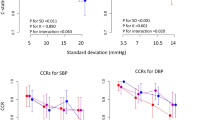
Abstract
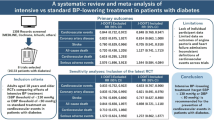
Home blood pressure (HBP) monitoring is a better prognostic predictor than clinical BP monitoring. However, the suggested number of HBP measurements in each occasion varies across guidelines. The study aimed to identify which HBP measurements in each occasion are more closely associated with new cardiovascular events in patients with type 2 diabetes. This retrospective cohort study included 1058 patients with type 2 diabetes without a history of macrovascular complications. HBP was measured three times each morning and evening for 14 days, and the average value over the 14 days was calculated. During a median follow-up of 7.0 years, 117 patients (11.1%) had cardiovascular events. The Cox proportional hazards model was used to examine the association between the average morning home systolic BP (MHSBP) for the 1st, 2nd, and 3rd measurements and cardiovascular events. The adjusted hazard ratios (HR) (95% confidence interval) for the onset of cardiovascular events in the 2nd and 3rd mean MHSBP were 1.129 (1.008–1.265) and 1.135 (1.010–1.275), respectively. The area under the receiver-operating characteristic curve (AUC) for the 2nd, 1st/2nd, 2nd/3rd, and 1st/2nd/3rd mean MHSBP was significantly greater than that of the 1st mean MHSBP (p = 0.040, p = 0.014, p = 0.020, and p = 0.021, respectively). No significant difference was observed between the AUC of the 2nd/3rd and 1st/2nd/3rd mean MHSBP and that of the 1st/2nd mean MHSBP. We recommend that HBP measurements be taken just twice per occasion to predict cardiovascular events in patients with type 2 diabetes.

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Change history
13 November 2025
“The original online version of this article was revised: In the sentences beginning ‘This retrospective cohort study...’ and ‘This study shows that,...’ in this article, the value ‘1082’ have been updated to ‘1058’.”.
19 November 2025
A Correction to this paper has been published: https://doi.org/10.1038/s41440-025-02469-5
References
Aliño-Dies M, Sánchez-Ortí JV, Correa-Ghisays P, Balanzá-Martínez V, Vila-Francés J, Selva-Vera G, et al. Grip strength, neurocognition, and social functioning in people with type-2 diabetes mellitus, major depressive disorder, bipolar disorder, and schizophrenia. Front Psychol. 2020;11:525231.
Baskar V, Kamalakannan D, Holland MR, Singh BM. Does ethnic origin have an independent impact on hypertension and diabetic complications? Diabetes Obes Metab. 2006;28:214–19.
Shimbo D, Artinian NT, Basile JN, Krakoff LR, Margolis KL, Rakotz MK, et al. Self-measured blood pressure monitoring at home circulation. Circulation. 2020;142:42–63.
Stergiou GS, Argyraki KK, Moyssakis I, Mastorantonakis SE, Achimastos AD, Karamanos VG, et al. Home blood pressure is as reliable as ambulatory blood pressure in predicting target-organ damage in hypertension. Am J Hypertens. 2007;20:616–21.
Kario K, Saito I, Kushiro T, Teramukai S, Ishikawa Y, Mori Y, et al. Home blood pressure and cardiovascular outcomes in patients during antihypertensive therapy primary results of HONEST, a large-scale prospective, real-world observational study. Hypertension. 2014;64:989–96.
Elsayed NA, Aleppo G, Aroda VR, Bannuru RR, Brown FM, Bruemmer D, et al. 2. Classification and diagnosis of diabetes: Standards of care in diabetes-2023. Diabetes Care. 2023;46:S19–40.
Coleman A, Freeman P, Steel S, Shennan A. Validation of the Omron 705IT (HEM-759-E) oscillometric blood pressure monitoring device according to the British Hypertension Society protocol. Blood Press Monit. 2006;11:27–32.
Imai Y, Kario K, Shimada K, Kawano Y, Hasebe N, Matsuura H, et al. Japanese Society of Hypertension Committee for Guidelines for Self-monitoring of Blood Pressure at Home. The Japanese Society of Hypertension guidelines for self-monitoring of blood pressure at home (Second edition). Hypertens Res. 2012;35:777–95.
Sogunuru GP, Kario K, Shin J, Chen C-H, Buranakitjaroen P, Chia YC, et al. Morning surge in blood pressure and blood pressure variability in Asia: Evidence and statement from the HOPE Asia Network. J Clin Hypertens. 2019;21:324–34.
Zain-El Abdin MH, Snincak M, Pahuli K, Solarova Z, Hrabcakova P. Non-dipping morning blood pressure and isolated systolic hypertension in elderly. Bratisl Lek Listy. 2013;114:150–4.
Bonten TN, Snoep JD, Assendelft WJJ, Zwaginga JJ, Eikenboom J, Huisman MV, et al. Time-dependent effects of aspirin on blood pressure and morning platelet reactivity: A randomized cross-over trial. Hypertension. 2015;65:743–50.
Thosar SS, Butler MP, Shea SA. Role of the circadian system in cardiovascular disease. J Clin Invest. 2018;128:2157–67.
Kamoi K, Ito T, Miyakoshi M, Minagawa S. Usefulness of home blood pressure measurement in the morning in patients with Type 2 diabetes: long-term results of a prospective longitudinal study. Clin Exp Hypertens. 2010;32:184–92.
Uzu T. Salt and hypertension in diabetes. Diabetol Int. 2017;8:154–9.
Friedman O, Logan AG. Can nocturnal hypertension predict cardiovascular risk? Integr Blood Press Control. 2009;2:22–37.
Ishikawa J, Kario K, Hoshide S, Eguchi K, Morinari M, Kaneda R, et al. Determinants of exaggerated difference in morning and evening blood pressure measured by self-measured blood pressure monitoring in medicated hypertensive patients: Jichi Morning Hypertension Research (J-MORE) Study. Am J Hypertens. 2005;18:958–65.
Kawabe H, Saito I, Saruta T. Status of home blood pressure measured in morning and evening: Evaluation in normotensives and hypertensives in Japanese urban population. Hypertens Res. 2005;28:491–8.
Fujiwara T, Hoshide S, Kanegae H, Nishizawa M, Kario K. Reliability of morning, before-dinner, and at-bedtime home blood pressure measurements in patients with hypertension. J Clin Hypertens. 2018;20:315–23.
Turana Y, Tengkawan J, Chia YC, Nathaniel M, Wang J-G, Sukonthasarn A, et al. Hypertension and stroke in Asia: A comprehensive review from HOPE Asia. J Clin Hypertens. 2021;23:513–21.
Eastwood SV, Tillin T, Chaturvedi N, Hughes AD. Baseline and follow-up measurements ethnic differences in associations between blood pressure and stroke in South Asian and European men epidemiology/population. Hypertension. 2015;66:481–8.
Mancia G, Kreutz R, Brunström M, Burnier M, Grassi G, Januszewicz A, et al. 2023 ESH Guidelines for the management of arterial hypertension the Task Force for the management of arterial hypertension of the European Society of Hypertension: Endorsed by the International Society of Hypertension (ISH) and the European Renal Association (ERA). J Hypertens. 2023;41:1874–2071.
Umemura S, Arima H, Arima S, Asayama K, Dohi Y, Hirooka Y, et al. The Japanese Society of Hypertension Guidelines for the Management of Hypertension (JSH 2019). Hypertens Res. 2019;42:1235–481.
Niiranen TJ, Johansson JK, Reunanen A, Jula AM. Optimal schedule for home blood pressure measurement based on prognostic data: the Finn-Home Study. Hypertension. 2011;57:1081–6.
Parati G, Faini A, Valentini M. Blood pressure variability: its measurement and significance in hypertension. Curr Hypertens Rep. 2006;8:199–204.
Acknowledgements
The authors express their gratitude to Dr. Yoshihiro Kitagawa and Dr. Shinichi Mogami of Osaka General Hospital, West Japan Railway Company, as well as Dr. Atsushi Omoto and Dr. Wataru Fukuda of Kyoto First Red Cross Hospital, for their support with data collection. We also extend our thanks to Terumi Kaneko, Naoko Higo, and Machiko Hasegawa of Kyoto Prefectural University of Medicine for their guidance to patients on HBP measurement and to Sayoko Tanaka, also from Kyoto Prefectural University of Medicine, for her administrative assistance. We extend our gratitude to Editage (www.editage.com) for their invaluable assistance in editing the English language content.
Funding
Emi Ushigome received grant support from the Japanese Study Group for Physiology and Management of Blood Pressure and the Astellas Foundation for Research on Metabolic Disorders (Grant number: 4024).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
“The original online version of this article was revised: In the sentences beginning ‘This retrospective cohort study...’ and ‘This study shows that,...’ in this article, the value ‘1082’ have been updated to ‘1058’.”.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sumi, M., Ushigome, E., Kitagawa, N. et al. Second home blood pressure measurements per occasion predict incident cardiovascular events in type 2 diabetes: KAMOGAWA-HBP study. Hypertens Res 48, 950–958 (2025). https://doi.org/10.1038/s41440-024-02049-z
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41440-024-02049-z
Keywords
This article is cited by
-
Comment to “Comment on: Second home blood pressure measurements per occasion predict incident cardiovascular events in type 2 diabetes: KAMOGAWA-HBP study”
Hypertension Research (2025)
-
Comment on: Second home blood pressure measurements per occasion predict incident cardiovascular events in type 2 diabetes: KAMOGAWA-HBP study
Hypertension Research (2025)
-
Is it possible to establish a doctor-patient relationship in the future where type 2 diabetes patients voluntarily measure their blood pressure twice in the early morning?
Hypertension Research (2025)