Abstract
Purposes
To explore a new method to improve the diagnostic efficiency of forme fruste keratoconus (FFKC) using the combination of Fourier parameters and corneal epithelial aberrations.
Design
Prospective, case-control analysis.
Methods
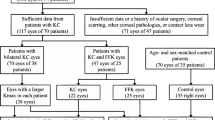
This prospective study enrolled 55 FFKC patients and 68 healthy subjects. The same experienced operator performed Casia 2 (Tomey, Nagoya, Japan) and MS-39 (CSO, Florence, Italy) examinations to obtain Fourier parameters and corneal epithelial aberrations within the central 6 mm of the cornea. Independent-samples T tests were applied to compare statistical differences between the two groups. Significant variables were selected through dual logistic regression analysis with a stepwise method. The areas under the receiver operating characteristic curves (AUROC) were calculated to estimate the diagnostic ability for each parameter and the combined model, and the Youden index was used to determine the cut-off value. Delong test was performed to compare the differences among the AUROC in different conditions.
Results
The spherical component in Fourier parameters of the posterior surface of the cornea (P = 0.002), the asymmetry of the posterior surface of the cornea (P < 0.001), the higher-order irregularity in Fourier parameters at the posterior surface of the cornea (P = 0.026), and corneal epithelial Z (3, ±1) coma (P = 0.035) were selected as explanatory variables. The combined model demonstrated significantly improved diagnostic efficiency with the highest AUROC value of 0.95 (sensitivity, 0.855; specificity, 0.897; cut-off, 0.400). And the AUROC of the combined model was significantly different from that of the single parameter (P < 0.05).
Conclusion
The integration of Fourier parameters and corneal epithelial aberrations holds potential in enhancing the diagnostic efficacy of FFKC, thus serving as a valuable reference for future clinical applications.
This is a preview of subscription content, access via your institution
Access options

Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Santodomingo-Rubido J, Carracedo G, Suzaki A, Villa-Collar C, Vincent S, Wolffsohn J. Keratoconus: an updated review. Contact Lens Anterior Eye. 2022;45:101559.
Wang YM, Chan TCY, Yu M, Jhanji V. Comparison of corneal dynamic and tomographic analysis in normal, forme fruste keratoconic, and keratoconic eyes. J Refract Surg. 2017;33:632–8.
Neuhann L, Vogel D, Hall J, Dreyhaupt J, Werner J, Garip-Kuebler A et al. Keratometry changes between year one to seven after corneal cross-linking in patients with keratoconus. Cornea. 2024;431397–402.
Bevara A, Vaddavalli P. The evolution of diagnostics for keratoconus: from ophthalmometry to biomechanics. Semin Ophthalmol. 2023;38:265–74.
Niazi S, Jiménez-García M, Findl O, Gatzioufas Z, Doroodgar F, Shahriari M et al. Keratoconus diagnosis: from fundamentals to artificial intelligence: a systematic narrative review. Diagnostics. 2023;13:2715.
Randleman J, Zhang H, Asroui L, Tarib I, Dupps W, Scarcelli G. Subclinical keratoconus detection and characterization using motion tracking Brillouin microscopy. Ophthalmology. 2024:131:310–21.
Ambrósio R, Machado A, Leão E, Lyra J, Salomão M, Esporcatte L, et al. Optimized artificial intelligence for enhanced ectasia detection using Scheimpflug-based corneal tomography and biomechanical data. Am J Ophthalmol. 2023;251:126–42.
Chandapura R, Salomão MQ, Ambrósio R, Swarup R, Shetty R, Sinha Roy A. Bowman’s topography for improved detection of early ectasia. J Biophotonics. 2019;12:e201900126.
Reinstein DZ, Gobbe M, Archer TJ, Silverman RH, Coleman DJ. Epithelial, stromal, and total corneal thickness in keratoconus: three-dimensional display with artemis very-high frequency digital ultrasound. J Refract Surg. 2010;26:259–71.
Salomão MQ, Hofling-Lima AL, Gomes Esporcatte LP, Correa FF, Meneses EF, Li Y, et al. Corneal ectasia detection by epithelial pattern standard deviation from OCT. J Cataract Refract Surg. 2023;49:190–4.
Sherwin T, Brookes NH, Loh IP, Poole CA, Clover GM. Cellular incursion into Bowman’s membrane in the peripheral cone of the keratoconic cornea. Exp Eye Res. 2002;74:473–82.
Nan-Ji L, Robert H, Lin W, Ioannis MA, Jia-Qi A, Qin-Mei W, et al. Depicting the epithelium and stroma profiles of post-laser vision correction ectasia by optical coherence tomography. J Cataract Refract Surg. 2025. https://doi.org/10.1097/j.jcrs.0000000000001684. Online ahead of print.
Mocan MC, Yilmaz PT, Irkec M, Orhan M. In vivo confocal microscopy for the evaluation of corneal microstructure in keratoconus. Curr Eye Res. 2008;33:933–9.
Ozgurhan EB, Kara N, Yildirim A, Bozkurt E, Uslu H, Demirok A. Evaluation of corneal microstructure in keratoconus: a confocal microscopy study. Am J Ophthalmol. 2013;156:885–893.e882.
Matalia H, Francis M, Gangil T, Chandapura R, Kurian M, Shetty R, et al. Noncontact quantification of topography of anterior corneal surface and Bowman’s layer with high-speed OCT. J Refract Surg. 2017;33:330–6.
Khamar P, Shetty R, Ahuja P, Chandapura R, Narasimhan R, Nuijts R, et al. Accuracy of OCT curvature and aberrations of Bowman’s layer: a prospective comparison with physical removal of epithelium. J Refract Surg. 2020;36:193–8.
Oie Y, Yasukura Y, Nishida N, Koh S, Kawasaki R, Maeda N, et al. Fourier analysis on regular and irregular astigmatism of anterior and posterior corneal surfaces in fuchs endothelial corneal dystrophy. Am J Ophthalmol. 2021;223:33–41.
Yamamoto R, Ono T, Toyono T, Shirakawa R, Noda M, Yoshida J, et al. Assessment of long-term anterior and posterior topographic changes in the cornea after ptosis surgery using fourier harmonic analysis. Cornea. 2021;40:440–4.
Maeno S, Koh S, Inoue R, Oie Y, Maeda N, Jhanji V, et al. Fourier analysis on irregular corneal astigmatism using optical coherence tomography in various severity stages of keratoconus. Am J Ophthalmol. 2022;243:55–65.
Zhang M, Ji S, Huo Y, Bai S, Tao Z, Zhang J et al. Analyzing the effect of surgical and corneal parameters on the postoperative refractive outcomes of SMILE in myopic eyes based on machine learning. Am J Ophthalmol. 2025;271:455–65.
Rabinowitz YS, Rasheed K. KISA% index: a quantitative videokeratography algorithm embodying minimal topographic criteria for diagnosing keratoconus. J Cataract Refract Surg. 1999;25:1327–35.
Almeida GC Jr, Guido RC, Balarin Silva HM, Brandao CC, de Mattos LC, Lopes BT, et al. New artificial intelligence index based on Scheimpflug corneal tomography to distinguish subclinical keratoconus from healthy corneas. J Cataract Refract Surg. 2022;48:1168–74.
Henriquez MA, Hadid M, Izquierdo L Jr. A systematic review of subclinical keratoconus and forme fruste keratoconus. J Refract Surg. 2020;36:270–9.
Toprak I, Gunes CE. Increased epithelial backscatter: a novel finding in subclinical and clinical keratoconus. Clin Exp Ophthalmol. 2021;49:1000–8.
Oshika T, Tanabe T, Tomidokoro A, Amano S. Progression of keratoconus assessed by fourier analysis of videokeratography data. Ophthalmology. 2002;109:339–42.
Oshika T, Tomidokoro A, Maruo K, Tokunaga T, Miyata N. Quantitative evaluation of irregular astigmatism by fourier series harmonic analysis of videokeratography data. Invest Ophthalmol Vis Sci. 1998;39:705–9.
Shetty R, Narasimhan R, Dadachanji Z, Patel P, Maheshwari S, Chabra A, et al. Early corneal and epithelial remodeling differences identified by OCT imaging and artificial intelligence between two transepithelial PRK platforms. J Refract. 2020;36:678–86.
Elkitkat R, Rifay Y, Gharieb H, Ziada H. Accuracy of the indices of MS-39 anterior segment optical coherence tomography in the diagnosis of keratoconic corneas. Eur J Ophthalmol. 2022;32:2116–24.
Shiga S, Kojima T, Nishida T, Nakamura T, Ichikawa K. Evaluation of CorvisST biomechanical parameters and anterior segment optical coherence tomography for diagnosing forme fruste keratoconus. Acta Ophthalmol. 2021;99:644–51.
DeLong ER, DeLong DM, Clarke-Pearson DL. Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics. 1988;44:837–45.
Ferdi AC, Nguyen V, Gore DM, Allan BD, Rozema JJ, Watson SL. Keratoconus natural progression: a systematic review and meta-analysis of 11 529 eyes. Ophthalmology. 2019;126:935–45.
Ferrari G, Rama P. The keratoconus enigma: a review with emphasis on pathogenesis. Ocul Surf. 2020;18:363–73.
Zhao X, Yuan Y, Sun T, Zhang Y, Chen Y. Associations between keratoconus and the level of sex hormones: a cross-sectional study. Front Med. 2022;9:828233.
Salman A, Kailani O, Marshall J, Ghabra M, Balamoun A, Darwish T, et al. Evaluation of anterior and posterior corneal higher order aberrations for the detection of keratoconus and suspect keratoconus. Tomography. 2022;8:2864–73.
Koh S, Inoue R, Maeno S, Mihashi T, Maeda N, Jhanji V, et al. Characteristics of higher-order aberrations in different stages of keratoconus. Eye Contact Lens. 2022;48:256–60.
Hashemi H, Beiranvand A, Yekta A, Maleki A, Yazdani N, Khabazkhoob M. Pentacam top indices for diagnosing subclinical and definite keratoconus. J Curr Ophthalmol. 2016;28:21–26.
Xu Z, Li W, Jiang J, Zhuang X, Chen W, Peng M, et al. Characteristic of entire corneal topography and tomography for the detection of sub-clinical keratoconus with Zernike polynomials using Pentacam. Sci Rep. 2017;7:16486.
Heidari Z, Mohammadpour M, Hashemi H, Jafarzadehpur E, Moghaddasi A, Yaseri M, et al. Early diagnosis of subclinical keratoconus by wavefront parameters using Scheimpflug, Placido and Hartmann-Shack based devices. Int Ophthalmol. 2020;40:1659–71.
Li Y, Tan O, Brass R, Weiss J, Huang D. Corneal epithelial thickness mapping by Fourier-domain optical coherence tomography in normal and keratoconic eyes. Ophthalmology. 2012;119:2425–33.
Ning R, Wang Y, Xu Z, Gustafsson I, Li J, Savini G, et al. Assessing progression limits in different grades of keratoconus from a novel perspective: precision of measurements of the corneal epithelium. Eye Vis. 2024;11:1.
Temstet C, Sandali O, Bouheraoua N, Hamiche T, Galan A, El Sanharawi M, et al. Corneal epithelial thickness mapping using Fourier-domain optical coherence tomography for detection of form fruste keratoconus. J Cataract Refract Surg. 2015;41:812–20.
Koppen C, Jiménez-García M, Kreps E, Ní Dhubhghaill S, Rozema J. Definitions for keratoconus progression and their impact on clinical practice. Eye & Contact Lens. 2024;50:1–9.
Akincioglu D, Ozge G, Ayyildiz O, Gokce G, Karaca U, Mutlu F. Fourier analysis of corneal Scheimpflug imaging: clinical use in keratoconus. Int J Ophthalmol. 2021;14:1963–9.
Vega-Estrada A, Fariselli C, Alio J. Posterior corneal features in patients with Down syndrome and their relation with keratoconus. Brit J Ophthalmol. 2020;104:1683–9.
Gomes JA, Tan D, Rapuano CJ, Belin MW, Ambrosio R Jr, Guell JL, et al. Global consensus on keratoconus and ectatic diseases. Cornea. 2015;34:359–69.
Pérez-Rueda A, Jiménez-Rodríguez D, Castro-Luna G. Diagnosis of subclinical keratoconus with a combined model of biomechanical and topographic parameters. J Clin Med. 2021;10:2746.
Zhang M, Zhang F, Li Y, Song Y, Wang Z. Early diagnosis of keratoconus in Chinese myopic eyes by combining Corvis ST with Pentacam. Current eye Res. 2020;45:118–23.
Luz A, Lopes B, Hallahan KM, Valbon B, Fontes B, Schor P, et al. Discriminant value of custom ocular response analyzer waveform derivatives in forme fruste keratoconus. Am J Ophthalmol. 2016;164:14–21.
Kirgiz A, Karaman Erdur S, Atalay K, Gurez C. The role of ocular response analyzer in differentiation of forme fruste keratoconus from corneal astigmatism. Eye Contact Lens. 2019;45:83–87.
Gharieb HM, Abdelatif MK, Gharieb HM, Othman IS. Early, forme fruste keratoconus and normal thin cornea, evaluation of sensitive parameters by combined Placido Scheimpflug topography. Eur J Ophthalmol. 2024;34:59–70.
Tian L, Zhang D, Guo L, Qin X, Zhang H, Zhang H, et al. Comparisons of corneal biomechanical and tomographic parameters among thin normal cornea, forme fruste keratoconus, and mild keratoconus. Eye Vis. 2021;8:44.
Kozobolis V, Sideroudi H, Giarmoukakis A, Gkika M, Labiris G. Corneal biomechanical properties and anterior segment parameters in forme fruste keratoconus. Eur J Ophthalmol. 2012;22:920–30.
Naderan M, Jahanrad A, Farjadnia M. Ocular, corneal, and internal aberrations in eyes with keratoconus, forme fruste keratoconus, and healthy eyes. Int Ophthalmol. 2018;38:1565–73.
Thulasidas M, Teotia P. Evaluation of corneal topography and tomography in fellow eyes of unilateral keratoconus patients for early detection of subclinical keratoconus. Indian J Ophthalmol. 2020;68:2415–20.
Zhang H, Tian L, Guo L, Qin X, Zhang D, Li L, et al. Comprehensive evaluation of corneas from normal, forme fruste keratoconus and clinical keratoconus patients using morphological and biomechanical properties. Int Ophthalmol. 2021;41:1247–59.
Scarcelli G, Besner S, Pineda R, Kalout P, Yun SH. In vivo biomechanical mapping of normal and keratoconus corneas. JAMA Ophthalmol. 2015;133:480–2.
Hwang E, Perez-Straziota C, Kim S, Santhiago M, Randleman J. Distinguishing highly asymmetric keratoconus eyes using combined scheimpflug and spectral-domain OCT analysis. Ophthalmology. 2018;125:1862–71.
Ambrósio R, Lopes B, Faria-Correia F, Salomão M, Bühren J, Roberts C, et al. Integration of Scheimpflug-based corneal tomography and biomechanical assessments for enhancing Ectasia detection. J Refract Surg. 2017;33:434–43.
Funding
This work was supported in part by Science and Technology Commission of Shanghai Municipality (Grant No. 22S11900200, 23XD1420500); EYE & ENT Hospital of Fudan University High-level Talents Program (Grant No. 2021318); Program for Professor of Special Appointment (Eastern Scholar, TP2022046) at Shanghai Institutions of Higher Learning; Medical Engineering fund of Fudan University (yg2023-06, yg2023-26). Shanghai Yangpu District Clinical Special Project for Young Researchers (YPQ202407). The funders had no role in study design, data collection and analysis, decision to publish, or reparation of the manuscript. Shanghai Municipal Health Commission Health Industry General Clinical Research Project (No. 202540083).
Author information
Authors and Affiliations
Contributions
Patient data was gathered by RN, YL, JWL, and XNY. RN and YL prepared the main manuscript content. YZY, IG, XTZ and XYW have drafted the work or substantively revised it. JHH and XYW reviewed statistical techniques and provided article ideas. The manuscript was reviewed by all authors.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics
The authors are accountable for all aspects of the work. This includes ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The trial was conducted in accordance with the Declaration of Helsinki. The study was approved by Ethics Committee of the Eye and ENT Hospital of Fudan University (2021174) and informed consent was obtained from all individual participants.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ning, R., Li, Y., li, J. et al. Improving the diagnostic efficiency of forme fruste keratoconus by a new combined model with Fourier parameters and corneal epithelial aberrations. Eye 39, 2945–2951 (2025). https://doi.org/10.1038/s41433-025-03975-z
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41433-025-03975-z