Abstract
Introduction Poor oral health and barriers to accessing dental services are common among people experiencing social exclusion. This population experience a disproportionate and inequitable burden of oral disease. A small number of dental services have published models of care that target this population, but no national surveys have been conducted.
Aims This study aims to identify what types of services are providing dental and oral healthcare for people experiencing social exclusion in England and the models of delivery adopted by these services.
Methods A snowballing sampling strategy was used to identify services that provide targeted for adults experiencing social exclusion. The study used a survey to collect data about the location, service models and barriers and enablers of these services.
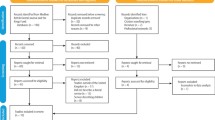
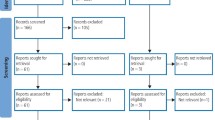
Results In total, 74 responses from different services met the inclusion criteria for the study. Seventy one were included in the mapping exercise and 53 provided free-text comments that contributed to an understanding of barriers and enablers of services.
Discussion Most services operated to meet the needs of the mainstream population and described inflexibilities in their service design models as barriers to providing care for socially excluded groups.
Conclusion Limitations of current models of service delivery create frustrations for providers and people experiencing social exclusion. Creative commissioning and organisational flexibility are key to facilitating adaptable services.
Key points
-
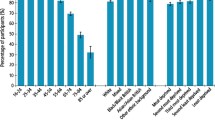
Most services providing dental care for people experiencing social exclusion provide care from fixed sites, operate within routine working hours and allocate fixed appointments.
-
There may be a mismatch between the way these services operate and the needs of people experiencing social exclusion.
-
Numerous challenges exist in delivering appropriate services, including confusion around patient payment, language barriers, rigidity of service delivery strategies, inflexibility of commissioning and lack of resources, including appropriately trained staff.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
International Institute for Labour Studies United Nations Development Programme. Social exclusion and anti-poverty policy: a debate. 1997. Available at https://citeseerx.ist.psu.edu/viewdoc/download?doi=10.1.1.130.260&rep=rep1&type=pdf (accessed June 2022).
O'Donnell P, O'Donovan D, Elmusharaf K. Measuring social exclusion in healthcare settings: a scoping review. Int J Equity Health 2018; 17: 15.
Freeman R. Promoting Inclusion Oral Health: Social Interventions to Reduce Oral Health Inequities. Dent J (Basel) 2020; 8: 5.
Luchenski S, Maguire N, Aldridge R W et al. What works in inclusion health: overview of effective interventions for marginalised and excluded populations. Lancet 2018; 391: 266-280.
Freeman R, Doughty J, Macdonald M E, Muirhead V. Inclusion oral health: Advancing a theoretical framework for policy, research and practice. Community Dent Oral Epidemiol 2020; 48: 1-6.
Groundswell. Healthy Mouths. 2017. Available at https://groundswell.org.uk/wp-content/uploads/2018/10/Groundswell-Healthy-Mouths-Report-Full-Report-Web.pdf (accessed June 2022).
Walsh T, Tickle M, Milsom K, Buchanan K, Zoitopoulos L. An investigation of the nature of research into dental health in prisons: a systematic review. Br Dent J 2008; 204: 683-689.
Daly B, Newton T, Batchelor P, Jones K. Oral health care needs and oral health-related quality of life (OHIP-14) in homeless people. Community Dent Oral Epidemiol 2010; 38: 136-144.
Fennell-Wells A V L, Yusuf H. Child refugees and asylum seekers: oral health and its place in the UK system. Br Dent J 2020; 228: 44-49.
Lewer D, Tweed E J, Aldridge R W, Morley K I. Causes of hospital admission and mortality among 6683 people who use heroin: A cohort study comparing relative and absolute risks. Drug Alcohol Depend 2019; DOI: 10.1016/j.drugalcdep.2019.06.027.
Caton S, Greenhalgh F, Goodacre L. Evaluation of a community dental service for homeless and 'hard to reach' people. Br Dent J 2016; 220: 67-70.
Simons D, Pearson N, Movasaghi Z. Developing dental services for homeless people in East London. Br Dent J 2012; DOI: 10.1038/sj.bdj.2012.891.
Doughty J, Stagnell S, Shah N, Vasey A, Gillard C. The Crisis at Christmas Dental Service: a review of an annual volunteer-led dental service for homeless and vulnerably housed people in London. Br Dent J 2018; 224: 43-47.
Paisi M, Baines R, Worle C, Withers L, Witton R. Evaluation of a community dental clinic providing care to people experiencing homelessness: A mixed methods approach. Health Expect 2020; 23: 1289-1299.
Rodriguez A, Arora G, Beaton L, Fernandes F L, Freeman R. Reflexive mapping exercise of services to support people experiencing or at risk of homelessness: a framework to promote health and social care integration. J Soc Distress Homeless 2020; 30: 181-190.
von Elm E, Altman D G, Egger M et al. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet 2007; 370: 1453-1457.
Saurman E. Improving access: modifying Penchansky and Thomas's Theory of Access. J Health Serv Res Policy 2016; 21: 36-39.
Penchansky R, Thomas J W. The concept of access: definition and relationship to consumer satisfaction. Med Care 1981; 19: 127-140.
Paisi M, Kay E, Plessas A et al. Barriers and enablers to accessing dental services for people experiencing homelessness: A systematic review. Community Dent Oral Epidemiol 2019; 47: 103-111.
Coles E, Freeman R. Exploring the oral health experiences of homeless people: a deconstruction-reconstruction formulation. Community Dent Oral Epidemiol 2016; 44: 53-63.
Hill K B, Rimington D. Investigation of the oral health needs for homeless people in specialist units in London, Cardiff, Glasgow and Birmingham. Prim Health Care Res Dev 2011; 12: 135-144.
Witton R, Plessas A, Wheat H et al. The future of dentistry post-COVID-19: perspectives from Urgent Dental Care centre staff in England. Br Dent J 2021; DOI: 10.1038/s41415-021-3405-1.
Pritchett R M, Hine C E, Franks M A, Fisher-Brown L. Student-led oral health education for the homeless community of East London. Br Dent J 2014; 217: 85-88.
Acknowledgements
The authorship team would like to acknowledge and express our thanks to those individuals and organisations who contributed to the design and distribution of the study, including the British Association for the Study of Community Dentistry and the British Dental Association England Community Dental Services Committee. Of special note is Dr Lyndsey Withers for her review and edits to the results section. Our thanks also go to all those who kindly took the time to participate in the survey.
Author information
Authors and Affiliations
Contributions
Janine Doughty was lead author and coordinated the survey, data analysis and drawing together of the manuscript. Alina Grossman, Tim Newton and Sarah Kaddour supported development of the survey tool and editing the document. Tim Newton and Alina Grossman contributed to data analysis plan. Martha Paisi conducted the final qualitative data analysis and write-up and supported the development of the manuscript. Christina Tran produced the introductory section and synthesised all comments from co-authors. Andrea Rodriguez and Garima Arora produced the mapping and provided input across the document. Vanessa Muirhead has provided conceptual insight throughout, supported the development of the study protocol and provided feedback and edits to the final draft.
Corresponding author
Ethics declarations
The authors declare no conflicts of interest.
Rights and permissions
About this article
Cite this article
Doughty, J., Grossman, A., Paisi, M. et al. A survey of dental services in England providing targeted care for people experiencing social exclusion: mapping and dimensions of access. Br Dent J (2022). https://doi.org/10.1038/s41415-022-4391-7
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41415-022-4391-7
This article is cited by
-
Barriers to access through a student's eyes: A literature review
BDJ In Practice (2025)
-
At the Deep End of dental inequality
British Dental Journal (2025)
-
Best practice models for dental care delivery for people experiencing homelessness
British Dental Journal (2023)
-
Racial inequality in complete dental prosthesis delivered: can public services reduce inequities?
Clinical Oral Investigations (2023)