Abstract
Objective
Determine the association between initial treatment method (tap and inject [T/I] or pars plana vitrectomy [PPV]) and microbiology findings on post-treatment visual acuity (VA) in endophthalmitis patients.
Methods
This retrospective study evaluated patients treated for endophthalmitis in Toronto, Canada. The association between treatment, microbiology, and VA at 1-, 3-, 6-, and 12-months post-treatment was analysed using linear regression, adjusted for age, sex, time to treatment, and baseline VA.
Results
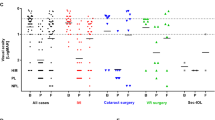
A total of 111 patients were treated with initial T/I (n = 93, 84%) or PPV (n = 18, 16%) between 2011 and 2023. Microbiology identified 69 (62%) culture-negative, 36 (32%) bacterial, and 6 (5%) fungal cases. Adjusted VA improvement did not differ between bacterial and culture-negative groups at all timepoints, including 1 month (–0.68 ± 0.86 vs. –0.69 ± 0.87 logMAR, p = 0.98, n = 102) and last measured follow-up (–1.01 ± 0.90 vs. –0.84 ± 0.83 logMAR, p = 0.35, n = 105). VA improvement also did not differ between T/I and PPV at all timepoints, including at 1 month (–0.66 ± 0.87 vs. –0.50 ± 0.78 logMAR, p = 0.55, n = 108) and last measured follow-up (–0.91 ± 0.86 vs. -0.60 ± 0.80 logMAR, p = 0.20, n = 111). Last measured follow-up time did not differ between T/I and PPV (6.0 vs. 3.8 months, p = 0.05) or between bacterial and culture-negative groups (6.1 vs. 5.6 months, p = 0.85). Retreatment rates were similar between T/I and PPV (35% vs. 33%, OR = 0.95, p = 0.93), but higher in bacterial vs. culture-negative cases (56% vs. 22%, OR = 4.80, p < 0.01).
Conclusions
Visual outcomes did not differ by treatment or microbiology. Bacterial cases had higher retreatment rates than culture-negative cases.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The dataset analysed during the current study is not publicly available due patient privacy but is available from the corresponding author in a deidentified format upon reasonable request.
References
Durand ML. Endophthalmitis. Clin Microbiol Infect. 2013;19:227–34.
Mirzania D, Fleming TL, Robbins CB, Feng HL, Fekrat S. Time to Presentation after Symptom Onset in Endophthalmitis: Clinical Features and Visual Outcomes. Ophthalmol Retin. 2021;5:324–9.
Durand ML. Bacterial and Fungal Endophthalmitis. Clin Microbiol Rev. 2017;30:597–613.
Welch S, Bhikoo R, Wang N, Siemerink MJ, Shew W, Polkinghorne PJ, et al. Better visual outcome associated with early vitrectomy in the management of endophthalmitis. Br J Ophthalmol. 2022;106:1145–9.
Results of the Endophthalmitis Vitrectomy Study: A Randomized Trial of Immediate Vitrectomy and of Intravenous Antibiotics for the Treatment of Postoperative Bacterial Endophthalmitis. Arch Ophthalmol. 1995;113:1479–96.
Mihalache A, Patil NS, Popovic MM, Sedrak P, Kertes PJ, Muni RH. Tap and inject of intravitreal antibiotics versus pars plana vitrectomy for post-cataract surgery endophthalmitis: a meta-analysis. Can J Ophthalmol J Can Ophtalmol. 2024;59:73–8.
Gan IM, van Dissel JT, Beekhuis WH, Swart W, van Meurs JC. Intravitreal vancomycin and gentamicin concentrations in patients with postoperative endophthalmitis. Br J Ophthalmol. 2001;85:1289–93.
Chen KJ, Lai CC, Sun MH, Chen TL, Yang KJ, Kuo YH, et al. Postcataract endophthalmitis caused by Enterococcus faecalis. Ocul Immunol Inflamm. 2009;17:364–9.
Kumar A, Sridhar MS, Dada T, Tewari HK, Gupta SK. Intravitreal pefloxacin therapy in postoperative endophthalmitis. Clin Exp Ophthalmol. 2000;28:38–40.
Torabi H, Tabatabai SA, Khodabande A. Treatment outcomes of post cataract surgery endophthalmitis in a tertiary referral center in Iran. J Curr Ophthalmol. 2018;30:152–5.
Wu PC, Kuo HK, Li M, Lai IC, Fang PC, Lin SA, et al. Nosocomial postoperative endophthalmitis: a 14-year review. Graefes Arch Clin Exp Ophthalmol Albrecht Von Graefes Arch Klin Exp Ophthalmol. 2006;244:920–9.
Krikonis TS, Panagiotoglou TD, Tsika C, Alegakis A, Pallikaris IG, Tsilimbaris MK. Endophthalmitis after cataract extraction: incidence, treatment, and outcome in Crete, Greece, during period 2000-2008. Semin Ophthalmol. 2009;24:234–8.
Far PM, Yeung SC, Farimani PL, Qian J, Zhang AQ, Kertes PJ, et al. TAP AND INJECT VERSUS PARS PLANA VITRECTOMY FOR POSTPROCEDURAL ENDOPHTHALMITIS: A Meta-analysis. Retina Philos Pa. 2021;41:2009–16.
Gokce G, Sobaci G, Ozgonul C. Post-Traumatic Endophthalmitis: A Mini-Review. Semin Ophthalmol. 2015;30:470–4.
Khoshnood B, Mesbah M, Jeanbat V, Lafuma A, Berdeaux G. Transforming scales of measurement of visual acuity at the group level. Ophthalmic Physiol Opt J Br Coll Ophthalmic Opt Optom. 2010;30:816–23.
Maalouf F, Abdulaal M, Hamam RN. Chronic Postoperative Endophthalmitis: A Review of Clinical Characteristics, Microbiology, Treatment Strategies, and Outcomes. Int J Inflamm. 2012;2012:313248.
Crosby NJ, Westcott M, Michael E, Cunningham WJ, Welch S, Polkinghorne PJ. Comparative Outcomes of Primary Vitrectomy Versus Tap and Inject for Endophthalmitis Following Phacoemulsification Cataract Surgery. Ocul Immunol Inflamm. 2022;30:727–33.
Duan F, Wu K, Liao J, Zheng Y, Yuan Z, Tan J, et al. Causative Microorganisms of Infectious Endophthalmitis: A 5-Year Retrospective Study. J Ophthalmol. 2016;2016:6764192.
Shivaramaiah HS, Relhan N, Pathengay A, Mohan N, Flynn HW. Endophthalmitis caused by gram-positive bacteria resistant to vancomycin: Clinical settings, causative organisms, antimicrobial susceptibilities, and treatment outcomes. Am J Ophthalmol Case Rep. 2018;10:211–4.
Haseeb AA, Elhusseiny AM, Siddiqui MZ, Ahmad KT, Sallam AB. Fungal Endophthalmitis: A Comprehensive Review. J Fungi. 2021;7:996.
Miyazaki H, Miyazaki Y, Geber A, Parkinson T, Hitchcock C, Falconer DJ, et al. Fluconazole resistance associated with drug efflux and increased transcription of a drug transporter gene, PDH1, in Candida glabrata. Antimicrob Agents Chemother. 1998;42:1695–701.
Anderson MZ, Saha A, Haseeb A, Bennett RJ. A chromosome 4 trisomy contributes to increased fluconazole resistance in a clinical isolate of Candida albicans. Microbiol Read Engl. 2017;163:856–65.
Callegan MC, Engelbert M, Parke DW, Jett BD, Gilmore MS. Bacterial Endophthalmitis: Epidemiology, Therapeutics, and Bacterium-Host Interactions. Clin Microbiol Rev. 2002;15:111–24.
David DB, Kirkby GR, Noble BA. Bacillus cereus endophthalmitis. Br J Ophthalmol. 1994;78:577–80.
Gao Z, Zhang Y, Gao X, Zhang X, Ma T, Li G, et al. Clinical analysis and predictive factors associated with improved visual acuity of infectious endophthalmitis. BMC Ophthalmol. 2020;20:256.
Study Details | Endophthalmitis Post Intravitreal Injections | ClinicalTrials.gov [Internet]. [cited 2024 Jul 11]. Available from: https://clinicaltrials.gov/study/NCT04035369.
Acknowledgements
Dr. Rajeev H. Muni’s research is supported by the Silber TARGET Fund.
Author information
Authors and Affiliations
Contributions
Shayaan Kaleem, AM, AG, AL, CJ, and Sameen Kaleem were responsible for designing the study, extracting the data, and analysing the data. MMP, PJK, RHM, and DTW were responsible for interpreting results and overseeing the project. All authors contributed to the writing and review of the manuscript and have approved the final version.
Corresponding author
Ethics declarations
Competing interests
MMP: Financial support (to institution) – PSI Foundation, Fighting Blindness Canada. PJK: Honoraria: Novartis, Bayer, Roche, Boehringer Ingelheim, RegenxBio, Apellis; Advisory board – Novartis, Bayer, Roche, Apellis, Novelty Nobility, Viatris, Biogen, AdMare, Kriya Therapeutics; Financial support (to institution) – Roche, Novartis, Bayer, RegenxBio. DTW: Consultant – AbbVie, Alcon, Apellis, Bayer, Bausch Health, Biogen, Boehringer Ingelheim, Novartis, Ripple Therapeutics, Roche, Topcon, Zeiss. Research grants from Novartis, Roche. RHM: Consultant- Alcon,Apellis, AbbVie, Bayer, Bausch Health, Roche; Financial Support (to institution) - Alcon, AbbVie, Bayer, Novartis, Roche.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kaleem, S., Mihalache, A., Golrokhian-Sani, AA. et al. The association between treatment method, microbiological findings, and visual acuity in endophthalmitis patients: A retrospective, multi-centred study. Eye 40, 406–411 (2026). https://doi.org/10.1038/s41433-025-04125-1
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41433-025-04125-1