Abstract
Objectives
To determine the correlation of inner retinal hyper-reflective foci (HRFs) number with Flood-illumination Adaptive Optics Ophthalmoscopy (FIAOO) grading and systemic organ involvement in a cohort of patients with Fabry disease (FD).
Methods
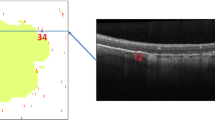
Observational and cross-sectional study. Thirty-two eyes of 16 genetically proven FD patients (11 females) were included in the analysis. Data regarding therapeutic regimen and organ involvement (heart, kidney, and brain) of each patient were reviewed. Patients underwent full ophthalmological examination including best-corrected visual acuity, retinography, spectral domain optical coherence tomography and FIAOO imaging grading of retinal vessels. The number of inner-retinal HRFs was determined within the central 2500 μm at the foveal level in each patient and correlation with ocular imaging findings and systemic involvement parameters was assessed through Spearman correlation analysis and Generalized Linear Models (GLM) with a robust Huber White standard error estimation.
Results
Inner retinal HRFs number showed a significant association with male gender, use of enzyme replacement therapy and presence of retinal vessel tortuosity (all p < 0.001). Severity of NHYA class and presence of cornea verticillata reached a quasi-significant association (p = 0.089 and p = 0.07, respectively). Increase of FIAOO grading was associated to increased HRFs number (p < 0.001) and increase in estimated glomerular filtration rate was inversely associated with HRFs number (p = 0.04).
Conclusions
Inner retinal HRF number correlated with organ involvement and ocular imaging findings in FD patients. They may represent a biomarker of disease severity in diagnosed patients and their presence should enhance the suspect of FD in the appropriate clinical setting.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Echevarria L, Benistan K, Toussaint A, Dubourg O, Hagege AA, Eladari D, et al. X-chromosome inactivation in female patients with Fabry disease. Clin Genet. 2016;89:44–54. https://doi.org/10.1111/cge.12613.
Waldek S, Patel MR, Banikazemi M, Lemay R, Lee P. Life expectancy and cause of death in males and females with Fabry disease: Findings from the Fabry Registry. Genet Med. 2009;11:790–6. https://doi.org/10.1097/GIM.0b013e3181bb05bb.
Ortiz A, Germain DP, Desnick RJ, Politei J, Mauer M, Burlina A, et al. Fabry disease revisited: Management and treatment recommendations for adult patients. Mol Genet Metab. 2018;123:416–27. https://doi.org/10.1016/j.ymgme.2018.02.014.
Lidove O, Jaussaud R, Aractingi S. Dermatological and soft-tissue manifestations of Fabry disease: characteristics and response to enzyme replacement therapy. In: Mehta A, Beck M, Sunder-Plassmann G, editors. Fabry Disease: Perspectives from 5 Years of FOS. Oxford: Oxford PharmaGenesis; 2006. Chapter 24. Available from: https://www.ncbi.nlm.nih.gov/books/NBK11605/.
El Dib R, Gomaa H, Carvalho RP, Camargo SE, Bazan R, Barretti P, et al. Enzyme replacement therapy for Anderson-Fabry disease. Cochrane Database Syst Rev. 2016;2016:006663. https://doi.org/10.1002/14651858.CD006663.pub4.
Tsujiuchi M, Ebato M, Maezawa H, Mizukami T, Nogi A, Ikeda N, et al. Long-term effects of enzyme replacement therapy for anderson-fabry disease. Int Heart J. 2019;60:208–14. https://doi.org/10.1536/ihj.17-688.
Van Der Tol L, Sminia ML, Hollak CEM, Biegstraaten M. Cornea verticillata supports a diagnosis of Fabry disease in non-classical phenotypes: Results from the Dutch cohort and a systematic review. Br J Ophthalmol. 2016;100:3–8. https://doi.org/10.1136/bjophthalmol-2014-306433.
Samiy N. Ocular features of fabry disease: diagnosis of a treatable life-threatening disorder. Surv Ophthalmol. 2008;53:416–23. https://doi.org/10.1016/j.survophthal.2008.04.005.
Sodi A, Ioannidis AS, Mehta A, Davey C, Beck M, Pitz S. Ocular manifestations of Fabry’s disease: Data from the Fabry Outcome Survey. Br J Ophthalmol. 2007;91:210–4. https://doi.org/10.1136/bjo.2006.100602.
Pitz S, Kalkum G, Arash L, Karabul N, Sodi A, Larroque S, et al. Ocular signs correlate well with disease severity and genotype in Fabry disease. PLoS ONE. 2015;10:0120814. https://doi.org/10.1371/journal.pone.0120814.
Sodi A, Germain DP, Bacherini D, Finocchio L, Pacini B, Marziali E, et al. In vivo observation of retinal vascular deposits using adaptive optics imaging in Fabry disease. Retina. 2020;40:1623–9. https://doi.org/10.1097/IAE.0000000000002648.
Akyol E, Hagag AM, Sivaprasad S, Lotery AJ. Adaptive optics: principles and applications in ophthalmology. Eye. 2021;35:244–64. https://doi.org/10.1038/s41433-020-01286-z.
Atiskova Y, Rassuli R, Koehn AF, Golsari A, Wagenfeld L, du Moulin M, et al. Retinal hyperreflective foci in Fabry disease. Orphanet J Rare Dis. 2019;14:296 https://doi.org/10.1186/s13023-019-1267-2.
Yanık Ö, Çıkı K, Özmert E, Sivri S. Vascular and structural analyses of retinal and choroidal alterations in Fabry disease: the effect of hyperreflective foci and retinal vascular tortuosity. Ophthalmic Genet. 2022;43:344–53. https://doi.org/10.1080/13816810.2022.2025607.
Lee H, Lee J, Chung H, Kim HC. Baseline spectral domain optical coherence tomographic hyperreflective foci as a predictor of visual outcome and recurrence for central serous chorioretinopathy. Retina. 2016;36:1372–80. https://doi.org/10.1097/IAE.0000000000000929.
Romano F, Mercuri S, Arrigo A, Marchese A, Cicinelli MV, Albertini GC, et al. Identification of hyperreflective foci in angioid streaks. Eye. 2019;33:1916–23. https://doi.org/10.1038/s41433-019-0483-2.
Parodi MB, Arrigo A, Romano F, Aragona E, Marchese A, Cicinelli MV, et al. Hyperreflective foci number correlates with choroidal neovascularization activity in angioid streaks. Investig Ophthalmol Vis Sci. 2018;59:3314–9. https://doi.org/10.1167/iovs.18-24291.
Giansanti F, Mercuri S, Vannozzi L, Govetto A, Minnella AM, Caporossi T, et al. Adaptive optics imaging to analyze the photoreceptor layer reconstitution in acute syphilitic posterior placoid chorioretinopathy. Life. 2022;12:1361 https://doi.org/10.3390/life12091361.
Murro V, Mucciolo DP, Giorgio D, Pavese L, Boraldi F, Quaglino D, et al. Adaptive optics imaging in patients affected by pseudoxanthoma elasticum. Am J Ophthalmol. 2021;224:84–95. https://doi.org/10.1016/j.ajo.2020.12.007.
Koch E, Rosenbaum D, Brolly A, Sahel JA, Chaumet-Riffaud P, Girerd X, et al. Morphometric analysis of small arteries in the human retina using adaptive optics imaging: Relationship with blood pressure and focal vascular changes. J Hypertens. 2014;32:890–8. https://doi.org/10.1097/HJH.0000000000000095.
Fragiotta S, Abdolrahimzadeh S, Dolz-Marco R, Sakurada Y, Gal-Or O, Scuderi G. Significance of hyperreflective foci as an optical coherence tomography biomarker in retinal diseases: characterization and clinical implications. J Ophthalmol. 2021;2021:6096017 https://doi.org/10.1155/2021/6096017.
Huang H, Jansonius NM, Chen H, Los LI. Hyperreflective dots on OCT as a predictor of treatment outcome in diabetic macular edema: a systematic review. Ophthalmol Retin. 2022;6:814–27. https://doi.org/10.1016/j.oret.2022.03.020.
Berasategui B, Fonollosa A, Artaraz J, Ruiz-Arruza I, Ríos J, Matas J, et al. Behavior of hyperreflective foci in non-infectious uveitic macular edema, a 12-month follow-up prospective study. BMC Ophthalmol. 2018;18:179 https://doi.org/10.1186/s12886-018-0848-5.
Puthenparampil M, Torresin T, Franciotta S, Marin A, De Napoli F, Mauceri VA, et al. Hyper-reflecting foci in multiple sclerosis retina associate with macrophage/microglia-derived cytokines in cerebrospinal fluid. Front Immunol. 2022;13:852183 https://doi.org/10.3389/fimmu.2022.852183.
Pilotto E, Miante S, Torresin T, Puthenparampil M, Frizziero L, Federle L, et al. Hyperreflective foci in the retina of active relapse-onset multiple sclerosis. Ophthalmology. 2020;127:1774–6. https://doi.org/10.1016/j.ophtha.2020.03.024.
Schmidt MF, Pihl-Jensen G, Torm MEW, Passali M, Larsen M, Frederiksen JL. Hyperreflective dots in the avascular outer retina in relapsing-remitting multiple sclerosis. Mult Scler Relat Disord. 2023;72:104617 https://doi.org/10.1016/j.msard.2023.104617.
Menean M, Apuzzo A, Mastaglio S, Bernardi M, Ciceri F, Modorati G, et al. Imaging biomarkers of leukaemic choroidopathy. Acta Ophthalmol. 2023;101:553–9. https://doi.org/10.1111/aos.15637.
Author information
Authors and Affiliations
Contributions
Conception or design of the work: DB, SM, AS, GV, FG. Acquisition, analysis, or interpretation of data for the work: DB, SM, AS, GV, FG. Drafting the work or reviewing it critically for important intellectual content: DB, SM, AS, GG, CR, SR, FF, LC, ED, GV, FG. Final approval of the version to be published: DB, SM, AS, GG, CR, SR, FF, LC, ED, GV, FG.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bacherini, D., Mercuri, S., Sodi, A. et al. Inner retinal hyper-reflective foci number correlates with flood-illumination adaptive optics ophthalmoscopy grading and systemic organ involvement in patients with Fabry disease. Eye 39, 1578–1583 (2025). https://doi.org/10.1038/s41433-025-03721-5
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41433-025-03721-5