Abstract
Aortic root dilatation has been proposed as hypertension-mediated organ damage (HMOD). Nevertheless, the role of the aortic root dilatation as a possible additional HMOD is still unclear since studies conducted so far are quite heterogeneous regarding the type of population analyzed, the aortic tract considered, and the type of outcomes accounted for. The aim of the present study is to assess whether the presence of aortic dilatation is associated with strong cardiovascular (CV) events (MACE: heart failure, CV death, stroke, acute coronary syndrome, myocardial revascularization) in a population of patients affected by essential hypertension. Four hundred forty-five hypertensive patients from six Italian hospitals were recruited as part of ARGO-SIIA study1. For all centers, follow-up was obtained by re-contacting all patients by telephone and through the hospital’s computer system. Aortic dilatation (AAD) was defined through absolute sex-specific thresholds as in previous studies (41 mm for males, 36 mm for females). Median follow-up was 60 months. AAD was found to be associated with the occurrence of MACE (HR = 4.07 [1.81–9.17], p < 0.001). This result was confirmed after correction for main demographic characteristics such as age, sex and BSA (HR = 2.91 [1.18–7.17], p = 0.020). At penalized Cox regression, age, left atrial dilatation, left ventricular hypertrophy and AAD were identified as best predictor of MACEs and AAD resulted a significant predictor of MACEs even after correction for these confounders (HR = 2.43 [1.02–5.78], p = 0.045). The presence of AAD was found to be associated with an increased risk of MACE independently of for major confounders, including established HMODs.

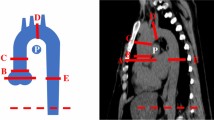
AAD ascending aorta dilatation, LAe left atrial enlargement, LVH left ventricular hypertrophy, MACEs major adverse cardiovascular events, SIIA Società Italiana dell’Ipertensione Arteriosa (Italian Society for Arterial Hypertension).
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Tadic M, Gherbesi E, Sala C, Carugo S, Cuspidi C. Is thoracic aortic diameter an independent predictor of cardiovascular disease and mortality? A narrative review. Front Cardiovasc Med. 2022;9:1–7.
Williams B, Mancia G, Spiering W, Agabiti Rosei E, Azizi M, Burnier M, et al. ESC/ESH guidelines for the management of arterial hypertension. Eur Heart J. 2018;00:1–98.
Volpe M, Battistoni A, Tocci G, Rosei EA, Catapano AL, Coppo R, et al. Cardiovascular risk assessment beyond systemic coronary risk estimation: a role for organ damage markers. J Hypertens. 2012;30:1056–64.
Sehestedt T, Jeppesen J, Hansen TW, Wachtell K, Ibsen H, Torp-petersen C, et al. Risk prediction is improved by adding markers of subclinical organ damage to SCORE. Eur Heart J. 2010;31:883–91.
Lai CL, Chien KL, Hsu HC, Su TC, Chen MF, Lee YT. Aortic root dimension as an independent predictor for all-cause death in adults <65 years of age (from the chin-shan community cardiovascular cohort study). Echocardiography. 2010;27:487–95.
Lam CSP, Gona P, Larson MG, Aragam J, Lee DS, Mitchell GF, et al. Aortic root remodeling and risk of heart failure in the framingham heart study. JACC Heart Fail. 2013;1:79–83.
Cuspidi C, Facchetti R, Bombelli M, Re A, Cairoa M, Sala C, et al. Aortic root diameter and risk of cardiovascular events in a general population: data from the PAMELA study. J Hypertens. 2014;32:1879–87.
Canciello G, Mancusi C, Losi MA, Izzo R, Trimarco B, de Simone G, et al. Aortic root dilatation is associated with incident cardiovascular events in a population of treated hypertensive patients: the Campania Salute Network. Am J Hypertens. 2018; 31:1317–23.
Qazi S, Massaro JM, Chuang ML, D’Agostino RB, Hoffmann U, O’Donnell CJ. Increased aortic diameters on multidetector computed tomographic scan are independent predictors of incident adverse cardiovascular events: the Framingham Heart Study. Circ Cardiovasc Imaging. 2017;10:1–8.
Gondrie MJA, Van Der Graaf Y, Jacobs PC, Buckens SCFM, Mali WPTM. The prognostic value of vascular diameter measurements on routine chest computed tomography in patients not referred for cardiovascular indications. J Comput Assist Tomogr. 2011;35:734–41.
Leone D, Airale L, Bernardi S, Mingrone G, Astarita A, Cesareo M, et al. Prognostic role of the ascending aorta dilatation in patients with arterial hypertension. J Hypertens. 2021;38:1–7.
Mancia G, Fagard R, Narkiewicz K, Redon J, Zanchetti A, Böhm M, et al. ESH/ESC guidelines for the management of arterial hypertension: the Task Force for the management of arterial hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). Eur Heart J. 2013;34:2159–219.
Lang RM, Badano LP, Mor-Avi V, Afilalo J, Armstrong A, Ernande L, et al. Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Eur Heart J Cardiovasc Imaging. 2015;16:233–71.
Patel HN, Miyoshi T, Addetia K, Citro R, Daimon M, Gutierrez Fajardo P, et al. Normal values of aortic root size according to age, sex, and race: results of the World Alliance of Societies of Echocardiography Study. J Am Soc Echocardiogr. 2021;35:267–74.
Milan A, Degli Esposti D, Salvetti M, Izzo R, Moreo A, Pucci G, et al. Prevalence of proximal ascending aorta and target organ damage in hypertensive patients: the multicentric ARGO-SIIA project (Aortic RemodellinG in hypertensiOn ofthe Italian Society ofHypertension). J Hypertens. 2019;37:57–64.
Cameli M, Lembo M, Sciaccaluga C, Bandera F, Ciccone MM, D Andrea A, et al. Identification of cardiac organ damage in arterial hypertension: insights by echocardiography for a comprehensive assessment. J Hypertens. 2020;38:588–98.
Vriz O, Driussi C, Bettio M, Ferrara F, D’Andrea A, Bossone E. Aortic root dimensions and stiffness in healthy subjects. Am J Cardiol. 2013;112:1224–9.
Lam CSP, Xanthakis V, Sullivan LM, Lieb W, Aragam J, Redfield MM, et al. Aortic root remodeling over the adult life course: longitudinal data from the framingham heart study. Circulation. 2010;122:884–90.
Covella M, Milan A, Totaro S, Cuspidi C, Re A, Rabbia F, et al. Echocardiographic aortic root dilatation in hypertensive patients: a systematic review and meta-analysis. J Hypertens. 2014;32:1928–35.
Tosello F, Leone D, Laurent S, Veglio F, Milan A. Out of proportion proximal aortic remodeling: a subclinical marker of early vascular ageing? A systematic review. Int J Cardiol. 2016;223:999–1006.
O’Rourke MF, Nichols WW. Aortic diameter, aortic stiffness, and wave reflection increase with age and isolated systolic hypertension. Hypertension. 2005;45:652–8.
Azadani AN, Chitsaz S, Matthews PB, Jaussaud N, Leung J, Tsinman T, et al. Comparison of mechanical properties of human ascending aorta and aortic sinuses. Ann Thorac Surg. 2012;93:87–94.
Devereux RB, de Simone G, Arnett DK, Best LG, Boerwinkle E, Howard BV, et al. Normal limits in relation to age, body size and gender of two-dimensional echocardiographic aortic root dimensions in persons ≥15 years of age. Am J Cardiol. 2012;110:1189–94.
Biaggi P, Matthews F, Braun J, Rousson V, Kaufmann PA, Jenni R. Gender, age, and body surface area are the major determinants of ascending aorta dimensions in subjects with apparently normal echocardiograms. J Am Soc Echocardiogr. 2009;22:720–5.
SCORE2 Working Group and ESC Cardiovascular Risk Collaboration. SCORE2 risk prediction algorithms: new models to estimate 10-year risk of cardiovascular disease in Europe. Eur Heart J. 2021;42:2439–54.
Acknowledgements
The authors thank all the centers that participated in the study. We would like to thank Prof. Maria Lorenza Muiesan, Prof. Daniela Degli Esposti, Cristina Giannattasio and Prof. Nicola De Luca who supervised the study, Deborah Stassaldi and Sara Cappellini who helped in the collection of data.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Airale, L., Borrelli, F., Arrivi, A. et al. Ascending aorta dilatation is associated to hard cardiovascular events, follow-up from multicentric ARGO-Perspective project. Hypertens Res 46, 2016–2023 (2023). https://doi.org/10.1038/s41440-023-01340-9
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41440-023-01340-9
Keywords
This article is cited by
-
Aortic dilatation and cardiovascular events: a new piece of the puzzle?
Hypertension Research (2023)