of the article. Junmin Liao, Shuangshuang Li, Dingding Wang, Kaiyun Hua, Yichao Gu, Yanan Zhang, Xinyue Tan, Zhaohong Zheng, Jinghua Jiao, Dan Don, and Dayan Sun contributed to the acquisition of data and interpretation of data. Jinshi Huang contributed to the study’s conception and design and final approval of the version to be published.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Consent statement
This retrospective chart review study involving human participants was in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This study obtained approval from the Ethics Committee of Beijing Children’s Hospital, Capital Medical University (Ethical approval ID: 2019-k-333). Individual consent for this retrospective analysis was waived.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhao, Y., Li, Z., Tan, S. et al. Congenital H-type tracheoesophageal fistula: Experience from a large Chinese center. Pediatr Res (2026). https://doi.org/10.1038/s41390-026-05050-z
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41390-026-05050-z