Abstract
Study Design
Retrospective multicenter study.
Objectives
To identify predictors associated with failure of neurological improvement after posterior decompression surgery for degenerative cervical myelopathy (DCM).
Setting
17 institutions in Japan.
Methods
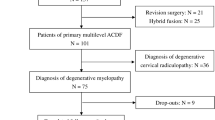
Patients who underwent posterior decompression surgery and were followed up for >1 year were enrolled. The Japanese Orthopedic Association (JOA) recovery rate was determined, and patients were divided into three outcome groups based on the JOA recovery rate: fair (recovery rate, <22.2%: mean-1SD), moderate (22.3%–77.1%), and good (>77.2%: mean+1 SD) groups. Demographic information, postoperative complications, and radiographic parameters were assessed, and predictors of poor outcomes were identified using the multinominal logistic regression analysis.
Results
Of 868 patients enrolled, 140 (16.1%), 586 (67.5%), and 142 (16.3%) were assigned to the fair, moderate, and good groups, respectively, with mean JOA recovery rates of 6.2% ± 13.7%, 50.1% ± 15.0%, and 90.6% ± 8.3%. Although there were significant differences in the frequency of diabetes mellitus among the three groups in the univariate analysis (26.4% vs. 23.0% vs. 14.1%; p = 0.03), the multinominal regression analysis revealed that old age was a significant independent predictor of poor outcomes in the comparison between the fair and good groups (odds ratio [OR], 1.62; 95% confidence interval [CI], 1.27–2.07; p < 0.01). Old age was also significantly associated with failure of neurological improvement between the fair and moderate groups (OR, 1.35; 95% CI 1.15–1.59; p < 0.01).
Conclusions
Old age may be an independent predictor of failure of neurological improvement after posterior decompression surgery in patients with DCM.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
The datasets generated and analyzed in this study are available from the corresponding author on request.
References
Fehlings MG, Tetreault LA, Wilson JR, Skelly AC. Cervical spondylotic myelopathy: current state of the art and future directions. Spine (Phila Pa 1976). 2013;38:S1–8.
Nouri A, Tetreault L, Singh A, Karadimas SK, Fehlings MG. Degenerative cervical myelopathy: epidemiology, genetics, and pathogenesis. Spine (Phila Pa 1976). 2015;40:E675–93.
King JT Jr., Tsevat J, Moossy JJ, Roberts MS. Preference-based quality of life measurement in patients with cervical spondylotic myelopathy. Spine (Phila Pa 1976). 2004;29:1271–80.
Nakashima H, Tetreault LA, Nagoshi N, Nouri A, Kopjar B, Arnold PM, et al. Does age affect surgical outcomes in patients with degenerative cervical myelopathy? Results from the prospective multicenter AOSpine International study on 479 patients. J Neurol Neurosurg Psychiatry. 2016;87:734–40.
Hirabayashi K, Satoshi K. Operative procedure and results of expansive open-door laminoplasty. Spine (Phila Pa 1976). 1988;13:870–6.
Seichi A, Takeshita K, Ohishi I, Kawaguchi H, Akune T, Anamizu Y, et al. Long-term results of double-door laminoplasty for cervical stenotic myelopathy. Spine (Phila Pa 1976). 2001;26:479–87.
Shiraishi T, Fukuda K, Yato Y, Nakamura M, Ikegami T. Results of skip laminectomy-minimum 2-year follow-up study compared with open-door laminoplasty. Spine (Phila Pa 1976). 2003;28:2667–72.
Karpova A, Arun R, Davis AM, Kulkarni AV, Massicotte EM, Mikulis DJ, et al. Predictors of surgical outcome in cervical spondylotic myelopathy. Spine (Phila Pa 1976). 2013;38:392–400.
Kim HJ, Moon SH, Kim HS, Moon ES, Chun HJ, Jung M, et al. Diabetes and smoking as prognostic factors after cervical laminoplasty. J Bone Joint Surg Br. 2008;90:1468–72.
Tetreault L, Wilson JR, Kotter MR, Nouri A, Côté P, Kopjar B, et al. Predicting the minimum clinically important difference in patients undergoing surgery for the treatment of degenerative cervical myelopathy. Neurosurg Focus. 2016;40:E14.
Kohno K, Kumon Y, Oka Y, Matsui S, Ohue S, Sakaki S. Evaluation of prognostic factors following expansive laminoplasty for cervical spinal stenotic myelopathy. Surg Neurol. 1997;48:237–45.
Fujimura Y, Nishi Y, Chiba K, Nakamura M, Hirabayashi K. Multiple regression analysis of the factors influencing the results of expansive open-door laminoplasty for cervical myelopathy due to ossification of the posterior longitudinal ligament. Arch Orthop Trauma Surg. 1988;117:471–4.
Kato S, Oshima Y, Oka H, Chikuda H, Takeshita Y, Miyoshi K, et al. Comparison of the Japanese Orthopaedic Association (JOA) score and modified JOA (mJOA) score for the assessment of cervical myelopathy: a multicenter observational study. PLoS One. 2015;10:e0123022.
Kato S, Oshima Y, Matsubayashi Y, Taniguchi Y, Tanaka S, Takeshita K. Minimum clinically important difference and patient acceptable symptom state of japanese orthopaedic association score in degenerative cervical myelopathy patients. Spine (Phila Pa 1976). 2019;44:691–7.
Chiba K, Toyama Y, Matsumoto M, Maruiwa H, Watanabe M, Hirabayashi K. Segmental motor paralysis after expansive open-door laminoplasty. Spine (Phila Pa 1976). 2002;27:2108–15.
Hirabayashi K, Miyakawa J, Satomi K, Maruyama T, Wakano K. Operative results and postoperative progression of ossification among patients with ossification of cervical posterior longitudinal ligament. Spine (Phila Pa 1976). 1981;6:354–64.
Zhang JT, Wang LF, Wang S, Li J, Shen Y. Risk factors for poor outcome of surgery for cervical spondylotic myelopathy. Spinal Cord. 2016;54:1127–31.
Matsuda Y, Shibata T, Oki S, Kawatani Y, Mashima N, Oishi H. Outcomes of surgical treatment for cervical myelopathy in patients more than 75 years of age. Spine (Phila Pa 1976). 1999;24:529–34.
Tetreault LA, Kopjar B, Vaccaro A, Yoon ST, Arnold PM, Massicotte EM, et al. A clinical prediction model to determine outcomes in patients with cervical spondylotic myelopathy undergoing surgical treatment: data from the prospective, multi-center AOSpine North America study. J Bone Joint Surg Am. 2013;95:1659–66.
Tetreault LA, Côté P, Kopjar B, Arnold P, Fehlings MG. A clinical prediction model to assess surgical outcome in patients with cervical spondylotic myelopathy: internal and external validations using the prospective multicenter AOSpine North American and international datasets of 743 patients. Spine J. 2015;15:388–97.
Hasegawa K, Homma T, Chiba Y, Hirano T, Watanabe K, Yamazaki A. Effects of surgical treatment for cervical spondylotic myelopathy in patients > or = 70 years of age: a retrospective comparative study. J Spinal Disord Tech. 2002;15:458–60.
Isogai N, Nagoshi N, Iwanami A, Kono H, Kobayashi Y, Tsuji T. Surgical treatment of cervical spondylotic myelopathy in the elderly: outcomes in patients aged 80 years or older. Spine (Phila Pa 1976). 2018;43:E1430–e6.
Pop-Busui R, Boulton AJ, Feldman EL, Bril V, Freeman R, Malik RA, et al. Diabetic neuropathy: a position statement by the American diabetes association. Diabetes care. 2017;40:136–54.
Arnold PM, Fehlings MG, Kopjar B, Yoon ST, Massicotte EM, Vaccaro AR, et al. Mild diabetes is not a contraindication for surgical decompression in cervical spondylotic myelopathy: results of the AOSpine North America multicenter prospective study (CSM). Spine J. 2014;14:65–72.
Machino M, Yukawa Y, Ito K, Inoue T, Kobayakawa A, Matsumoto T, et al. Risk factors for poor outcome of cervical laminoplasty for cervical spondylotic myelopathy in patients with diabetes. J Bone Joint Surg Am. 2014;96:2049–55.
Smith JS, Lafage V, Ryan DJ, Shaffrey CI, Schwab FJ, Patel AA, et al. Association of myelopathy scores with cervical sagittal balance and normalized spinal cord volume: analysis of 56 preoperative cases from the AOSpine North America Myelopathy study. Spine (Phila Pa 1976). 2013;38:S161–70.
Uehara M, Takahashi J, Ikegami S, Tokida R, Nishimura H, Sakai N, et al. Sagittal spinal alignment deviation in the general elderly population: a Japanese cohort survey randomly sampled from a basic resident registry. Spine J. 2019;19:349–56.
Pedro KM, Alvi MA, Hejrati N, Quddusi AI, Singh A, Fehlings MG. Machine learning-based cluster analysis identifies four unique phenotypes of patients with degenerative cervical myelopathy with distinct clinical profiles and long-term functional and neurological outcomes. EBioMedicine. 2024;106:105226.
Martin AR, Jentzsch T, Wilson JRF, Moghaddamjou A, Jiang F, Rienmueller A, et al. Inter-rater reliability of the modified Japanese orthopedic association score in degenerative cervical myelopathy: a cross-sectional study. Spine (Phila Pa 1976). 2021;46:1063–9.
Ganau M, Holly LT, Mizuno J, Fehlings MG. Future directions and new technologies for the management of degenerative cervical myelopathy. Neurosurg Clin N Am. 2018;29:185–93.
Acknowledgements
The authors would like to thank Dr Soraya Nishimura, Shusuke Matsuda, Kazuki Takeda, Yuichiro Mima and Ryutaro Tanaka for collection of data.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Author information
Authors and Affiliations
Contributions
SS contributed to the data collection, data analysis, data interpretation and preparation of the initial draft of the manuscript. NN and JY contributed to the study design, data analysis, data interpretation, and assistance with manuscript preparation. KF, RA, OT, EO, NF, MY, TT, KW were responsible for the data collection and interpretation of the results. MN, MM, KI were responsible for the interpretation of the results, and supervision of the manuscript. All authors critically reviewed and approved the final version.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
This study was conducted following the tenets of the World Medical Association Declaration of Helsinki, and performed after approval from the Ethics and Institutional Review Board of Keio University School of Medicine (approval number: #20110142). All participants provided informed consent before surgery.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Suzuki, S., Nagoshi, N., Fujiyoshi, K. et al. Predictors of poor outcomes after posterior decompression surgery in patients with degenerative cervical myelopathy. Spinal Cord 63, 538–543 (2025). https://doi.org/10.1038/s41393-025-01107-8
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41393-025-01107-8