Abstract
This study aimed to investigate the clinicopathological characteristics, response to chemotherapy, and clinical outcomes according to estrogen receptor (ER) expression levels in breast cancer (BC) patients treated with neoadjuvant chemotherapy (NAC). ER expression levels were categorized as ER-negative (expression in <1% of tumor cells), ER-low positive (1-10%), ER-intermediate positive (11-50%), and ER- high positive (>50%). Of the 1,365 cases, 647 (47.4%) were classified as ER-negative, 49 (3.6%) as ER- low positive, 48 (3.5%) as ER-intermediate positive, and 621 (45.5%) as ER-high positive BCs in pre-NAC biopsies. ER-intermediate positive tumors as well as ER-low positive tumors showed no differences in clinicopathological characteristics compared to ER-negative tumors with the exception of progesterone receptor positivity. While ER-low positive and ER-negative tumors showed similar chemo-responsiveness, ER-intermediate positive tumors were less responsive to NAC compared to ER-negative tumors. In patients with residual disease, pre- and post-NAC ER expression levels were found to be independent prognostic factors, but with no significant differences among ER-negative, ER-low positive, and ER-intermediate positive tumors. Our study indicates that ER-low positive BCs are similar to ER-negative BCs and that ER-intermediate positive BCs exhibit characteristics heterogeneous between ER-negative and ER-high positive BCs in terms of clinicopathological characteristics, chemo-responsiveness, and clinical outcomes.
Similar content being viewed by others
Introduction
Breast cancer is a heterogeneous disease with different biologic features and prognosis depending on its molecular subtype1,2,3. Currently, breast cancer subtypes can be classified based on the status of four surrogate markers: estrogen receptor (ER), progesterone receptor (PR), human epidermal growth factor receptor 2 (HER2), and Ki-67, and different treatment strategies are applied according to each subtype4. Among the subtypes, ER-positive breast cancers account for 70–80% of all breast cancers5,6,7 which are less responsive to chemotherapy8,9 and typically treated with endocrine therapy (ET)10.
ER positivity has been defined as having at least 1% positive tumor nuclei in immunohistochemistry (IHC) assays11. However, studies have revealed that breast cancers with 1–10% ER positivity exhibit characteristics similar to ER-negative breast cancers and do not significantly benefit from ET12,13,14. Reflecting these findings, the 2020 ASCO/CAP guidelines recommend that breast cancers with 1–10% ER-positive tumor cells be reported under a new category: “ER-low positive”5.
In addition to ER-low positive breast cancer, various cutoffs for ER-intermediate positivity, such as 10–20% or 10–50%, have been explored in further studies to determine whether these groups exhibit clinical outcomes more similar to ER-negative tumors15,16. Some studies have shown that breast cancers with ER-intermediate expression, defined as 10–50%, might resemble ER-high positive rather than ER-negative tumors in outcomes17, though no consensus exists on the definition of ER-intermediate threshold.
Furthermore, studies on chemotherapy response according to ER expression levels have yielded conflicting results. Some studies have suggested that a 10% ER cutoff discriminates response to neoadjuvant chemotherapy (NAC) fairly well18,19,20. However, other studies argue that the best cutoff for predicting response is higher at 30%21 or even 80%22. This variability highlights the importance of further investigation on the impact of ER expression levels on treatment outcomes of NAC.
Therefore, this study aims to investigate the clinicopathological characteristics, response to chemotherapy, and clinical outcomes according to ER expression levels in breast cancer patients treated with NAC, focusing on ER-low positive and ER-intermediate positive breast cancers.
Results
Clinicopathological characteristics of the patients according to ER expression levels
The clinicopathological characteristics of the patients included in this study are summarized in Supplementary Table S1. ER expression levels were categorized as ER-negative (expression in <1% of tumor cells), ER-low positive (1–10%), ER-intermediate positive (11–50%), and ER-high positive (>50%). Of the 1365 cases, 647 (47.4%) were classified as ER-negative, 49 (3.6%) as ER-low positive, 48 (3.5%) as ER-intermediate positive, and 621 (45.5%) as ER-high positive breast cancers in pre-NAC biopsies. Representative examples of each ER category are shown in Fig. 1. Significant differences were found in age at diagnosis (p < 0.001), menopausal status (p < 0.001), clinical N stage (p = 0.001), histologic grade (p < 0.001), PR expression (p < 0.001), HER2 status (p < 0.001), Ki-67 index (p < 0.001), NAC regimen (p < 0.001), and ET use (p < 0.001) across the four categories (Table 1).
a ER-negative, with expression in <1% of tumor cells. b ER-low positive, with expression in 1–10% of tumor cells. c ER-intermediate positive, with expression in 11–50% of tumor cells. d ER-high positive, with expression in >50% of tumor cells. ER, estrogen receptor.
When comparing two groups from the four categories, PR status was significantly different in all comparisons. Clinicopathological characteristics of ER-low and ER-intermediate positive breast cancers were not different from ER-negative breast cancers except for PR status and ET use. ER-low and intermediate positive tumors showed higher histologic grade (adj. p < 0.001), lower PR positivity (adj. p < 0.001), and higher Ki-67 index (adj. p < 0.001) compared to ER-high positive tumors. In ER-low positive tumors, the use of ET was significantly lower than ER-intermediate and ER-high positive tumors (adj. p < 0.001). (Supplementary Table S2).
Regression of tumor after NAC in relation to pre-NAC ER expression levels
Among the 1365 patients, the overall pathologic complete response (pCR) rate was 29.7% (n = 406). Higher ER expression levels were associated with decreased chemo-responsiveness with lower pCR rate, higher Residual Cancer Burden (RCB) class, and lower Miller-Payne (MP) grade (all p < 0.001; Fig. 2). pCR was achieved in 44.8% (n = 290) of ER-negative, 40.8% (n = 20) of ER-low positive, 20.8% (n = 10) of ER-intermediate positive, and 13.8% (n = 86) of ER-high positive breast cancers.
ER expression levels were divided into three groups with cutoff values of 1% and 10%. a–c and four groups with cutoff values of 1%, 10%, and 50% (d–f). a, d Pathologic complete response (pCR) status: yellow = pCR, dark blue = non-pCR. b, e Residual Cancer Burden (RCB) class: yellow = RCB 0, light brown = RCB 1, blue-gray = RCB 2, dark blue = RCB 3. c, f Miller–Payne (MP) grade: dark blue = grade 1, blue-gray = grade 2, taupe = grade 3, light brown = grade 4, yellow = grade 5. Asterisk (*) indicates a significant difference between two groups with p value < 0.05. NAC neoadjuvant chemotherapy, pCR pathologic complete remission, RCB Residual Cancer Burden, MP grade Miller-Payne grade.
When comparing two groups from the four categories, ER-low positive tumors showed pCR rates, RCB class, and MP grade similar to ER-negative tumors (all adj. p = 1.000). ER-intermediate positive tumors revealed no statistical differences in pCR rates, RCB class, and MP grade compared to ER-low positive or ER-high positive tumors; however, ER-intermediate positive tumors exhibited significant differences in pCR rate (adj. p = 0.008), RCB class (adj. p = 0.018), and MP grade (adj. p = 0.042) compared to ER-negative tumors. When ER expression levels were categorized into three groups (using cutoff values of 1% and 10%), all response rates were significantly different between ER < 1% or 1% ≤ ER < 10% and ER ≥ 10% (Fig. 2).
Clinicopathological characteristics of patients according to ER expression levels in cases with residual disease
As NAC can change clinicopathological characteristics of tumor after NAC, we compared clinicopathological characteristics of tumors according to pre-NAC ER expression levels in 959 cases which did not achieve pCR. The association between pre-NAC ER expression levels and pre-NAC characteristics were similar to the whole group. As for post-NAC characteristics, ypT stage (p < 0.001), ypN stage (p < 0.001), histologic grade (p < 0.001), LVI (p < 0.001), RCB class (p < 0.001), PR status (p < 0.001), HER2 status (p = 0.048), Ki-67 index (p < 0.001), and ET use (p < 0.001) were significantly different among the four groups (Table 2). When comparing two groups with regards to post-NAC characteristics, no difference was found between ER-negative and ER-low positive tumors except for ET use (adj. p < 0.001) (Supplementary Table S3). ER-intermediate positive tumors revealed higher PR positivity (adj. p < 0.001) and lower Ki-67 index (adj. p = 0.009) compared to ER-negative tumors, and showed lower ypT stage (adj. p = 0.006), higher histologic grade (adj. p < 0.001), lower PR positivity (adj. p < 0.001), and higher Ki-67 index (adj. p = 0.003) compared to ER-high positive tumors.
As clinicopathological characteristics of patients may be different depending on the NAC regimen, and the largest group of patients (40.5%) received the AC-D regimen (doxorubicin plus cyclophosphamide followed by docetaxel) of chemotherapy, we also analyzed AC-D treated subgroup with residual disease. Differences in variables according to the ER expression levels were consistent with those observed in the overall patient group, except for pre- and post-NAC HER2 status (p = 0.052 and p = 0.808, respectively), which showed no significant differences (Supplementary Table S4). ER-low and intermediate positive tumors were consistently comparable to ER-negative tumors. Also, ER-intermediate positive tumors had lower ypT stage (adj. p = 0.023), lower ypN stage (adj. p = 0.024), higher histologic grade (adj. p = 0.009), and lower PR positivity (adj. p < 0.001) compared to ER-high positive tumors.
Changes in ER expression levels after NAC
As NAC can change ER expression levels of the tumor, we compared ER expression levels of pre- and post-NAC specimens in 913 cases with residual disease for which post-NAC ER data were available. Overall ER status remained stable with a kappa value of 0.813 (Table 3; Supplementary Fig. S1). ER change differed according to pre-NAC ER expression levels (p < 0.001), with relatively stable ER-negative and ER-high positive tumors (concordance rate of 95.2% and 94.6%, respectively) and unstable ER-low positive and ER-intermediate positive tumors (concordance rate of 13.8% and 33.3%, respectively). While ER-low positive tumors changed mostly to ER-negative (58.6%, 17/29) tumors, ER-intermediate positive tumors showed a wide range of changes with ER-high positive in 36.1% (13/36), ER-intermediate positive in 33.3% (12/36), ER-negative in 19.4% (7/36), and ER-low positive in 11.1% (4/36) in decreasing order.
Prognosis of patients according to ER expression levels
The median follow-up duration for the entire cohort was 5.74 years. ER expression levels were not related to disease-free survival (DFS) of the patients in the whole group (Supplementary Table S5). However, in cases with residual disease, pre- and post-NAC ER expression levels were associated with DFS of the patients (p = 0.002 and p < 0.001, respectively, by the Log Rank test; Fig. 3). As for pre-NAC ER expression levels, ER-high positive tumors showed the best prognosis, which was significantly different from ER-negative and ER-low positive tumors (p < 0.001 and p = 0.031, respectively; Table 4) but not from ER-intermediate positive tumors (p = 0.292; Table 4). There were no statistical differences in DFS among ER-negative, ER-low positive, and ER-intermediate positive tumors in both pre- and post-NAC. In multivariate analyses, both pre- and post-NAC ER expression levels remained independent prognostic factors (p < 0.001; Table 4). Especially, as for pre-NAC ER expression levels, ER negativity [hazard ratio (HR) 1.974; 95% confidence interval (CI) 1.470-2.650; p < 0.001] and ER-low positivity (HR 2.141; 95% CI 1.080–4.244; p = 0.029) were revealed as independent poor prognostic factors for DFS. Besides ER expression levels, clinical stage, pre-NAC HER2 status, LVI, post-NAC Ki-67 index, RCB class, and MP grade were also found to be independent factors for DFS (Table 4). However, in the AC-D treated subgroup, ER expression levels were not related to DFS in cases with residual disease (p = 0.273 for pre-NAC; p = 0.166 for post-NAC; Supplementary Table S6).
Disease-free survival of patients according to a pre-NAC ER expression levels and b post-NAC ER expression levels, and overall survival of the patients according to c pre-NAC ER expression levels and d post-NAC ER expression levels in cases with residual disease. The pink line indicates ER-negative, the orange line ER-low positive, the green line ER-intermediate positive, and the blue line ER-high positive. P-values represent comparisons across all ER expression levels. NAC neoadjuvant chemotherapy, ER estrogen receptor.
Analysis of overall survival (OS) in cases with residual disease showed that pre- and post-NAC ER expression levels were also associated with survival of the patients (p = 0.010 and p = 0.003, respectively, by the Log Rank test; Fig. 3). Again, there were no statistical differences in OS among ER-negative, ER-low positive, and ER-intermediate positive tumors in both pre- and post-NAC. In multivariate analyses, pre-NAC ER expression levels did not remain a significant prognostic factor; however, post-NAC ER expression levels were revealed as an independent prognostic factor (p = 0.006) with ER negativity (HR 3.341; 95% CI 1.671–6.679; p = 0.001) as an independent poor prognostic factor for OS (Supplementary Table S7).
Prognostic impact of endocrine therapy and completion status across ER categories
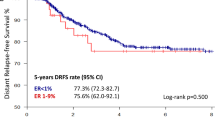
As ET use can influence patient survival, we further analyzed clinical outcomes according to ET use within each ER category. In the overall cohort, the proportion of patients receiving ET increased with ER expression levels (ER-negative, 3.4%; ER-low, 67.3%; ER-intermediate, 97.9%; ER-high positive, 100%; Table 1), demonstrating a strong correlation with ER categories (Spearman’s rho = 0.935, p < 0.001). ET use itself was not associated with patient outcomes. However, ET completion was associated with improved survival among patients who received ET (DFS, p < 0.001; OS, p < 0.001) and conferred significant DFS benefits in the ER-low, ER-intermediate, and ER-high positive subgroups (p = 0.005, p < 0.001, and p < 0.001, respectively). ET completion was also associated with longer OS in the ER-high positive subgroup (p < 0.001), but not in the ER-low or ER-intermediate positive subgroups (p not evaluable and p = 0.300, respectively).
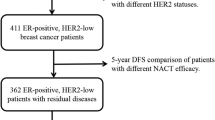
In patients with residual disease, both ET use and ET completion significantly impacted on survival (all p < 0.001 for DFS and OS). Subgroup analyses by ER expression level showed that ET use alone was not associated with outcomes. However, among those who received ET, completion was significantly associated with improved DFS in the ER-low, ER-intermediate, and ER-high positive subgroups (p = 0.017, p < 0.001, and p < 0.001, respectively; Fig. 4). ET completion was also associated with longer OS in the ER-high positive subgroup (p < 0.001; Fig. 4), but not in the ER-low or ER-intermediate positive subgroups (p not evaluable and p = 0.351, respectively; Fig. 4).
Disease-free survival in a ER-low, b ER-intermediate, and c ER-high positive groups, and overall survival in d ER-low, e ER-intermediate, and f ER-high positive groups. The orange line indicates patients who did not complete ET, and the blue line indicates patients who completed ET. ER estrogen receptor, ET endocrine therapy, NE not evaluable.
Discussion
In this study, we showed that ER expression levels were associated with clinicopathological characteristics of tumors, chemo-responsiveness, and clinical outcomes in breast cancer patients treated with NAC. We confirmed that ER-low positive tumors were more similar to ER-negative tumors, highlighting the importance of separation of this group of tumors from the conventional category of ER-positive tumors. Furthermore, we revealed that ER-intermediate positive tumors had higher variability in ER expression levels after NAC and that they showed heterogeneous features between ER-negative and ER-high positive tumors.
Of the whole study population, ER-negative tumors accounted for 47.4%, ER-low positive tumors 3.6%, ER-intermediate tumors 3.5%, and ER-high positive tumors 45.5%. Among ER-positive tumors, ER-low positive tumors comprised 6.8%, ER-intermediate positive tumors 6.7%, and ER-high positive tumors 86.5%. Since our study is based on advanced breast cancer patients who were treated with NAC, the proportion of ER-negative tumors were relatively high. Similarly, ER-low positive tumors were higher in frequency compared to previous studies (2–3% of ER-positive5 or all breast cancers23,24). However, the proportion of ER-intermediate positive tumors was comparable to the previously reported frequency of 4.7%24.
The four groups based on ER expression levels showed significantly different clinicopathological features. Higher ER expression level was associated with lower histologic grade and higher PR expression as previously reported16,17. Higher ER expression levels were also associated with younger age at diagnosis and premenopausal status, which is consistent with Korean breast cancer statistics indicating that hormone receptor–positive cases are more frequent at younger ages25. This finding may reflect ethnic differences as well as lifestyle factors among younger individuals that contribute to the increasing incidence of ER-positive breast cancer26.
When comparing each pair of groups, ER-negative, ER-low positive, and ER-intermediate positive tumors showed no significant differences except for PR expression and ET use, suggesting that clinicopathological features of ER-low and ER-intermediate positive tumors were comparable to those of ER-negative tumors. In contrast, ER-low and ER-intermediate positive tumors were different from ER-high positive tumors in histologic grade, PR expression, and Ki-67 index. Bari et al. showed that when using a 20% cutoff, ER-low and ER-intermediate positive breast cancers did not show a significant difference in any clinicopathological characteristics15. Voorwerk et al. reported that using a 50% cutoff, stromal tumor-infiltrating lymphocyte (TIL) level and expression of immune-related genes were similar in ER-negative, ER-low, and ER-intermediate positive tumors; however, ER-high positive tumors had significantly lower stromal TIL and immune-related genes than ER-intermediate positive tumors16, suggesting that ER-low and ER-intermediate positive tumors are similar to ER-negative than ER-high positive tumors. However, Massa et al. showed that with a 50% cutoff, ER-negative and ER-low positive tumors had a similar TIL level, and ER-intermediate positive tumors had a TIL level significantly lower than ER-low positive tumors, in contrast to previous studies17. Although further studies are needed to investigate the clinicopathological characteristics of ER-intermediate positive breast cancers and to determine the appropriate cutoff values, it seems to be clear that lower ER expression levels are associated with distinct clinicopathological characteristics.
In this study, pCR rate was 44.8% in ER-negative, 40.8% in ER-low positive, 20.8% in ER-intermediate positive, and 13.8% in ER-high positive breast cancers, consistent with previous findings that pCR rates decrease as ER level increases22,27. In terms of clinicopathological characteristics, ER-negative, ER-low positive, and ER-intermediate positive tumors were similar to each other except for PR positivity. However, with respect to chemo-responsiveness, ER-low positive tumors showed a pCR rate comparable to ER-negative tumors, while ER-intermediate positive tumors had a significantly lower pCR rate than ER-negative tumors. Additionally, there was no statistical difference in chemo-responsiveness between ER-intermediate positive and ER-high positive tumors. When ER levels were categorized into three groups (using cutoff values of 1% and 10%), ER-low positive tumors also showed a significantly higher pCR rate than tumors with ER > 10% (14.3%). These findings are in line with a previous study where no significant difference in pCR rate was observed between ER < 1% (40.6%) and 1% ≤ ER < 10% (25.0%), while ER ≥ 10% (7.4%) showed significantly lower pCR rates18. RCB class and MP grades followed a similar pattern as pCR rates. The three-group classification effectively differentiated chemo-responsiveness, indicating that 10% may be the optimal cutoff value to estimate response to NAC.
Of the 959 cases with residual disease after NAC, post-NAC clinicopathological characteristics, except for MP grade, were significantly different among the four groups. Although the chemotherapeutic regimen differed significantly among the four groups, the chemotherapeutic regimen did not affect the clinicopathological characteristics of patients based on ER expression levels. Among the cases with residual disease, in the subgroup treated by the AC-D regimen, differences in pre- and post-NAC variables according to the ER expression levels were consistent with those observed in the overall patient group, except for pre- and post-NAC HER2 status. The AC-D regimen is generally indicated for HER2-negative cases, and combining trastuzumab (AD-DH) is preferred for HER2-positive cases28,29, which likely increased the overall proportion of HER2-negative patients and reduced differences among the groups.
In this study, ER expression levels remained relatively stable after NAC with 89.8% of cases showing consistency with a kappa value of 0.813. However, ER-low and ER-intermediate positive groups showed lower concordance rates of 13.8% and 33.3% compared to the ER-negative (95.2%) and ER-high positive (94.6%) groups. These findings are consistent with the results from a previous study where cases with ER expression of 1–10% had a higher conversion rate (53.3%) compared to ER < 1% (7.1%) or ER > 10% (0.7%)30 The higher variability in ER expression levels in ER-low and ER-intermediate positive breast cancers can be attributed to their biological heterogeneity16,17.
In survival analyses of the cases with residual disease, both pre- and post-NAC ER expression levels were revealed as significant prognostic factors. ER-high positive tumors showed the most favorable outcomes in both cases. Typically, higher ER levels are associated with better DFS15,24 and OS31. In this study, there was a significant difference in DFS and OS between ER-high positive and ER-negative tumors and in DFS between ER-high positive and ER-low positive tumors; however, no significant differences were found between ER-high positive and ER-intermediate positive tumors. Paired comparisons between ER-negative, ER-low positive, and ER-intermediate positive tumors showed no significant differences. This may reflect the biologic similarities between ER-negative, ER-low positive, and ER-intermediate positive breast cancers. However, the small sample sizes of the ER-low and ER-intermediate positive groups call for caution in the interpretation of the results. Accordingly, our observations in these subgroups should be regarded as hypothesis-generating and highlight the need for studies with larger cohorts and more comprehensive adjustment for clinical variables. Furthermore, in this study, ER expression levels were not a significant prognostic factor in the homogeneous treated (AC-D treated) group, and some studies have reported that survival outcomes were not significantly influenced by ER levels17,22. Taken together, these findings highlight the complexity of ER status as a prognostic factor in residual disease, emphasizing the need for further research to elucidate the role of ER expression levels in modifying survival outcomes.
In this study, we evaluated the prognostic significance of ET use and ET completion within each ER category. In both the overall cohort and among patients with residual disease, ET use did not significantly influence outcomes within individual ER categories. By contrast, ET completion had a significant impact on DFS in the ER-low, ER-intermediate, and ER-high positive groups, and was further associated with improved OS in the ER-high positive group. These findings suggest that ET completion plays a pivotal role in patient outcomes, with its effect becoming more pronounced as ER expression increases. Consistent with our results, Choong et al. reported that omission of ET in ER-low early-stage breast cancer was associated with worse overall survival32. In our study, although ET use itself was not associated with survival in the ER-low positive group, ET completion was linked to improved survival, underscoring the importance of ET completion even in patients with ER-low positive tumors.
This study has several limitations. First, our study was conducted in a relatively homogeneous Korean population. Previous reports have shown that Asian patients tend to show more favorable clinical outcomes compared with African American or White patients33. Therefore, the findings of this study may not be directly generalizable to more diverse populations. Second, it is a retrospective study. The use of various chemotherapeutic regimens may have influenced the findings of the study. While there were no significant differences in radiotherapy or HER2-targeted therapy across the groups, ET and chemotherapy regimens varied significantly, which may have contributed to the differences in clinical outcomes. Among these, patients treated with the most commonly used AC-D regimen showed clinicopathological characteristics largely consistent with the overall cohort but exhibited notable differences in prognosis, highlighting a potential limitation. Third, as previously mentioned, the small sample sizes of the ER-low and intermediate positive groups likely reduced statistical power, limiting the ability to detect significant differences for these subgroups. Additionally, while some studies have suggested that incorporating both the percentage of ER-positive cells and staining intensity using a semi-quantitative method may better define clinicopathological characteristics and prognosis34,35, this study considered only the percentage of ER-positive cells. However, the key strength of the current study is a large cohort with consistent evaluation of ER expression levels. ER status was reported not only as negative or positive but also as a percentage by experienced breast pathologists, allowing accurate classification of ER-low and ER-intermediate positive categories.
In summary, we demonstrated that clinicopathological characteristics of ER-low and ER-intermediate positive tumors were more like those of ER-negative tumors. Also, we found significant differences in chemo-responsiveness based on ER expression levels. Especially, while ER-low positive tumors exhibited response rates to NAC similar to ER-negative tumors, ER-intermediate positive tumors were less responsive to NAC compared to ER-negative tumors. Pre- and post-NAC ER expression levels showed strong agreement, but ER-low and intermediate positive tumors showed greater variability. ER expression levels showed a significant impact on survival of the patients in cases with residual disease, but with no survival difference between ER-negative, ER-low positive, and ER-intermediate positive tumors. To conclude, our study indicated that ER-low positive tumors were similar to ER-negative tumors and that ER-intermediate positive tumors exhibited features heterogeneous between ER-negative and ER-high positive tumors with respect to clinicopathological characteristics, chemo-responsiveness, and clinical outcome. Further investigation is needed to determine whether these findings are due to the intrinsic role of ER or differences in treatment responses based on ER expression levels, and also to establish optimal cutoff values for ER expression categories.
Methods
Patient selection
Data of the patients who were diagnosed as invasive breast cancer and received NAC for breast cancer followed by surgery at the Seoul National University Bundang Hospital between 2004 and 2020 were collected. Of the 1377 patients, those with in situ or microinvasive carcinoma in biopsy specimen (n = 3), and those who had not received biomarker testing on biopsy specimen before NAC (n = 9) were excluded. Finally, a total of 1365 patients were included in this study. This study was approved by the Institutional Review Board at Seoul National University Bundang Hospital (IRB No. B-2310-860-101), and the requirement of informed consent was waived. This study was performed in accordance with the Declaration of Helsinki.
Clinicopathological information
Clinical information was collected from the electronic medical records. The following clinical data were recorded: age at diagnosis, initial clinical T and N stage (according to the American Joint Committee on Cancer Staging, 8th edition), NAC regimen, cycle of NAC, ET use and regimen, ET completion, HER2-targeted therapy and regimen, date of diagnosis for primary breast cancer, date of start of NAC, date of surgical resection, date of diagnosis for recurrence (if applicable), and date of last contact or death.
Pathological information, such as histologic subtype (by WHO classification), histologic grade (by the Bloom and Richardson grading system), lymphovascular invasion (LVI), and pathologic T and N stages after NAC, was obtained from the pathology reports and slide reviews. The degree of chemo-responsiveness was evaluated by Residual Cancer Burden (RCB) class36, and Miller-Payne grade (MP grade)37. Pathologic complete response (pCR) was defined as no residual invasive tumor cells in both the breast and axillary lymph node, regardless of the presence of residual ductal carcinoma in situ in the breast38.
Immunohistochemical data
IHC results of standard biomarkers, including ER, PR, HER2, and Ki-67 were obtained from both pre-NAC biopsy specimens and post-NAC resection specimens. Cases without IHC results of standard biomarkers in pre-NAC biopsy specimens were excluded in this study, while those without IHC results from post-NAC resection specimens were included but considered as missing data (mostly cases with unmeasurable residual disease). IHC staining was carried out on BenchMark XT autostainer (Ventana Medical Systems, Tucson, USA) using an i-View detection kit (Ventana Medical Systems, until 2012) or ultraView Universal DAB Detection Kit (Ventana Medical Systems). The antibodies used were as follows: ER (1:100, clone SP1, Labvision, Fremont, CA; ready-to-use, clone SP1, Ventana Medical Systems), PR (1:70, PgR 636, Dako, Carpinteria, CA; ready-to-use, clone 1E2, Ventana Medical Systems), HER2 (1:700, rabbit polyclonal A0485, Dako; ready to use, clone 4B5, Ventana Medical Systems), and Ki-67 (1:200, clone MIB-1, Dako).
IHC results of PR were regarded as positive if 1% or more of the tumor nuclei were stained5. HER2 IHC was re-scored using the 2018 ASCO/CAP guideline39. For IHC results of 2+ cases, HER2 in situ hybridization (ISH) was performed by fluorescence ISH using the PathVysion assay (Abbott Molecular, Downers Grove, IL) or by silver ISH using INFORM HER2 DNA and Chromosome 17 probes (Ventana Medical Systems). The final HER2 status was determined based on the 2018 ASCO/CAP guidelines39. For Ki-67 proliferation index in pre-NAC specimen, cases with 20% or more positive tumor cells were interpreted as high and others as low, and a 10% cutoff was used for post-NAC specimen.
Evaluation of ER expression level and categorization
ER expression was evaluated by experienced breast pathologists in daily practice and was reported with the proportion of positive cells and intensity. During this study, based on this ER status report, ER expression levels were categorized into four groups: ER-negative, ER-low positive, ER-intermediate positive, and ER-high positive. ER-negative was defined as expression in <1% of tumor cells in IHC, ER-low positive as expression in 1–10% of tumor cells, ER-intermediate positive as expression in 11–50% of tumor cells, and ER-high positive as expression in >50% tumor cells.
Molecular subtype
Breast cancer subtype was determined with standard biomarker profiles according to the 2013 St. Gallen International Expert Consensus40 with modification. Each subtype was defined as follows: luminal A (ER and PR positive, HER2 negative, Ki-67 low), luminal B (ER positive, HER2 negative and at least one of: Ki-67 high or PR negative; ER positive, HER2 positive, any Ki-67, any PR), HER2 positive (HER2 positive, ER and PR negative) and triple-negative (ER and PR negative, HER2 negative). Other cases were placed in the unclassified category, including those with ER negativity and PR positivity.
Statistical analysis
SPSS version 29.0.0 for Windows (IBM Corporation, New York, USA) was used for statistical analyses. Pearson’s chi-square test and Fisher’s exact test were used to compare the clinicopathological characteristics and regression of the tumor according to ER categories. Bonferroni correction was made for multiple testing, and adjusted (adj.) p-values were applied. Cohen’s kappa coefficient (κ) was used to evaluate concordance of the ER categories between pre- and post-NAC specimens. Disease-free survival (DFS) and overall survival (OS) were calculated as the time between the date of start of NAC and the date of recurrence or death. Survival curves were plotted by the Kaplan–Meier method, and their significance of differences was assessed using the Log Rank (Mantel-Cox) test. Multivariate analysis was conducted using a Cox proportional hazards model with a backward stepwise selection method. Variables significant in univariate analysis were included. When ER expression levels were significant, variables differing among ER categories were incorporated into the multivariate analysis, except for ET use (highly correlated with ER categories and analyzed separately) and NAC regimen (analyzed separately). Hazard ratio (HR) and 95% confidence intervals (CIs) were calculated for the significant variables. All p-values were two-sided, and p values less than 0.05 were considered statistically significant.
Data availability
The datasets generated and/or analyzed during the current study are not publicly available due to privacy concerns and institutional policy, but are available from the corresponding author on reasonable request.
References
Perou, C. M. et al. Molecular portraits of human breast tumours. Nature 406, 747–752 (2000).
Sørlie, T. et al. Gene expression patterns of breast carcinomas distinguish tumor subclasses with clinical implications. Proc. Natl. Acad. Sci. USA 98, 10869–10874 (2001).
Cancer Genome Atlas Network Comprehensive molecular portraits of human breast tumours. Nature 490, 61–70 (2012).
Korde, L. A. et al. Neoadjuvant chemotherapy, endocrine therapy, and targeted therapy for breast cancer: ASCO guideline. J. Clin. Oncol. 39, 1485–1505 (2021).
Allison, K. H. et al. Estrogen and progesterone receptor testing in breast cancer: ASCO/CAP guideline update. J. Clin. Oncol. 38, 1346–1366 (2020).
Hwang, K. T. et al. Impact of breast cancer subtypes on prognosis of women with operable invasive breast cancer: a population-based study using SEER database. Clin. Cancer Res. 25, 1970–1979 (2019).
Łukasiewicz, S. et al. Breast cancer-epidemiology, risk factors, classification, prognostic markers, and current treatment strategies-an updated review. Cancers 13, 4287 (2021).
Faneyte, I. F. et al. Breast cancer response to neoadjuvant chemotherapy: predictive markers and relation with outcome. Br. J. Cancer 88, 406–412 (2003).
Berry, D. A. et al. Estrogen-receptor status and outcomes of modern chemotherapy for patients with node-positive breast cancer. JAMA 295, 1658–1667 (2006).
Harvey, J. M., Clark, G. M., Osborne, C. K. & Allred, D. C. Estrogen receptor status by immunohistochemistry is superior to the ligand-binding assay for predicting response to adjuvant endocrine therapy in breast cancer. J. Clin. Oncol. 17, 1474–1481 (1999).
Hammond, M. E. et al. American Society of Clinical Oncology/College of American Pathologists guideline recommendations for immunohistochemical testing of estrogen and progesterone receptors in breast cancer. J. Clin. Oncol. 28, 2784–2795 (2010).
Raghav, K. P. et al. Impact of low estrogen/progesterone receptor expression on survival outcomes in breast cancers previously classified as triple negative breast cancers. Cancer 118, 1498–1506 (2012).
Chen, T. et al. Borderline ER-positive primary breast cancer gains no significant survival benefit from endocrine therapy: a systematic review and meta-analysis. Clin. Breast Cancer 18, 1–8 (2018).
Iwamoto, T. et al. Estrogen receptor (ER) mRNA and ER-related gene expression in breast cancers that are 1% to 10% ER-positive by immunohistochemistry. J. Clin. Oncol. 30, 729–734 (2012).
Bari, S. et al. A real-world data retrospective cohort study of low estrogen receptor-positive early breast cancer: natural history and treatment outcomes. Breast Cancer 14, 199–210 (2022).
Voorwerk, L. et al. Immune landscape of breast tumors with low and intermediate estrogen receptor expression. NPJ Breast Cancer 9, 39 (2023).
Massa, D. et al. Immune and gene-expression profiling in estrogen receptor low and negative early breast cancer. J. Natl. Cancer Inst. 116, 1914–1927 (2024).
Ohara, A. M. et al. PAM50 for prediction of response to neoadjuvant chemotherapy for ER-positive breast cancer. Breast Cancer Res. Treat. 173, 533–543 (2019).
Paakkola, N. M., Karakatsanis, A., Mauri, D., Foukakis, T. & Valachis, A. The prognostic and predictive impact of low estrogen receptor expression in early breast cancer: a systematic review and meta-analysis. ESMO Open 6, 100289 (2021).
Reinert, T. et al. Clinical implication of low estrogen receptor (ER-low) expression in breast cancer. Front. Endocrinol. 13, 1015388 (2022).
Osako, T., Nishimura, R., Okumura, Y., Toyozumi, Y. & Arima, N. Predictive significance of the proportion of ER-positive or PgR-positive tumor cells in response to neoadjuvant chemotherapy for operable HER2-negative breast cancer. Exp. Ther. Med. 3, 66–71 (2012).
Raphael, J., Gandhi, S., Li, N., Lu, F. I. & Trudeau, M. The role of quantitative estrogen receptor status in predicting tumor response at surgery in breast cancer patients treated with neoadjuvant chemotherapy. Breast Cancer Res. Treat. 164, 285–294 (2017).
Yi, M. et al. Which threshold for ER positivity? A retrospective study based on 9639 patients. Ann. Oncol. 25, 1004–1011 (2014).
Zhang, Z. et al. Pathological features and clinical outcomes of breast cancer according to levels of oestrogen receptor expression. Histopathology 65, 508–516 (2014).
Choi, J. E. et al. Breast cancer statistics in Korea, 2019. J. Breast Cancer 26, 207–220 (2023).
Kim, J. et al. Survival outcomes of young-age female patients with early breast cancer: an international multicenter cohort study. ESMO Open 9, 103732 (2024).
Fujii, T. et al. Revisiting the definition of estrogen receptor positivity in HER2-negative primary breast cancer. Ann. Oncol. 28, 2420–2428 (2017).
Slamon, D. et al. Adjuvant trastuzumab in HER2-positive breast cancer. N. Engl. J. Med. 365, 1273–1283 (2011).
Gradishar, W. J. et al. Breast cancer, version 3.2024, NCCN clinical practice guidelines in oncology. J. Natl. Compr. Cancer Netw. 22, 331–357 (2024).
Chen, H. L., Huang, F. B., Chen, Q. & Deng, Y. C. Impact of estrogen receptor expression level on response to neoadjuvant chemotherapy and prognosis in HER2-negative breast cancers. BMC Cancer 23, 841 (2023).
Dieci, M. V. et al. Quantitative expression of estrogen receptor on relapse biopsy for ER-positive breast cancer: prognostic impact. Anticancer Res. 34, 3657–3662 (2014).
Choong, G. M., Hoskin, T. L., Boughey, J. C., Ingle, J. N. & Goetz, M. P. Endocrine therapy omission in estrogen receptor-low (1%-10%) early-stage breast cancer. J. Clin. Oncol. 43, 1875–1885 (2025).
Taparra, K. et al. Disaggregation of Asian American and Pacific Islander Women With Stage 0-II breast cancer unmasks disparities in survival and surgery-to-radiation intervals: a national cancer database analysis from 2004 to 2017. JCO Oncol. Pr. 18, e1255–e1264 (2022).
Landmann, A. et al. Low estrogen receptor (ER)-positive breast cancer and neoadjuvant systemic chemotherapy: is response similar to typical ER-positive or ER-negative disease?. Am. J. Clin. Pathol. 150, 34–42 (2018).
Moldoveanu, D. et al. Clinical behavior, management, and treatment response of estrogen receptor low (1-10%) breast cancer. Ann. Surg. Oncol. 30, 6475–6483 (2023).
Symmans, W. F. et al. Measurement of residual breast cancer burden to predict survival after neoadjuvant chemotherapy. J. Clin. Oncol. 25, 4414–4422 (2007).
Ogston, K. N. et al. A new histological grading system to assess response of breast cancers to primary chemotherapy: prognostic significance and survival. Breast 12, 320–327 (2003).
von Minckwitz, G. et al. Definition and impact of pathologic complete response on prognosis after neoadjuvant chemotherapy in various intrinsic breast cancer subtypes. J. Clin. Oncol. 30, 1796–1804 (2012).
Wolff, A. C. et al. Human epidermal growth factor receptor 2 testing in breast cancer: American Society of Clinical Oncology/College of American Pathologists clinical practice guideline focused update. J. Clin. Oncol. 36, 2105–2122 (2018).
Goldhirsch, A. et al. Personalizing the treatment of women with early breast cancer: highlights of the St Gallen international expert consensus on the primary therapy of early breast cancer 2013. Ann. Oncol. 24, 2206–2223 (2013).
Acknowledgements
This study was funded by National Research Foundation of Korea (NRF)’s Basic Science Research Program to Park SY by the Ministry of Science and ICT (Grant No. 2022R1F1A1065468). The funder played no role in study design, data collection, analysis and interpretation of data, or the writing of this manuscript.
Author information
Authors and Affiliations
Contributions
K.B. participated in the interpretation and analysis of data and drafted the manuscript. H.J.S. and Y.R.C. participated in the acquisition and interpretation of pathological data. H.C.S., E.K.K., K.J.S., S.H.K., and J.H.K. participated in the acquisition of clinical data. H.J.K. and S.Y.P. conceived of the study, participated in its design and interpretation, and were responsible for the preparation of the manuscript. All authors read and approved of the final paper.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Bai, K., Sung, HJ., Chung, Y.R. et al. Impact of estrogen receptor expression levels on chemo-responsiveness and prognosis of breast cancer patients treated with neoadjuvant chemotherapy. npj Breast Cancer 12, 37 (2026). https://doi.org/10.1038/s41523-026-00907-2
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41523-026-00907-2