Abstract
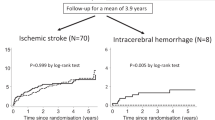
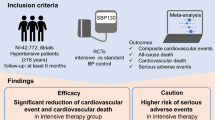
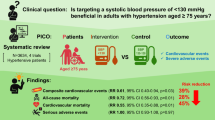
In this systematic review of randomized controlled trials, we examined the optimal blood pressure (BP) target for patients with prior stroke, comparing intensive BP control (systolic BP [SBP] <130 mmHg) with standard BP control (SBP < 140 mmHg). Literature searches of PubMed/MEDLINE, the Cochrane Database, and Ichu-shi identified seven randomized controlled trials for quantitative analysis. Meta-analyses were performed using random-effects models, with most included trials assessed as having low risks of bias. The meta-analysis showed significant reductions in recurrent stroke (risk ratio [RR], 0.79; 95% confidence interval [CI], 0.65–0.96) and major cardiovascular events (RR, 0.86; 95% CI, 0.76–0.97) in the intensive BP control arm. Intensive BP control was more effective in reducing recurrent hemorrhagic stroke (RR, 0.33; 95% CI, 0.15–0.74) than ischemic stroke (RR, 0.87; 95% CI, 0.71–1.08). However, adverse events such as syncope or dizziness were significantly more frequent in the intensive BP control arm (RR, 1.30; 95% CI, 1.00–1.68). Absolute risk reductions (per 1,000 persons) for recurrent stroke (−14; 95% CI, −24 to −4) and major cardiovascular events (−17; 95% CI, −28 to −6) outweighed the absolute increase in syncope or dizziness (4; 95% CI, 0–9). We recommend a lower SBP target of <130 mmHg, with careful monitoring for hypotension-related symptoms, to prevent recurrent stroke and major cardiovascular events in patients with prior stroke.

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Ferrari AJ, Santomauro DF, Aali A, Abate YH, Abbafati C, Abbastabar H, et al. Global incidence, prevalence, years lived with disability (YLDs), disability-adjusted life-years (DALYs), and healthy life expectancy (HALE) for 371 diseases and injuries in 204 countries and territories and 811 subnational locations, 1990–2021: a systematic analysis for the Global Burden of Disease Study 2021. Lancet. 2024;403:2133–61.
Feigin VL, Abate MD, Abate YH, Abd ElHafeez S, Abd-Allah F, Abdelalim A, et al. Global, regional, and national burden of stroke and its risk factors, 1990–2021: a systematic analysis for the Global Burden of Disease Study 2021. Lancet Neurol. 2024;23:973–1003.
Mohan KM, Wolfe CDA, Rudd AG, Heuschmann PU, Kolominsky-Rabas PL, Grieve AP. Risk and cumulative risk of stroke recurrence: A systematic review and meta-analysis. Stroke. 2011;42:1489–94.
MacMahon S, Neal B, Tzourio C, Rodgers A, Woodward M, Cutler J, et al. Randomised trial of a perindopril-based blood-pressure-lowering regimen among 6105 individuals with previous stroke or transient ischaemic attack. Lancet. 2001;358:1033–41.
Hardie K, Hankey GJ, Jamrozik K, Broadhurst RJ, Anderson C. Ten-year risk of first recurrent stroke and disability after first-ever stroke in the perth community stroke study. Stroke. 2004;35:731–5.
Koton S, Pike JR, Johansen M, Knopman DS, Lakshminarayan K, Mosley T, et al. Association of Ischemic Stroke Incidence, Severity, and Recurrence with Dementia in the Atherosclerosis Risk in Communities Cohort Study. JAMA Neurol. 2022;79:271–80.
Friday G, Alter M, Lai SM. Control of hypertension and risk of stroke recurrence. Stroke. 2002;33:2652–7.
Hankey GJ, Warlow CP. Treatment and secondary prevention of stroke: evidence, costs, and effects on individuals and populations. LANCET. 1999;354:1457–63.
Lawes CMM, Bennett DA, Feigin VL, Rodgers A. Blood pressure and stroke: an overview of published reviews. Stroke. 2004;35:776–85.
O’Donnell MJ, Denis X, Liu L, Zhang H, Chin SL, Rao-Melacini P, et al. Risk factors for ischaemic and intracerebral haemorrhagic stroke in 22 countries (the INTERSTROKE study): a case-control study. Lancet. 2010;376:112–23.
Zonneveld TP, Richard E, Vergouwen MDI, Nederkoorn PJ, de Haan R, Roos YB, et al. Blood pressure-lowering treatment for preventing recurrent stroke, major vascular events, and dementia in patients with a history of stroke or transient ischaemic attack. Cochrane Database of Systematic Reviews. John Wiley and Sons Ltd; 2018.
SPS3 Study Group, Benavente OR, Coffey CS, Conwit R, Hart RG, McClure LA, et al. Blood-pressure targets in patients with recent lacunar stroke: The SPS3 randomised trial. Lancet. 2013;382:507–15.
Kitagawa K, Yamamoto Y, Arima H, Maeda T, Sunami N, Kanzawa T, et al. Effect of Standard vs Intensive Blood Pressure Control on the Risk of Recurrent Stroke: A Randomized Clinical Trial and Meta-analysis. JAMA Neurol. 2019;76:1309–18.
Miyamoto S, Ogasawara K, Kuroda S, Itabashi R, Toyoda K, Itoh Y, et al. Japan stroke society guideline 2021 for the treatment of stroke. Int J Stroke. 2022;17:1039–49.
Kleindorfer DO, Towfighi A, Chaturvedi S, Cockroft KM, Gutierrez J, Lombardi-Hill D, et al. 2021 Guideline for the prevention of stroke in patients with stroke and transient ischemic attack: A Guideline From the American Heart Association/American Stroke Association. Stroke Wolters Kluwer Health. 2021;52:E364–467.
Dawson J, Béjot Y, Christensen LM, De Marchis GM, Dichgans M, Hagberg G, et al. European Stroke Organisation (ESO) guideline on pharmacological interventions for long-term secondary prevention after ischaemic stroke or transient ischaemic attack. Eur Stroke J. 2022;7:I–II.
Birns J, Markus H, Kalra L. Blood pressure reduction for vascular risk: Is there a price to be paid? Stroke. 2005;36:1308–13.
The SPRINT Research Group. A Randomized Trial of Intensive versus Standard Blood-Pressure Control. New England Journal Medicine. 2015;373:2103–16.
STATA META-ANALYSIS REFERENCE MANUAL RELEASE 18 [Internet]. Available from: www.stata.com
Park JM, Kim BJ, Kwon SU, Hwang YH, Heo SH, Rha JH, et al. Intensive blood pressure controlmay not be safe in subacute ischemic stroke by intracranial atherosclerosis: A result of randomized trial. J Hypertens. 2018;36:1936–41.
Liu J, Li Y, Ge J, Yan X, Zhang H, Zheng X, et al. Lowering systolic blood pressure to less than 120 mm Hg versus less than 140 mm Hg in patients with high cardiovascular risk with and without diabetes or previous stroke: an open-label, blinded-outcome, randomised trial. Lancet. 2024;404:245–55.
Bath PM, Scutt P, Blackburn DJ, Ankolekar S, Krishnan K, Ballard C, et al. Intensive versus guideline blood pressure and lipid lowering in patients with previous stroke: main results from the pilot prevention of decline in cognition after Stroke trial’ (PODCAST) randomised controlled trial. PLoS ONE. 2017;12:e0164608.
Mant J, McManus RJ, Roalfe A, Fletcher K, Taylor CJ, Martin U, et al. Different systolic blood pressure targets for people with history of stroke or transient ischaemic attack: PAST-BP (Prevention after Stroke-Blood Pressure) randomised controlled trial. BMJ (Online). 2016;352:i708.
Markus HS, Egle M, Croall ID, Sari H, Khan U, Hassan A, et al. PRESERVE: randomized trial of intensive versus standard blood pressure control in small vessel disease. Stroke. 2021;52:2484–93.
Irie K, Yamaguchi T, Minematsu K, Omae T. The J-curve phenomenon in stroke recurrence. Stroke. 1993;24:1844–9.
Dolui S, Detre JA, Gaussoin SA, Herrick JS, Wang DJJ, Tamura MK, et al. Association of Intensive vs Standard Blood Pressure Control With Cerebral Blood Flow Secondary Analysis of the SPRINT MIND Randomized Clinical Trial. JAMA Neurol Am Med Assoc. 2022;79:380–9.
Suzuki K, Izumi M. The incidence of hemorrhagic stroke in Japan is twice compared with western countries: the Akita stroke registry. Neurol Sci. 2015;36:155–60.
Ueshima H, Sekikawa A, Miura K, Turin TC, Takashima N, Kita Y, et al. Cardiovascular disease and risk factors in Asia: A selected review. Circulation. 2008;118:2702–9.
Huang WY, Saver JL, Wu YL, Lin CJ, Lee M, Ovbiagele B. Frequency of intracranial hemorrhage with low-dose aspirin in individuals without symptomatic cardiovascular disease: a systematic review and meta-analysis. JAMA Neurol Am Med Assoc. 2019;76:906–14.
Shen AYJ, Yao JF, Brar SS, Jorgensen MB, Chen W. Racial/ethnic differences in the risk of intracranial hemorrhage among patients with atrial fibrillation. J Am Coll Cardiol. 2007;50:309–15.
Kitagawa K, Arima H, Yamamoto Y, Ueda S, Rakugi H, Kohro T, et al. Intensive or standard blood pressure control in patients with a history of ischemic stroke: RESPECT post hoc analysis. Hypertens Res. 2022;45:591–601.
Rothwell PM, Howard SC, Spence JD. Relationship between blood pressure and stroke risk in patients with symptomatic carotid occlusive disease. Stroke. 2003;34:2583–90.
Sink KM, Evans GW, Shorr RI, Bates JT, Berlowitz D, Conroy MB, et al. Syncope, hypotension, and falls in the treatment of hypertension: results from the randomized clinical systolic blood pressure intervention trial. J Am Geriatr Soc. 2018;66:679–86.
Rocco MV, Sink KM, Lovato LC, Wolfgram DF, Wiegmann TB, Wall BM, et al. Effects of Intensive Blood Pressure Treatment on Acute Kidney Injury Events in the Systolic Blood Pressure Intervention Trial (SPRINT). Am J Kidney Dis. 2018;71:352–61.
Benetos A, Rossignol P, Cherubini A, Joly L, Grodzicki T, Rajkumar C, et al. Polypharmacy in the aging patient: management of hypertension in octogenarians. JAMA. 2015;314:170–80.
Benetos A, Petrovic M, Strandberg T. Hypertension management in older and frail older patients. Circ Res. 2019;124:1045–60.
Cheung AK, Chang TI, Cushman WC, Furth SL, Hou FF, Ix JH, et al. KDIGO 2021 Clinical Practice Guideline for the Management of Blood Pressure in Chronic Kidney Disease. Kidney Int. 2021;99:S1–87.
Toyoda K, Inoue M, Koga M. Small but steady steps in stroke medicine in Japan. J Am Heart Assoc. 2019;8:e013306.
Murad MH, Wang Z, Zhu Y, Saadi S, Chu H, Lin L. Methods for deriving risk difference (absolute risk reduction) from a meta-analysis. BMJ. 2023;381:e073141.
Acknowledgements
This study is a report of the Japanese Society of Hypertension Task Force on the Guidelines for Management of Hypertension 2025 (JSH2025). TM and SI contributed to developing the search strategy and conducting the searches. TM, YO, SI, YI, TF, YS, NO, and TN participated in the initial and full-text screenings. TM, SI, and YI were responsible for extracting relevant results and evaluating the risk of bias. HA, KT, HK, and MK supervised the study and provided valuable feedback. TM drafted the initial manuscript, and all authors critically revised subsequent drafts to ensure inclusion of crucial intellectual content. All authors approved the final version of the manuscript for publication. We thank Angela Morben, DVM, ELS, from Edanz (https://jp.edanz.com/ac) for editing a draft of this manuscript.
Funding
This work was supported by JSPS KAKENHI Grant Number JP21K17317.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There is no conflict of interest regarding this study.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Maeda, T., Ohya, Y., Ishida, S. et al. Optimal blood pressure target for patients with prior stroke: A systematic review and meta-analysis. Hypertens Res 48, 1859–1869 (2025). https://doi.org/10.1038/s41440-025-02183-2
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41440-025-02183-2
Keywords
This article is cited by
-
Blood pressure management in stroke: comparative review of the 2025 AHA/ACC/AANP/ACPM/AGS/AMA/ASPC/NMA/PCNA/SGIM, 2024 ESC, 2023 ESH, and 2025 JSH guidelines
Hypertension Research (2026)
-
The conservative–challenging paradigm of antihypertensive therapy in JSH2025: a comparative perspective with contemporary Western guidelines
Hypertension Research (2026)
-
Advancing evidence-based blood pressure targets in JSH2025
Hypertension Research (2026)
-
The Japanese Society of Hypertension Guidelines for the management of elevated blood pressure and hypertension 2025 (JSH2025)
Hypertension Research (2026)
-
Comment on: Optimal blood pressure target for patients with prior stroke: a systematic review and meta-analysis
Hypertension Research (2025)