Abstract
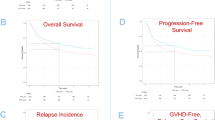
The EBMT recommends rabbit anti-thymocyte or anti-T-lymphocyte globulin (rATG/ATLG) as GVHD prophylaxis in matched sibling donor (MSD) allogeneic hematopoietic cell transplantation (allo-HCT). However, discrepancies between recommendations and clinical practice were reflected in the EBMT survey. Therefore, we performed retrospective EBMT registry analysis from 2014 to 2021 to reinforce the real-world evidence context of rATG/ATLG impact on post-transplantation outcomes. This study included 11,420 adult patients (non-ATG n = 7680 and ATG n = 3740) with hematological malignancies after the first allo-HCT from peripheral blood. Use of ATG was associated with a reduced risk of aGVHD II-IV (Day +100: non-ATG vs ATG, 27.6% vs. 21.6%; adjusted HR 0.7, p < 0.001) and cGVHD (2-year: non-ATG vs ATG, 48.9% vs 30%; adjusted HR 0.45, p < 0.001), improved OS (2-year: 62.9% vs 63.3%; adjusted HR 0.89, p = 0.009), reduced NRM (2-year: 16% vs 12.5%; adjusted HR 0.63, p < 0.001), and higher GRFS (2-year: 32.2% vs 40.7%; adjusted HR 0.72, p < 0.001). While RI was higher in the ATG group (2-year: non-ATG vs ATG, 30.2% vs 34.7%; adjusted HR 1.22, p < 0.001) it did not translate into a significantly lower PFS (2-year: 53.9% vs 52.8%; adjusted HR not significant). Overall, outcomes were favorable for the intermediate rATG/ATLG dose ranges compared to the low and high dose ranges. Administration of rATG/ATLG improved outcomes in MSD allo-HCT recipients, supporting the EBMT recommendation for its use.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Bacigalupo A, Lamparelli T, Bruzzi P, Guidi S, Alessandrino PE, di Bartolomeo P, et al. Antithymocyte globulin for graft-versus-host disease prophylaxis in transplants from unrelated donors: 2 randomized studies from Gruppo Italiano Trapianti Midollo Osseo (GITMO). Blood. 2001;98:2942–7.
Finke J, Bethge WA, Schmoor C, Ottinger HD, Stelljes M, Zander AR, et al. Standard graft-versus-host disease prophylaxis with or without anti-T-cell globulin in haematopoietic cell transplantation from matched unrelated donors: a randomised, open-label, multicentre phase 3 trial. Lancet Oncol. 2009;10:855–64.
Crocchiolo R, Esterni B, Castagna L, Furst S, El-Cheikh J, Devillier R, et al. Two days of antithymocyte globulin are associated with a reduced incidence of acute and chronic graft-versus-host disease in reduced-intensity conditioning transplantation for hematologic diseases. Cancer. 2013;119:986–92.
Deeg HJ, Storer BE, Boeckh M, Martin PJ, McCune JS, Myerson D, et al. Reduced incidence of acute and chronic graft-versus-host disease with the addition of thymoglobulin to a targeted busulfan/cyclophosphamide regimen. Biol Blood Marrow Transpl. 2006;12:573–84.
Devillier R, Crocchiolo R, Castagna L, Furst S, El Cheikh J, Faucher C, et al. The increase from 2.5 to 5 mg/kg of rabbit anti-thymocyte-globulin dose in reduced intensity conditioning reduces acute and chronic GVHD for patients with myeloid malignancies undergoing allo-SCT. Bone Marrow Transpl. 2012;47:639–45.
Dulery R, Mohty M, Duhamel A, Robin M, Beguin Y, Michallet M, et al. Antithymocyte globulin before allogeneic stem cell transplantation for progressive myelodysplastic syndrome: a study from the French Society of Bone Marrow Transplantation and Cellular Therapy. Biol Blood Marrow Transpl. 2014;20:646–54.
Kroger N, Solano C, Bonifazi F. Antilymphocyte globulin for chronic graft-versus-host disease. N Engl J Med. 2016;374:1894–5.
Walker I, Panzarella T, Couban S, Couture F, Devins G, Elemary M, et al. Pretreatment with anti-thymocyte globulin versus no anti-thymocyte globulin in patients with haematological malignancies undergoing haemopoietic cell transplantation from unrelated donors: a randomised, controlled, open-label, phase 3, multicentre trial. Lancet Oncol. 2016;17:164–73.
Baron F, Mohty M, Blaise D, Socie G, Labopin M, Esteve J, et al. Anti-thymocyte globulin as graft-versus-host disease prevention in the setting of allogeneic peripheral blood stem cell transplantation: a review from the Acute Leukemia Working Party of the European Society for Blood and Marrow Transplantation. Haematologica. 2017;102:224–34.
Penack O, Marchetti M, Ruutu T, Aljurf M, Bacigalupo A, Bonifazi F, et al. Prophylaxis and management of graft versus host disease after stem-cell transplantation for haematological malignancies: updated consensus recommendations of the European Society for Blood and Marrow Transplantation. Lancet Haematol. 2020;7:e157–e67.
Penack O, Marchetti M, Aljurf M, Arat M, Bonifazi F, Duarte RF, et al. Prophylaxis and management of graft-versus-host disease after stem-cell transplantation for haematological malignancies: updated consensus recommendations of the European Society for Blood and Marrow Transplantation. Lancet Haematol. 2024;11:e147–e59.
Piekarska A, Czyz A, Peczynski C, Ambron P, Polge E, Moiseev I, et al. ATG or no ATG? - survey of clinical practice in EBMT centers on behalf of the Transplant Complications Working Party of EBMT. Bone Marrow Transpl. 2023;58:337–9.
Shichijo T, Fuji S, Nagler A, Bazarbachi A, Mohty M, Savani BN. Personalizing rabbit anti-thymocyte globulin therapy for prevention of graft-versus-host disease after allogeneic hematopoietic cell transplantation: is there an optimal dose? Bone Marrow Transpl. 2020;55:505–22.
Chang YJ, Wu DP, Lai YR, Liu QF, Sun YQ, Hu J, et al. Antithymocyte globulin for matched sibling donor transplantation in patients with hematologic malignancies: a multicenter, open-label, randomized controlled study. J Clin Oncol. 2020;38:3367–76.
Bonifazi F, Solano C, Wolschke C, Sessa M, Patriarca F, Zallio F, et al. Acute GVHD prophylaxis plus ATLG after myeloablative allogeneic haemopoietic peripheral blood stem-cell transplantation from HLA-identical siblings in patients with acute myeloid leukaemia in remission: final results of quality of life and long-term outcome analysis of a phase 3 randomised study. Lancet Haematol. 2019;6:e89–e99.
Wolschke C, Zabelina T, Ayuk F, Alchalby H, Berger J, Klyuchnikov E, et al. Effective prevention of GVHD using in vivo T-cell depletion with anti-lymphocyte globulin in HLA-identical or -mismatched sibling peripheral blood stem cell transplantation. Bone Marrow Transpl. 2014;49:126–30.
Bonifazi F, Bandini G, Arpinati M, Tolomelli G, Stanzani M, Motta MR, et al. Intensification of GVHD prophylaxis with low-dose ATG-F before allogeneic PBSC transplantation from HLA-identical siblings in adult patients with hematological malignancies: results from a retrospective analysis. Bone Marrow Transpl. 2012;47:1105–11.
Kumar A, Reljic T, Hamadani M, Mohty M, Kharfan-Dabaja MA. Antithymocyte globulin for graft-versus-host disease prophylaxis: an updated systematic review and meta-analysis. Bone Marrow Transpl. 2019;54:1094–106.
Baron F, Labopin M, Blaise D, Lopez-Corral L, Vigouroux S, Craddock C, et al. Impact of in vivo T-cell depletion on outcome of AML patients in first CR given peripheral blood stem cells and reduced-intensity conditioning allo-SCT from a HLA-identical sibling donor: a report from the Acute Leukemia Working Party of the European Group for Blood and Marrow Transplantation. Bone Marrow Transpl. 2014;49:389–96.
Soiffer RJ, Lerademacher J, Ho V, Kan F, Artz A, Champlin RE, et al. Impact of immune modulation with anti-T-cell antibodies on the outcome of reduced-intensity allogeneic hematopoietic stem cell transplantation for hematologic malignancies. Blood. 2011;117:6963–70.
Shimony O, Nagler A, Gellman YN, Refaeli E, Rosenblum N, Eshkar-Sebban L, et al. Anti-T lymphocyte globulin (ATG) induces generation of regulatory T cells, at least part of them express activated CD44. J Clin Immunol. 2012;32:173–88.
Beider K, Naor D, Voevoda V, Ostrovsky O, Bitner H, Rosenberg E, et al. Dissecting the mechanisms involved in anti-human T-lymphocyte immunoglobulin (ATG)-induced tolerance in the setting of allogeneic stem cell transplantation - potential implications for graft versus host disease. Oncotarget. 2017;8:90748–65.
Feng X, Kajigaya S, Solomou EE, Keyvanfar K, Xu X, Raghavachari N, et al. Rabbit ATG but not horse ATG promotes expansion of functional CD4+CD25highFOXP3+ regulatory T cells in vitro. Blood. 2008;111:3675–83.
Bonifazi F, Rubio MT, Bacigalupo A, Boelens JJ, Finke J, Greinix H, et al. Rabbit ATG/ATLG in preventing graft-versus-host disease after allogeneic stem cell transplantation: consensus-based recommendations by an international expert panel. Bone Marrow Transpl. 2020;55:1093–102.
Battipaglia G, Labopin M, Kroger N, Vitek A, Afanasyev B, Hilgendorf I, et al. Posttransplant cyclophosphamide vs antithymocyte globulin in HLA-mismatched unrelated donor transplantation. Blood. 2019;134:892–9.
Bolanos-Meade J, Hamadani M, Wu J, Al Malki MM, Martens MJ, Runaas L, et al. Post-transplantation cyclophosphamide-based graft-versus-host disease prophylaxis. N Engl J Med. 2023;388:2338–48.
Desai N, Altareb M, Remberger M, Chen C, Alfaro Moya T, Al-Shaibani E, et al. PTCy-based graft-versus-host disease prophylaxis for matched sibling donor allogeneic hematopoietic cell transplantation. Blood Adv. 2025;9:660–9.
Battipaglia G, Labopin M, Blaise D, Diez-Martin JL, Bazarbachi A, Vitek A, et al. Impact of the addition of antithymocyte globulin to post-transplantation cyclophosphamide in haploidentical transplantation with peripheral blood compared to post-transplantation cyclophosphamide alone in acute myelogenous leukemia: a retrospective study on behalf of the acute leukemia working party of the European Society for Blood and Marrow Transplantation. Transpl Cell Ther. 2022;28:587 e1–e7.
Waller EK, Langston AA, Lonial S, Cherry J, Somani J, Allen AJ, et al. Pharmacokinetics and pharmacodynamics of anti-thymocyte globulin in recipients of partially HLA-matched blood hematopoietic progenitor cell transplantation. Biol Blood Marrow Transpl. 2003;9:460–71.
Chawla S, Dharmani-Khan P, Liu Y, Prokopishyn N, Amlish Munir M, Griffiths C, et al. High serum level of antithymocyte globulin immediately before graft infusion is associated with a low likelihood of chronic, but not acute, graft-versus-host disease. Biol Blood Marrow Transpl. 2014;20:1156–62.
Remberger M, Ringden O, Hagglund H, Svahn BM, Ljungman P, Uhlin M, et al. A high antithymocyte globulin dose increases the risk of relapse after reduced intensity conditioning HSCT with unrelated donors. Clin Transpl. 2013;27:E368–74.
Remberger M, Sundberg B. Low serum levels of total rabbit-IgG is associated with acute graft-versus-host disease after unrelated donor hematopoietic stem cell transplantation: results from a prospective study. Biol Blood Marrow Transpl. 2009;15:996–9.
Jamani K, Dabas R, Kangarloo SB, Prokopishyn NL, Luider J, Dharmani-Khan P, et al. Rabbit antithymocyte globulin serum levels: factors impacting the levels and clinical outcomes impacted by the levels. Biol Blood Marrow Transpl. 2019;25:639–47.
Baron F, Labopin M, Niederwieser D, Vigouroux S, Cornelissen JJ, Malm C, et al. Impact of graft-versus-host disease after reduced-intensity conditioning allogeneic stem cell transplantation for acute myeloid leukemia: a report from the Acute Leukemia Working Party of the European group for blood and marrow transplantation. Leukemia. 2012;26:2462–8.
Baron F, Maris MB, Sandmaier BM, Storer BE, Sorror M, Diaconescu R, et al. Graft-versus-tumor effects after allogeneic hematopoietic cell transplantation with nonmyeloablative conditioning. J Clin Oncol. 2005;23:1993–2003.
Gill S, Porter DL. Reduced-intensity hematopoietic stem cell transplants for malignancies: harnessing the graft-versus-tumor effect. Annu Rev Med. 2013;64:101–17.
Mohty M, Bay JO, Faucher C, Choufi B, Bilger K, Tournilhac O, et al. Graft-versus-host disease following allogeneic transplantation from HLA-identical sibling with antithymocyte globulin-based reduced-intensity preparative regimen. Blood. 2003;102:470–6.
Author information
Authors and Affiliations
Contributions
AP: concept and design of a study, interpretation of the results, reference search, writing a manuscript, preparing tables and figures; MA: Registry data preparation, statistical analysis, preparing tables and figures, drafting and critical revision of the manuscript; WB: Registry data preparation, statistical analysis, drafting and critical revision of the manuscript; ChP: Registry data preparation, statistical analysis, drafting and critical revision of the manuscript; JMZ: concept of a study, interpretation of the results, drafting and critical revision of the manuscript; NK: drafting and critical revision of the manuscript; RZ: critical revision of the manuscript; FC: drafting and critical revision of the manuscript; TS: critical revision of the manuscript; TL: critical revision of the manuscript; JP: critical revision of the manuscript; DK: critical revision of the manuscript; MS: critical revision of the manuscript; IWB: critical revision of the manuscript; UP: critical revision of the manuscript; IJ-A: critical revision of the manuscript; DB: critical revision of the manuscript; AMR: critical revision of the manuscript; JT: critical revision of the manuscript; EMW-D: critical revision of the manuscript; JW: critical revision of the manuscript; ChS: critical revision of the manuscript; GGW: critical revision of the manuscript; ME: critical revision of the manuscript; JM: critical revision of the manuscript; FS: critical revision of the manuscript; JV: critical revision of the manuscript; PZ: critical revision of the manuscript; IM: drafting and critical revision of the manuscript; HS: drafting and critical revision of the manuscript; OP: drafting and critical revision of the manuscript; ZP: drafting and critical revision of the manuscript. All authors approved the final version.
Corresponding author
Ethics declarations
Competing interests
Nothing to declare for this topic, except potential relatedness to HCT/GVHD topics: AP has received honoraria or travel support from Alexion, AstraZeneca, Astellas, Gilead, MSD, Novartis, Pierre Fabre, Pfizer, Sanofi, and the EBMT (European Society for Blood and Marrow transplantation) which not directly related to this work. NK received honorarium from Mallinckrodt, Novartis, Kit/Gilead, BMS, Takeda, Medac, Neovii, Sanofi IYA: received honoraria from Gilead/Kite, BMS, Novartis and AstraZeneca. EMW-D reports personal fees from Novartis, Takeda, Janssen, Incyte, MEDAC. FS has received travel support from Janssen and Medac, honoraria from Medac, GWT, Abbvie, Servier and Pierre Fabre and research funding from Medac and Servier. HS reports having received personal fees from Incyte, Janssen, Novartis, Sanofi and from the Belgian Hematological Society (BHS), as well as research grants from Novartis and the BHS, all paid to her institution and not directly related to this work. She has also received non-financial support (travel grants) from Gilead, Pfizer, EBMT and the CIBMTR (Center for International Bone Marrow Transplantation Research). OP has received honoraria or travel support from Gilead, Jazz, MSD, Neovii, Novartis, Pfizer and Therakos. He has received research support from Incyte and Priothera. He is member of advisory boards to Equillium Bio, Jazz, Gilead, Novartis, MSD, Omeros, Priothera, Sanofi, Shionogi and SOBI. RZ reports having received personal fees from Incyte, MNK, Novartis, Sanofi, Medac and Neovii.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Piekarska, A., Abouqateb, M., Boreland, W. et al. Improved GVHD-free relapse-free survival when rATG/ATLG is used in allo-HCT from matched sibling donors - an EBMT registry study by the Transplant Complications Working Party. Bone Marrow Transplant 60, 1574–1583 (2025). https://doi.org/10.1038/s41409-025-02692-1
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41409-025-02692-1