Abstract
The measurement of an individual’s blood pressure (BP) while he or she is in a seated position is the standard BP measurement method. The significance of BP measurements obtained from an individual while he or she is in the supine position has also been described. Supine BP values are usually lower than seated BP values, and thus the condition of high supine BP is abnormal and called ‘supine hypertension.’ Although the mechanisms that underlie supine hypertension are not completely understood, it has been speculated that fluid retention and abnormal sympathetic nervous activity can lead to supine hypertension. Hypertension-mediated organ damage and cardiovascular events have been shown to be associated with supine hypertension; not only supine hypertension with neurogenic orthostatic hypotension but also supine hypertension without it. The treatment of supine hypertension has not been established. Considering the pathophysiological background of this condition, the use of antihypertensive drugs and bedtime dosing may be effective. Further research is necessary to clarify the significance of supine hypertension and to establish the optimal treatment for this condition.

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Aamir A, Mohammed R, Shaffi K, Khalil K. Syndrome of supine hypertension with orthostatic hypotension: pathophysiology and clinical approach. Curr Cardiol Rev. 2020;16:48–54.
Chisholm P, Anpalahan M. Orthostatic hypotension: pathophysiology, assessment, treatment and the paradox of supine hypertension. Intern Med J. 2017;47:370–9.
Jordan J, Fanciulli A, Tank J, Calandra-Buonaura G, Cheshire WP, Cortelli P, et al. Management of supine hypertension in patients with neurogenic orthostatic hypotension: scientific statement of the American Autonomic Society, European Federation of Autonomic Societies, and the European Society of Hypertension. J Hypertens. 2019;37:1541–6.
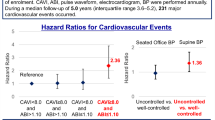
Kario K, Hoshide S, Kabutoya T, Nishizawa M, Yamagiwa K, Kawashima A, et al. Impact of vascular biomarkers and supine hypertension on cardiovascular outcomes in hypertensive patients: first results from the Cardiovascular Prognostic COUPLING Study in Japan. Hypertens Res. 2025;48:693–701.
Giao DM, Col H, Larbi Kwapong F, Turkson-Ocran RA, Ngo LH, Cluett JL, et al. Supine blood pressure and risk of cardiovascular disease and mortality. JAMA Cardiol. 2025;10:265–75.
Umemura S, Arima H, Arima S, Asayama K, Dohi Y, Hirooka Y, et al. The Japanese Society of Hypertension Guidelines for the Management of Hypertension (JSH 2019). Hypertens Res. 2019;42:1235–481.
McEvoy JW, McCarthy CP, Bruno RM, Brouwers S, Canavan MD, Ceconi C, et al. 2024 ESC Guidelines for the management of elevated blood pressure and hypertension: developed by the task force on the management of elevated blood pressure and hypertension of the European Society of Cardiology (ESC) and endorsed by the European Society of Endocrinology (ESE) and the European Stroke Organisation (ESO). Eur Heart J. 2024;45:3912–4018.
Whelton PK, Carey RM, Aronow WS, Casey DE, Collins KJ, Dennison Himmelfarb C, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Hypertension. 2018;71:e13–e115.
Fanciulli A, Jordan J, Biaggioni I, Calandra-Buonaura G, Cheshire WP, Cortelli P, et al. Consensus statement on the definition of neurogenic supine hypertension in cardiovascular autonomic failure by the American Autonomic Society (AAS) and the European Federation of Autonomic Societies (EFAS) : Endorsed by the European Academy of Neurology (EAN) and the European Society of Hypertension (ESH). Clin Auton Res. 2018;28:355–62.
Gibbons CH, Schmidt P, Biaggioni I, Frazier-Mills C, Freeman R, Isaacson S, et al. The recommendations of a consensus panel for the screening, diagnosis, and treatment of neurogenic orthostatic hypotension and associated supine hypertension. J Neurol. 2017;264:1567–82.
Smit AA, Halliwill JR, Low PA, Wieling W. Pathophysiological basis of orthostatic hypotension in autonomic failure. J Physiol. 1999;519:1–10.
Kario K, Chen CH, Park S, Park CG, Hoshide S, Cheng HM, et al. Consensus document on improving hypertension management in Asian patients, taking into account Asian characteristics. Hypertension. 2018;71:375–82.
Kotsis V, Stabouli S, Bouldin M, Low A, Toumanidis S, Zakopoulos N. Impact of obesity on 24-hour ambulatory blood pressure and hypertension. Hypertension. 2005;45:602–7.
Kimura G, Saito F, Kojima S, Yoshimi H, Abe H, Kawano Y, et al. Renal function curve in patients with secondary forms of hypertension. Hypertension. 1987;10:11–5.
Kario K. Nocturnal hypertension: new technology and evidence. Hypertension. 2018;71:997–1009.
Nolde JM, Kiuchi MG, Carnagarin R, Frost S, Kannenkeril D, Lugo-Gavidia LM, et al. Supine blood pressure-A clinically relevant determinant of vascular target organ damage in hypertensive patients. J Clin Hypertens. 2020;23:44–52.
Liu J, Li Y, Asayama K, Zhang XJ, Cheng HM, Park S, et al. Asian expert consensus on nocturnal hypertension management. Hypertension. 2025;82:945–56.
Wang F, Zhao H, Yang C, Kong G, Song L, Li C, et al. Association of blood pressure in the supine position with target organ damage in subjects over 60 years old. J Int Med Res. 2017;45:123–33.
Frewen J, Finucane C, Savva GM, Boyle G, Kenny RA. Orthostatic hypotension is associated with lower cognitive performance in adults aged 50 plus with supine hypertension. J Gerontol A Biol Sci Med Sci. 2014;69:878–85.
Newman L, O’Connor JD, Romero-Ortuno R, Reilly RB, Kenny RA. Supine hypertension is associated with an impaired cerebral oxygenation response to orthostasis: finding from the Irish Longitudinal Study on ageing. Hypertension. 2021;78:210–9.
Baik I, Kim NH, Kim SH, Shin C. Association of blood pressure measurements in sitting, supine, and standing positions with the 10-year risk of mortality in Korean adults. Epidemiol Health. 2023;45:e2023055.
Juraschek SP, Cortez MM, Flack JM, Ghazi L, Kenny RA, Rahman M, et al. Orthostatic hypotension in adults with hypertension: a scientific statement from the American Heart Association. Hypertension. 2024;81:e16–e30.
Raber I, Belanger MJ, Farahmand R, Aggarwal R, Chiu N, Al Rifai M, et al. Orthostatic hypotension in hypertensive adults: Harry Goldblatt Award for early career investigators 2021. Hypertension. 2022;79:2388–96.
Park JW, Okamoto LE, Biaggioni I. Advances in the pathophysiology and management of supine hypertension in patients with neurogenic orthostatic hypotension. Curr Hypertens Rep. 2022;24:45–54.
Okamoto LE, Celedonio JE, Smith EC, Gamboa A, Shibao CA, Diedrich A, et al. Local passive heat for the treatment of hypertension in autonomic failure. J Am Heart Assoc. 2021;10:e018979.
Arnold AC, Okamoto LE, Gamboa A, Shibao C, Raj SR, Robertson D, et al. Angiotensin II, independent of plasma renin activity, contributes to the hypertension of autonomic failure. Hypertension. 2013;61:701–6.
Arnold AC, Okamoto LE, Gamboa A, Black BK, Raj SR, Elijovich F, et al. Mineralocorticoid receptor activation contributes to the supine hypertension of autonomic failure. Hypertension. 2016;67:424–9.
Okamoto LE, Gamboa A, Shibao CA, Arnold AC, Choi L, Black BK, et al. Nebivolol, but not metoprolol, lowers blood pressure in nitric oxide-sensitive human hypertension. Hypertension. 2014;64:1241–7.
Shibao C, Gamboa A, Abraham R, Raj SR, Diedrich A, Black B, et al. Clonidine for the treatment of supine hypertension and pressure natriuresis in autonomic failure. Hypertension. 2006;47:522–6.
Komori T, Eguchi K, Saito T, Hoshide S, Kario K. Riser pattern is a novel predictor of adverse events in heart failure patients with preserved ejection fraction. Circ J. 2017;81:220–6.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declares no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Komori, T. Supine blood pressure measurement and its emerging role in cardiovascular risk stratification. Hypertens Res 49, 734–739 (2026). https://doi.org/10.1038/s41440-025-02531-2
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41440-025-02531-2