Abstract
Objectives
The relationship between gastroesophageal reflux disease (GERD) and primary acquired nasolacrimal duct obstruction (PANDO) remains underexplored, and large-scale global studies are lacking. This study aims to evaluate the association between GERD and PANDO on an international scale.
Methods
This retrospective cohort study utilized data from the TriNetX Global Collaborative Network, encompassing over 157 million patients across 18 countries. Patients with GERD and controls without GERD were included from January, 2004, through November, 2024. Patients with pre-existing lacrimal passage disorders were excluded. The primary outcome was the incidence of PANDO. Patients were followed for up to 20 years. Propensity score matching was employed to balance baseline characteristics. Cox proportional hazards regression was used to calculate hazard ratios (HRs), and Kaplan-Meier analysis was conducted to assess the cumulative incidence.
Results
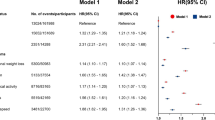
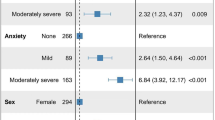
After matching, 876,330 patients were included in both the GERD and control cohorts. GERD was associated with a significantly higher risk of PANDO (HR: 2.49; 95% CI: 2.18–2.85; P < 0.001). Risk stratification analyses demonstrated greater risks in females (HR: 2.74; 95% CI: 2.32–3.24) and in older age groups (HR for ≥60 years: 3.12; 95% CI: 2.59–3.74). Comorbidities such as diabetes, dyslipidaemia, hypertension, ischemic heart disease, chronic kidney disease, and sinusitis further increased the risk of PANDO.
Conclusions
GERD increases the risk of PANDO, particularly in females, older adults, and patients with cardiovascular comorbidities or sinusitis. Clinicians should educate GERD patients about the potential risk of PANDO and arrange referrals when necessary.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The TriNetX platform is a fully deidentified multinational, cloud-based database that adheres to all the relevant adheres to all standards laid out by Section §164,514(b) (1) of the Health Insurance Portability and Accountability Act (HIPPA) as well as ISO 27001:2013. Due to privacy restrictions, data from the TriNetX database is not publicly available. However, the population-level aggregate and deidentified data supporting the findings of this study are openly accessible upon reasonable request to the TriNetX administrators through their website (https://trinetx.com/) or by contacting the TriNetX administrators directly (Privacy@TriNetX.com). Alternatively, the corresponding author may also be contacted (k2001621@gmail.com and b101090109@tmu.edu.tw).
References
Das AV, Rath S, Naik MN, Ali MJ. The incidence of lacrimal drainage disorders across a tertiary eye care network: customization of an indigenously developed electronic medical record system-eyeSmart. Ophthalmic Plast Reconstr Surg. 2019;35:354–6.
Linberg JV, McCormick SA. Primary acquired nasolacrimal duct obstruction. A clinicopathologic report and biopsy technique. Ophthalmology. 1986;93:1055–63.
Ali MJ. Etiopathogenesis of primary acquired nasolacrimal duct obstruction (PANDO). Prog Retin Eye Res. 2023;96:101193.
Ali MJ, Paulsen F. Etiopathogenesis of primary acquired nasolacrimal duct obstruction: what we know and what we need to know. Ophthalmic Plast Reconstr Surg. 2019;35:426–33.
Dent J, El-Serag HB, Wallander MA, Johansson S. Epidemiology of gastro-oesophageal reflux disease: a systematic review. Gut. 2005;54:710–7.
Kahrilas PJ. Clinical practice. Gastroesophageal reflux disease. N Engl J Med. 2008;359:1700–7.
Belafsky PC. Abnormal endoscopic pharyngeal and laryngeal findings attributable to reflux. Am J Med. 2003;115:90S–96S.
DiBaise JK, Olusola BF, Huerter JV, Quigley EM. Role of GERD in chronic resistant sinusitis: a prospective, open label, pilot trial. Am J Gastroenterol. 2002;97:843–50.
Weaver EM. Association between gastroesophageal reflux and sinusitis, otitis media, and laryngeal malignancy: a systematic review of the evidence. Am J Med. 2003;115:81S–89S.
Owji N, Abtahi SM. Does gastroesophageal reflux contribute to development of acquired nasolacrimal duct obstruction? Med Hypotheses. 2010;74:455–6.
Mehta S, Ying GS, Hussain A, Harvey JT. Is gastroesophageal reflux disease associated with primary acquired nasolacrimal duct obstruction? Orbit. 2018;37:135–9.
Owji N, Radaei M, Khademi B. The relationship between primary acquired nasolacrimal duct obstruction and gastroesophageal reflux. Curr Eye Res. 2018;43:1239–43.
Rim TH, Ko J, Kim SS, Yoon JS. Lacrimal drainage obstruction and gastroesophageal reflux disease: a nationwide longitudinal cohort study. J Clin Gastroenterol. 2019;53:277–83.
von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP. The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet. 2007;370:1453–7.
Austin PC. An introduction to propensity score methods for reducing the effects of confounding in observational studies. Multivar Behav Res. 2011;46:399–424.
Austin PC. A comparison of 12 algorithms for matching on the propensity score. Stat Med. 2014;33:1057–69.
Chu YY, Ho CH, Chen YC, Kuo SC. Stroke risk following nonarteritic anterior ischemic optic neuropathy. JAMA Netw Open. 2024;7:e2444534.
Chu YY, Lee CY, Huang WY, Lin JK, Liu CC, Lin HY, et al. Association of atopic dermatitis and risk of glaucoma surgery: a global population-based study. J Glaucoma. 2024;33:735–41.
Haukoos JS, Lewis RJ. The propensity score. JAMA. 2015;314:1637–8.
Janssen AG, Mansour K, Bos JJ, Castelijns JA. Diameter of the bony lacrimal canal: normal values and values related to nasolacrimal duct obstruction: assessment with CT. AJNR Am J Neuroradiol. 2001;22:845–50.
McCormick A, Sloan B. The diameter of the nasolacrimal canal measured by computed tomography: gender and racial differences. Clin Exp Ophthalmol. 2009;37:357–61.
Ali MJ, Schicht M, Paulsen F. Qualitative hormonal profiling of the lacrimal drainage system: potential insights into the etiopathogenesis of primary acquired nasolacrimal duct obstruction. Ophthalmic Plast Reconstr Surg. 2017;33:381–8.
Kashkouli MB, Sadeghipour A, Kaghazkanani R, Bayat A, Pakdel F, Aghai GH. Pathogenesis of primary acquired nasolacrimal duct obstruction. Orbit. 2010;29:11–15.
Chen C, Gong X, Yang X, Shang X, Du Q, Liao Q, et al. The roles of estrogen and estrogen receptors in gastrointestinal disease. Oncol Lett. 2019;18:5673–80.
Kang A, Khokale R, Awolumate OJ, Fayyaz H, Cancarevic I. Is estrogen a curse or a blessing in disguise? role of estrogen in gastroesophageal reflux disease. Cureus. 2020;12:e11180.
Asanuma K, Iijima K, Shimosegawa T. Gender difference in gastro-esophageal reflux diseases. World J Gastroenterol. 2016;22:1800–10.
Kim YS, Kim N, Kim GH. Sex and gender differences in gastroesophageal reflux disease. J Neurogastroenterol Motil. 2016;22:575–88.
Nemet AY, Vinker S. Associated morbidity of nasolacrimal duct obstruction-a large community based case-control study. Graefes Arch Clin Exp Ophthalmol. 2014;252:125–30.
Long AN, Dagogo-Jack S. Comorbidities of diabetes and hypertension: mechanisms and approach to target organ protection. J Clin Hypertens (Greenwich). 2011;13:244–51.
Yen FS, Wei JC, Chiu LT, Hsu CC, Hwu CM. Diabetes, hypertension, and cardiovascular disease development. J Transl Med. 2022;20:9.
Author information
Authors and Affiliations
Contributions
Y-YC and Y-SL had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Conceptualization: Y-YC, Y-SL; Methodology: Y-YC, C-HH, Y-CC, Y-SL; Formal analysis and investigation: Y-YC, C-HH, Y-CC; Writing—original draft preparation: Y-YC, Y-SL; Writing—review and editing: Y-YC, Y-SL, C-HH, Y-CC, S-CK, P-YL.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
This study was approved by the Institutional Review Board of the Chi Mei Medical Center and conducted under the principles of the Declaration of Helsinki (approval number: 11210-E02).
Consent to participate/Consent to publish
The necessity for obtaining informed consent was exempted given that the study was based exclusively on aggregated data and statistical summaries derived from de-identified information.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chu, YY., Ho, CH., Chen, YC. et al. Risk of primary acquired nasolacrimal duct obstruction among gastroesophageal reflux disease patients: a global population-based study. Eye 39, 1817–1824 (2025). https://doi.org/10.1038/s41433-025-03759-5
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41433-025-03759-5