Abstract
Background
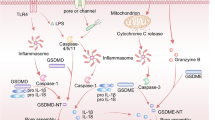
Pyroptosis is closely associated with chemotherapeutic drugs and immune response. Here, we investigated whether oxaliplatin, a key drug in FOLFOX-hepatic artery infusion chemotherapy (FOLFOX-HAIC), induces pyroptosis in hepatoma cells and enhances antitumor immunity after tumor cell death.
Methods
Hepatoma cells were treated with oxaliplatin. Pyroptosis and immunoreactivity were evaluated in vitro and in vivo.
Results
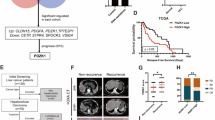
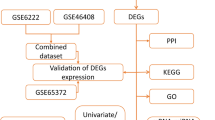
Oxaliplatin activated caspase-3-mediated gasdermin E (GSDME) cleavage and induced pyroptosis in Hep G2 and SK-Hep-1 cells in vitro. Liver cancer cells with high levels of GSDME expression are prone to pyroptosis. Bioinformatic analysis revealed that pyrolysis-related genes are closely related to immunity. In vivo experiments revealed that oxaliplatin exhibited superior antitumor efficacy in mice with normal immune function and more pronounced inhibitory effect on hepatocellular carcinoma with high GSDME levels. Higher levels of cytokines and greater CD8+ T cell infiltration were observed in tumor tissues with better efficacy. Furthermore, an in vitro coculture assay confirmed that oxaliplatin-induced pyroptosis in Hep G2 cells overexpressing GSDME and activated the p38/MAPK signaling pathway to improve the cytotoxicity of CD8+ T cells. Analysis of clinical samples of HCC suggested that the efficacy of FOLFOX-HAIC in patients with high GSDME expression was better than that in patients with low GSDME expression.
Conclusions
Oxaliplatin induced pyroptosis in hepatoma cells by activating caspase-3-mediated cleavage of GSDME, which enhanced the cytotoxicity of CD8+ T cells by regulating the p38/MAPK signaling pathway. These results suggest that GSDME level may be used as a marker to predict the efficacy of FOLFOX-HAIC.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout









Similar content being viewed by others
Data availability
All data associated with this study are present within the main text or the Supplementary Materials.
References
Siegel RL, Miller KD, Fuchs HE, Jemal A. Cancer statistics, 2022. CA Cancer J Clin 2022;72:7–33. https://doi.org/10.3322/caac.21708.
Villanueva A. Hepatocellular Carcinoma. N Engl J Med. 2019;380:1450–62. https://doi.org/10.1056/NEJMra1713263.
Vogel A, Meyer T, Sapisochin G, Salem R, Saborowski A. Hepatocellular carcinoma. Lancet. 2022;400:1345–62. https://doi.org/10.1016/S0140-6736(22)01200-4.
Reig M, Forner A, Rimola J, Ferrer-Fabrega J, Burrel M, Garcia-Criado A, et al. BCLC strategy for prognosis prediction and treatment recommendation: The 2022 update. J Hepatol 2022;76:681–93. https://doi.org/10.1016/j.jhep.2021.11.018.
Sangro B, Sarobe P, Hervas-Stubbs S, Melero I. Advances in immunotherapy for hepatocellular carcinoma. Nat Rev Gastroenterol Hepatol 2021;18:525–43. https://doi.org/10.1038/s41575-021-00438-0.
Mei J, Li SH, Li QJ, Sun XQ, Lu LH, Lin WP, et al. Anti-PD-1 Immunotherapy Improves the Efficacy of Hepatic Artery Infusion Chemotherapy in Advanced Hepatocellular Carcinoma. J Hepatocell Carcinoma. 2021;8:167–76. https://doi.org/10.2147/JHC.S298538.
Finn RS, Qin S, Ikeda M, Galle PR, Ducreux M, Kim TY, et al. Atezolizumab plus Bevacizumab in Unresectable Hepatocellular Carcinoma. N Engl J Med. 2020;382:1894–905. https://doi.org/10.1056/NEJMoa1915745.
Llovet JM, Castet F, Heikenwalder M, Maini MK, Mazzaferro V, Pinato DJ, et al. Immunotherapies for hepatocellular carcinoma. Nat Rev Clin Oncol. 2022;19:151–72. https://doi.org/10.1038/s41571-021-00573-2.
He M, Li Q, Zou R, Shen J, Fang W, Tan G, et al. Sorafenib Plus Hepatic Arterial Infusion of Oxaliplatin, Fluorouracil, and Leucovorin vs Sorafenib Alone for Hepatocellular Carcinoma With Portal Vein Invasion: A Randomized Clinical Trial. JAMA Oncol. 2019;5:953–60. https://doi.org/10.1001/jamaoncol.2019.0250.
Li QJ, He MK, Chen HW, Fang WQ, Zhou YM, Xu L, et al. Hepatic Arterial Infusion of Oxaliplatin, Fluorouracil, and Leucovorin Versus Transarterial Chemoembolization for Large Hepatocellular Carcinoma: A Randomized Phase III Trial. J Clin Oncol 2022;40:150–60. https://doi.org/10.1200/JCO.21.00608.
Deng, M, Zhong, C, Li, D, Guan, R, Lee, C, Chen, H et al. Hepatic arterial infusion chemotherapy-based conversion hepatectomy in responders versus nonresponders with hepatocellular carcinoma: A multicenter cohort study. Int J Surg. 2024. https://doi.org/10.1097/JS9.0000000000002043.
Ouyang L, Shi Z, Zhao S, Wang FT, Zhou TT, Liu B, et al. Programmed cell death pathways in cancer: a review of apoptosis, autophagy and programmed necrosis. Cell Prolif. 2012;45:487–98. https://doi.org/10.1111/j.1365-2184.2012.00845.x.
Sun Y, Peng ZL. Programmed cell death and cancer. Postgrad Med J 2009;85:134–40. https://doi.org/10.1136/pgmj.2008.072629.
Shi J, Gao W, Shao F. Pyroptosis: Gasdermin-Mediated Programmed Necrotic Cell Death. Trends Biochem Sci 2017;42:245–54. https://doi.org/10.1016/j.tibs.2016.10.004.
Wang Y, Gao W, Shi X, Ding J, Liu W, He H, et al. Chemotherapy drugs induce pyroptosis through caspase-3 cleavage of a gasdermin. Nature. 2017;547:99–103. https://doi.org/10.1038/nature22393.
Zhang Z, Zhang Y, Xia S, Kong Q, Li S, Liu X, et al. Gasdermin E suppresses tumour growth by activating anti-tumour immunity. Nature. 2020;579:415–20. https://doi.org/10.1038/s41586-020-2071-9.
Hage C, Hoves S, Strauss L, Bissinger S, Prinz YTPS, et al. Sorafenib Induces Pyroptosis in Macrophages and Triggers Natural Killer Cell-Mediated Cytotoxicity Against Hepatocellular Carcinoma. Hepatology. 2019;70:1280–97. https://doi.org/10.1002/hep.30666.
Wang S, Zhang MJ, Wu ZZ, Zhu SW, Wan SC, Zhang BX, et al. GSDME Is Related to Prognosis and Response to Chemotherapy in Oral Cancer. J Dent Res. 2022;101:848–58. https://doi.org/10.1177/00220345211073072.
Yan H, Luo B, Wu X, Guan F, Yu X, Zhao L, et al. Cisplatin Induces Pyroptosis via Activation of MEG3/NLRP3/caspase-1/GSDMD Pathway in Triple-Negative Breast Cancer. Int J Biol Sci. 2021;17:2606–21. https://doi.org/10.7150/ijbs.60292.
Li RY, Zheng ZY, Li ZM, Heng JH, Zheng YQ, Deng DX, et al. Cisplatin-induced pyroptosis is mediated via the CAPN1/CAPN2-BAK/BAX-caspase-9-caspase-3-GSDME axis in esophageal cancer. Chem Biol Interact. 2022;361:109967 https://doi.org/10.1016/j.cbi.2022.109967.
Zhang CC, Li CG, Wang YF, Xu LH, He XH, Zeng QZ, et al. Chemotherapeutic paclitaxel and cisplatin differentially induce pyroptosis in A549 lung cancer cells via caspase-3/GSDME activation. Apoptosis. 2019;24:312–25. https://doi.org/10.1007/s10495-019-01515-1.
Riddell IA. Cisplatin and Oxaliplatin: Our Current Understanding of Their Actions. Met Ions Life Sci. 2018;18. https://doi.org/10.1515/9783110470734-007.
Sharif S, O’Connell MJ, Yothers G, Lopa S, Wolmark N. FOLFOX and FLOX regimens for the adjuvant treatment of resected stage II and III colon cancer. Cancer Invest. 2008;26:956–63. https://doi.org/10.1080/07357900802132550.
Livak KJ, Schmittgen TD. Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)) Method. Methods. 2001;25:402–8. https://doi.org/10.1006/meth.2001.1262.
Llovet JM, Kelley RK, Villanueva A, Singal AG, Pikarsky E, Roayaie S, et al. Hepatocellular carcinoma. Nat Rev Dis Prim. 2021;7:6 https://doi.org/10.1038/s41572-020-00240-3.
Deng, M, Lei, Q, Wang, J, Lee, C, Guan, R, Li, S et al. Nomograms for predicting the recurrence probability and recurrence-free survival in patients with hepatocellular carcinoma after conversion hepatectomy based on hepatic arterial infusion chemotherapy: a multicenter, retrospective study. Int J Surg. 2023. https://doi.org/10.1097/JS9.0000000000000376.
Li, SH, Mei, J, Cheng, Y, Li, Q, Wang, QX, Fang, CK et al. Postoperative Adjuvant Hepatic Arterial Infusion Chemotherapy With FOLFOX in Hepatocellular Carcinoma With Microvascular Invasion: A Multicenter, Phase III, Randomized Study. J Clin Oncol. 2022; JCO2201142. https://doi.org/10.1200/JCO.22.01142.
Yu P, Zhang X, Liu N, Tang L, Peng C, Chen X. Pyroptosis: mechanisms and diseases. Signal Transduct Target Ther. 2021;6:128 https://doi.org/10.1038/s41392-021-00507-5.
Yu J, Li S, Qi J, Chen Z, Wu Y, Guo J, et al. Cleavage of GSDME by caspase-3 determines lobaplatin-induced pyroptosis in colon cancer cells. Cell Death Dis. 2019;10:193 https://doi.org/10.1038/s41419-019-1441-4.
Zhang X, Zhang H. Chemotherapy drugs induce pyroptosis through caspase-3-dependent cleavage of GSDME. Sci China Life Sci 2018;61:739–40. https://doi.org/10.1007/s11427-017-9158-x.
Kovacs SB, Miao EA. Gasdermins: Effectors of Pyroptosis. Trends Cell Biol. 2017;27:673–84. https://doi.org/10.1016/j.tcb.2017.05.005.
Elmore S. Apoptosis: a review of programmed cell death. Toxicol Pathol 2007;35:495–516. https://doi.org/10.1080/01926230701320337.
Zhang CC, Li CG, Wang YF, Xu LH, He XH, Zeng QZ, et al. Chemotherapeutic paclitaxel and cisplatin differentially induce pyroptosis in A549 lung cancer cells via caspase-3/GSDME activation. Apoptosis Int J Program Cell Death. 2019;24:312–25. https://doi.org/10.1007/s10495-019-01515-1.
Bertheloot D, Latz E, Franklin BS. Necroptosis, pyroptosis and apoptosis: an intricate game of cell death. Cell Mol Immunol 2021;18:1106–21. https://doi.org/10.1038/s41423-020-00630-3.
Liu J, Hong M, Li Y, Chen D, Wu Y, Hu Y. Programmed Cell Death Tunes Tumor Immunity. Front Immunol 2022;13:847345 https://doi.org/10.3389/fimmu.2022.847345.
Jiang M, Qi L, Li L, Li Y. The caspase-3/GSDME signal pathway as a switch between apoptosis and pyroptosis in cancer. Cell Death Discov. 2020;6:112 https://doi.org/10.1038/s41420-020-00349-0.
Garcia-Diaz A, Shin DS, Moreno BH, Saco J, Escuin-Ordinas H, Rodriguez GA, et al. Interferon Receptor Signaling Pathways Regulating PD-L1 and PD-L2 Expression. Cell Rep. 2017;19:1189–201. https://doi.org/10.1016/j.celrep.2017.04.031.
Liu, J, Wei, L, Hu, N, Wang, D, Ni, J, Zhang, S et al. FBW7-mediated ubiquitination and destruction of PD-1 protein primes sensitivity to anti-PD-1 immunotherapy in non-small cell lung cancer. J Immunother Cancer. 2022; 10. https://doi.org/10.1136/jitc-2022-005116.
Tang R, Xu J, Zhang B, Liu J, Liang C, Hua J, et al. Ferroptosis, necroptosis, and pyroptosis in anticancer immunity. J Hematol Oncol 2020;13:110 https://doi.org/10.1186/s13045-020-00946-7.
Deng M, Sun S, Zhao R, Guan R, Zhang Z, Li S, et al. The pyroptosis-related gene signature predicts prognosis and indicates immune activity in hepatocellular carcinoma. Mol Med. 2022;28:16 https://doi.org/10.1186/s10020-022-00445-0.
Xia X, Wang X, Cheng Z, Qin W, Lei L, Jiang J, et al. The role of pyroptosis in cancer: pro-cancer or pro-“host”? Cell Death Dis. 2019;10:650 https://doi.org/10.1038/s41419-019-1883-8.
Kaplanski G. Interleukin-18: Biological properties and role in disease pathogenesis. Immunol Rev 2018;281:138–53. https://doi.org/10.1111/imr.12616.
Romagnani S. T-cell subsets (Th1 versus Th2). Ann Allergy Asthma Immunol. 2000;85:21 https://doi.org/10.1016/S1081-1206(10)62426-X.
Romagnani S. Human TH1 and TH2 subsets: regulation of differentiation and role in protection and immunopathology. Int Arch Allergy Immunol. 1992;98:279–85. https://doi.org/10.1159/000236199.
Rabinovitch A, Suarez-Pinzon WL. Cytokines and their roles in pancreatic islet beta-cell destruction and insulin-dependent diabetes mellitus. Biochem Pharmacol. 1998;55:1139–49. https://doi.org/10.1016/s0006-2952(97)00492-9.
Powrie F, Coffman RL. Cytokine regulation of T-cell function: potential for therapeutic intervention. Immunol Today. 1993;14:270–4. https://doi.org/10.1016/0167-5699(93)90044-L.
Mosmann TR, Coffman RL. TH1 and TH2 cells: different patterns of lymphokine secretion lead to different functional properties. Annu Rev Immunol. 1989;7:145–73. https://doi.org/10.1146/annurev.iy.07.040189.001045.
Ren J, Tao Y, Peng M, Xiao Q, Jing Y, Huang J, et al. Targeted activation of GPER enhances the efficacy of venetoclax by boosting leukemic pyroptosis and CD8+ T cell immune function in acute myeloid leukemia. Cell Death Dis. 2022;13:915 https://doi.org/10.1038/s41419-022-05357-9.
Zhang W, Liu HT. MAPK signal pathways in the regulation of cell proliferation in mammalian cells. Cell Res. 2002;12:9–18. https://doi.org/10.1038/sj.cr.7290105.
Coulthard LR, White DE, Jones DL, McDermott MF, Burchill SA. p38(MAPK): stress responses from molecular mechanisms to therapeutics. Trends Mol Med. 2009;15:369–79. https://doi.org/10.1016/j.molmed.2009.06.005.
Acknowledgements
We are grateful to all patients and healthy participants for their involvement. We would like to thank Figdraw (www.figdraw.com).
Funding
This study was supported by the National Natural Science Foundation of China (No. 82303156, No. 82172579); Science and Technology Planning Project of Guangzhou (No. 2023A04J1777, No. 2023A04J1781); Clinical Trials Project (5010 Project) of Sun Yat-sen University (No. 5010-2017009, No. 5010-2023001).
Author information
Authors and Affiliations
Contributions
M. Deng, R. Zhao, and R. Guo were involved in the study conceptualization; M. Deng, R. Zhao, H. Zou, J. Wang, C. Lee, H. Cai and R. Guo contributed in the investigation and methodology; M. Deng, H. Zou, J. Wang, R. Guan, B. He, and J. Zhou performed the experiments; M. Deng, H. Zou, and H. Cai contributed in data curation and software analysis; M. Deng, R. Zhao, S. Li, W. Wei, H. Cai, and R. Guo contributed in formal analysis; M. Deng, R. Guan, and B. He collected the clinical samples; W. Wei and R. Guo provided supervision. H. Cai, W. Wei and R. Guo contributed in funding acquisition; M. Deng, H. Zou, R. Zhao, R. Guan, H. Cai, and R. Guo prepared the manuscript; All authors were involved in the critical review and editing of the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval and consent to participate
Informed consent was obtained from all patients included in this study. The research was carried out according to the World Medical Association Declaration of Helsinki and approved by the Institutional Ethical Review Board of the SYSUCC (B202031801). The animal procedures were approved by the Institutional Animal Care and Use Committee of Sun Yat-sen University Cancer Center (L102042022020D).
Consent for publication
All authors have reviewed the final version of the manuscript and are in agreement its content and submission.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Deng, M., Zhao, R., Zou, H. et al. Oxaliplatin induces pyroptosis in hepatoma cells and enhances antitumor immunity against hepatocellular carcinoma. Br J Cancer 132, 371–383 (2025). https://doi.org/10.1038/s41416-024-02908-z
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41416-024-02908-z