Abstract
Background
Previous studies using a single obesity indicator cannot fully assess the association between body shape and mortality. We aimed to investigate the association between complementary anthropometric measures and all-cause mortality risk.
Methods
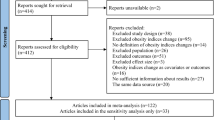
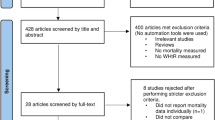
We combined National Health and Nutrition Examination Survey (NHANES) data from 2011 to 2016 with mortality data up to December 31, 2019. After excluding individuals with cancer at baseline, 13,728 participants were included. Cox regression models and restricted cubic spline (RCS) analyses were used to explore the association between general obesity, central obesity, and peripheral fat indicators and all-cause mortality risk.
Results
A total of 743 deaths occurred over a median follow-up of 5.83 years. In multivariable-adjusted Cox models, each 10-cm increase in waist circumference (WC), each 0.1-unit increase in waist-to-height ratio (WHtR), and each 0.01-unit increase in A Body Shape Index (ABSI) were associated with 20% (HR = 1.20; 95% CI: 1.02–1.41), 119% (2.19; 1.70–2.83), and 5% (1.05; 1.03–1.08) increased all-cause mortality risk, respectively. Conversely, each 1-cm increment in mid-arm circumference (MAC) was associated with 13% (HR = 0.87; 95% CI: 0.83–0.92) decreased mortality risk. Compared with normal group (body mass index (BMI): 18.5- <25.0), underweight (HR = 1.97; 95% CI: 1.12–3.45) and grade 3 obesity (1.37; 1.04–1.81) were at higher mortality risk. However, after further adjustment for WC, the effect of grade 3 obesity disappeared, and the RCS analyses for BMI changed from a J-shaped (P < 0.05 for non-linearity test) to a negative association (P < 0.01).
Conclusions
Underweight, grade 3 obesity, and central obesity were associated with an increased mortality risk, while peripheral fat was inversely associated with mortality.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
Publicly available datasets were analyzed in this study. This data can be found here: https://wwwn.cdc.gov/nchs/nhanes/ (accessed on 27 May 2023).
References
Wang Y, Zhao L, Gao L, Pan A, Xue H. Health policy and public health implications of obesity in China. Lancet Diabetes Endocrinol. 2021;9:446–461.
van Dijk SJ, Tellam RL, Morrison JL, Muhlhausler BS, Molloy PL. Recent developments on the role of epigenetics in obesity and metabolic disease. Clin Epigenetics. 2015;7:66.
Seravalle G, Grassi G. Obesity and hypertension. Pharm Res. 2017;122:1–7.
Redfield MM, Borlaug BA. Heart failure with preserved ejection fraction: a review. JAMA. 2023;329:827–38.
Tang X, Zhao W, Lu M, Zhang X, Zhang P, Xin Z, et al. Relationship between central obesity and the incidence of cognitive impairment and dementia from cohort studies involving 5,060,687 participants. Neurosci Biobehav Rev. 2021;130:301–13.
Ng ACT, Delgado V, Borlaug BA, Bax JJ. Diabesity: the combined burden of obesity and diabetes on heart disease and the role of imaging. Nat Rev Cardiol. 2021;18:291–304.
Morais AHA, Passos TS, de Lima Vale SH, da Silva Maia JK, Maciel BLL. Obesity and the increased risk for COVID-19: mechanisms and nutritional management. Nutr Res Rev. 2021;34:209–21.
Flegal K, Graubard B, Williamson D, Gail M. Excess deaths associated with underweight, overweight, and obesity. JAMA. 2005;293:1861–7.
World Health Organization. Obesity. 2023. https://www.who.int/health-topics/obesity#tab=tab_1 .
Chooi YC, Ding C, Magkos F. The epidemiology of obesity. Metab: Clin Exp. 2019;92:6–10.
World Obesity Federation. World Obesity Atlas 2023. 2023. https://data.worldobesity.org/publications/?cat=19 .
Liu B, Du Y, Wu Y, Snetselaar LG, Wallace RB, Bao W. Trends in obesity and adiposity measures by race or ethnicity among adults in the United States 2011-18: population based study. Bmj. 2021;372:n365.
Krakauer NY, Krakauer JC. A new body shape index predicts mortality hazard independently of body mass index. PloS One. 2012;7:e39504.
Powell-Wiley TM, Poirier P, Burke LE, Després JP, Gordon-Larsen P, Lavie CJ, et al. Obesity and cardiovascular disease: a scientific statement from the American Heart Association. Circulation. 2021;143:e984–e1010.
Jayedi A, Soltani S, Zargar MS, Khan TA, Shab-Bidar S. Central fatness and risk of all cause mortality: systematic review and dose-response meta-analysis of 72 prospective cohort studies. Bmj. 2020;370:m3324.
Wu LW, Lin YY, Kao TW, Lin CM, Wang CC, Wang GC, et al. Mid-arm circumference and all-cause, cardiovascular, and cancer mortality among obese and non-obese US adults: the National Health and Nutrition Examination Survey III. Sci Rep. 2017;7:2302.
National Health and Nutrition Examination Survey. About NHANES. 2021. https://www.cdc.gov/nchs/nhanes/participant/participant-about.htm.
Global BMIMC, Di Angelantonio E, Bhupathiraju ShN, Wormser D, Gao P, Kaptoge S, et al. Body-mass index and all-cause mortality: individual-participant-data meta-analysis of 239 prospective studies in four continents. Lancet (Lond, Engl). 2016;388:776–86.
National Health and Nutrition Examination Survey. NHANES 2011-2012 Procedure Manuals. https://wwwn.cdc.gov/nchs/nhanes/continuousnhanes/manuals.aspx?BeginYear=2011 .
National Health and Nutrition Examination Survey. NHANES 2013-2014 Procedure Manuals. https://wwwn.cdc.gov/nchs/nhanes/continuousnhanes/manuals.aspx?BeginYear=2013 .
National Health and Nutrition Examination Survey. NHANES 2015-2016 Procedure Manuals. https://wwwn.cdc.gov/nchs/nhanes/continuousnhanes/manuals.aspx?BeginYear=2015 .
Butt JH, Petrie MC, Jhund PS, Sattar N, Desai AS, Køber L, et al. Anthropometric measures and adverse outcomes in heart failure with reduced ejection fraction: revisiting the obesity paradox. Eur Heart J. 2023;44:1136–53.
Petursson H, Sigurdsson JA, Bengtsson C, Nilsen TI, Getz L. Body configuration as a predictor of mortality: comparison of five anthropometric measures in a 12 year follow-up of the Norwegian HUNT 2 study. PloS one. 2011;6:e26621.
He L, Yang N, Wang J, Huang J, Li W, Xu L, et al. Mid-arm muscle and subcutaneous fat associated with all-cause mortality independent of BMI: a prospective cohort study. Obes (Silver Spring, Md). 2021;29:1203–14.
Koster A, Leitzmann MF, Schatzkin A, Mouw T, Adams KF, van Eijk JT, et al. Waist circumference and mortality. Am J Epidemiol. 2008;167:1465–75.
Simpson JA, MacInnis RJ, Peeters A, Hopper JL, Giles GG, English DR. A comparison of adiposity measures as predictors of all-cause mortality: the Melbourne Collaborative Cohort Study. Obes (Silver Spring, Md). 2007;15:994–1003.
Fan J, Yu C, Guo Y, Bian Z, Sun Z, Yang L, et al. Frailty index and all-cause and cause-specific mortality in Chinese adults: a prospective cohort study. Lancet Public Health. 2020;5:e650–e660.
Weng L, Fan J, Yu C, Guo Y, Bian Z, Wei Y, et al. Body-mass index and long-term risk of sepsis-related mortality: a population-based cohort study of 0.5 million Chinese adults. Crit Care. 2020;24:534.
Li B, Chen L, Hu X, Tan T, Yang J, Bao W, et al. Association of serum uric acid with all-cause and cardiovascular mortality in diabetes. Diabetes Care. 2023;46:425–33.
Sun YQ, Burgess S, Staley JR, Wood AM, Bell S, Kaptoge SK, et al. Body mass index and all cause mortality in HUNT and UK Biobank studies: linear and non-linear mendelian randomisation analyses. Bmj. 2019;364:l1042.
Aune D, Sen A, Prasad M, Norat T, Janszky I, Tonstad S, et al. BMI and all cause mortality: systematic review and non-linear dose-response meta-analysis of 230 cohort studies with 3.74 million deaths among 30.3 million participants. Bmj. 2016;353:i2156.
Berrington de Gonzalez A, Hartge P, Cerhan JR, Flint AJ, Hannan L, MacInnis RJ, et al. Body-mass index and mortality among 1.46 million white adults. N. Engl J Med. 2010;363:2211–9.
Jiang K, Singh Maharjan SR, Slee A, Davenport A. Differences between anthropometric and bioimpedance measurements of muscle mass in the arm and hand grip and pinch strength in patients with chronic kidney disease. Clin Nutr. 2021;40:320–3.
Wu T, Xu H, Zou Y, Cui J, Xu K, Zhou M et al. Mid-arm muscle circumference or body weight-standardized hand grip strength in the GLIM superiorly predicts survival in chinese colorectal cancer patients. Nutrients 2022; 14(23):5166.
Mason C, Craig CL, Katzmarzyk PT. Influence of central and extremity circumferences on all-cause mortality in men and women. Obes (Silver Spring, Md). 2008;16:2690–5.
Howell CR, Mehta T, Ejima K, Ness KK, Cherrington A, Fontaine KR. Body composition and mortality in Mexican American adults: results from the national health and nutrition examination survey. Obes (Silver Spring, Md). 2018;26:1372–80.
Mehran L, Amouzegar A, Fanaei SM, Masoumi S, Azizi F. Anthropometric measures and risk of all-cause and cardiovascular mortality: an 18 years follow-up. Obes Res Clin Pr. 2022;16:63–71.
Acknowledgements
We acknowledge the staff at the National Center for Health Statistics at the CDC, who design, collect, administer the NHANES data and release the data available for public use. We are thankful to all study participants for their cooperation.
Funding
This work was supported by Natural Science Foundation of Shandong Province (ZR2023QH188), China Postdoctoral Science Foundation (2023M731839), Qingdao Postdoctoral Innovation Project (QDBSH20230102012), Qingdao University Scientific Research Startup Fund (DC2200002531), Mount Taishan Scholar Youth Program. The funders had no role in the study design, data collection, data analysis and interpretation, writing of the report, or the decision to submit the article for publication.
Author information
Authors and Affiliations
Contributions
JF conceived and designed the study. XS and LC analyzed the data. XS drafted the manuscript. JF and LC helped the interpretation of the results. JF contributed to the critical revision of the manuscript for important intellectual content and approved the final version of the manuscript. All authors reviewed and approved the final manuscript. DZ is the guarantor.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shi, X., Chai, L., Zhang, D. et al. Association between complementary anthropometric measures and all-cause mortality risk in adults: NHANES 2011–2016. Eur J Clin Nutr 79, 71–78 (2025). https://doi.org/10.1038/s41430-024-01496-8
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41430-024-01496-8