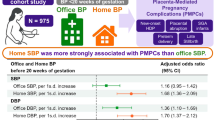
Abstract
This study investigated the associations between dynamic blood pressure (BP) trajectories during pregnancy and adverse birth outcomes using data from the China-US Collaborative Project on Neural Tube Defect Prevention. Among 281,224 pregnant women (mean age 25.07 ± 3.57 years), group-based trajectory modeling (GBTM) identified three distinct systolic (SBP) and diastolic (DBP) BP patterns: “Low-stable”, “Fast-increasing”, and “High-stable”. Compared to the Low-stable SBP group, women with Fast-increasing or High-stable SBP trajectories had significantly elevated risks of adverse outcomes, including an 16% higher risk of preterm birth (adjusted OR = 1.16, 95% CI:1.09–1.23) and 37% increased risk of low birth weight (LBW) (aOR=1.37,1.27–1.49) in the High-stable group. For DBP, the Fast-increasing trajectory showed the strongest associations, with a 19% higher preterm birth risk (aOR=1.19,1.11–1.26) and 63% increased LBW risk (aOR=1.63,1.51–1.76). Each 10 mmHg rise in SBP and DBP from mid-to-late pregnancy was independently linked to higher risks of preterm birth (SBP: aOR=1.10,1.06–1.12; DBP: aOR=1.16,1.13–1.20) and low birth weight (SBP: aOR=1.12,1.09–1.14; DBP: aOR=1.22,1.18–1.26). These findings highlight that dynamic BP changes during pregnancy are robust predictors of adverse birth outcomes, underscoring the importance of continuous BP monitoring for early risk identification and intervention.

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Haddad-Tóvolli R, Claret M. Metabolic and feeding adjustments during pregnancy. Nat Rev Endocrinol. 2023;19:564–80. https://doi.org/10.1038/s41574-023-00871-y. Nature Publishing Group.
Troiano NH. Physiologic and Hemodynamic Changes During Pregnancy. AACN Adv Crit Care. 2018;29:273–83. https://doi.org/10.4037/aacnacc2018911.
Macdonald-Wallis C, Lawlor DA, Fraser A, May M, Nelson SM, Tilling K. Blood pressure change in normotensive, gestational hypertensive, preeclamptic, and essential hypertensive pregnancies. Hypertens Dallas Tex. 2012;59:1241–8. https://doi.org/10.1161/HYPERTENSIONAHA.111.187039.
Reddy M, Rolnik DL, Harris K, Li W, Mol BW, Da Silva Costa F, et al. Challenging the definition of hypertension in pregnancy: a retrospective cohort study. Am J Obstet Gynecol. 2020;222:606.e1–606.e21. https://doi.org/10.1016/j.ajog.2019.12.272.
Zhu J, Zhang J, Ng MJ, Chern B, Yeo GS, Tan KH. Angiogenic factors during pregnancy in Asian women with elevated blood pressure in early pregnancy and the risk of preeclampsia: a longitudinal cohort study. BMJ Open. 2019;9:e032237 https://doi.org/10.1136/bmjopen-2019-032237.
Khan SS, Cameron NA, Lindley KJ. Pregnancy as an Early Cardiovascular Moment: Peripartum Cardiovascular Health. Circ Res Am Heart Assoc. 2023;132:1584–606. https://doi.org/10.1161/CIRCRESAHA.123.322001.
Gaillard R, Jaddoe VWV. Maternal cardiovascular disorders before and during pregnancy and offspring cardiovascular risk across the life course. Nat Rev Cardiol. 2023;20:617–30. https://doi.org/10.1038/s41569-023-00869-z. Nature Publishing Group.
Ma S, Wu L, Yu Q, Chen D, Geng C, Peng H, et al. Associations between trajectory of different blood pressure components in pregnancy and risk of adverse birth outcomes – a real world study. Risk Manag Health Policy. 2021;14:3255–63. https://doi.org/10.2147/RMHP.S318956.
Churchill D, Perry IJ, Beevers DG. Ambulatory blood pressure in pregnancy and fetal growth. Lancet. 1997;349:7–10. https://doi.org/10.1016/S0140-6736(96)06297-6. Elsevier.
Nuckols VR, Holwerda SW, Luehrs RE, DuBose LE, Stroud AK, Brandt D, et al. Beat-to-Beat Blood Pressure Variability in the First Trimester Is Associated With the Development of Preeclampsia in a Prospective Cohort. Hypertension. 2020;76:1800–7. https://doi.org/10.1161/HYPERTENSIONAHA.120.15019. American Heart Association.
Nobles CJ, Mendola P, Mumford SL, Naimi AI, Yeung EH, Kim K, et al. Preconception blood pressure levels and reproductive outcomes in a prospective cohort of women attempting pregnancy. Hypertens Dallas Tex. 2018;71:904–10. https://doi.org/10.1161/HYPERTENSIONAHA.117.10705.
Thilaganathan B. Association of higher maternal blood pressure with lower infant birthweight. Hypertension. 2016;67:499–500. https://doi.org/10.1161/HYPERTENSIONAHA.115.06880. American Heart Association.
Berry RJ, Li Z, Erickson JD, Li S, Moore CA, Wang H, et al. Prevention of neural-tube defects with folic acid in China. China-U.S. Collaborative Project for Neural Tube Defect Prevention. N Engl J Med. 1999;341:1485–90. https://doi.org/10.1056/NEJM199911113412001.
Gindler J, Li Z, Berry RJ, Zheng J, Correa A, Sun X, et al. Folic acid supplements during pregnancy and risk of miscarriage. Lancet Lond Engl. 2001;358:796–800. https://doi.org/10.1016/s0140-6736(01)05969-4.
Nagin DS. Group-based trajectory modeling: an overview. Ann Nutr Metab. 2014;65:205–10. https://doi.org/10.1159/000360229.
Nguena Nguefack HL, Pagé MG, Katz J, Choinière M, Vanasse A, Dorais M, et al. Trajectory modelling techniques useful to epidemiological research: a comparative narrative review of approaches. Clin Epidemiol. 2020;12:1205–22. https://doi.org/10.2147/CLEP.S265287.
Jones BL, Nagin DS. A note on a stata plugin for estimating group-based trajectory models. Socio Methods Res. 2013;42:608–13. https://doi.org/10.1177/0049124113503141. Thousand Oaks: SAGE Publications Inc.
LifeCycle Project-Maternal Obesity and Childhood Outcomes Study Group, Voerman E, Santos S, Inskip H, Amiano P, Barros H, et al. Association of gestational weight gain with adverse maternal and infant outcomes. JAMA. 2019;321:1702–15. https://doi.org/10.1001/jama.2019.3820.
Goldstein RF, Abell SK, Ranasinha S, Misso M, Boyle JA, Black MH, et al. Association of gestational weight gain with maternal and infant outcomes: a systematic review and meta-analysis. JAMA. 2017;317:2207–25. https://doi.org/10.1001/jama.2017.3635.
Goldenberg RL, Culhane JF, Iams JD, Romero R. Epidemiology and causes of preterm birth. Lancet Lond Engl. 2008;371:75–84. https://doi.org/10.1016/S0140-6736(08)60074-4.
The Apgar Score in the 21st Century | New England Journal of Medicine [Internet]. [cited 2024 Oct 4]. https://www.nejm.org/doi/full/10.1056/NEJM200102153440709. Accessed 4 Oct 2024
The Continuing Value of the Apgar Score for the Assessment of Newborn Infants | New England Journal of Medicine [Internet]. [cited 2024 Oct 4]. https://www.nejm.org/doi/full/10.1056/NEJM200102153440701. Accessed 4 Oct 2024
Siega-Riz AM, Viswanathan M, Moos M-K, Deierlein A, Mumford S, Knaack J, et al. A systematic review of outcomes of maternal weight gain according to the Institute of Medicine recommendations: birthweight, fetal growth, and postpartum weight retention. Am J Obstet Gynecol. 2009;201:339.e1–14. https://doi.org/10.1016/j.ajog.2009.07.002.
Mook-Kanamori DO, Steegers EAP, Eilers PH, Raat H, Hofman A, Jaddoe VWV. Risk factors and outcomes associated with first-trimester fetal growth restriction. JAMA. 2010;303:527–34. https://doi.org/10.1001/jama.2010.78.
Jieyu L, Yingying C, Tian G, Jiaxiang W, Jiawen L, Yingjie G, et al. Visit-to-visit blood pressure variability is associated with gestational hypertension and pre-eclampsia. Pregnancy Hypertens [Internet]. Pregnancy Hypertens; 2019 [cited 2024 Oct 16];18. https://doi.org/10.1016/j.preghy.2019.09.009
Bakker R, Steegers EAP, Hofman A, Jaddoe VWV. Blood pressure in different gestational trimesters, fetal growth, and the risk of adverse birth outcomes: the generation R study. Am J Epidemiol. 2011;174:797–806. https://doi.org/10.1093/aje/kwr151.
Magee LA, Singer J, Lee T, McManus RJ, Lay-Flurrie S, Rey E, et al. Are blood pressure level and variability related to pregnancy outcome? Analysis of control of hypertension in pregnancy study data. Pregnancy Hypertens. 2020;19:87–93. https://doi.org/10.1016/j.preghy.2019.12.002.
Rothwell PM, Howard SC, Dolan E, O’Brien E, Dobson JE, Dahlöf B, et al. Prognostic significance of visit-to-visit variability, maximum systolic blood pressure, and episodic hypertension. Lancet Lond Engl. 2010;375:895–905. https://doi.org/10.1016/S0140-6736(10)60308-X.
Hauspurg A, Parry S, Mercer BM, Grobman W, Hatfield T, Silver RM, et al. Blood pressure trajectory and category and risk of hypertensive disorders of pregnancy in nulliparous women. Am J Obstet Gynecol. 2019;221:277.e1–277.e8. https://doi.org/10.1016/j.ajog.2019.06.031.
Gunnarsdottir J, Akhter T, Högberg U, Cnattingius S, Wikström AK Elevated diastolic blood pressure until mid-gestation is associated with preeclampsia and small-for-gestational-age birth: a population-based register study. BMC Pregnancy Childbirth [Internet]. BMC. 2019 [cited 2024 Oct 16];19. https://doi.org/10.1186/s12884-019-2319-2
Zhu B, Huang K, Bao W, Yan S, Hao J, Zhu P, et al. Dose-response relationship between maternal blood pressure in pregnancy and risk of adverse birth outcomes: Ma’anshan birth cohort study. Pregnancy Hypertens. 2019;15:16–22. https://doi.org/10.1016/j.preghy.2018.09.004.
Li Y, Wei F-F, Wang S, Cheng Y-B, Wang J-G. Cardiovascular risks associated with diastolic blood pressure and isolated diastolic hypertension. Curr Hypertens Rep. 2014;16:489 https://doi.org/10.1007/s11906-014-0489-x.
Li W. Blood pressure self-management after hypertensive pregnancy. JAMA. 2024;331:1156 https://doi.org/10.1001/jama.2024.1965.
Kitt J, Krasner S, Barr L, Frost A, Tucker K, Bateman PA, et al. Cardiac remodeling after hypertensive pregnancy following physician-optimized blood pressure self-management: the POP-HT randomized clinical trial imaging substudy. Circulation. 2024;149:529–41. https://doi.org/10.1161/CIRCULATIONAHA.123.067597.
The BOSHI Study Group, Iwama N, Oba MS, Satoh M, Ohkubo T, Ishikuro M, et al. Association of maternal home blood pressure trajectory during pregnancy with infant birth weight: the BOSHI study. Hypertens Res. 2020;43:550–9. https://doi.org/10.1038/s41440-020-0416-2.
Youngstrom M, Tita A, Grant J, Szychowski JM, Harper LM. Perinatal outcomes in women with a history of chronic hypertension but normal blood pressures before 20 weeks of gestation. Obstet Gynecol. 2018;131:827–34. https://doi.org/10.1097/AOG.0000000000002574.
Teng H, Wang Y, Han B, Liu J, Cao Y, Wang J, et al. Gestational systolic blood pressure trajectories and risk of adverse maternal and perinatal outcomes in Chinese women. BMC Pregnancy Childbirth. 2021;21:155. https://doi.org/10.1186/s12884-021-03599-7.
High Blood Pressure During Pregnancy and Development of Risk Factors for Cardiovascular Disease. Ann Intern Med. 2018;169. https://doi.org/10.7326/P18-0008
Wu P, Green M, Myers JE. Hypertensive disorders of pregnancy. Bmj Br Med J. 2023;381:e071653 https://doi.org/10.1136/bmj-2022-071653. Publishing Group.
Umesawa M, Kobashi G. Epidemiology of hypertensive disorders in pregnancy: prevalence, risk factors, predictors and prognosis. Hypertens Res. 2017;40:213–20. https://doi.org/10.1038/hr.2016.126. Nature Publishing Group.
Burger RJ, Delagrange H, van Valkengoed IGM, de Groot CJM, van den Born B-JH, Gordijn SJ, et al. Hypertensive disorders of pregnancy and cardiovascular disease risk across races and ethnicities: a review. Front Cardiovasc Med. [Internet]. Frontiers; 2022 [cited 2026 Feb 20];9. https://doi.org/10.3389/fcvm.2022.933822
Acknowledgements
We sincerely thank all participants and staff of this Cohort Study for their invaluable contributions to data collection and study implementation.
Funding
This work was supported by the Noncommunicable Chronic Diseases-National Science and Technology Major Project [Grant Number 2023ZD0508600].
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Dawuti, W., Du, J., Tian, X. et al. Association of dynamic blood pressure trajectory during pregnancy with adverse birth outcomes: a large prospective cohort study in China. Hypertens Res (2026). https://doi.org/10.1038/s41440-026-02615-7
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41440-026-02615-7