Abstract
Study design
Cross-sectional study.
Objective
To identify the relationship of prescription opioid use, self-reported misuse of opioids, and binge drinking days with suicidal ideation (SI) in a cohort of participants with spinal cord injury (SCI).
Setting
Medical university in the southeastern United States.
Methods
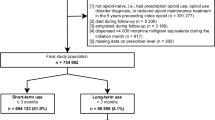
This was a cross-sectional analysis of self-report data from 1253 study participants with SCI, all of whom were enrolled in a longitudinal study of health outcomes. SI was assessed and dichotomized using item 9 on the Patient Health Questionnaire-9.
Results
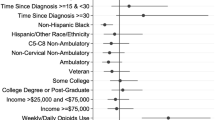
Occasional use of 3 or more prescription opioids was associated with greater odds of SI (OR = 3.53, CI = 1.50–8.31), as was self-reported misuse of prescription opioids (OR = 3.51, CI = 1.83–6.72). Days of binge drinking was unrelated to SI. Odds of SI were higher for those with depression (OR = 5.98, CI = 3.60–9.92) and those who reported 15 or more painful days in a month (OR = 2.15, CI = 1.24–3.73). Compared with the most severe SCI (high cervical, non-ambulatory), participants who were ambulatory (OR = 0.36, CI = 0.15-0.86) or were non-cervical/non-ambulatory (OR = 0.32, CI = 0.14-0.75) reported lower odds of SI.
Conclusions
Prescription opioid use needs to be closely monitored by healthcare professionals for those who use multiple opioids and who self-report misusing opioids, as there is a relationship with SI, even when considering multiple covariates pain and depression.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Data availability
The data set is not currently publicly available and has not been sufficiently de-identified. It will be made publicly available at the end grant cycle, consistent with federal regulations.
References
Jensen MP, Truitt AR, Schomer KG, Yorkston KM, Baylor C, Molton IR. Frequency and age effects of secondary health conditions in individuals with spinal cord injury: a scoping review. Spinal Cord. 2013;51:882–92.
Hagen EM, Rekand T. Management of neuropathic pain associated with spinal cord injury. Pain. Ther. 2015;4:51–65.
Jensen MP, Molton IR, Groah SL, Campbell ML, Charlifue S, Chiodo A, et al. Secondary health conditions in individuals aging with SCI: terminology, concepts and analytic approaches. Spinal Cord. 2012;50:373–8.
Hatch MN, Cushing TR, Carlson GD, Chang EY. Neuropathic pain and SCI: Identification and treatment strategies in the 21st century. J. Neurol. Sci. 2018;384:75–83.
McCullumsmith CB, Kalpakjian CZ, Richards JS, Forchheimer M, Heinemann AW, Richardson EJ, et al. Novel risk factors associated with current suicidal ideation and lifetime suicide attempts in individuals with spinal cord injury. Arch. Phys. Med. Rehabil. 2015;96:799–808.
Cao Y, Massaro JF, Krause JS, Chen Y, Devivo MJ. Suicide mortality after spinal cord injury in the United States: injury cohorts analysis. Arch. Phys. Med. Rehabil. 2014;95:230–5.
Clark JMR, Krause JS. Suicidal ideation among individuals aging with spinal cord injury. Rehabil. Psychol. 2024;69:153–8.
Graupensperger S, Corey JJ, Turrisi RJ, Evans MB. Individuals with spinal cord injury have greater odds of substance use disorders than non-sci comparisons. Drug. Alcohol. Depend. 2019;205:107608.
Clark JM, Cao Y, Krause JS. Risk of pain medication misuse after spinal cord injury: the role of substance use, personality, and depression. J. Pain. 2017;18:166–77.
Krause JS, DiPiro ND, Dismuke-Greer CE. Self-Reported prescription opioid use among participants with chronic spinal cord injury. Top. Spinal Cord. Inj. Rehabil. 2024;30:131–9.
Engel GL. The need for a new medical model: a challenge for biomedicine. Science. 1977;196:129–36.
Krause JS, Dismuke-Greer CE, DiPiro ND, Clark JMR, Laursen-Roesler J. Relationships of Self-reported opioid use and misuse and pain severity with probable major depression among participants with spinal cord injury. Arch. Phys. Med. Rehabil. 2024;105:1506–12.
Centers for Disease Control and Prevention. Web-based Injury Statistics Query and Reporting System 2022. Accessed March 15, 2025. https://wisqars.cdc.gov/lcd/?o=LCD&y1=2022&y2=2022&ct=12&cc=ALL&g=00&s=0&r=0&ry=3&e=0&ar=lcd1age&at=groups&ag=lcd1age&a1=0&a2=199.
Williams R, Murray A. Prevalence of depression after spinal cord injury: a meta-analysis. Arch. Phys. Med. Rehabil. 2015;96:133–40.
Judd FK, Brown DJ. Suicide following acute traumatic spinal cord injury. Paraplegia. 1992;30:173–7.
Racine M. Chronic pain and suicide risk: a comprehensive review. Prog. Neuropsychopharmacol. Biol. Psychiatry. 2018;87:269–80.
Shoup JA, Welter J, Binswanger IA, Hess F, Dullenkopf A, Coker J, et al. Spinal cord injury and prescribed opioids for pain: a scoping review. Pain. Med. 2023;24:1138–52.
DiPiro ND, Murday D, Corley EH, DiPiro TV, Krause JS. Opioid use among individuals with spinal cord injury: prevalence estimates based on state prescription drug monitoring program data. Arch. Phys. Med. Rehabil. 2021;102:828–34.
Hand BN, Krause JS, Simpson KN. Dose and duration of opioid use in propensity score-matched, privately insured opioid users with and without spinal cord injury. Arch. Phys. Med. Rehabil. 2018;99:855–61.
Guilcher SJT, Hogan ME, Calzavara A, Hitzig SL, Patel T, Packer T, et al. Prescription drug claims following a traumatic spinal cord injury for older adults: a retrospective population-based study in Ontario, Canada. Spinal Cord. 2018;56:1059–68.
Harris PA, Taylor R, Minor BL, Elliott V, Fernandez M, O’Neal L, et al. The REDCap consortium: Building an international community of software platform partners. J. Biomed. Inf. 2019;95:103208.
National Survey on Drug Use and Health (NSDUH). The 2019 National Survey on Drug Use and Health. Rockville, MD., USA: Dept. of Health & Human Services, Substance Abuse & Mental Health Services Administration, Center for Behavioral Health Statistics and Quality.; 2019. Accessed March 15, 2025. https://www.samhsa.gov/data/sites/default/files/reports/rpt23057/NSDUHmrbCAISpecs2019.pdf.
Centers for Disease Control and Prevention (CDC). Behavioral Risk Factor Surveillance System Survey Questionnaire. Atlanta, Georgia: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention; 2010. Accessed March 15, 2025. http://www.cdc.gov/brfss/questionnaires/pdf-ques/2010brfss.pdf.
The National Institute on Alcohol Abuse and Alcoholism (NIAAA). Defining binge drinking. What colleges need to know now 2007. Accessed March 15, 2025. https://www.collegedrinkingprevention.gov/sites/cdp/files/documents/1College_Bulletin-508_361C4E.pdf.
Kroenke K, Spitzer RL, Williams JB. The PHQ-9: validity of a brief depression severity measure. J. Gen. Intern. Med. 2001;16:606–13.
Rossom RC, Coleman KJ, Ahmedani BK, Beck A, Johnson E, Oliver M, et al. Suicidal ideation reported on the PHQ9 and risk of suicidal behavior across age groups. J. Affect. Disord. 2017;215:77–84.
Louzon SA, Bossarte R, McCarthy JF, Katz IR. Does suicidal ideation as measured by the PHQ-9 predict suicide among VA patients? Psychiatr. Serv. 2016;67:517–22.
Ataoglu E, Tiftik T, Kara M, Tunc H, Ersoz M, Akkus S. Effects of chronic pain on quality of life and depression in patients with spinal cord injury. Spinal Cord. 2013;51:23–6.
Kennedy P, Hasson L. The relationship between paid and mood following spinal cord injury. J. Spinal Cord. Med. 2017;40:275–9.
Craig A, Tran Y, Middleton J. Psychological morbidity and spinal cord injury: a systematic review. Spinal Cord. 2009;47:108–14.
Mashola MK, Korkie E, Mothabeng DJ. Exploring the experience of living with pain after spinal cord injury: a qualitative study. Behav. Neurol. 2024;2024:9081530.
Charlifue SW, Gerhart KA. Behavioral and demographic predictors of suicide after traumatic spinal cord injury. Arch. Phys. Med. Rehabil. 1991;72:488–92.
Rizk MM, Herzog S, Dugad S, Stanley B. Suicide risk and addiction: the impact of alcohol and opioid use disorders. Curr. Addict. Rep. 2021;8:194–207.
Hunt C, Moman R, Peterson A, Wilson R, Covington S, Mustafa R, et al. Prevalence of chronic pain after spinal cord injury: a systematic review and meta-analysis. Reg. Anesth. Pain. Med. 2021;46:328–36.
van Gorp S, Kessels AG, Joosten EA, van Kleef M, Patijn J. Pain prevalence and its determinants after spinal cord injury: a systematic review. Eur. J. Pain. 2015;19:5–14.
Fuentes AV, Pineda MD, Venkata KCN. Comprehension of top 200 prescribed drugs in the US as a resource for pharmacy teaching, training and practice. Pharmacy. 2018;6:43.
Bohnert ASB, Ilgen MA. Understanding links among opioid use, overdose, and suicide. N. Engl. J. Med. 2019;380:71–9.
Ilgen MA, Bohnert ASB, Ganoczy D, Bair MJ, McCarthy JF, Blow FC. Opioid dose and risk of suicide. Pain. 2016;157:1079–84.
Centers for Disease Control and Prevention. About Prescription Opioids 2025 updated 2025. Accessed March 15, 2025. https://www.cdc.gov/overdose-prevention/about/prescription-opioids.html?CDC_AAref_Val=https://www.cdc.gov/opioids/basics/prescribed.html.
Scherrer JF, Salas J, Copeland LA, Stock EM, Ahmedani BK, Sullivan MD, et al. Prescription opioid duration, dose, and increased risk of depression in 3 large patient populations. Ann. Fam. Med. 2016;14:54–62.
Bryce TN. Opioids should not be prescribed for chronic pain after spinal cord injury. Spinal Cord. Ser. Cases. 2018;4:66.
Funding
The contents of this publication were developed under a grant from the National Institute on Disability, Independent Living, and Rehabilitation Research (NIDILRR grant number 90DPHF0009). NIDILRR is a Center within the Administration for Community Living (ACL), Department of Health and Human Services (HHS). The contents of this publication do not necessarily represent the policy of NIDILRR, ACL, HHS, and you should not assume endorsement by the Federal Government.
Author information
Authors and Affiliations
Contributions
JK was the principal investigator who developed the purpose and overall design and who contributed to the development of the methods, discussion and conclusion sections. CDG was responsible for conducting the analyses and writeup of the statistical methods. DS developed the introduction and parts of the discussion and contributed to the development of the results. ND contributed to the literature review, as well as linking the current findings to the literature.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval and consent to participate
We certify that all applicable institutional and governmental regulations concerning the ethical use of human volunteers were followed during the course of this research. This study was approved by the Institutional Review Board (IRB) of the Medical University of South Carolina (Pro00104259). Informed consent was obtained from all participants, with a waiver of written informed consent approved by the IRB.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Krause, J.S., Dismuke-Greer, C.E., Smith, D.E. et al. Relationship of prescription and nonprescription opioid use, opioid misuse, and alcohol use with suicidal ideation among people with spinal cord injury. Spinal Cord (2026). https://doi.org/10.1038/s41393-026-01192-3
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41393-026-01192-3