Abstract
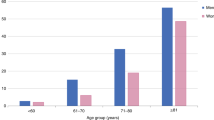
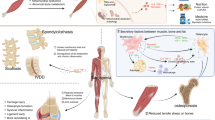
Sarcopenia is the accelerated loss of skeletal muscle mass and function commonly, but not exclusively, associated with advancing age. It is observed across many species including humans in whom it can lead to decline in physical function and mobility as well as to increased risk of adverse outcomes including falls, fractures and premature mortality. Although prevalence estimates vary because sarcopenia has been defined in different ways, even using a conservative approach, the prevalence is between 5% and 10% in the general population. A life course framework has been proposed for understanding not only the occurrence of sarcopenia in later life but also influences operating at earlier life stages with potentially important implications for preventive strategies. Harnessing progress in understanding the hallmarks of ageing has been key to understanding sarcopenia pathophysiology. Considerable convergence in approaches to diagnosis of sarcopenia has occurred over the last 10 years, with a growing emphasis on the central importance of muscle strength. Resistance exercise is currently the mainstay of treatment; however, it is not suitable for all. Hence, adjunctive and alternative treatments to improve quality of life are needed. An internationally agreed approach to definition and diagnosis will enable a step change in the field and is likely to be available in the near future through the Global Leadership Initiative in Sarcopenia.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$32.99 / 30 days
cancel any time
Subscribe to this journal
Receive 1 digital issues and online access to articles
$119.00 per year
only $119.00 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Cruz-Jentoft, A. J. & Sayer, A. A. Sarcopenia. Lancet 393, 2636–2646 (2019). This is a state of the art seminar paper on sarcopenia with a clinical focus.
Fielding, R. A. et al. Sarcopenia: an undiagnosed condition in older adults. Current consensus definition: prevalence, etiology, and consequences. International Working Group on Sarcopenia. J. Am. Med. Dir. Assoc. 12, 249–256 (2011). This is one of two substantive consensus definitions for sarcopenia developed and published almost simultaneously in 2010/2011 (see Cruz-Jentoft et al. (2010) for the other). This definition was developed by investigators in the USA under the leadership of the International Working Group on Sarcopenia (IWGS).
Anker, S. D. et al. Welcome to the ICD-10 code for sarcopenia. J. Cachexia Sarcopenia Muscle 7, 512–514 (2016).
Guralnik, J. M. et al. A short physical performance battery assessing lower extremity function: association with self-reported disability and prediction of mortality and nursing home admission. J. Gerontol. 49, M85–M94 (1994).
Visser, M. & Schaap, L. A. Consequences of sarcopenia. Clin. Geriatr. Med. 27, 387–399 (2011).
Zhang, X. et al. Sarcopenia as a predictor of all-cause mortality among older nursing home residents: a systematic review and meta-analysis. BMJ Open. 8, e021252 (2018).
Cawthon, P. M. et al. Putative cut-points in sarcopenia components and incident adverse health outcomes: an SDOC analysis. J. Am. Geriatr. Soc. 68, 1429–1437 (2020).
Xu, J. et al. Sarcopenia is associated with mortality in adults: a systematic review and meta analysis. Gerontology 68, 361–376 (2022).
Rosenberg, I. H. Summary comments. Am. J. Clin. Nutr. 50, 1231–1233 (1989). This is widely believed to be the first publication to use the term ‘sarcopenia’.
Evans, W. J. & Campbell, W. W. Sarcopenia and age-related changes in body composition and functional capacity. J. Nutr. 123, 465–468 (1993).
Bijlsma, A. Y. et al. Chronology of age-related disease definitions: osteoporosis and sarcopenia. Ageing Res. Rev. 11, 320–324 (2012).
Cawthon, P. M. Recent progress in sarcopenia research: a focus on operationalizing a definition of sarcopenia. Curr. Osteoporos. Rep. 16, 730–737 (2018).
Coletta, G. & Phillips, S. M. An elusive consensus definition of sarcopenia impedes research and clinical treatment: a narrative review. Ageing Res. Rev. 86, 101883 (2023).
Muscaritoli, M. et al. Consensus definition of sarcopenia, cachexia and pre-cachexia: joint document elaborated by Special Interest Groups (SIG) “cachexia-anorexia in chronic wasting diseases” and “nutrition in geriatrics”. Clin. Nutr. 29, 154–159 (2010). A paper by the Special Interest Group (SIG) of the European Society for Clinical Nutrition and Metabolism (ESPEN) that emphasized the need for a clear clinical definition of sarcopenia to enable the application of effective diagnostic and treatment approaches.
Cruz-Jentoft, A. J. et al. Sarcopenia: European consensus on definition and diagnosis: report of the European Working Group on Sarcopenia in Older People. Age Ageing 39, 412–423 (2010). This is one of two substantive consensus definitions for sarcopenia developed and published almost simultaneously in 2010/2011 (see Fielding et al. (2011) for the other). This definition was developed by investigators in Europe under the leadership of the European Working Group on Sarcopenia in Older People (EWGSOP).
Chen, L. K. et al. Sarcopenia in Asia: consensus report of the Asian Working Group for Sarcopenia. J. Am. Med. Dir. Assoc. 15, 95–101 (2014).
Studenski, S. A. et al. The FNIH sarcopenia project: rationale, study description, conference recommendations, and final estimates. J. Gerontol. A Biol. Sci. Med. Sci. 69, 547–558 (2014).
Cruz-Jentoft, A. J. et al. Sarcopenia: revised European consensus on definition and diagnosis. Age Ageing 48, 16–31 (2019). This is an updated sarcopenia definition produced by the European Working Group on Sarcopenia in Older People 2 (EWGSOP) that has replaced their earlier definition (Cruz-Jentoft et al. (2010)).
Bhasin, S. et al. Sarcopenia definition: the position statements of the Sarcopenia Definition and Outcomes Consortium. J. Am. Geriatr. Soc. 68, 1410–1418 (2020). A paper outlining the position statements of the Sarcopenia Definitions and Outcomes Consortium (SDOC), which provides an evidence-based definition of sarcopenia.
Chen, L. K. et al. Asian Working Group for Sarcopenia: 2019 Consensus update on sarcopenia diagnosis and treatment. J. Am. Med. Dir. Assoc. 21, 300–07.e2 (2020). This paper outlines a definition of sarcopenia proposed by the Asian Working Group for Sarcopenia (AWGS).
Zanker, J. et al. Consensus guidelines for sarcopenia prevention, diagnosis and management in Australia and New Zealand. J. Cachexia Sarcopenia Muscle 14, 142–156 (2023). This paper outlines consensus recommendations for sarcopenia developed by the Australian and New Zealand Society for Sarcopenia and Frailty Research (ANZSSFR) Sarcopenia Diagnosis and Management Task Force.
Dodds, R. M. et al. Global variation in grip strength: a systematic review and meta-analysis of normative data. Age Ageing 45, 209–216 (2016).
Sayer, A. A. & Cruz-Jentoft, A. Sarcopenia definition, diagnosis and treatment: consensus is growing. Age Ageing 51, afac220 (2022).
Cawthon, P. M. et al. Defining terms commonly used in sarcopenia research: a glossary proposed by the Global Leadership in Sarcopenia (GLIS) Steering Committee. Eur. Geriatr. Med. 13, 1239–1244 (2022).
Kirk, B. et al. The conceptual definition of sarcopenia: Delphi consensus from the Global Leadership Initiative in Sarcopenia (GLIS). Age Ageing 53, afae052 (2024). This paper reports on the first global conceptual definition of sarcopenia that has been created by the Global Leadership Initiative in Sarcopenia (GLIS) using a Delphi consensus process.
Shafiee, G. et al. Prevalence of sarcopenia in the world: a systematic review and meta-analysis of general population studies. J. Diabetes Metab. Disord. 16, 21 (2017).
Mayhew, A. J. et al. The prevalence of sarcopenia in community-dwelling older adults, an exploration of differences between studies and within definitions: a systematic review and meta analyses. Age Ageing 48, 48–56 (2019).
Carvalho do Nascimento, P. R., Bilodeau, M. & Poitras, S. How do we define and measure sarcopenia? A meta-analysis of observational studies. Age Ageing 50, 1906–1913 (2021).
Petermann-Rocha, F. et al. Global prevalence of sarcopenia and severe sarcopenia: a systematic review and meta-analysis. J. Cachexia Sarcopenia Muscle 13, 86–99 (2022).
Mballa Yene, B. V. et al. Prevalence of sarcopenia in Africa: a systematic review. Clin. Interv. Aging 18, 1021–1035 (2023).
Yuan, S. & Larsson, S. C. Epidemiology of sarcopenia: prevalence, risk factors, and consequences. Metabolism 144, 155533 (2023). This is a comprehensive review that summarizes evidence from 130 studies that have examined the risk factors and consequences of sarcopenia.
Yang, L., Smith, L. & Hamer, M. Gender-specific risk factors for incident sarcopenia: 8-year follow up of the English Longitudinal Study of Ageing. J. Epidemiol. Community Health 73, 86–88 (2019).
Sallfeldt, E. S. et al. Sarcopenia prevalence and incidence in older men – a MrOs Sweden study. Geriatr. Nurs. 50, 102–108 (2023).
Zhou, S. et al. Longitudinal association between uric acid and incident sarcopenia. Nutrients 15, 3097 (2023).
Lang, T. et al. Sarcopenia: etiology, clinical consequences, intervention, and assessment. Osteoporos. Int. 21, 543–559 (2010).
Cruz-Jentoft, A. J., Gonzalez, M. C. & Prado, C. M. Sarcopenia ≠ low muscle mass. Eur. Geriatr. Med. 14, 225–228 (2023).
Zuo, X. et al. Sarcopenia and cardiovascular diseases: a systematic review and meta-analysis. J. Cachexia Sarcopenia Muscle 14, 1183–1198 (2023).
Surov, A. & Wienke, A. Prevalence of sarcopenia in patients with solid tumors: a meta-analysis based on 81,814 patients. JPEN J. Parenter. Enter. Nutr. 46, 1761–1768 (2022).
Luo, L. et al. Sarcopenia as a risk factor of progression-free survival in patients with metastases: a systematic review and meta-analysis. BMC Cancer 23, 127 (2023).
Bullock, A. F. et al. Malnutrition, sarcopenia and cachexia: exploring prevalence, overlap, and perceptions in older adults with cancer. Eur. J. Clin. Nutr. 78, 486–493 (2024).
Kim, G. et al. Prognostic value of sarcopenia in patients with liver cirrhosis: a systematic review and meta-analysis. PLoS ONE 12, e0186990 (2017).
Prado, C. M. et al. Sarcopenic obesity in older adults: a clinical overview. Nat. Rev. Endocrinol. 20, 261–277 (2024).
Fagundes Belchior, G. et al. Osteosarcopenia: beyond age-related muscle and bone loss. Eur. Geriatr. Med. 11, 715–724 (2020).
Sato, S. et al. Respiratory sarcopenia: a position paper by four professional organizations. Geriatr. Gerontol. Int. 23, 5–15 (2023).
Wakabayashi, H. et al. Diagnosis and treatment of sarcopenic dysphagia: a scoping review. Dysphagia 36, 523–531 (2021).
SeyedAlinaghi, S. et al. A systematic review of sarcopenia prevalence and associated factors in people living with human immunodeficiency virus. J. Cachexia Sarcopenia Muscle 14, 1168–1182 (2023).
Gao, Q. et al. Associated factors of sarcopenia in community-dwelling older adults: a systematic review and meta-analysis. Nutrients 13, 4291 (2021).
Liu, J. C. et al. Multi-omics research in sarcopenia: current progress and future prospects. Ageing Res. Rev. 76, 101576 (2022).
Rai, M. et al. Skeletal muscle degeneration and regeneration in mice and flies. Curr. Top. Dev. Biol. 108, 247–281 (2014).
Frontera, W. R. in DeLisa’s Physical Medicine and Rehabilitation: Principles and Practice 6th edn (ed Frontera, W. R.) 69–88 (Lippincott Williams and Wilkins, 2019).
Schiaffino, S. & Reggiani, C. Fiber types in mammalian skeletal muscles. Physiol. Rev. 91, 1531 (2011).
Lloyd, E. M. et al. Slow or fast: implications of myofibre type and associated differences for manifestation of neuromuscular disorders. Acta Physiol. 238, e14012 (2023).
Granic, A. et al. Hallmarks of ageing in human skeletal muscle and implications for understanding the pathophysiology of sarcopenia in women and men. Clin. Sci. 137, 1721–1751 (2023). This comprehensive review evaluates how each of the nine original hallmarks of ageing (see Lopez-Otin et al. (2013)) contributes to the pathophysiology of sarcopenia. It also proposes five novel hallmarks of skeletal muscle ageing and considers their clinical relevance.
Holtze, S. et al. Alternative animal models of aging research. Front. Mol. Biosci. 8, 660959 (2021).
Shavlakadze, T. et al. Age-related gene expression signatures from limb skeletal muscles and the diaphragm in mice and rats reveal common and species-specific changes. Skelet. Muscle 13, 11 (2023).
Korstanje, R. et al. The Jackson Laboratory Nathan Shock Center: impact of genetic diversity on aging. Geroscience 43, 2129–2137 (2021).
Moaddel, R. et al. Proteomics in aging research: a roadmap to clinical, translational research. Aging Cell 20, e13325 (2021).
Ciciliot, S. et al. Muscle type and fiber type specificity in muscle wasting. Int. J. Biochem. Cell Biol. 45, 2191–2199 (2013).
Lopez-Otin, C. et al. The hallmarks of aging. Cell 153, 1194–1217 (2013). A seminal paper in ageing research that proposes nine cellular and molecular hallmarks of ageing that contribute to the ageing process and influence age-related phenotypes: genomic instability, telomere attrition, epigenetic alterations, loss of proteostasis, deregulated nutrient sensing, mitochondrial dysfunction, cellular senescence, stem cell exhaustion, and altered intercellular communication.
Schmauck-Medina, T. et al. New hallmarks of ageing: a 2022 Copenhagen Ageing Meeting summary. Aging 14, 6829–6839 (2022).
López-Otín, C. et al. Hallmarks of aging: an expanding universe. Cell 186, 243–278 (2023).
Van Ancum, J. M. et al. Lack of knowledge contrasts the willingness to counteract sarcopenia among community-dwelling adults. J. Aging Health 32, 787–794 (2020).
Guralnik, J. M. et al. Limited physician knowledge of sarcopenia: a survey. J. Am. Geriatr. Soc. 71, 1595–1602 (2023).
Welch, C. et al. Acute sarcopenia secondary to hospitalisation – an emerging condition affecting older adults. Aging Dis. 9, 151–164 (2018).
Montero-Errasquín, B. & Cruz-Jentoft, A. J. Acute sarcopenia. Gerontology 69, 519–525 (2023).
Beaudart, C. et al. Health outcomes of sarcopenia: a systematic review and meta-analysis. PLoS ONE 12, e0169548 (2017).
Malmstrom, T. K. et al. SARC-F: a symptom score to predict persons with sarcopenia at risk for poor functional outcomes. J. Cachexia Sarcopenia Muscle 7, 28–36 (2016).
Bahat, G., Erdoğan, T. & İlhan, B. SARC-F and other screening tests for sarcopenia. Curr. Opin. Clin. Nutr. Metab. Care 25, 37–42 (2022).
Huang, L. et al. The accuracy of screening instruments for sarcopenia: a diagnostic systematic review and meta-analysis. Age Ageing 52, afad152 (2023).
Cooper, R. et al. Objectively measured physical capability levels and mortality: systematic review and meta-analysis. BMJ 341, c4467 (2010).
Cooper, R. et al. Physical capability in mid-life and survival over 13 years of follow-up: British Birth Cohort Study. BMJ 348, g2219 (2014).
Koopman, J. J. et al. Handgrip strength, ageing and mortality in rural Africa. Age Ageing 44, 465–470 (2015).
Leong, D. P. et al. Prognostic value of grip strength: findings from the Prospective Urban Rural Epidemiology (PURE) study. Lancet 386, 266–273 (2015).
Celis-Morales, C. A. et al. Associations of grip strength with cardiovascular, respiratory, and cancer outcomes and all cause mortality: prospective cohort study of half a million UK Biobank participants. BMJ 361, k1651 (2018).
Bohannon, R. W. et al. Grip and knee extension muscle strength reflect a common construct among adults. Muscle Nerve 46, 555–558 (2012).
Roberts, H. C. et al. A review of the measurement of grip strength in clinical and epidemiological studies: towards a standardised approach. Age Ageing 40, 423–429 (2011). This paper outlines a standardized protocol for the assessment of hand grip strength.
Beaudart, C. et al. Assessment of muscle function and physical performance in daily clinical practice: a position paper endorsed by the European Society for Clinical and Economic Aspects of Osteoporosis, Osteoarthritis and Musculoskeletal Diseases (ESCEO). Calcif. Tissue Int. 105, 1–14 (2019).
Sanchez-Rodriguez, D., Marco, E. & Cruz-Jentoft, A. J. Defining sarcopenia: some caveats and challenges. Curr. Opin. Clin. Nutr. Metab. Care 23, 127–132 (2020).
Mijnarends, D. M. et al. Validity and reliability of tools to measure muscle mass, strength, and physical performance in community-dwelling older people: a systematic review. J. Am. Med. Dir. Assoc. 14, 170–178 (2013).
Compher, C. et al. Guidance for assessment of the muscle mass phenotypic criterion for the Global Leadership Initiative on Malnutrition diagnosis of malnutrition. JPEN J. Parenter. Enter. Nutr. 46, 1232–1242 (2022).
Nijholt, W. et al. The reliability and validity of ultrasound to quantify muscles in older adults: a systematic review. J. Cachexia Sarcopenia Muscle 8, 702–712 (2017).
Perkisas, S. et al. Application of ultrasound for muscle assessment in sarcopenia: 2020 SARCUS update. Eur. Geriatr. Med. 12, 45–59 (2021).
Pagano, A. P. et al. Estimating muscle mass using D3-creatine dilution: a narrative review of clinical implications and comparison with other methods. J. Gerontol. A Biol. Sci. Med. Sci. 79, glad280 (2024).
McCarthy, C. et al. D3-creatine dilution for skeletal muscle mass measurement: historical development and current status. J. Cachexia Sarcopenia Muscle 13, 2595–2607 (2022).
Verstraeten, L. M. G. et al. Handgrip strength rather than chair stand test should be used to diagnose sarcopenia in geriatric rehabilitation inpatients: REStORing health of acutely unwell adulTs (RESORT). Age Ageing 51, afac242 (2022).
Johansson, J. et al. Comparing associations of handgrip strength and chair stand performance with all-cause mortality – implications for defining probable sarcopenia: the Tromso Study 2015-2020. BMC Med. 21, 451 (2023).
Dodds, R. M. et al. Grip strength across the life course: normative data from twelve British studies. PLoS ONE 9, e113637 (2014). By pooling data from 12 British population-based studies this paper presents empirical data that demonstrate how mean levels of grip strength change across life and provides compelling evidence of the need for a life-course approach to the study of sarcopenia. The data presented in this paper have been used to identify cut-off points for low grip strength in the European Working Group on Sarcopenia in Older People 2 revised consensus definition for sarcopenia (see Cruz-Jentoft et al. (2019)).
Azzolino, D. et al. Musculoskeletal changes across the lifespan: nutrition and the life-course approach to prevention. Front. Med. 8, 697954 (2021).
Kulkarni, B., Hills, A. P. & Byrne, N. M. Nutritional influences over the life course on lean body mass of individuals in developing countries. Nutr. Rev. 72, 190–204 (2014).
Robinson, S. et al. The role of nutrition in the prevention of sarcopenia. Am. J. Clin. Nutr. 118, 852–864 (2023).
Santos, L., Elliott-Sale, K. J. & Sale, C. Exercise and bone health across the lifespan. Biogerontology 18, 931–946 (2017).
Bull, F. C. et al. World Health Organization 2020 guidelines on physical activity and sedentary behaviour. Br. J. Sports Med. 54, 1451–1462 (2020).
Cooper, R., Mishra, G. D. & Kuh, D. Physical activity across adulthood and physical performance in midlife: findings from a British birth cohort. Am. J. Prev. Med. 41, 376–384 (2011).
Dodds, R. et al. Physical activity levels across adult life and grip strength in early old age: updating findings from a British birth cohort. Age Ageing 42, 794–798 (2013).
Hurst, C. et al. Resistance exercise as a treatment for sarcopenia: prescription and delivery. Age Ageing 51, afac003 (2022). This paper outlines the principles of effective resistance exercise prescription and proposes a resistance exercise programme that can be used as a resource for clinicians and exercise practitioners treating older adults with sarcopenia.
Shen, Y. et al. Exercise for sarcopenia in older people: a systematic review and network meta analysis. J. Cachexia Sarcopenia Muscle 14, 1199–1211 (2023).
Fragala, M. S. et al. Resistance training for older adults: position statement from the National Strength and Conditioning Association. J. Strength. Cond. Res. 33, 2019–2052 (2019).
Liu, C. J. & Latham, N. K. Progressive resistance strength training for improving physical function in older adults. Cochrane Database Syst. Rev. 2009, Cd002759 (2009).
Dodds, R. M. et al. Sarcopenia, long-term conditions, and multimorbidity: findings from UK Biobank participants. J. Cachexia Sarcopenia Muscle 11, 62–68 (2020).
Bernabei, R. et al. Multicomponent intervention to prevent mobility disability in frail older adults: randomised controlled trial (SPRINTT project). BMJ 377, e068788 (2022).
Kirwan, R. P. et al. Protein interventions augment the effect of resistance exercise on appendicular lean mass and handgrip strength in older adults: a systematic review and meta-analysis of randomized controlled trials. Am. J. Clin. Nutr. 115, 897–913 (2022).
Nunes, E. A. et al. Systematic review and meta-analysis of protein intake to support muscle mass and function in healthy adults. J. Cachexia Sarcopenia Muscle 13, 795–810 (2022).
Granic, A. et al. Myoprotective whole foods, muscle health and sarcopenia: a systematic review of observational and intervention studies in older adults. Nutrients 12, 2257 (2020).
Bauer, J. et al. Evidence-based recommendations for optimal dietary protein intake in older people: a position paper from the PROT-AGE Study Group. J. Am. Med. Dir. Assoc. 14, 542–559 (2013).
Chen, L. K. et al. Roles of nutrition in muscle health of community-dwelling older adults: evidence-based expert consensus from Asian Working Group for Sarcopenia. J. Cachexia Sarcopenia Muscle 13, 1653–1672 (2022).
Deutz, N. E. et al. Protein intake and exercise for optimal muscle function with aging: recommendations from the ESPEN Expert Group. Clin. Nutr. 33, 929–936 (2014).
Ikizler, T. A. et al. KDOQI clinical practice guideline for nutrition in CKD: 2020 update. Am. J. Kidney Dis. 76, S1–S107 (2020).
Duarte, M. P. et al. Prevalence of sarcopenia in patients with chronic kidney disease: a global systematic review and meta-analysis. J. Cachexia Sarcopenia Muscle 15, 501–512 (2024).
Beaudart, C. et al. The effects of vitamin D on skeletal muscle strength, muscle mass, and muscle power: a systematic review and meta-analysis of randomized controlled trials. J. Clin. Endocrinol. Metab. 99, 4336–4345 (2014).
Cheng, S. H. et al. The optimal strategy of vitamin D for sarcopenia: a network meta-analysis of randomized controlled trials. Nutrients 13, 3589 (2021).
Prokopidis, K. et al. Effect of vitamin D monotherapy on indices of sarcopenia in community dwelling older adults: a systematic review and meta-analysis. J. Cachexia Sarcopenia Muscle 13, 1642–1652 (2022).
Sanders, K. M. et al. Annual high-dose oral vitamin D and falls and fractures in older women: a randomized controlled trial. JAMA 303, 1815–1822 (2010).
Pinto Pereira, S. M. et al. Linear and nonlinear associations between vitamin D and grip strength: a mendelian randomization study in UK Biobank. J. Gerontol. A Biol. Sci. Med. Sci. 78, 1483–1488 (2023).
Kirk, B., Zanker, J. & Duque, G. Osteosarcopenia: epidemiology, diagnosis, and treatment – facts and numbers. J. Cachexia Sarcopenia Muscle 11, 609–618 (2020).
Bagherniya, M. et al. The beneficial therapeutic effects of plant-derived natural products for the treatment of sarcopenia. J. Cachexia Sarcopenia Muscle 13, 2772–2790 (2022).
Bauer, J. M. et al. Effects of a vitamin D and leucine-enriched whey protein nutritional supplement on measures of sarcopenia in older adults, the PROVIDE study: a randomized, double blind, placebo-controlled trial. J. Am. Med. Dir. Assoc. 16, 740–747 (2015).
Sargeant, J. A. et al. A review of the effects of glucagon-like peptide-1 receptor agonists and sodium-glucose cotransporter 2 inhibitors on lean body mass in humans. Endocrinol. Metab. 34, 247–262 (2019).
Wu, S. et al. Effects of vibration therapy on muscle mass, muscle strength and physical function in older adults with sarcopenia: a systematic review and meta-analysis. Eur. Rev. Aging Phys. Act. 17, 14 (2020).
de Oliveira, T. M. D. et al. Effects of whole-body electromyostimulation on health indicators of older people: systematic review and meta-analysis of randomized trials. J. Bodyw. Mov. Ther. 31, 134–145 (2022).
Hardy, E. J. et al. Post-operative electrical muscle stimulation attenuates loss of muscle mass and function following major abdominal surgery in older adults: a split body randomised control trial. Age Ageing 51, afac234 (2022).
Rolland, Y. et al. Current and investigational medications for the treatment of sarcopenia. Metabolism 149, 155597 (2023).
Achison, M. et al. Effect of perindopril or leucine on physical performance in older people with sarcopenia: the LACE randomized controlled trial. J. Cachexia Sarcopenia Muscle 13, 858–871 (2022).
Lee, S. J. Targeting the myostatin signaling pathway to treat muscle loss and metabolic dysfunction. J. Clin. Invest. 131, e148372 (2021).
Lee, S. J. et al. Challenges and future prospects of targeting myostatin/activin A signaling to treat diseases of muscle loss and metabolic dysfunction. J. Gerontol. A Biol. Sci. Med. Sci. 78 (Suppl. 1), 32–37 (2023).
Fonseca, G. et al. Selective androgen receptor modulators (SARMs) as pharmacological treatment for muscle wasting in ongoing clinical trials. Expert. Opin. Investig. Drugs 29, 881–891 (2020).
Membrez, M. et al. Trigonelline is an NAD+ precursor that improves muscle function during ageing and is reduced in human sarcopenia. Nat. Metab. 6, 433–447 (2024).
Witham, M. D. et al. New horizons in cellular senescence for clinicians. Age Ageing 52, afad127 (2023).
Liu, S. et al. Effect of urolithin A supplementation on muscle endurance and mitochondrial health in older adults: a randomized clinical trial. JAMA Netw. Open. 5, e2144279 (2022).
Parker, S. G. et al. What is Comprehensive Geriatric Assessment (CGA)? An umbrella review. Age Ageing 47, 149–155 (2018).
Ellis, G. et al. Comprehensive geriatric assessment for older adults admitted to hospital. Cochrane Database Syst. Rev. 9, Cd006211 (2017).
Ambagtsheer, R. C. et al. Does CGA improve health outcomes in the community? An umbrella review. J. Am. Med. Dir. Assoc. 24, 782–789.e15 (2023).
Norman, K. & Otten, L. Financial impact of sarcopenia or low muscle mass – a short review. Clin. Nutr. 38, 1489–1495 (2019).
Sayer, A. A. et al. Is grip strength associated with health-related quality of life? Findings from the Hertfordshire Cohort Study. Age Ageing 35, 409–415 (2006).
Cooper, R. et al. Physical capability and subsequent positive mental wellbeing in older people: findings from five HALCyon cohorts. Age 36, 445–456 (2014).
Rizzoli, R. et al. Quality of life in sarcopenia and frailty. Calcif. Tissue Int. 93, 101–120 (2013).
Woo, T., Yu, S. & Visvanathan, R. Systematic literature review on the relationship between biomarkers of sarcopenia and quality of life in older people. J. Frailty Aging 5, 88–99 (2016).
Tsekoura, M. et al. Sarcopenia and its impact on quality of life. Adv. Exp. Med. Biol. 987, 213–218 (2017).
Beaudart, C. et al. Measuring health-related quality of life in sarcopenia: summary of the SarQoL psychometric properties. Aging Clin. Exp. Res. 35, 1581–1593 (2023). The Sarcopenia Quality of Life questionnaire (SarQoL) was developed in 2015 to assess health-related quality of life as it relates to sarcopenia. This review summarizes all available published evidence on the utility of the SarQoL up to January 2023.
Barbosa, M. V. et al. Association between functional aspects and health-related quality of life in patients with colorectal cancer: can handgrip strength be the measure of choice in clinical practice? Support. Care Cancer 31, 144 (2023).
da Costa Pereira, J. P. et al. Sarcopenia and dynapenia is correlated to worse quality of life perception in middle-aged and older adults with Parkinson’s disease. Nutr. Neurosci. 27, 310–318 (2023).
Beaudart, C. et al. Development of a self-administrated quality of life questionnaire for sarcopenia in elderly subjects: the SarQoL. Age Ageing 44, 960–966 (2015).
Witham, M. D. et al. Performance of the SarQoL quality of life tool in a UK population of older people with probable sarcopenia and implications for use in clinical trials: findings from the SarcNet registry. BMC Geriatr. 22, 368 (2022).
Molzahn, A. et al. The importance of facets of quality of life to older adults: an international investigation. Qual. Life Res. 19, 293–298 (2010).
Pinedo-Villanueva, R. et al. Health care costs associated with muscle weakness: a UK population-based estimate. Calcif. Tissue Int. 104, 137–144 (2019).
Offord, N. J. et al. Current practice in the diagnosis and management of sarcopenia and frailty – results from a UK-wide survey. J. Frailty Sarcopenia Falls 4, 71–77 (2019).
Caulfield, L. A., et al. The Benchmarking Exercise Programme for Older People (BEPOP): design, results and recommendations from the first wave of data collection. J. Frailty Sarcopenia Falls www.jfsf.eu/accepted/JFSF-23M-11-037.pdf (2024).
Dodds, R. M. et al. Advancing our understanding of skeletal muscle across the lifecourse: protocol for the MASS_Lifecourse study and characteristics of the first 80 participants. Exp. Gerontol. 166, 111884 (2022).
Cummings, S. R. et al. The Study of Muscle, Mobility and Aging (SOMMA): a unique cohort study about the cellular biology of aging and age-related loss of mobility. J. Gerontol. A Biol. Sci. Med. Sci. 78, 2083–2093 (2023).
Grounds, M. D. in Skeletal Muscle Repair and Regeneration (eds Schiaffino, S. & Partridge, P. A.) 269–302 (Springer, 2008).
McMahon, C. D. et al. Lifelong exercise and locally produced insulin-like growth factor-1 (IGF-1) have a modest influence on reducing age-related muscle wasting in mice. Scand. J. Med. Sci. Sports 24, e423–e435 (2014).
Soffe, Z. et al. Effects of loaded voluntary wheel exercise on performance and muscle hypertrophy in young and old male C57Bl/6J mice. Scand. J. Med. Sci. Sports 26, 172–188 (2016).
Pannérec, A. et al. A robust neuromuscular system protects rat and human skeletal muscle from sarcopenia. Aging 8, 712–729 (2016).
Acknowledgements
The authors thank H. Atkinson (Patient and Public Involvement and Engagement Manager for the Ageing, Sarcopenia and Multimorbidity Theme within the National Institute for Health and Care Research Newcastle Biomedical Research Centre) and the 11 people who shared their experiences of sarcopenia for contributing to the patient experience box. A.A.S., R.C. and M.D.W. acknowledge support from the National Institute for Health and Care Research (NIHR) Newcastle Biomedical Research Centre (reference NIHR203309). R.C. also receives support as part of a generous donation made by the McArdle family to Newcastle University for research that will benefit the lives of older people in the UK. R.A.F. acknowledges support from the US Department of Agriculture, under agreement no. 58-1950-4-003.
Author information
Authors and Affiliations
Contributions
Introduction (R.A.F. and R.C.), Epidemiology (P.M.C., H.A., M.-J.N.E. and R.C.), Mechanisms (M.D.G.), Diagnosis, screening and prevention (A.J.C.-J., H.A. and M.-J.N.E.), Management (M.D.W., H.A. and M.-J.N.E.), Quality of life (R.C.), Outlook (A.A.S.), overview of the Primer (A.A.S. and R.C.).
Corresponding author
Ethics declarations
Competing interests
A.A.S. reports research grant funding from the National Institute for Health and Care Research UK, UK Research and Innovation, a research collaboration agreement with Regeneron Pharmaceuticals and a previous Pfizer Investigator Initiated Research Grant. R.C. reports research grant funding from the National Institute for Health and Care Research UK and UK Research and Innovation. H.A. has no funding or other conflicts of interest to disclose. P.M.C. is a consultant to and owns stock in Myocorps. M.-J.N.E. has no funding or other conflicts of interest to disclose. R.A.F. reports grants from the National Institutes of Health and USDA Agricultural Research Service; grants and personal fees from Axcella Health, Juvicell, Inside Tracker and Biophytis; and personal fees from Amazentis, Nestle, Pfizer, Rejuvenate Biomed, Embion and Hevolution Foundation, outside the submitted work. M.G. has no funding or other conflicts of interest to disclose. M.D.W. reports research grant funding from the National Institute for Health and Care Research UK and UK Research and Innovation. A.J.C.-J. has no funding to disclose. A.J.C.-J. has received honoraria for lectures or for organizing independent educational events from Abbott Nutrition, Danone-Nutricia, Nestlé Health Science and Fresenius-Kabi, and consulting fees from Akros Pharma, Chugai Pharmaceutical, Rejuvenate Biomed, Reneo Pharmaceutical and Toray Industries.
Peer review
Peer review information
Nature Reviews Disease Primers thanks S. von Haehling; N. Martinez-Velilla, who co-reviewed with A. Cedeno-Veloz; D. Scott; and H. Wakabayashi, for their contribution to the peer review of this work.
Additional information
Informed consent
The authors affirm that all contributors to the patient experience box provided informed consent for publication of their experiences.
Disclaimer The views expressed in this publication are those of the authors and do not necessarily reflect the views of the National Institute for Health and Care Research, the Department of Health and Social Care, the McArdle family or the US Department of Agriculture.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sayer, A.A., Cooper, R., Arai, H. et al. Sarcopenia. Nat Rev Dis Primers 10, 68 (2024). https://doi.org/10.1038/s41572-024-00550-w
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41572-024-00550-w
This article is cited by
-
Association between diabetes and sarcopenia in US adults and the role of adiposity: a survey-weighted analysis of NHANES 2011–2018
BMC Public Health (2026)
-
Gluteus maximus cross-sectional area/density in 1-year mortality prediction for oldest-old hip fracture patients
BMC Geriatrics (2026)
-
SARC-F and six modified versions: prognostic role for prolonged hospital stay and 1-year mortality in older inpatients
BMC Geriatrics (2026)
-
Physical activity levels, awareness, and associations with geriatric syndromes in hospitalized older adults: a cross-sectional study
BMC Geriatrics (2026)
-
Predicting fall risk among older adults with sarcopenia in China using machine learning models: a six-year longitudinal study from CHARLS
BMC Geriatrics (2026)