Abstract
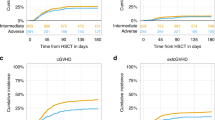
We assessed outcomes of allogeneic transplantation (HSCT) in favorable risk AML in CR1 over 3 time periods. 1850 patients were included, 2005 to 2009- 222, 2010 to 2014 -392, and 2015 to 2021-1236; 526 with t (8:21), 625 with inv (16), and 699 with NPM1mutFLT3WT. Patients transplanted in 2015–2021 were older (p < 0.0001) with more patients ≥60 years of age (p < 0.0001). The most frequent diagnosis in 2015–2021 was NPM1mutFLT3WT vs. t (8:21) in the 2 earlier periods, (p < 0001). Haploidentical transplants (Haplo) increased from 5.9% to 14.5% (p < 0.0001). Graft-versus-host disease (GVHD) prophylaxis with post-transplant cyclophosphamide (PTCy) was more frequent in 2015–2021 vs. the other 2 periods (p < 0.0001). On multivariate analysis, incidence of total chronic GVHD was reduced in HSCTs performed ≥2015 vs. those performed in 2005–2009, hazard ratio (HR) = 0.74 (95% CI 0.56–0.99, p = 0.046) and GVHD-free, relapse-free survival (GRFS) improved for patients transplanted from 2010–2014 vs. those transplanted in 2005–2009, HR = 0.74 (95% CI 0.56–0.98, p = 0.037). Other HSCT outcomes did not differ with no improvement ≥2015. LFS, OS, and GRFS were inferior in patients with t (8:21) with HR = 1.32 (95% CI 1.03–1.68, p = 0.026), HR = 1.38 (95% CI 1.04–1.83, p = 0.027) and HR = 01.25 (95% CI 1.02–1.53, p = 0.035), respectively. In conclusion, this retrospective analysis of HSCT in patients with favorable risk AML, transplanted over 16 years showed an increased number of transplants in patients ≥60 years, from Haplo donors with PTCy. Most importantly, 3-year GRFS improved ≥2010 and total chronic GVHD reduced ≥2015, with no significant change in other HSCT outcomes.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
AN, ML and MM had full access to all the data in the study (available upon data specific request).
References
Döhner H, Wei AH, Appelbaum FR, Craddock C, DiNardo CD, Dombret H, et al. Diagnosis and management of AML in adults: 2022 recommendations from an international expert panel on behalf of the ELN. Blood. 2022;140:1345–77.
Arber DA, Orazi A, Hasserjian RP, Borowitz MJ, Calvo KR, Kvasnicka HM, et al. International consensus classification of myeloid neoplasms and acute leukemias: integrating morphologic, clinical, and genomic data. Blood. 2022;140:1200–28.
Shimony S, Stahl M, Stone RM. Acute myeloid leukemia: 2023 update on diagnostic, risk-stratification, and management. Am J Hematol. 2023;98:502–26.
Dholaria B, Savani BN, Hamilton BK, Oran B, Liu HD, Tallman MS, et al. Hematopoietic cell transplantation in the treatment of newly diagnosed adult acute myeloid leukemia: an evidence-based review from the American Society of Transplantation and Cellular Therapy. Transpl Cell Ther. 2021;27:6–20.
Shouval R, Fein JA, Labopin M, Cho C, Bazarbachi A, Baron F, et al. Development and validation of a disease risk stratification system for patients with hematological malignancies: a retrospective cohort study of the European Society for Blood and Marrow Transplantation registry. Lancet Haematol. 2021;8:e205–15.
Shouval R, Labopin M, Bondi O, Mishan-Shamay H, Shimoni A, Ciceri F, et al. Prediction of allogeneic hematopoietic stem-cell transplantation mortality 100 days after transplantation using a machine learning algorithm: a European Group for Blood and Marrow Transplantation Acute Leukemia Working Party Retrospective Data Mining Study. J Clin Oncol. 2015;33:3144–51.
Borthakur G, Kantarijian H. Core binding factor acute myelogenous leukemia-2021 treatment algorithm. Blood Cancer J 2021;11:114.
Boddu P, Kantarjian H, Borthakur G, Kadia T, Daver N, Pierce S, et al. Co-occurrence of FLT3-TKD and NPM1 mutations defines a highly favorable prognostic AML group. Blood Adv. 2017;1:1546–50.
Schlenk RF, Benner A, Krauter J. Individual patient data-based meta-analysis of patients aged 16 to 60 years with core binding factor acute myeloid leukemia: a survey of the German Acute Myeloid Leukemia Intergroup. J Clin Oncol. 2004;22:3741–50.
Appelbaum FR, Kopecky KJ, Tallman MS. The clinical spectrum of adult acute myeloid leukaemia associated with core binding factor translocations. Br J Haeamtol. 2006;135:165–73.
Mosna F, Papayannidis C, Martinelli G. Complex karyotype, older age, and reduced first-line dose intensity determine poor survival in core binding factor acute myeloid leukemia patients with long-term follow-up. Am J Hematol. 2015;90:515–23.
Falini B, Brunetti L, Martelli MP. How I diagnosed and treat NPM1-mutated AML. Blood. 2021;137:589–99.
Cornelissen JJ, Gratwohl A, Schlenk RF, Sierra J, Bornhäuser M, Juliusson G, et al. The European LeukemiaNet AML Working Party consensus statement on allogeneic HSCT for patients with AML in remission: an integrated-risk adapted approach. Nat Rev Clin Oncol. 2012;9:579–90.
Halaburda K, Labopin M, Mailhol A, Socié G, Craddock C, Aljurf M, et al. Allogeneic stem cell transplantation in second complete remission for core binding factor acute myeloid leukemia: a study from the Acute Leukemia Working Party of the European Society for Blood and Marrow Transplantation. Haematologica. 2020;105:1723–30.
Loke J, Buka R, Craddock C. Allogeneic stem cell transplantation for acute myeloid leukemia: who, when, and how. Front Immunol. 2021;12:659595.
Bazarbachi A, Schmid C, Labopin M, Beelen D, Blau IW, Potter V, et al. Evaluation of Trends and prognosis over time in patients with AML relapsing after allogeneic hematopoietic cell transplant reveals improved survival for young patients in recent years. Clin Cancer Res. 2020;26:6475–82.
Nagler A, Ngoya M, Galimard JE, Labopin M, Bornhäuser M, Stelljes M, et al. Longitudinal outcome over two decades of unrelated allogeneic stem cell transplantation for relapsed/refractory acute myeloid leukemia: An ALWP/EBMT Analysis. Clin Cancer Res. 2022;28:4258–66.
Bazarbachi A, Labopin M, Gedde-Dahl T, Remenyi P, Forcade E, Kröger N, et al. Improved posttransplant outcomes in recent years for AML Patients with FLT3-ITD and wild-type NPM1: A Report from the EBMT Acute Leukemia Working Party. Clin Cancer Res. 2023;29:4441–8.
Bazarbachi A, Labopin M, Moukalled N, Kröger N, Rautenberg C, Schetelig J et al. Improvements in posttransplant outcomes over two decades in older patients with acute myeloid leukemia in the EBMT ALWP Study. Clin Cancer Res. 2024:OF1-OF10.
Shouval R, Fein JA, Labopin M, Kröger N, Duarte RF, Bader P, et al. Outcomes of allogeneic haematopoietic stem cell transplantation from HLA-matched and alternative donors: a European Society for Blood and Marrow Transplantation registry retrospective analysis. Lancet Haematol. 2019;6:e573–584.
Penack O, Peczynski C, Mohty M, Yakoub-Agha I, Styczynski J, Montoto S, et al. How much has allogeneic stem cell transplant-related mortality improved since the 1980s? A retrospective analysis from the EBMT. Blood Adv. 2020;4:6283–90.
Canaani J, Beohou E, Labopin M, Ghavamzadeh A, Beelen D, Hamladji RM, et al. Trends in patient outcome over the past two decades following allogeneic stem cell transplantation for acute myeloid leukaemia: an ALWP/EBMT analysis. J Intern Med. 2019;285:407–41.
McDonald GB, Sandmaier BM, Mielcarek M, Sorror M, Pergam SA, Cheng GS, et al. Survival, nonrelapse mortality, and relapse-related mortality after allogeneic hematopoietic cell transplantation: comparing 2003-2007 versus 2013-2017 cohort. Ann Intern Med. 2020;172:229–39.
Bacigalupo A, Ballen K, Rizzo D, Giralt S, Lazarus H, Ho V, et al. Defining the intensity of conditioning regimens: working definitions. Biol Blood Marrow Transpl. 2009;15:1628–33.
Przepiorka D, Weisdorf D, Martin P, Klingemann HG, Beatty P, Hows J, et al. Consensus conference on acute GVHD grading. Bone Marrow Transpl. 1995;15:825–8.
Shulman HM, Sullivan KM, Weiden PL, McDonald GB, Striker GE, Sale GE, et al. Chronic graft-versus-host syndrome in man. A long-term clinicopathologic study of 20 Seattle patients. Am J Med. 1980;69:204–17.
Ruggeri A, Labopin M, Ciceri F, Mohty M, Nagler A. Definition of GvHD-free, relapse-free survival for registry-based studies: an ALWP-EBMT analysis on patients with AML in remission. Bone Marrow Transpl. 2016;51:610–1.
Kanate AS, Nagler A, Savani B. Summary of scientific and statistical methods, study endpoints and definitions for observational and registry-based studies in hematopoietic cell transplantation. Clin Hematol Int. 2019;2:2–4.
Andersen PK, Klein JP, Zhang MJ. Testing for center effects in multi-center survival studies: a Monte Carlo comparison of fixed and random effects tests. Stat Med. 1999;18:1489–500.
R Core Team. R: a language and environment for statistical computing. R Foundation for Statistical Computing; 2020. https://www.R-project.org/.
A language and environment for statistical computing. https://www.R-project.org/. R Core Team: R Foundation for Statistical Computing, Vienna, Austria; 2020.
Rashidi A, Ebadi M, Colditz GA, DiPersio JF. Outcomes of allogeneic stem cell transplantation in elderly patients with acute myeloid leukemia: a systematic review and meta-analysis. Biol Blood Marrow Transpl. 2016;22:651–7.
Maffini E, Labopin M, Kröger N, Finke J, Stelljes M, Schroeder T,et al. Allogeneic hematopoietic cell transplantation for older patients with AML with active disease. A study from the Acute Leukemia Working Party of the European Society for Blood and Marrow Transplantation (EBMT). Bone Marrow Transplant. https://doi.org/10.1038/s41409-024-02275-6 2024.
Passweg JR, Baldomero H, Chabannon C, Basak GW, de la Cámara R, Corbacioglu S, et al. Hematopoietic cell transplantation and cellular therapy survey of the EBMT: monitoring of activities and trends over 30 years. Bone Marrow Transpl. 2021;56:1651–64.
Bittencourt MC, Ciurea SO. Recent advances in allogeneic hematopoietic stem cell transplantation for acute myeloid leukemia. Biol Blood Marrow Transpl. 2020;26:e215–221.
Schlenk RF, et al. HLA-identical sibling allogeneic transplants versus chemotherapy in acute myelogenous leukemia with t(8;21) in first complete remission: collaborative study between the German AML Intergroup and CIBMTR. Biol Blood Marrow Transpl. 2008;14:187–96.
Penack O, Marchetti M, Aljurf M, Arat M, Bonifazi F, Duarte RF, et al. Prophylaxis and management of graft versus host disease after stem-cell transplantation for hematological malignancies: updated consensus recommendations of the European Society for Blood and Marrow Transplantation. Lancet Haematol. 2024;11:e147–159.
Kröger N, Solano C, Wolschke C, Bandini G, Patriarca F, Pini M, et al. Anti -lymphocyte globulin for prevention of chronic graft-versus-host disease. N. Engl J Med. 2016;374:43–53.
Bolaños-Meade J, Hamadani M, Wu J, Al Malki MM, Martens MJ, Runaas L, et al. Post-transplantation cyclophosphamide-based graft-versus-host disease prophylaxis. N Engl J Med. 2023;388:2338–48.
Gorin NC, Labopin M, Frassoni F, Milpied N, Attal M, Blaise D, et al. Identical outcome after autologous or allogeneic genoidentical hematopoietic stem-cell transplantation in first remission of acute myelocytic leukemia carrying inversion 16 or t(8;21): a retrospective study from the European Cooperative Group for Blood and Marrow Transplantation. J Clin Oncol. 2008;26:3183–8.
Delaunay J, Vey N, Leblanc T, Fenaux P, Rigal-Huguet F, Witz F, et al. Prognosis of inv (16)/t (16;16) acute myeloid leukemia (AML): a survey of 110 cases from the French AML Intergroup. Blood. 2003;102:462–9.
Schetelig J, de Wreede LC, van Gelder M, Koster L, Finke J, Niederwieser D, et al. Late treatment-related mortality versus competing causes of death after allogeneic transplantation for myelodysplastic syndromes and secondary acute myeloid leukemia. Leukemia. 2019;33:686–95.
Moukalled N, Labopin M, Versluis J, Socié G, Blaise D, Salmenniemi U, et al. Complex karyotype but no other cytogenetic abnormalities is associated with worse posttransplant survival of patients with nucleophosmin 1-mutated acute myeloid leukemia: A study from the European Society for Blood and Marrow Transplantation Acute Leukemia Working Party. Am J Hematol. 2024;99:360–9.
Aldoss I, Nakamura R, Yang D, Salhotra A, Stein AS, Pullarkat V, et al. Favorable outcomes for allogeneic hematopoietic cell transplantation in elderly patients with NPM1-mutated and FLT3-ITD-negative acute myeloid leukemia. Bone Marrow Transpl. 2020;55:473–5.
Shimoni A, Labopin M, Angelucci E, Blaise D, Ciceri F, Koc Y, et al. The association of graft-versus-leukemia effect and graft-versus-host disease in haploidentical transplantation with post-transplant cyclophosphamide for AML. Bone Marrow Transpl. 2022;57:384–90.
Leotta S, Condorelli A, Sciortino R, Milone GA, Bellofiore C, Garibaldi B et al. Prevention and treatment of acute myeloid leukemia relapse after hematopoietic stem cell transplantation: the state of the art and future perspectives. J Clin Med. 2022 4;11253.
Lee CJ, Savani BN, Mohty M, Gorin NC, Labopin M, Ruggeri A, et al. Post-remission strategies for the prevention of relapse following allogeneic hematopoietic cell transplantation for high-risk acute myeloid leukemia: expert review from the Acute Leukemia Working Party of the European Society for Blood and Marrow Transplantation. Bone Marrow Transpl. 2019;54:519–30.
Boddu P, Kantarjian H. Core binding factor acute myeloid leukemia-2021 treatment algorithm. Blood CA J. 2021;11:14.
Darwish C, Farina K, Tremblay D. The core concepts of core binding factor acute myeloid leukemia: Current considerations for prognosis and treatment. Blood Rev. 2023;62:101117.
Faber ZJ, Chen X, Gedman AL, Boggs K, Cheng J, Ma J, et al. The genomic landscape of core-binding factor acute myeloid leukemias. Nat Genet. 2016;48:1551–6.
Nagler A, Labopin M, Mielke S, Passweg J, Blaise D, Gedde-Dahl T, et al. Matched related versus unrelated versus haploidentical donors for allogeneic transplantation in AML patients achieving first complete remission after two induction courses: a study from the ALWP/EBMT. Bone Marrow Transpl. 2023;58:791–800.
Gorin NC, Labopin M, Blaise D, de Groot M, Socié G, Bourhis JH, et al. Stem cell transplantation from a haploidentical donor versus a genoidentical sister for adult male patients with acute myelogenous leukemia in first remission: a retrospective study from the acute leukemia working party of the European Society for Blood and Marrow Transplantation. Cancer. 2020;126:1004–15.
Nagler A, Labopin M, Dholaria B, Angelucci E, Afanasyev B, Cornelissen JJ, et al. Comparison of haploidentical bone marrow versus matched unrelated donor peripheral blood stem cell transplantation with posttransplant cyclophosphamide in patients with acute leukemia. Clin Cancer Res. 2021;27:843–51.
Nagler A, Labopin M, Swoboda R, Schroeder T, Hamladji RM, Griskevicius L et al. Post-transplant cyclophosphamide, calcineurin inhibitor, and mycophenolate mofetil compared to anti-thymocyte globulin, calcineurin inhibitor, and methotrexate combinations as graft-versus-host disease prophylaxis post allogeneic stem cell transplantation from sibling and unrelated donors in patients with acute myeloid leukemia: A study on behalf of the Acute Leukemia Working Party of the European Society for Blood and Marrow Transplantation. Bone Marrow Transpl. https://doi.org/10.1038/s41409-024-02284-5 2024.
Greinix HT, Eikema DJ, Koster L, Penack O, Yakoub-Agha I, Montoto S, et al. Improved outcome of patients with graft-versus-host disease after allogeneic hematopoietic cell transplantation for hematologic malignancies over time: an EBMT mega-file study. Haematologica. 2022;107:1054–63.
Ishikawa Y. Molecular pathogenesis and treatment of core binding factor-acute myeloid leukemia. Rinsho Ketsuek 2018;59:1997–2006.
Kawashima N, Akashi A, Nagata Y, Kihara R, Ishikawa Y, Asou N, et al. Clinical significance of ASXL2 and ZBTB7A mutations and C-terminally truncated RUNX1-RUNX1T1 expression in AML patients with t(8;21) enrolled in the JALSG AML201 study. Ann Hematol. 2019;98:83–91.
Bourne G, Diebold K, Espinoza-Gutarra M, Al-Kadhimi Z, Bachiashvili K, Rangaraju S, et al. Addition of single dose gemtuzumab ozogamicin to intensive induction chemotherapy in core-binding factor acute myeloid leukemia. Leuk Res 2024;139:107467.
Ragon BK, Daver N, Garcia-Manero G, Ravandi F, Cortes J, Kadia T, et al. Minimal residual disease eradication with epigenetic therapy in core binding factor acute myeloid leukemia. Am J Hematol. 2017;92:845–50.
Senapati J, Shoukier M, Garcia-Manero G, Wang X, Patel K, Kadia T, et al. Activity of decitabine as maintenance therapy in core binding factorable acute myeloid leukemia. Am J Hematol. 2022;97:574–82.
DiNardo CD, Jonas BA, Pullarkat V, Thirman MJ, Garcia JS, Wei AH, et al. Azacitidine and venetoclax in previously untreated acute myeloid leukemia. N Engl J Med. 2020;383:617–29.
Paschka P, Schlenk RF, Weber D, Benner A, Bullinger L, Heuser M, et al. Adding dasatinib to intensive treatment in core-binding factor acute myeloid leukemia-results of the AMLSG 11-08 trial. Leukemia 2018;32:1621–30.
Erba HP, Montesinos P, Kim HJ, Patkowska E, Vrhovac R, Žák P, et al. Quizartinib plus chemotherapy in newly diagnosed patients with FLT3-internal-tandem-duplication-positive acute myeloid leukaemia (QuANTUM-First): a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet. 2023;401:1571–83.
Kadia TM, Ravandi F, Molica M, Bataller A, Borthakur G, Daver N, et al. Phase II study of cladribine, idarubicin, and ara-C (CLIA) with or without sorafenib as initial therapy for patients with acute myeloid leukemia. Am J Hematol. 2023;98:1711–20.
Levis MJ, Hamadani M, Logan B, Jones RJ, Singh AK, Litzow M, et al. Gilteritinib as post-transplant maintenance for acute myeloid leukemia with internal tandem duplication mutation of FLT3. J Clin Oncol. 2024;42:1766–75.
Acknowledgements
We thank all of the EBMT centers and national registries for contributing patients to this study (Supplementary Appendix material). We also thank the data managers for their excellent work and the patients who have contributed data.
Author information
Authors and Affiliations
Contributions
AN wrote the manuscript, designed the study, and interpreted the data. ML and MM designed the study, performed the statistical analyses, interpreted the data, and edited the manuscript US, DW, DB, AR, PR, EF, RPdL, PC, PvdB, DB, CS, JM, NK, GB, MA, JV, KH, and FC reviewed the manuscript and provided clinical data. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
The scientific boards of the ALWP of the EBMT approved this study. The study was performed in accordance with the Declaration of Helsinki and approved by the Sheba Medical Center Helsinki committee (SMC-770920). Informed consent was obtained from all subjects.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Data presented in part at ASH 2023 (publication number 3525).
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nagler, A., Labopin, M., Salmenniemi, U. et al. Trends in allogeneic transplantation for favorable risk acute myeloid leukemia in first remission: a longitudinal study of >15 years from the ALWP of the EBMT. Bone Marrow Transplant 59, 1563–1576 (2024). https://doi.org/10.1038/s41409-024-02379-z
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41409-024-02379-z