Abstract
Purpose
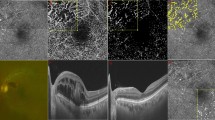
To compare the time to resolution of perivascular infiltrates in tubercular retinal vasculitis (TRV) between anti-tubercular therapy (ATT) alone, and in combination with systemic corticosteroids.
Methods
Observational retrospective cohort study in a tertiary eye centre in eastern India. Patients with TRV who were treated with anti-tubercular therapy (ATT) alone (Group A), or in combination with systemic corticosteroids (Group B) were included in the study. Eyes with additional inflammatory signs (cystoid macular oedema, vitritis ≥2+, optic disc oedema) were excluded. Resolution was defined as complete disappearance of perivascular infiltrates on seven-field fundus photographs. Descriptive statistics were used for demographic data. A linear mixed effects model was applied to adjust for intereye correlations, in patients with bilateral disease. The primary outcome measure was time to resolution of perivascular infiltrates. Secondary outcome measure was need for laser or surgical intervention for management of complications of TRV.
Results
Fifty eyes of 39 patients (Group A 21/18 and Group B 29/21) were included. Both groups had similar demographics and severity of vasculitis. All patients had complete resolution of TRV. On adjusting for intereye correlation, the mean difference in time to resolution between the two groups (Group A, 3.24 [95% CI 2.69–3.77] months, and Group B, 4.76 [95% CI 3.52–5.99] months) was not statistically significant (0.96 weeks [−0.52 to 2.45] p = 0.21). Vaso-occlusive complications and healing patterns were similar in both groups.
Conclusions
ATT alone, may be sufficient for resolution of perivascular infiltrates, in TRV without additional inflammatory signs.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Bansal R, Gupta A, Gupta V, Dogra MR, Bambery P, Arora SK. Role of anti-tubercular therapy in uveitis with latent/manifest tuberculosis. Am J Ophthalmol. 2008;146:772–9. https://doi.org/10.1016/j.ajo.2008.06.011.
Basu S, Nayak S, Padhi TR, Das T. Progressive ocular inflammation following anti-tubercular therapy for presumed ocular tuberculosis in a high-endemic setting. Eye. 2013;27:657–62. https://doi.org/10.1038/eye.2013.5.
Kee AR, Gonzalez-Lopez JJ, Al-Hity A, Gupta B, Lee CS, Gunasekeran DV, et al. Anti-tubercular therapy for intraocular tuberculosis: a systematic review and meta-analysis. Surv Ophthalmol. 2016;61:628–53. https://doi.org/10.1016/j.survophthal.2016.03.001.
Nahon-Esteve S, Martel A, Maschi C, Alketbi M, Baillif S, Tieulie N. Uveitis associated with latent tuberculosis: a comparative study of the impact of antitubercular therapy combined or not with systemic corticosteroids. Eur J Ophthalmol. 2020:1120672120962066. https://doi.org/10.1177/1120672120962066.
Gupta V, Shoughy SS, Mahajan S, Khairallah M, Rosenbaum JT, Curi A, et al. Clinics of ocular tuberculosis. Ocul Immunol Inflamm. 2015;23:14–24. https://doi.org/10.3109/09273948.2014.986582.
Gunasekeran DV, Agrawal R, Agarwal A, Carreño E, Raje D, Aggarwal K, et al. The Collaborative Ocular Tuberculosis Study (COTS)-1: a multinational review of 251 patients with tubercular retinal vasculitis. Retina 2019;39:1623–30. https://doi.org/10.1097/IAE.0000000000002194.
Kaza H, Tyagi M, Pathangay A, Basu S. Clinical predictors of tubercular retinal vasculitis in a high endemic country. Retina. 2021;41:438–44. https://doi.org/10.1097/IAE.0000000000002829.
Hamade IH, Tabbara KF. Complications of presumed ocular tuberculosis. Acta Ophthalmol. 2010;88:905–9. https://doi.org/10.1111/j.1755-3768.2009.01579.x.
Patel SS, Saraiya NV, Tessler HH, Goldstein DA. Mycobacterial ocular inflammation: delay in diagnosis and other factors impacting morbidity. JAMA Ophthalmol. 2013;131:752–8. https://doi.org/10.1001/jamaophthalmol.2013.71.
Gupta V, Bansal R, Gupta A. Continuous progression of tubercular serpiginous-like choroiditis after initiating antituberculosis treatment. Am J Ophthalmol. 2011;152:857–63.e2. https://doi.org/10.1016/j.ajo.2011.05.004.
Agarwal M, Biswas J. Unilateral frosted branch angiitis in a patient with abdominal tuberculosis. Retin Cases Brief Rep. 2008;2:39–40. https://doi.org/10.1097/01.iae.0000247167.81281.53.
El-Asrar AM, Al-Kharashi SA. Full panretinal photocoagulation and early vitrectomy improve prognosis of retinal vasculitis associated with tuberculoprotein hypersensitivity (Eales’ disease). Br J Ophthalmol. 2002;86:1248–51. https://doi.org/10.1136/bjo.86.11.1248.
Verhoeff FH, Simpson GV. Tubercle within central retinal vein: haemorrhagic glaucoma; periphlebitis retinalis in other eye. Arch Ophthalmol. 1940;24:645.
Saini JS, Mukherjee AK, Nadkarni N. Primary tuberculosis of the retina. Br J Ophthalmol. 1986;70:533–5.
Basu S, Mittal R, Balne PK, Sharma S. Intraretinal tuberculosis. Ophthalmology. 2012;119:2192–3.e1.
Gupta A, Gupta V, Arora S, Dogra MR, Bambery P. PCR-positive tubercular retinal vasculitis: clinical characteristics and management. Retina. 2001;21:435–44.
Singh R, Toor P, Parchand S, Sharma K, Gupta V, Gupta A. Quantitative polymerase chain reaction for Mycobacterium tuberculosis in so-called Eales’ disease. Ocul Immunol Inflamm. 2012;20:153–7. https://doi.org/10.3109/09273948.2012.658134.
Verma A, Biswas J, Dhanurekha L, Gayathri R, Therese KL. Detection of Mycobacterium tuberculosis with nested polymerase chain reaction analysis in enucleated eyeball in Eales’ disease. Int Ophthalmol. 2016;36:413–7. https://doi.org/10.1007/s10792-015-0144-9.
Gupta A, Bansal R, Gupta V, Sharma A, Bambery P. Ocular signs predictive of tubercular uveitis. Am J Ophthalmol. 2010;149:562–70.
Fountain JA, Werner RB. Tuberculous retinal vasculitis. Retina 1984;4:48–50. https://doi.org/10.1097/00006982-198400410-00008.
Simmons CP, Thwaites GE, Quyen NT, Chau TT, Mai PP, Dung NT, et al. The clinical benefit of adjunctive dexamethasone in tuberculous meningitis is not associated with measurable attenuation of peripheral or local immune responses. J Immunol. 2005;175:579–90. https://doi.org/10.4049/jimmunol.175.1.579.
Thwaites GE, Macmullen-Price J, Tran TH, Pham PM, Nguyen TD, Simmons CP, et al. Serial MRI to determine the effect of dexamethasone on the cerebral pathology of tuberculous meningitis: an observational study. Lancet Neurol. 2007;6:230–6. https://doi.org/10.1016/S1474-4422(07)70034-0.
Shah SM, Howard RS, Sarkies NJ, Graham EM. Tuberculosis presenting as retinal vasculitis. J R Soc Med. 1988;81:232–3.
Doycheva D, Pfannenberg C, Hetzel J, Deuter CM, Pavesio C, Kempf VA, et al. Presumed tuberculosis-induced retinal vasculitis, diagnosed with positron emission tomography (18F-FDG-PET/CT), aspiration biopsy, and culture. Ocul Immunol Inflamm. 2010;18:194–9. https://doi.org/10.3109/09273948.2010.483318.
Agarwal A, Karkhur S, Aggarwal K, Invernizzi A, Singh R, Dogra MR, et al. Epidemiology and clinical features of inflammatory retinal vascular occlusions: pooled data from two tertiary-referral institutions. Clin Exp Ophthalmol. 2018;46:62–74.
Acknowledgements
The study was supported by Hyderabad Eye Research Foundation. We also thank Krishna Gopal Panda and Aniruddha Banerjee for fundus photography, Bhawna Garg for most statistical analyses, Mohammed Hasnat Ali for performing statistical analysis for intereye corelation.
Author information
Authors and Affiliations
Contributions
AK: Data collection and analysis; revision of manuscript; final approval. VG: Data collection and analysis; revision of manuscript; final approval. AK: Data collection and analysis; revision of manuscript; final approval. SB: Conception of study; analysis; initial draft and revision of manuscript. All authors approved the submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kelgaonkar, A., Govindhari, V., Khalsa, A. et al. Anti-tubercular therapy alone for treatment of isolated tubercular retinal vasculitis. Eye 36, 1777–1782 (2022). https://doi.org/10.1038/s41433-021-01727-3
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41433-021-01727-3