Abstract
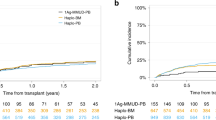
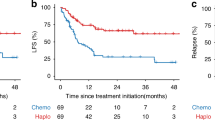
Haploidentical hematopoietic stem cell transplant (Haplo-HSCT) has emerged as an alternative for patients lacking matched human leukocyte antigen (HLA) donors. The scarcity of stem cell donor registries and cord banks across the Eastern Mediterranean (EM) region has led to increased need of Haplo-HSCT as a mean to overcome this limitation. In this study, we aimed to assess trends in Haplo-HSCT utilization within the Eastern Mediterranean Blood and Marrow Transplantation (EMBMT) registry from 2012 to 2024, and describe key clinical and transplant-related factors associated with patient outcomes. We conducted a retrospective, multicenter registry-based analysis of patients who had their first un-manipulated Haplo-HSCT in ten EMBMT centers across six countries, who responded and accepted to participate in the study. Due to the variability in time-to-event reporting across different centers, survival and relapse-related outcomes were analyzed descriptively. Continuous variables were summarized using medians and ranges, and categorical variables were described by counts and percentages. The association between individual baseline variables and patient survival, was conducted using a univariate analysis utilizing the chi-square test. Categorical variables such as patient and transplant characteristics were compared against survival status at last follow-up. All variables were further evaluated in the multivariate analysis. Overall survival (OS) and progression-free survival (PFS) were estimated using Kaplan-Meier survival analysis. Between 2012 and 2024, a total of 673 patients received haplo-HSCT across ten centers, in six EMBMT-registered countries. Median age was 25 years, and the predominant indication for haplo-HSCT was leukemia (64.3%). Transplant was done using stem cells collected from peripheral blood in majority of cases (65.7%), and Total Body Irradiation (TBI) was utilized in 37.6% of all patient. 76.5% had malignant hematological disorders, while 23.5% had non-malignant disorders. Relapse was reported in 232 patients (34.5%) and death in 220 patients (32.7%). Of these, 88 deaths (12.8%) were attributed to disease progression. Haplo-HSCT activity increased steadily over the study period, with a marked increase in the last few years, reflecting broader regional adoption. PFS was 66% and 60% at 1- and 2- years after transplantation. Also, the 1-year and 2-year post-transplant OS was 71% and 65%, respectively. Multivariate analysis identified disease type and chronic GVHD as factors associated with improved outcomes. Despite variability across centers, outcomes were consistent with international benchmarks, underscoring the growing feasibility and therapeutic value of haplo-HSCT in the EMRO region. Haplo-HSCT is increasingly adopted across the EMRO region as the primary alternative donor HSCT modality. Our findings confirm its clinical efficacy, with outcomes comparable to international benchmarks. These results underscore the importance of continued regional collaboration and the development of personalized strategies to address challenges such as graft-versus-host disease (GVHD), disease relapse, and disparities in access to transplantation services.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The datasets generated and analyzed in this study are available from the corresponding author on reasonable request.
References
Chen J, Wang H, Zhou J, Feng S. Advances in the understanding of poor graft function following allogeneic hematopoietic stem-cell transplantation. Therapeut Adv Hematol. 2020;11:2040620720948743.
Huang X-J. Overcoming graft failure after haploidentical transplantation: Is this a possibility? Best Pract Res Clin Haematol. 2021;34:101255.
Wachsmuth LP, Patterson MT, Eckhaus MA, Venzon DJ, Gress RE, Kanakry CG. Post-transplantation cyclophosphamide prevents graft-versus-host disease by inducing alloreactive T cell dysfunction and suppression. J Clin Invest. 2019;129:2357–2373.
Shabbir-Moosajee M, Lombardi L, Ciurea SO. An overview of conditioning regimens for haploidentical stem cell transplantation with post-transplantation cyclophosphamide. Am J Hematol. 2015;90:541–48.
Muhsen IN, Neiderwieser D, Garderet L, Penack O, Greinix HT, Fakih RE, et al. Patterns of Graft-Versus-Host Disease (GvHD) Prevention Practices in the Eastern Mediterranean (EM) Region: A Worldwide Network for Blood & Marrow Transplantation (WBMT) Global Study. Hematol Oncol Stem Cell Ther. 2025;18:100–7.
Aljurf M, Zaidi SZ, Solh HE, Hussain F, Ghavamzadeh A, Mahmoud HK, et al. Special issues related to hematopoietic SCT in the Eastern Mediterranean region and the first regional activity report. Bone Marrow Transpl. 2009;43:1–12.
Ahmed SO, Ghavamzadeh A, Zaidi SZ, Baldomero H, Pasquini MC, Hussain F, et al. Trends of hematopoietic stem cell transplantation in the Eastern Mediterranean region, 1984-2007. Biol Blood Marrow Transpl. 2011;17:1352–61.
Ahmed SO, Fakih RE, Elhaddad A, Hamidieh AA, Altbakhi A, Chaudhry QN, et al. Strategic priorities for hematopoietic stem cell transplantation in the EMRO region. Hematol Oncol Stem Cell Ther. 2023;16:162–69.
Aljurf M, Nassar A, Hamidieh AA, Elhaddad A, Hamladji R, Bazarbachi A, et al. Hematopoietic stem cell transplantation in the Eastern Mediterranean Region (EMRO) 2011–2012: A comprehensive report on behalf of the Eastern Mediterranean Blood and Marrow Transplantation group (EMBMT). Hematol/Oncol Stem Cell Ther. 2015;8:167–75.
Parvanova, I. and J. Finkelstein, Disparities in racial and ethnic representation in stem cell clinical trials, in The Importance of Health Informatics in Public Health during a Pandemic. 2020, IOS Press. p. 358-61
Armand P, Kim HT, Logan BR, Wang Z, Alyea EP, Kalaycio ME, et al. Validation and refinement of the Disease Risk Index for allogeneic stem cell transplantation. Blood. 2014;123:3664–71.
Robinson TM, O’Donner PV, Fuchs EJ, Luznik L. Haploidentical bone marrow and stem cell transplantation: experience with post-transplantation cyclophosphamide. Semin Hematol. 2016;53:90–7.
Bacigalupo A, Ballen K, Rizzo D, Giralt S, Lazarus H, Ho V, et al. Defining the intensity of conditioning regimens: working definitions. Biol Blood Marrow Transpl. 2009;15:1628–33.
Hatzimichael E, Tuthill M. Hematopoietic stem cell transplantation. Stem Cells Cloning. 2010;3:105–17.
Lee SJ, Williams KM, Sarantopoulos S, Kitko CL, Cutler C, Pidala J, et al. NIH Chronic Graft-Versus-Host Disease Consensus Conference 2025 Update. Transpl Cell Ther. 2025;31:678 e1–678 e16.
El-Cheikh J, Bidaoui G, Sharrouf L, Zahreddine A, Massoud R, Nehme R, et al. Haploidentical stem cell transplantation with post-transplant cyclophosphamide: challenges and outcomes from a tertiary care center in Lebanon. Front Transpl. 2023;2:1149393.
Luo Y, Tan Y, Hu Y, Shi J, Zheng G, Zheng W, et al. Clinical Outcomes of Haploidentical Donor Compared with Unrelated and HLA-Matched Related Donor Hematopoietic Stem Cell Transplantation for Hematologic Malignancies. Blood. 2012;120:4159.
Kako S, Gomyo A, Akahoshi Y, Harada N, Kameda K, Ugai T, et al. Haploidentical transplantation using low-dose alemtuzumab: Comparison with haploidentical transplantation using low-dose thymoglobulin. Eur J Haematol. 2019;102:256–64.
Giebel S, Boumedil A, Labopin M, Seesaghur A, Baron F, Ciceri F, et al. Trends in the use of hematopoietic stem cell transplantation for adults with acute lymphoblastic leukemia in Europe: a report from the Acute Leukemia Working Party of the European Society for Blood and Marrow Transplantation (EBMT). Ann Hematol. 2019;98:2389–98.
Al Malki MM, Tsai N, Palmer J, Mokhtari S, Tsai W, Cao T, et al. Posttransplant cyclophosphamide as GVHD prophylaxis for peripheral blood stem cell HLA-mismatched unrelated donor transplant. Blood Adv. 2021;5:2650–59.
Battipaglia G, Galimard J, Labopin M, Raiola AM, Blaise D, Ruggeri A, et al. Post-transplant cyclophosphamide in one-antigen mismatched unrelated donor transplantation versus haploidentical transplantation in acute myeloid leukemia: a study from the Acute Leukemia Working Party of the EBMT. Bone Marrow Transpl. 2022;57:562–71.
Shimoni A, Peczynski C, Labopin M, Kulagin A, Meijer E, Cornelissen J, et al. Post-transplant cyclophosphamide separates graft-versus host disease and graft versus leukemia effects after HLA-matched stem-cell transplantation for acute myeloid leukemia. Leukemia. 2025;39:222–8.
Luznik L, Fuchs EJ. High-dose, post-transplantation cyclophosphamide to promote graft-host tolerance after allogeneic hematopoietic stem cell transplantation. Immunol Res. 2010;47:65–77.
Ruggeri L, Mancusi A, Burchielle E, Aversa F, Martelli M, Velardi A, et al. Natural killer cell alloreactivity in allogeneic hematopoietic transplantation. Curr Opin Oncol. 2007;19:142–147.
Fowler DH, Gress RE. Th2 and Tc2 cells in the regulation of GVHD, GVL, and graft rejection: considerations for the allogeneic transplantation therapy of leukemia and lymphoma. Leuk Lymphoma. 2000;38:221–34.
Mohty M, Fegeux N, Exbrayat C, Lu ZY, Legouffe E, Quittlet P, et al. Reduced intensity conditioning: enhanced graft-versus-tumor effect following dose-reduced conditioning and allogeneic transplantation for refractory lymphoid malignancies after high-dose therapy. Bone Marrow Transpl. 2001;28:335–9.
El Cheikh J, Bidaoui G, Sharrouf L, Zahreddine A, Massoud R, Nehme R, et al. Haploidentical stem cell transplantation with post-transplant cyclophosphamide challenges and outcome from a tertiary care center in Lebanon. Front Transpl. 2023;2:1149393.
Amouzegar A, Dey BR, Spitzer TR. Peripheral blood or bone marrow stem cells? Practical considerations in hematopoietic stem cell transplantation. Transfus Med Rev. 2019;33:43–50.
El Cheikh J, Bidaoui G, Atoui A, Khodr T, Sharrouf L, Zahreddine A, et al. Clofarabine and total body irradiation (TBI) as conditioning regimen for allogeneic stem cell transplantation in high-risk acute leukemia patients: a two-center retrospective cohort study. Bone Marrow Transpl. 2023;58:667–72.
George B, Kulkarni U, Lionel S, Devasia A, Aboobacker F, Lakshmi K, et al. Haploidentical transplantation is feasible and associated with reasonable outcomes despite major infective complications-A single center experience from India. Transpl Cell Ther. 2022;28:45 e1–45 e8.
Author information
Authors and Affiliations
Contributions
JEC and MA conceived and designed the study. AT performed data collection and registry coordination. JEC, IM, RR, HH, AH, MAY, KB, RY, MG, MA, AI, MM, SA, TG, REF, and MA contributed to patient data and clinical interpretation. AT contributed to data analysis and drafted the manuscript. All authors critically revised the manuscript and approved the final version.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
This study was conducted in accordance with the principles of the Declaration of Helsinki and all relevant institutional and national guidelines and regulations. Ethical approval for this study was obtained from the Institutional Review Board of American University of Beirut (BIO-2022-0246) and all other participating centers. The requirement for informed consent was waived by the Institutional Review Board due to the retrospective nature of the study.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
El Cheikh, J., Tarhini, A., Bazarbachi, A. et al. Twelve-year utilization and outcomes of haploidentical hematopoietic stem cell transplantation (HSCT) in the Eastern Mediterranean (EM) region: A multicenter EMBMT registry analysis. Bone Marrow Transplant (2026). https://doi.org/10.1038/s41409-026-02849-6
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41409-026-02849-6