Abstract
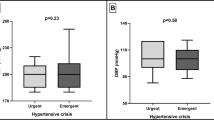
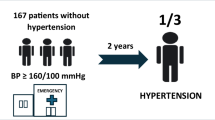
Hypertensive emergencies (HE) and urgencies (HU) are significant challenges for emergency physicians and hypertension specialists. The Eridano study is a prospective multicenter investigation assessing acute blood pressure (BP) disorders, subclinical hypertension-mediated organ damage (HMOD), and short- and long-term prognosis, including cardiovascular complications, new ED admissions, and BP control. Patients with symptomatic BP ≥ 180/110 mmHg admitted to the ED were enrolled and managed by ED personnel. Clinical evaluation and subclinical-HMOD assessment were performed at a Hypertension Centre within 72 h, followed by a 3-month follow-up. A total of 252 patients (21 HE, 231 HU) were included (mean age 61 ± 14 years, 52% males). Subclinical-HMOD was more common in HE (90% vs. 65%), including cardiac (76% vs. 43%), renal (40% vs. 11%), and cerebral (73% vs. 12%) damage. Vascular-HMOD was similar between the groups (54%), with increased pulse wave velocity (PWV) in 44% of patients. BP control (<140/90 mmHg) was achieved in 36% at 72 h. At 3 months, both groups showed lower systolic BP, and 29% of patients with uncontrolled BP at baseline achieved control. Female sex, lower ascending aorta diameter, and lower E/e’ ratio were associated with BP control. The composite endpoint (cardiovascular events and new ED admissions) occurred in 12% of patients at 3 months (4% major events, 7% new HU). Multivariate analysis showed female sex and PWV were associated with adverse outcomes. Two-thirds of patients had subclinical HMOD, primarily affecting large arteries and the heart. Female sex and PWV were associated with worse outcomes.

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Mancia G, Kreutz R, Brunström M, Burnier M, Grassi G, Januszewicz A, et al. 2023 ESH Guidelines for the management of arterial hypertension. The Task Force for the management of arterial hypertension of the European Society of Hypertension, endorsed by the International Society of Hypertension (ISH) and the European Renal Association. J Hypertens. 2023;41:1874–2071.
Astarita A, Covella M, Vallelonga F, Cesareo M, Totaro S, Ventre L, et al. Hypertensive emergencies and urgencies in emergency departments: a systematic review and meta-analysis. J Hypertens. 2020;38:1203–10.
Saladini F, Mancusi C, Bertacchini F, Spannella F, Maloberti A, Giavarini A, et al. Diagnosis and treatment of hypertensive emergencies and urgencies among Italian emergency and intensive care departments. Results from an Italian survey: Progetto GEAR (Gestione dell’Emergenza e urgenza in ARea critica). Eur J Intern Med. 2020;71:50–6.
Saladini F, Mancusi C, Bertacchini F, Spannella F, Maloberti A, Giavarini A, et al. Differences in Diagnosis and Management of Hypertensive Urgencies and Emergencies According to Italian Doctors from Different Departments Who Deal With Acute Increase in Blood Pressure-Data from Gear (Gestione Dell’emergenza e Urgenza in ARea Critica) Study. J Clin Med. 2022;11:2986.
Byrne RA, Rossello X, Coughlan JJ, Barbato E, Berry C, Chieffo A, et al. 2023 ESC Guidelines for the management of acute coronary syndromes. Eur Heart J. 2023;44:3720–826.
Erbel R, Aboyans V, Boileau C, Bossone E, Bartolomeo RD, Eggebrecht H, et al. 2014 ESC Guidelines on the diagnosis and treatment of aortic diseases: document covering acute and chronic aortic diseases of the thoracic and abdominal aorta of the adult. The task force for the diagnosis and treatment of aortic diseases of the European. Eur Heart J. 2014;35:2873–926.
Powers WJ, Rabinstein AA, Ackerson T, Adeoye OM, Bambakidis NC, Becker K, et al. Guidelines for the early management of patients with acute ischemic stroke: 2019 Update to the 2018 guidelines for the early management of acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. 2019;50:e344–418.
Greenberg SM, Ziai WC, Cordonnier C, Dowlatshahi D, Francis B, Goldstein JN, et al. 2022 Guideline for the management of patients with spontaneous intracerebral hemorrhage: a guideline from the American Heart Association/American Stroke Association. Stroke. 2022;53:e282–361.
Sinkey RG, Battarbee AN, Bello NA, Ives CW, Oparil S, Tita ATN. Prevention, diagnosis, and management of hypertensive disorders of pregnancy: a comparison of international guidelines. Curr Hypertens Rep. 2020;22:66.
Visseren FLJ, Mach F, Smulders YM, Carballo D, Koskinas KC, Bäck M, et al. 2021 ESC guidelines on cardiovascular disease prevention in clinical practice. Eur Heart J. 2021;42:3227–337.
Levy PD, Mahn JJ, Miller J, Shelby A, Brody A, Davidson R, et al. Blood pressure treatment and outcomes in hypertensive patients without acute target organ damage: a retrospective cohort. Am J Emerg Med. 2015;33:1219–24.
Patel KK, Young L, Howell EH, Hu B, Rutecki G, Thomas G, et al. Characteristics and outcomes of patients presenting with hypertensive urgency in the office setting. JAMA Intern Med. 2016;176:981–8.
Rothwell PM, Howard SC, Dolan E, O’Brien E, Dobson JE, Dahlöf B, et al. Prognostic significance of visit-to-visit variability, maximum systolic blood pressure, and episodic hypertension. Lancet. 2010;375:895–905.
Vlcek M, Bur A, Woisetschläger C, Herkner H, Laggner AN, Hirschl MM. Association between hypertensive urgencies and subsequent cardiovascular events in patients with hypertension. J Hypertens. 2008;26:657–62.
Paini A, Tarozzi L, Bertacchini F, Aggiusti C, Rosei CA, De Ciuceis C, et al. Cardiovascular prognosis in patients admitted to an emergency department with hypertensive emergencies and urgencies. J Hypertens. 2021;39:2514–20.
Vallelonga F, Cesareo M, Menon L, Leone D, Lupia E, Morello F, et al. Hypertensive emergencies and urgencies: a preliminary report of the ongoing Italian multicentric study ERIDANO. Hypertens Res. 2023;46:1570–81.
Van Den Born BJH, Lip GYH, Brguljan-Hitij J, Cremer A, Segura J, Morales E, et al. ESC council on hypertension position document on the management of hypertensive emergencies. Eur Heart J Cardiovasc Pharmacother. 2019;5:37–46.
Williams B, Mancia G, Spiering W, Rosei EA, Azizi M, Burnier M, et al. 2018 ESC/ESH Guidelines for the management of arterial hypertension. Eur Heart J. 2018;39:3021–104.
Marwick TH, Gillebert TC, Aurigemma G, Chirinos J, Derumeaux G, Galderisi M, et al. Recommendations on the use of echocardiography in adult hypertension: a report from the European Association of Cardiovascular Imaging (EACVI) and the American Society of Echocardiography (ASE). Eur Heart J Cardiovasc Imaging. 2015;16:577–605.
Lang RM, Badano LP, Mor-Avi V, Afilalo J, Armstrong A, Ernande L, et al. Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Eur Heart J Cardiovasc Imaging. 2015;16:233–71.
Nagueh SF, Smiseth OA, Appleton CP, Byrd BF, Dokainish H, Edvardsen T, et al. Recommendations for the evaluation of left ventricular diastolic function by echocardiography: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr. 2016;29:277–314.
Van Bortel LM, Laurent S, Boutouyrie P, Chowienczyk P, Cruickshank JK, De Backer T, et al. Expert consensus document on the measurement of aortic stiffness in daily practice using carotid-femoral pulse wave velocity. J Hypertens. 2012;30:445–8.
Cheung AK, Chang TI, Cushman WC, Furth SL, Hou FF, Ix JH, et al. Executive summary of the KDIGO 2021 clinical practice guideline for the management of blood pressure in chronic kidney disease. Kidney Int. 2021;99:559–69.
Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF 3rd, et al. A new equation to estimate glomerular filtration rate. Ann Intern Med. 2009;150:604–12.
Longstreth WTJ, Manolio TA, Arnold A, Burke GL, Bryan N, Jungreis CA, et al. Clinical correlates of white matter findings on cranial magnetic resonance imaging of 3301 elderly people. The Cardiovascular Health Study. Stroke. 1996;27:1274–82.
Boulestreau R, Lucas L, Cremer A, Debeugny S, Rubin S, Gaudissard J, et al. Neurologically asymptomatic patients frequently present cerebral injuries during malignant hypertension: an MRI study. J Hypertens. 2021;39:2463–9.
Vallelonga F, Cesareo M, Menon L, Airale L, Leone D, Astarita A, et al. Cardiovascular hypertension-mediated organ damage in hypertensive urgencies and hypertensive outpatients. Front Cardiovasc Med. 2022;9:889554.
Cuspidi C, Negri F, Muiesan ML, Capra A, Lonati L, Milan A, et al. Prevalence and severity of echocardiographic left ventricular hypertrophy in hypertensive patients in clinical practice. Blood Press. 2011;20:3–9.
Airale L, Borrelli F, Arrivi A, Baracchi A, Bertacchini F, Cartella I, et al. Ascending aorta dilatation is associated to hard cardiovascular events, follow-up from multicentric ARGO-Perspective project. Hypertens Res. 2023;46:2016–23.
Vasan RS, Song RJ, Xanthakis V, Beiser A, DeCarli C, Mitchell GF, et al. Hypertension-mediated organ damage: prevalence, correlates, and prognosis in the community. Hypertension. 2022;79:505–15.
Papazafiropoulou A, Skliros E, Sotiropoulos A, Papafragos C, Gikas A, Apostolou O, et al. Prevalence of target organ damage in hypertensive subjects attending primary care: C.V.P.C. study (epidemiological cardio-vascular study in primary care). BMC Fam Pract. 2011;12:75.
Korhonen PE, Kautiainen H, Järvenpää S, Kantola I. Target organ damage and cardiovascular risk factors among subjects with previously undiagnosed hypertension. Eur J Prev Cardiol. 2014;21:980–8.
Fan Y, Gao W, Li J, Fan F, Qin X, Liu L, et al. Effect of the baseline pulse wave velocity on short-term and long-term blood pressure control in primary hypertension. Int J Cardiol. 2020;317:193–9.
Ichihara A, Kaneshiro Y, Takemitsu T, Sakoda M, Hayashi M. Ambulatory blood pressure variability and brachial-ankle pulse wave velocity in untreated hypertensive patients. J Hum Hypertens. 2006;20:529–36.
Salvetti M, Paini A, Colonetti E, Tarozzi L, Bertacchini F, Aggiusti C, et al. Hypertensive emergencies and urgencies: a single-centre experience in Northern Italy 2008-2015. J Hypertens. 2020;38:52–8.
Fragoulis C, Polyzos D, Mavroudis A, Tsioufis PA, Kasiakogias A, Leontsinis I, et al. One-year outcomes following a hypertensive urgency or emergency. Eur J Intern Med. 2024;120:107–13.
Ji H, Kim A, Ebinger JE, Niiranen TJ, Claggett BL, Bairey Merz CN, et al. Sex differences in blood pressure trajectories over the life course. JAMA Cardiol. 2020;5:255–62.
Ryan MJ, Clemmer JS, Mathew RO, Faulkner JL, Taylor EB, Abais-Battad JM, et al. Revisiting sex as a biological variable in hypertension research. J Clin Investig. 2024;134:e180078.
Gerdts E, Novella S, Devaux Y, Magni P, Marti HP, Sopić M, et al. Biological sex and cardiovascular disease prevention in systemic arterial hypertension. Arterioscler Thromb Vasc Biol. 2025;45:1973–82.
Vlachopoulos C, Aznaouridis K, Stefanadis C. Prediction of cardiovascular events and all-cause mortality with arterial stiffness: a systematic review and meta-analysis. J Am Coll Cardiol. 2010;55:1318–27.
Pinna G, Pascale C, Fornengo P, Arras S, Piras C, Panzarasa P, et al. Hospital admissions for hypertensive crisis in the emergency departments: a large multicenter Italian study. PLoS ONE. 2014;9:e93542.
Gerdts E, Sudano I, Brouwers S, Borghi C, Bruno RM, Ceconi C, et al. Sex differences in arterial hypertension. Eur Heart J. 2022;43:4777–88.
Di Gangi S, Brenner R, Grischott T, Burgstaller JM, Senn O, Rosemann T, et al. Blood pressure control and antihypertensive treatment in Swiss general practice: a cross-sectional study using routine data. Swiss Med Wkly. 2024;154:3898.
Acknowledgements
We are grateful to staff physicians and fellows of the Emergency departments and Hypertensive centers for their work. We also thank Michela Algeri, Arianna Ardito, Giordano Bianchi, Saverio Fabbri, Claudio Pascale, Alessandra Piazza, Giuliano Pinna, Giovanni Saccà, and Nicole Saxinger for essential collaboration and useful discussion.
Eridano Consortium
Dario Leone1,2, Salvatore Fragapani1,2, Giulia Bruno1,2, Giulia Mingrone1,2, Anna Colomba1,2, Jacopo Ligato1,2, Elvira Fanelli1,2, Lorenzo Airale2, Arianna Paladino1,2, Francesca Novello1,2, Enrico Lupia9, Fulvio Morello9, Maria Tizzani9, Antonella Ioverno3, Paola Sormani4, Carmine De Luca5, Raffaele Izzo5, Nicola De Luca5, Nicola Nesti8
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Vallelonga, F., Cesareo, M., Sanapo, M. et al. “Short-term prognosis of hypertensive emergencies and urgencies: second preliminary report of the ongoing Italian multicenter ERIDANO study”. Hypertens Res (2026). https://doi.org/10.1038/s41440-026-02586-9
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41440-026-02586-9