Abstract
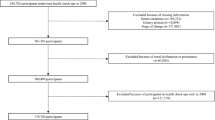
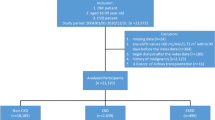
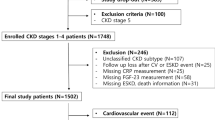
Exercise is well known to reduce the risk of cardiovascular diseases and mortality. However, studies in individuals with chronic kidney disease (CKD) are limited. This study used large population-based data to investigate the differences in the impact of exercise habits on all-cause and cardiovascular mortality between individuals with and without CKD. This study included participants from the Japan Specific Health Checkups (J-SHC) Study conducted between 2008 and 2014. The exposure of interest was self-reported daily exercise habits. The association between exercise habits and all-cause and cardiovascular mortality was examined using Cox regression analysis based on the CKD status. Of the 469,466 participants, 84,508 (18.0%) had CKD, and 39,343 (46.6%) exercised. During the median follow-up period of 44.0 months, 3932 (2.76/1000 person-years) and 1505 (5.09/1000 person-years) participants died in the non-CKD and CKD cohorts, respectively. Exercise habits were associated with a lower risk of all-cause mortality in the non-CKD and CKD cohorts, with adjusted hazard ratios and 95% confidence intervals of 0.80 (0.75–0.86) and 0.70 (0.63–0.78), respectively. The effect of exercise habits on mortality was greater in the CKD group (P for interaction = 0.02). Similar results were observed for cardiovascular mortality. Regular exercise was more strongly associated with decreased all-cause and cardiovascular mortality in individuals with CKD than in those without. Our study highlights the need for individuals with mild CKD to prioritize exercise habits over those without CKD.

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Go AS, Chertow GM, Fan D, McCulloch CE, Hsu CY. Chronic kidney disease and the risks of death, cardiovascular events, and hospitalization. N Eng J Med. 2004;351:1296–305.
Sarnak MJ. Cardiovascular complications in chronic kidney disease. Am J Kidney Dis. 2003;41:11–7.
Paffenbarger RS Jr, Hyde RT, Wing AL, Hsieh CC. Physical activity, all-cause mortality, and longevity of college alumni. N Engl J Med. 1986;314:605–13.
Lee IM, Skerrett PJ. Physical activity and all-cause mortality: what is the dose-response relation?. Med Sci Sports Exerc. 2001;33:S459–71. discussion S93-4.
Heiwe S, Jacobson SH. Exercise training in adults with CKD: a systematic review and meta-analysis. Am J Kidney Dis. 2014;64:383–93.
Johansen KL, Painter P. Exercise in individuals with CKD. Am J Kidney Dis. 2012;59:126–34.
Roshanravan B, Robinson-Cohen C, Patel KV, Ayers E, Littman AJ, de Boer IH, et al. Association between physical performance and all-cause mortality in CKD. J Am Soc Nephrol. 2013;24:822–30.
Andrassy KM. Comments on ‘KDIGO 2012 clinical practice guideline for the evaluation and management of chronic kidney disease. Kidney Int. 2013;84:622–3.
Tsuruya K, Yoshida H, Nagata M, Kitazono T, Hirakata H, Iseki K, et al. Association of the triglycerides to high-density lipoprotein cholesterol ratio with the risk of chronic kidney disease: analysis in a large Japanese population. Atherosclerosis. 2014;233:260–7.
Matsuo S, Imai E, Horio M, Yasuda Y, Tomita K, Nitta K, et al. Revised equations for estimated GFR from serum creatinine in Japan. Am J Kidney Dis. 2009;53:982–92.
Otaki Y, Watanabe T, Konta T, Watanabe M, Fujimoto S, Sato Y, et al. One-Year Change in Diastolic Blood Pressure and Aortic Disease-Related Mortality in a Japanese General Population Aged 50-75 Years. Circ J. 2021;85:2222–31.
Knol MJ, VanderWeele TJ, Groenwold RH, Klungel OH, Rovers MM, Grobbee DE. Estimating measures of interaction on an additive scale for preventive exposures. Eur J Epidemiol. 2011;26:433–8.
Hallan SI, Ovrehus MA, Shlipak MG, Potok OA, Romundstad S, Aspvik NP, et al. Long-term physical exercise for preventing CKD in older adults: a randomized controlled trial. J Am Soc Nephrol. 2025(e-pub ahead of print 2025/02/11;https://doi.org/10.1681/ASN.0000000636).
Peng W, Han M, Xu G. Gender differences in the association between physical activity and mortality in chronic kidney disease: results from the national health and nutrition examination survey (2011–2018). J Clin Med. 2023;12:779.
Cornacoff JB, Hebert LA, Sharma HM, Bay WH, Young DC. Adverse effect of exercise on immune complex-mediated glomerulonephritis. Nephron. 1985;40:292–6.
Finkelstein J, Joshi A, Hise MK. Association of physical activity and renal function in subjects with and without metabolic syndrome: a review of the Third National Health and Nutrition Examination Survey (NHANES III). Am J Kidney Dis. 2006;48:372–82.
Leehey DJ, Collins E, Kramer HJ, Cooper C, Butler J, McBurney C, et al. Structured exercise in obese diabetic patients with chronic kidney disease: a randomized controlled trial. Am J Nephrol. 2016;44:54–62.
Yang L, Wu X, Wang Y, Wang C, Hu R, Wu Y. Effects of exercise training on proteinuria in adult patients with chronic kidney disease: a systematic review and meta-analysis. BMC Nephrol. 2020;21:172.
Chen IR, Wang SM, Liang CC, Kuo HL, Chang CT, Liu JH, et al. Association of walking with survival and RRT among patients with CKD stages 3-5. Clin J Am Soc Nephrol. 2014;9:1183–9.
Beddhu S, Wei G, Marcus RL, Chonchol M, Greene T. Light-intensity physical activities and mortality in the United States general population and CKD subpopulation. Clin J Am Soc Nephrol. 2015;10:1145–53.
Bruinius JW, Hannan M, Chen J, Brown J, Kansal M, Meza N, et al. Self-reported physical activity and cardiovascular events in adults with ckd: findings from the CRIC (chronic renal insufficiency cohort) study. Am J Kidney Dis. 2022;80:751–61 e1.
Yamakoshi S, Nakamura T, Mori N, Suda C, Kohzuki M, Ito O. Effects of exercise training on renal interstitial fibrosis and renin-angiotensin system in rats with chronic renal failure. J Hypertens. 2021;39:143–52.
Pang Q, Wang P, Pan Y, Dong X, Zhou T, Song X, et al. Irisin protects against vascular calcification by activating autophagy and inhibiting NLRP3-mediated vascular smooth muscle cell pyroptosis in chronic kidney disease. Cell Death Dis. 2022;13:283.
Davies MD, Hughes F, Sandoo A, Alejmi A, Macdonald JH. The effect of exercise on vascular health in chronic kidney disease: a systematic review and meta-analysis of randomized controlled trials. Am J Physiol Ren Physiol. 2023;325:F638–F55.
Kirkman DL, Chavez DA. Exercise for chronic kidney disease: effects on vascular and cardiopulmonary function. Am J Physiol Heart Circ Physiol. 2024;326:H138–H47.
Bishop NC, Burton JO, Graham-Brown MPM, Stensel DJ, Viana JL, Watson EL. Exercise and chronic kidney disease: potential mechanisms underlying the physiological benefits. Nat Rev Nephrol. 2023;19:244–56.
Durstine JL, Grandjean PW, Davis PG, Ferguson MA, Alderson NL, DuBose KD. Blood lipid and lipoprotein adaptations to exercise: a quantitative analysis. Sports Med. 2001;31:1033–62.
Kodama S, Tanaka S, Saito K, Shu M, Sone Y, Onitake F, et al. Effect of aerobic exercise training on serum levels of high-density lipoprotein cholesterol: a meta-analysis. Arch Intern Med. 2007;167:999–1008.
Kelley GA, Kelley KS, Tran ZV. Walking, lipids, and lipoproteins: a meta-analysis of randomized controlled trials. Prev Med. 2004;38:651–61.
Igarashi Y, Akazawa N, Maeda S. Regular aerobic exercise and blood pressure in East Asians: a meta-analysis of randomized controlled trials. Clin Exp Hypertens. 2018;40:378–89.
Franklin BA, Eijsvogels TMH, Pandey A, Quindry J, Toth PP. Physical activity, cardiorespiratory fitness, and cardiovascular health: a clinical practice statement of the ASPC Part I: Bioenergetics, contemporary physical activity recommendations, benefits, risks, extreme exercise regimens, potential maladaptations. Am J Prev Cardiol. 2022;12:100424.
Saeidifard F, Medina-Inojosa JR, West CP, Olson TP, Somers VK, Bonikowske AR, et al. The association of resistance training with mortality: a systematic review and meta-analysis. Eur J Prev Cardiol. 2019;26:1647–65.
Delgado-Rodriguez M. Llorca J. Bias. J Epidemiol Community Health. 2004;58:635–41.
Loo G, Puar T, Foo R, Ong TK, Wang TD, Nguyen QN, et al. Unique characteristics of Asians with hypertension: what is known and what can be done? J Hypertens. 2024;42:1482–9.
Acknowledgements
We acknowledge the contributions of the staff members who collected the data and instructed subjects on urinalysis at the screening centers in Yamagata, Fukushima, Ibaraki, Niigata, Osaka, Fukuoka, Miyazaki, and Okinawa. We want to thank Editage for the English language editing.
Funding
This work was supported by Health and Labor Sciences Research Grants for Research on Design of the Comprehensive Health Care System for Chronic Kidney Disease (CKD) Based on the Risk Assessment by Specific Health Checkup from the Ministry of Health, Labor, and Welfare of Japan and a Grant-in-Aid for Research on Advanced Chronic Kidney Disease (REACH-J) and Practical Research Project for Renal Disease from the Japan Agency for Medical Research and Development (AMED).
Author information
Authors and Affiliations
Contributions
Research idea and study design: HTas, TK, ME, TU, HTam, RF, MN, MM, KS, KT; data acquisition: HY, KI, CI, KA, KY, TK, SF, IN, MKa, YS, TM, MKo, TW, KT; data analysis/interpretation: HTas, TK, ME, KT; statistical analysis: HTas, TK, ME; supervision or mentorship: TK, ME, KT. Each author contributed important intellectual content during manuscript drafting or revision and accepted accountability for the overall work by ensuring that questions about the accuracy or integrity of any portion of the work were appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethics approval and consent to participate
All procedures involving human participants followed the ethical standards of the institutional research committee at which the study was conducted (Fukushima Medical University; IRB Approval Number #1485, #2771) and the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This study was conducted following the Ethical Guidelines for Medical and Health Research Involving Human Subjects enacted by the Ministry of Health, Labor, and Welfare of Japan (http://www.mhlw.go.jp/file/06-Seisakujouhou-10600000-Daijinkanboukouseikagakuka/0000069410.pdf). According to these guidelines, investigators are not required to provide informed consent. Instead, we provided public information concerning the study on our website (http://www.fmu.ac.jp/univ/sangaku/data/koukai_2/2771.pdf). We ensured that there were opportunities for the research participants to refuse to use their personal information.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tasaki, H., Kosugi, T., Eriguchi, M. et al. Impact of exercise on all-cause and cardiovascular mortality in non-dialysis chronic kidney disease: the Japan specific health checkups (J-SHC) study. Hypertens Res 48, 2831–2840 (2025). https://doi.org/10.1038/s41440-025-02335-4
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41440-025-02335-4