Abstract
Background and objectives
Ocular trauma is a major cause of blindness. The objectives of this study were to report epidemiology, aetiology, visual outcomes, and interactions with ophthalmology services of paediatric ocular trauma patients.
Methods
A retrospective review of consecutive paediatric ocular trauma presentations between 01 January 2017 and 31 December 2019, within the Belfast Trust. Patients were younger than 16 years old at presentation.
Results
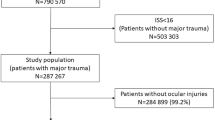
In total, 535 paediatric ocular trauma patients are reported. Epidemiology—Median age was 8.18 years old, with 63.8% of patients being male. Incidence was 0.45 cases per 1000 children aged 0–15, per year. Areas were ranked according to deprivation measures, incidence ranged from 0.43 in the 2nd quintile to 0.64 in the quintile with lowest deprivation measures. Aetiology—Blunt (n = 277, 52%), chemical (n = 96, 18%), sharp (n = 87, 16%), and laser injuries (n = 27, 5%) were the most common mechanisms. There were 2 open globe injuries reported (1.7 per 1,000,000 children aged 0–15, per year). Visual outcomes—Visual acuity at presentation was available for 408 eyes (72%), with 174 (43%) achieving 6/6 or better and 338 (83%) 6/12 or better. 6 eyes (3%) presented with vision worse than 6/60; three improved to better than 6/12 at follow-up, and two remained worse than 6/60. Ophthalmology services—16 patients (3.0%) were admitted.
Conclusions
Paediatric ocular trauma occurs most commonly in males, in the home setting, with a blunt injury mechanism. Chemical and laser eye mechanisms contribute a significant proportion of presentations.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Data availability
The datasets generated and analysed during the current study are not publicly available, but are available from the corresponding author on reasonable scientific request.
References
Li C, Fu Y, Liu S, Yu H, Yang X, Zhang M, Liu L. The global incidence and disability of eye injury: an analysis from the Global Burden of Disease Study 2019. eClinicalMedicine. 2023;62:102134.
Négrel A, Thylefors B. The global impact of eye injuries. Ophthalmic Epidemiol. 1998;5:143–69.
Sii F, Barry RJ, Abbott J, Blanch RJ, MacEwen CJ, Shah P. The UK Paediatric Ocular Trauma Study 2 (POTS2): demographics and mechanisms of injuries. Clin Ophthalmol (Auckl, NZ). 2018;12:105–11.
Kyriakaki EDO, Symvoulakis EK, Chlouverakis G, Detorakis ET. Causes, occupational risk and socio-economic determinants of eye injuries: a literature review. Med Pharm Rep. 2021;94:131–44.
Ahmmed AA, Ting DSJ, Figueiredo FC. Epidemiology, economic and humanistic burdens of Ocular Surface Chemical Injury: A narrative review - PubMed. Ocul Surf. 2021;20:199–211.
Barry Robert J, Sii Freda, Bruynseels Alice, Abbott Joseph, Blanch Richard J, MacEwen Caroline J, et al. The UK Paediatric Ocular Trauma Study 3 (POTS3): clinical features and | OPTH. Clinical Ophthalmol. 2019, 8;13.
Chen V, Pharr C, Junn S, Kraus CL, Fliotsos M, Park HJ, et al. Baltimore pediatric ocular trauma study: Health disparities and outcomes in pediatric and adolescent open globe trauma - PubMed. Injury. 2023;54:533–9.
Mir TA, Canner JK, Zafar Sidra, Srikumaran Divya, Friedman DS, Woreta FA. Characteristics of Open Globe Injuries in the United States From 2006 to 2014. JAMA Ophthalmol. 2020;138:268–75.
Uppuluri S, Uppuluri A, Zarbin MA, Bhagat N. Epidemiology of pediatric open globe injury in the United States - PubMed. J Pediatr Ophthalmol strabismus. 2021;58:232–9.
Cao HE, Li L, Zhang M, Li H. Epidemiology of pediatric ocular trauma in the Chaoshan region, China, 2001–10. PLOS ONE. 2013;8:8.
Snell DT, Lockey PD, Thompson DJ. Socioeconomic status is associated with mechanism and intent of injury in patients presenting to a UK Major Trauma Centre - PubMed. Injury. 2023;54:497–501.
General Comptroller and Auditor. Child Poverty in Northern Ireland. In: Office NIA, editor. 2024.
Kuhn F, Morris R, Witherspoon CD, Mester V. The Birmingham Eye Trauma Terminology system (BETT). PubMed J francais d’ophtalmologie. 2004;27:206–10.
Boret C, Brehin C, Cortey C, Chanut M, Houzé-Cerfon CH, Soler V, et al. Pediatric ocular trauma: Characteristics and outcomes among a French cohort (2007–16) - PubMed. Arch de Pediatr : organe officiel de la Soc francaise de Pediatr. 2020;27:128–34.
Brophy M, Sinclair SA, Hostetler SG, Xiang H. Pediatric eye injury-related hospitalizations in the United States - PubMed. Pediatrics. 2006;117:1263–71.
Matsa E, Shi J, Wheeler KK, McCarthy T, McGregor ML, Leonard JC. Trends in US emergency department visits for pediatric acute ocular injury - PubMed. JAMA Ophthalmol. 2018;136:895–903.
Viswanathan M, Gu W, Blanch RJ, Groves LL. Cataracts after ophthalmic and nonophthalmic trauma exposure in service members, U.S. Armed Forces - PubMed. Mil Med. 2024;189:1009.
Agency Northern Ireland Statistics and Research. 2025 [cited 2025 01 Mat 2025]. Available from: https://www.nisra.gov.uk/.
Low L, Hodson J, Morris D, Desai P, MacEwen C. Socioeconomic deprivation and serious ocular trauma in Scotland: a national prospective study - PubMed. Br J Ophthalmol. 2017;101:1395–8.
Kirkwood BR Sterne JAC. Essential Medical Statistics. 2nd ed. Oxford: Blackwell Science; 2003.
MacEwen CJ, Baines PS, Desai P. Eye injuries in children: the current picture - PubMed. Br J Ophthalmol. 1999;83:933–6.
Strahlman E, Elman M, Daub E. S Baker. Causes of pediatric eye injuries. A population-based study - PubMed. Arch Ophthalmol (Chic, Ill : 1960). 1990;108:603–6.
Karlson TA, Klein BE. The incidence of acute hospital-treated eye injuries - PubMed. Arch Ophthalmol (Chic, Ill : 1960). 1986;104:1473–6.
Canavan YM, O’Flaherty MJ, Archer DB, Elwood JH. A 10-year survey of eye injuries in Northern Ireland, 1967-76. Br J Ophthalmol. 1980;64:618–25.
Hart JT. The inverse care law. Lancet. 1971;297:405–12.
Author information
Authors and Affiliations
Contributions
EML, CS, and MM were involved with study inception and data collection. All authors were involved with methodology. TP, MM, and MA were involved with data analysis, all authors were involved in data interpretation and drafting the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Marshall, M., Anwar, M., Patterson, T. et al. Epidemiology, aetiology and outcomes of paediatric ocular trauma: a population-level study in Northern Ireland. Eye (2026). https://doi.org/10.1038/s41433-026-04406-3
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41433-026-04406-3