Abstract
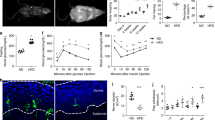
Diabetic peripheral neuropathy (DPN), a severe complication of diabetes, is a key risk factor for diabetic foot (DF) that contributes highly to amputation and mortality. The pathogenesis of DPN remains unclear and complex, with no effective treatments currently available. Monoamine oxidase (MAO), a flavin adenine dinucleotide (FAD)-dependent enzyme, catalyzes the oxidative deamination of critical biogenic amines. The MAO family comprises two subtypes, MAOA and MAOB, which play distinct roles in pathophysiology. In this study, we identified that MAOB but not MAOA is pathologically upregulated in the sciatic nerve (SN) tissues of DPN patients and in the SN/dorsal root ganglion (DRG) tissues of DPN model mice. Notably, the selective MAOB inhibitor Khellin (Khe) effectively alleviated DPN-like pathology in mice. To explore the mechanistic role of MAOB in DPN, we performed proteomic profiling of DRG tissues from DPN mice and validated the findings using a MAOB-specific knockdown DPN mice model treated with adeno-associated virus (AAV) 8-MAOB-RNAi. Our results demonstrate that Khe targets MAOB to mitigate DPN pathology through HIF-1α/BACE1/Aβ/NLRP3/tau pathway, mediated by Schwann cell/DRG neuron crosstalk. All findings suggest that selective MAOB inhibition represents a promising therapeutic strategy for DPN, with Khe as a potential candidate for clinical translation against this disease.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
References
Jang HN, Oh TJ. Pharmacological and nonpharmacological treatments for painful diabetic peripheral neuropathy. Diabetes Metab J. 2023;47:743–56.
Sun H, Saeedi P, Karuranga S, Pinkepank M, Ogurtsova K, Duncan BB, et al. IDF diabetes atlas: global, regional and country-level diabetes prevalence estimates for 2021 and projections for 2045. Diabetes Res Clin Pract. 2022;183:109119.
Su HY, Yang CY, Ou HT, Chen SG, Chen JC, Ho HJ, et al. Cost-effectiveness of novel macrophage-regulating treatment for wound healing in patients with diabetic foot ulcers from the Taiwan health care sector perspective. JAMA Netw Open. 2023;6:e2250639.
Marshall A, Alam U, Themistocleous A, Calcutt N, Marshall A. Novel and emerging electrophysiological biomarkers of diabetic neuropathy and painful diabetic neuropathy. Clin Ther. 2021;43:1441–56.
Elafros MA, Andersen H, Bennett DL, Savelieff MG, Viswanathan V, Callaghan BC, et al. Towards prevention of diabetic peripheral neuropathy: clinical presentation, pathogenesis, and new treatments. Lancet Neurol. 2022;21:922–36.
Lian J, Wang H, Cui R, Zhang C, Fu J. Status of analgesic drugs and quality of life results for diabetic peripheral neuropathy in China. Front Endocrinol. 2021;12:813210.
Feldman EL, Callaghan BC, Pop-Busui R, Zochodne DW, Wright DE, Bennett DL, et al. Diabetic neuropathy. Nat Rev Dis Primers. 2019;5:41.
Jia L, Du Y, Chu L, Zhang Z, Li F, Lyu D, et al. Prevalence, risk factors, and management of dementia and mild cognitive impairment in adults aged 60 years or older in China: a cross-sectional study. Lancet Public Health. 2020;5:e661–e671.
Janelidze S, Teunissen CE, Zetterberg H, Allue JA, Sarasa L, Eichenlaub U, et al. Head-to-head comparison of 8 plasma amyloid-beta 42/40 assays in Alzheimer disease. JAMA Neurol. 2021;78:1375–82.
Engelsman AsiriMMH, Eijkelkamp S, Hoppener N. JWM. Amyloid proteins and peripheral neuropathy. Cells. 2020;9:1553.
Jolivalt CG, Calcutt NA, Masliah E. Similar pattern of peripheral neuropathy in mouse models of type 1 diabetes and Alzheimer’s disease. Neuroscience. 2012;202:405–12.
Shigemori K, Nomura S, Umeda T, Takeda S, Tomiyama T. Peripheral Aβ acts as a negative modulator of insulin secretion. Proc Natl Acad Sci USA. 2022;119:e2117723119.
Lee HJ, Ryu JM, Jung YH, Lee SJ, Kim JY, Lee SH, et al. High glucose upregulates BACE1-mediated Abeta production through ROS-dependent HIF-1alpha and LXRalpha/ABCA1-regulated lipid raft reorganization in SK-N-MC cells. Sci Rep. 2016;6:36746.
Banerjee C, Tripathy D, Kumar D, Chakraborty J. Monoamine oxidase and neurodegeneration: mechanisms, inhibitors and natural compounds for therapeutic intervention. Neurochem Int. 2024;179:105831.
Naoi M, Maruyama W, Shamoto-Nagai M, Riederer P. Type a monoamine oxidase; its unique role in mood, behavior and neurodegeneration. J Neural Transm. 2025;132:387–406.
Lv Y, Zheng Z, Liu R, Guo J, Zhang C, Xie Y. Monoamine oxidase b inhibitors based on natural privileged scaffolds: a review of systematically structural modification. Int J Biol Macromol. 2023;251:126158.
Buneeva O, Medvedev A. Monoamine oxidase inhibitors in toxic models of Parkinsonism. Int J Mol Sci. 2025;26:1248.
Kim TT, Xu C, Amsterdam JD. Comparison of effectiveness and side effects of selegiline transdermal system versus oral monoamine oxidase inhibitors and tricyclic antidepressants for treatment-resistant depression. J Affect Disord. 2025;376:47–51.
Duarte P, Sánchez-Porro FJ, Crisman E, Cores A, Jiménez I, Cuadrado A, et al. Network-based drug optimization toward the treatment of Parkinson’s disease: NRF2, MAO-B, oxidative stress, and chronic neuroinflammation. J Med Chem. 2025;68:3495–517.
Chun H, Im H, Kang YJ, Kim Y, Shin JH, Won W, et al. Severe reactive astrocytes precipitate pathological hallmarks of Alzheimer’s disease via H2O2-production. Nat Neurosci. 2020;23:1555–66.
Sanchez-Rodriguez R, Munari F, Angioni R, Venegas F, Agnellini A, Castro-Gil MP, et al. Targeting monoamine oxidase to dampen NLRP3 inflammasome activation in inflammation. Cell Mol Immunol. 2021;18:1311–3.
Chen Q, Xu Y, Zhang H, Tan X, Liu SH, Yan F. Immunocytochemical localization of monoamine oxidase type b in rat’s peripheral nervous system. J Biochem Mol Toxicol. 2015;29:521–5.
Manzoor S, Hoda N. A comprehensive review of monoamine oxidase inhibitors as anti-Alzheimer’s disease agents: a review. Eur J Med Chem. 2020;206:112787.
Li Q, Li X, Tian B, Chen L. Protective effect of pterostilbene in a streptozotocin-induced mouse model of Alzheimer’s disease by targeting monoamine oxidase b. J Appl Toxicol. 2022;42:1777–86.
Miranda HF, Sierralta F, Jorquera V, Poblete P, Prieto JC, Noriega V. Antinociceptive interaction of gabapentin with minocycline in murine diabetic neuropathy. Inflammopharmacology. 2017;25:91–7.
De Gregorio C, Contador D, Diaz D, Carcamo C, Santapau D, Lobos-Gonzalez L, et al. Human adipose-derived mesenchymal stem cell-conditioned medium ameliorates polyneuropathy and foot ulceration in diabetic bks db/db mice. Stem Cell Res Ther. 2020;11:168.
Chaplan SR, Bach FW, Pogrel JW, Chung JM, Yaksh TL. Quantitative assessment of tactile allodynia in the rat paw. J Neurosci Methods. 1994;53:55–63.
Fan B, Li C, Szalad A, Wang L, Pan W, Zhang R, et al. Mesenchymal stromal cell-derived exosomes ameliorate peripheral neuropathy in a mouse model of diabetes. Diabetologia. 2020;63:431–43.
Zhu X, Chen Y, Xu X, Xu X, Lu Y, Huang X, et al. SP6616, as a Kv2.1 inhibitor, efficiently ameliorates peripheral neuropathy in diabetic mice. EBioMedicine. 2020;61:103061.
Yang J, Wei Y, Zhao T, Li X, Zhao X, Ouyang X, et al. Magnolol effectively ameliorates diabetic peripheral neuropathy in mice. Phytomedicine. 2022;107:154434.
Xu X, Xu X, Hao Y, Zhu X, Lu J, Ouyang X, et al. Antispasmodic drug drofenine as an inhibitor of Kv2.1 channel ameliorates peripheral neuropathy in diabetic mice. iScience. 2020;23:101617.
Wisniewski JR, Zougman A, Nagaraj N, Mann M. Universal sample preparation method for proteome analysis. Nat Methods. 2009;6:359–62.
Xu X, Wang W, Wang Z, Lv J, Xu X, Xu J, et al. DW14006, as a direct AMPKα activator, ameliorates diabetic peripheral neuropathy in mice. Diabetes. 2020;69:1974–88.
Ouyang X, Zhu D, Huang Y, Zhao X, Xu R, Wang J, et al. Khellin as a selective monoamine oxidase b inhibitor ameliorated paclitaxel-induced peripheral neuropathy in mice. Phytomedicine. 2023;111:154673.
Tian L, Yang M, Tu S, Chang K, Jiang H, Jiang Y, et al. Xiaoke Bitong capsule alleviates inflammatory impairment via inhibition of the TNF signaling pathway against diabetic peripheral neuropathy. Phytomedicine. 2024;132:155867.
Eid SA, Rumora AE, Beirowski B, Bennett DL, Hur J, Savelieff MG, et al. New perspectives in diabetic neuropathy. Neuron. 2023;111:2623–41.
Christianson JA, Ryals JM, Johnson MS, Dobrowsky RT, Wright DE. Neurotrophic modulation of myelinated cutaneous innervation and mechanical sensory loss in diabetic mice. Neuroscience. 2007;145:303–13.
Zhang K, Peng P, Huang J, Chen M, Liu F, Zhu C, et al. Integrating plasma metabolomics and gut microbiome to reveal the mechanisms of Huangqi Guizhi Wuwu Decoction intervene diabetic peripheral neuropathy. J Ethnopharmacol. 2024;319:117301.
Burgess J, Marshall A, Rapteas L, Hamill KJ, Marshall A, Malik RA, et al. Automated immunohistochemistry of intra-epidermal nerve fibres in skin biopsies: a proof-of-concept study. J Peripher Nerv Syst. 2024;29:329–38.
Chen H, Yang G, Xu DE, Du YT, Zhu C, Hu H, et al. Autophagy in oligodendrocyte lineage cells controls oligodendrocyte numbers and myelin integrity in an age-dependent manner. Neurosci Bull. 2025;41:374–90.
Yamaguchi M, Noda-Asano S, Inoue R, Himeno T, Motegi M, Hayami T, et al. Dipeptidyl peptidase (DPP)-4 inhibitors and pituitary adenylate cyclase-activating polypeptide, a DPP-4 substrate, extend neurite outgrowth of mouse dorsal root ganglia neurons: a promising approach in diabetic polyneuropathy treatment. Int J Mol Sci. 2024;25:8881.
Jia L, Wang L, Chopp M, Zhang Y, Szalad A, Zhang ZG. MicroRNA 146a locally mediates distal axonal growth of dorsal root ganglia neurons under high glucose and sildenafil conditions. Neuroscience. 2016;329:43–53.
Zhu Y, Han S, Li X, Gao Y, Zhu J, Yang X, et al. Paeoniflorin effect of Schwann cell-derived exosomes ameliorates dorsal root ganglion neurons apoptosis through IRE1alpha pathway. Evid Based Complement Alternat Med. 2021;2021:6079305.
Zhang L, Fu J, Cheng XH, Tang L. Tau protein function: the mechanical exploration of axonal transport disorder caused by persistent pressure in dorsal root ganglia. Mol Genet Genomic Med. 2019;7:e00580.
Yang K, Wang Y, Li YW, Chen YG, Xing N, Lin HB, et al. Progress in the treatment of diabetic peripheral neuropathy. Biomed Pharmacother. 2022;148:112717.
Marquez A, Guernsey LS, Frizzi KE, Cundiff M, Constantino I, Muttalib N, et al. Tau-associated peripheral and central neurodegeneration: identification of an early imaging marker for tauopathy. Neurobiol Dis. 2021;151:105273.
Kasa P, Papp H, Kovacs I, Forgon M, Penke B, Yamaguchi H. Human amyloid-beta1-42 applied in vivo inhibits the fast axonal transport of proteins in the sciatic nerve of rat. Neurosci Lett. 2000;278:117–9.
Lučiūnaitė A, McManus RM, Jankunec M, Rácz I, Dansokho C, Dalgėdienė I, et al. Soluble Aβ oligomers and protofibrils induce NLRP3 inflammasome activation in microglia. J Neurochem. 2020;155:650–61.
Ising C, Venegas C, Zhang S, Scheiblich H, Schmidt SV, Vieira-Saecker A, et al. NLRP3 inflammasome activation drives tau pathology. Nature. 2019;575:669–73.
Kling L, Schreiber A, Eckardt KU, Kettritz R. Hypoxia-inducible factors not only regulate but also are myeloid-cell treatment targets. J Leukoc Biol. 2021;110:61–75.
Callapina M, Zhou J, Schmid T, Kohl R, Brune B. No restores HIF-1alpha hydroxylation during hypoxia: Role of reactive oxygen species. Free Radic Biol Med. 2005;39:925–36.
Fandrey J. Oxygen-dependent and tissue-specific regulation of erythropoietin gene expression. Am J Physiol Regul Integr Comp Physiol. 2004;286:R977–988.
Jaakkola P, Mole DR, Tian YM, Wilson MI, Gielbert J, Gaskell SJ, et al. Targeting of HIF-alpha to the von Hippel-Lindau ubiquitylation complex by O2-regulated prolyl hydroxylation. Science. 2001;292:468–72.
Willson JA, Arienti S, Sadiku P, Reyes L, Coelho P, Morrison T, et al. Neutrophil HIF-1alpha stabilization is augmented by mitochondrial ROS produced via the glycerol 3-phosphate shuttle. Blood. 2022;139:281–6.
Lu C, Zhang Z, Fan Y, Wang X, Qian J, Bian Z. Shikonin induces ferroptosis in osteosarcomas through the mitochondrial ROS-regulated HIF-1alpha/HO-1 axis. Phytomedicine. 2024;135:156139.
Choi J, Chandrasekaran K, Inoue T, Muragundla A, Russell JW. PGC-1alpha regulation of mitochondrial degeneration in experimental diabetic neuropathy. Neurobiol Dis. 2014;64:118–30.
Lee S, Lee H, Kim KT. Optimization of experimental conditions and measurement of oxygen consumption rate (OCR) in zebrafish embryos exposed to organophosphate flame retardants (OPFRs). Ecotoxicol Environ Saf. 2019;182:109377.
Premkumar LS, Pabbidi RM. Diabetic peripheral neuropathy: role of reactive oxygen and nitrogen species. Cell Biochem Biophys. 2013;67:373–83.
Shippy DC, Evered AH, Ulland TK. Ketone body metabolism and the NLRP3 inflammasome in Alzheimer’s disease. Immunol Rev. 2025;329:e13365.
Xu JW, Ma L, Xiang Y, Dai MQ, Li QH, Jin XY, et al. Glabridin as a selective Kv2.1 inhibitor ameliorates DPN pathology by disrupting the Abeta/Kv2.1/JNK/NF-kappaB/NLRP3/p-Tau pathway. Acta Pharmacol Sin. 2025;46:2163–79.
Heneka MT, Kummer MP, Stutz A, Delekate A, Schwartz S, Vieira-Saecker A, et al. NLRP3 is activated in Alzheimer’s disease and contributes to pathology in APP/PS1 mice. Nature. 2013;493:674–8.
Sun J, Zhang Y, Kong Y, Ye T, Yu Q, Kumaran Satyanarayanan S, et al. Microbiota-derived metabolite indoles induced aryl hydrocarbon receptor activation and inhibited neuroinflammation in APP/PS1 mice. Brain Behav Immun. 2022;106:76–88.
Lu J, Zhou Q, Zhu D, Song H, Xie G, Zhao X, et al. Drofenine, as a Kv2.1 inhibitor, alleviated AD-like pathology in mice through Abeta/Kv2.1/microglial NLRP3/neuronal tau axis. Acta Pharm Sin B. 2025;15:371–91.
Cui Y, Liu KW, Liang Y, Ip MS, Mak JC. Inhibition of monoamine oxidase-b by selegiline reduces cigarette smoke-induced oxidative stress and inflammation in airway epithelial cells. Toxicol Lett. 2017;268:44–50.
Chand Dakal T, Choudhary K, Tiwari I, Yadav V, Kumar Maurya P, Kumar Sharma N. Unraveling the triad: hypoxia, oxidative stress and inflammation in neurodegenerative disorders. Neuroscience. 2024;552:126–41.
Al-Thani NA, Stewart GS, Costello DA. The role of the urea cycle in the Alzheimer’s disease brain. J Neurochem. 2025;169:e70033.
Liang C, Yuan Z, Yang S, Zhu Y, Chen Z, Can D, et al. Mannose promotes beta-amyloid pathology by regulating BACE1 glycosylation in Alzheimer’s disease. Adv Sci. 2025;12:e2409105.
Vrzal R, Frauenstein K, Proksch P, Abel J, Dvorak Z, Haarmann-Stemmann T. Khellin and visnagin differentially modulate AHR signaling and downstream CYP1A activity in human liver cells. PLoS One. 2013;8:e74917.
Usmani QI, Jahan N, Aleem M, Hasan SA. Aatrilal (Ammi majus L.), an important drug of the Unani system of medicine: a review. J Ethnopharmacol. 2021;276:114144.
Reagan-Shaw S, Nihal M, Ahmad N. Dose translation from animal to human studies revisited. FASEB J. 2008;22:659–61.
Bhagavathula AS, Mahmoud Al-Khatib AJ, Elnour AA, Al Kalbani NM, Shehab A. Ammi Visnaga in treatment of urolithiasis and hypertriglyceridemia. Pharmacognosy Res. 2014;7:397–400.
Hofer A, Kerl H, Wolf P. Long-term results in the treatment of vitiligo with oral khellin plus UVA. Eur J Dermatol. 2001;11:225–9.
Harvengt C, Desager JP. HDL-cholesterol increase in normolipaemic subjects on khellin: a pilot study. Int J Clin Pharmacol Res. 1983;3:363–6.
Acknowledgements
This work was supported by the National Natural Science Foundation of China (82473982, 82273930), Major Program of the Natural Science Foundation of the Jiangsu Higher Education Institutions of China (23KJA350002), and the Innovation Projects of State Key Laboratory on Technologies for Chinese Medicine Pharmaceutical Process Control and Intelligent Manufacture (NZYSKL240110).
Author information
Authors and Affiliations
Contributions
XS, JYW, NXS, YCW and TZ designed the study. XS reviewed the paper. NXS, YCW, TZ, ZSZ, JCL, and ZYC performed the animal and cell experiments. NXS, YCW and TZ analyzed interpreted data. NXS, YJH and JYW wrote the paper. XS, NXS, YCW, TZ, ZSZ, JCL, ZYC, YJH and JYW are the guarantors of this work and, as such, have full access to all data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis. All authors approved the paper.
Corresponding authors
Ethics declarations
Competing interests
The corresponding author Xu Shen is a member of the Editorial Board of the journal Acta Pharmacologica Sinica, but he has not been involved in the peer-review or decision-making process for this manuscript.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Song, Nx., Wang, Yc., Zhao, T. et al. Selective inhibition of monoamine oxidase B represents a therapeutic strategy for diabetic peripheral neuropathy. Acta Pharmacol Sin (2026). https://doi.org/10.1038/s41401-026-01764-2
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41401-026-01764-2